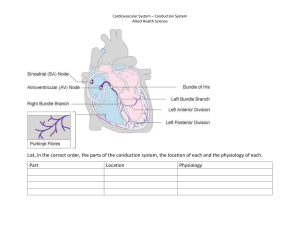
Cardiovascular Physiology Cardiovascular Physiology: Enrichment Prof. Mark A.W. Andrews, Ph.D. Prof. Mark Andrews, Ph.D. 1 Cardiovascular Physiology Cardiac Layers • epicardium (visceral pericardium) – serous membrane covering heart – adipose in thick layer in some places – coronary blood vessels travel through this layer Pericardial cavity Pericardial sac: • endocardium – smooth inner lining of heart and blood vessels – covers the valve surfaces and continuous with endothelium of blood vessels Fibrous layer Serous layer Epicardium • myocardium – layer of cardiac muscle proportional to work – muscle spirals around heart which produces wringing motion • fibrous skeleton of the heart - framework of collagenous and elastic fibers – provides structural support and attachment for cardiac muscle and anchor for valve tissue – electrical insulation between atria and ventricles important in timing and coordination of contractile activity Prof. Mark Andrews, Ph.D. Myocardium Endocardium Epicardium Pericardial sac 2 Cardiovascular Physiology Heart Chambers CO2 O2 • four chambers – right and left atria • • • – O2-poor, CO2-rich blood right and left ventricles • • Pulmonary circuit O2-rich, CO2-poor blood – • Systemic circuit Prof. Mark Andrews, Ph.D. Near fully saturated (96-98%) blood arrives from lungs via pulmonary veins Blood is sent to all organs of the body via aorta right side of heart • • CO2 Two inferior chambers Pump blood into arteries left side of heart • – Two superior chambers Receive blood returning to heart surface auricles (seen on surface) Lesser oxygenated blood (70-75%) arrives from inferior and superior vena cava Blood is sent to lungs via pulmonary trunk O2 3 Heart Valves Cardiovascular Physiology • valves ensure a one-way flow of blood through the heart • atrioventricular (AV) valves – controls blood flow between atria and ventricles – right AV valve has 3 cusps (tricuspid valve) – left AV valve has 2 cusps (mitral or bicuspid valve) – chordae tendineae - cords connect AV valves to papillary muscles on floor of ventricles • prevent AV valves from flipping inside out or bulging into the atria when the ventricles contract • semilunar valves - control flow into great arteries – open and close because of blood flow and pressure – pulmonary semilunar valve - in opening between right ventricle and pulmonary trunk – aortic semilunar valve in opening between left ventricle and aorta Prof. Mark Andrews, Ph.D. 4 Cardiovascular Physiology • Heart Valves fibrous skeleton of the heart - framework of collagen and elastin fibers – provides structural support and attachment for cardiac muscle and anchor for valve tissue. – Acts in electrical insulation between atria and ventricles for coordination of contractile activity. Left AV (bicuspid) valve Right AV (tricuspid) valve Fibrous skeleton Openings to coronary arteries Aortic valve Pulmonary valve Prof. Mark Andrews, Ph.D. 5 Cardiovascular Physiology Blood Flow Through the Heart 10 1 Blood enters right atrium from superior and inferior venae cavae. 2 Blood in right atrium flows through right Aorta AV valve into right ventricle. Left pulmonary artery 3 Contraction of right ventricle forces 11 5 4 Blood flows through pulmonary valve 9 Superior vena cava Right pulmonary veins pulmonary valve open. 5 Pulmonary trunk into pulmonary trunk. 4 6 6 1 7 3 Right atrium 8 Right AV (tricuspid) valve 2 Left pulmonary 5 Blood is distributed by right and left pulmonary arteries to the lungs, where it veins Left atrium Aortic valve Left ventricle 8 Contraction of left ventricle (simultaneous with step 3 ) forces aortic valve open. 9 Blood flows through aortic valve into ascending aorta. 10 Blood in aorta is distributed to every organ in the body, where it unloads O2 and loads CO2. 11 11 Blood returns to heart via venae cavae. • 5% (250 ml) of blood pumped by heart is pumped to the heart itself, through the coronary circulation to sustain its strenuous workload • Prof. Mark Andrews, Ph.D. 6 Blood returns from lungs via pulmonary veins to left atrium. Left AV 7 Blood in left atrium flows through left AV (bicuspid) valve valve into left ventricle. Right ventricle Inferior vena cava unloads CO2 and loads O2. requires abundant O2 and nutrients 6 Cardiovascular Physiology 1. Rapid 2. Diastasis Prof. Mark Andrews, Ph.D. Cardiac Cycle 1. Maximal 2. Reduced 7 Cardiovascular Physiology Wiggers’ Diagram Carl J. Wiggers (May 28, 1883 – April 28, 1963) Prof. Mark Andrews, Ph.D. 8 Cardiovascular Physiology • Phases of Cardiac Cycle (maximally seven) ventricular filling occurs in three phases: • (6) rapid ventricular filling - first one-third • blood enters very quickly and passively as it has been building up in atria via continuous venous return • (7) continued filling /diastasis - second one-third • marked by slower filling as venous return continues, going directly to the ventricles • P wave occurs at the end of diastasis, initiating… • (1) atrial systole - final one-third • atria contraction, forcing the final portion (10-20%) of cardiac filling (EDV) • QRS complex occurs at the end of this phase, initiating… • (2) isovolumic contraction • ventricular ejection occurs in two phases • (3) initial component is rapid once afterload is overcome • (4) as ejection continues, the volume ejected is reduced as the myocardium relaxes • (5) isovolumic relaxation as the afterload overcomes ventricular pressure • the remaining volume is ESV Prof. Mark Andrews, Ph.D. 9 Cardiovascular Physiology • Ventricular Ejection ejection of blood begins when the ventricular pressure exceeds arterial pressure and forces semilunar valves open • pressure peaks in left ventricle at about 120 mm Hg and 25 mm Hg in the right • blood spurts out of each ventricle rapidly at first – rapid ejection • then more slowly under reduced pressure – reduced ejection • ventricular ejections last about 200 – 250 msec • • stroke volume (SV) of about 70 mL of blood is ejected of the 130 mL in each ventricle • • • corresponds to the plateau phase of the cardiac action potential ejection fraction of about 54% as high as 80% in vigorous exercise end-systolic volume (ESV) – the 60 mL of 130 ml of blood left behind Prof. Mark Andrews, Ph.D. 10 Cardiovascular Physiology Contractile Parameters • cardiac cycle - one complete contraction and relaxation of chambers of the heart • stroke volume (SV) – amount ejected by one heart beat all four • SV = End diastolic volume (EDV) minus end systolic volume (ESV) • Ejection fraction (Ej%): SV/EDV • cardiac output (Q) – amount of blood ejected per minute • Q = heart rate x stroke volume • 4 to 6 L/min at rest • typically, an RBC leaving the left ventricle will arrive back in about one minute • vigorous exercise increases Q to 20+ L/min for fit person and can be greater than 35 L/min for elite athletes • cardiac reserve – the difference between a person’s maximum and resting Q; increases with fitness, and decreases with disease • cardiac index – Q per surface area (m2) • to keep cardiac output constant as we increase in age, the heart rate increases as the heart ages and SV decreases. Prof. Mark Andrews, Ph.D. 11 Cardiovascular Physiology Overview of Volume Changes end-systolic volume (ESV) -passively added to ventricle during atrial diastole -added by atrial systole total: end-diastolic volume (EDV) stroke volume (SV) ejected by ventricular systole leaves: end-systolic volume (ESV) 60 ml +60 ml +10 ml 130 ml -70 ml 60 ml both ventricles eject the same amount of blood Prof. Mark Andrews, Ph.D. 12 Cardiovascular Physiology Preload • three variables govern stroke volume: • Preload, Contractility, Afterload • example • increased preload or contractility causes increases stroke volume • increased afterload causes decrease stroke volume • preload – the amount of tension in ventricular myocardium immediately before it begins to contract (primarily due to blood volume) • • • • increased preload causes increased force of contraction exercise increases venous return and stretches myocardium cardiocytes generate more tension during contraction increased cardiac output matches increased venous return – Frank-Starling law of heart - SV∝ EDV • stroke volume is proportional to the end diastolic volume • ventricles eject as much blood as they receive • the more they are stretched, the harder they contract Prof. Mark Andrews, Ph.D. 13 Cardiovascular Physiology Prof. Mark Andrews, Ph.D. Cellular Basis of Starling’s Law of the Heart 14 Cardiovascular Physiology Contractility • contractility refers to how forcefully the myocardium contracts for a given preload • positive inotropic agents increase contractility • hypercalcemia can cause strong, prolonged contractions and even cardiac arrest in systole • catecholamines increase calcium levels • glucagon stimulates cAMP production • digitalis raises intracellular calcium levels and contraction strength • negative inotropic agents reduce contractility • hypocalcemia can cause weak, irregular heartbeat and cardiac arrest in diastole • hyperkalemia reduces strength of myocardial action potentials and the release of Ca2+ into the sarcoplasm • vagus nerves have effect on atria but too few nerves to ventricles for a significant inotropic effect Prof. Mark Andrews, Ph.D. 15 Cardiovascular Physiology Afterload • afterload – the blood pressure in the aorta and pulmonary trunk immediately distal to the semilunar valves • opposes the opening of these valves • limits stroke volume • hypertension increases afterload and opposes ventricular ejection • anything that impedes arterial circulation can also increase afterload • lung diseases that restrict pulmonary circulation • cor pulmonale – right ventricular failure due to obstructed pulmonary circulation • in emphysema, chronic bronchitis, and black lung disease Prof. Mark Andrews, Ph.D. 16 Cardiovascular Physiology Prof. Mark Andrews, Ph.D. Pressure-Volume (Work) Diagram 17 Cardiovascular Physiology Prof. Mark Andrews, Ph.D. 18 Cardiovascular Physiology Cardiac Conduction System 1 SA node fires. 2 Right atrium 2 1 Sinoatrial node (pacemaker) Left atrium 2 Atrioventricular node Atrioventricular bundle Purkinje fibers Prof. Mark Andrews, Ph.D. Purkinje fibers 3 Bundle branches 4 5 Excitation spreads through atrial myocardium, and Bachmann’s bundle 3 AV node fires. 4 Excitation spreads down AV bundle. 5 Purkinje fibers distribute excitation through ventricular myocardium. 19 Cardiovascular Physiology • Cardiac Conduction System coordinates the heartbeat • composed of an internal pacemaker and specialized myocardial conduction pathway • generates and conducts rhythmic electrical signals in the following order: • sinoatrial (SA) node - modified myocytes • in right atrium near base of superior vena cava • initiates each heartbeat and determines heart rate, ANS modulation • signal then spreads throughout atria; Bachmann’s bundle to L. atrium • atrioventricular (AV) node • located near the right AV valve at lower end of interatrial septum • electrical “gateway” to the ventricles; only conduction • fibrous skeleton, holding valves, acts as an insulator to prevent currents from getting to the ventricles from any other route • atrioventricular (AV) bundle (bundle of His) • enters into inverventricular septum • bundle then forks into right (one) and left (two) bundle branches • Purkinje fibers • specialized myocytes which are final connection of conductive fibers to all other ventricular cells Prof. Mark Andrews, Ph.D. 20 Cardiovascular Physiology • Nerve Supply to Heart sympathetic nerves • fibers terminate in SA and AV nodes, in atrial and ventricular myocardium, as well as the aorta, pulmonary trunk, and coronary arteries • increase heart rate and contraction strength • POSITIVE CHRONOTROPIC and INOTROPIC EFFECTS • also dilates coronary arteries to increase myocardial blood flow • parasympathetic nerves • pathway begins with nuclei of the vagus nerves in the medulla • fibers of right vagus nerve lead to the SA node • fibers of left vagus nerve lead to the AV node • stimulation reduces the heart rate; effect on strength is much less • NEGATIVE CHRONOTROPIC EFFECT Prof. Mark Andrews, Ph.D. 21 Cardiovascular Physiology • Chronotropic Effects of the ANS sympathetic postganglionic fibers are adrenergic • they release norepinephrine • binds to (β-) adrenergic receptors in the heart • activates c-AMP second-messenger system in cardiocytes and nodal cells • leads to opening of Ca2+ channels in plasma membrane • increased Ca2+ inflow accelerated depolarization of SA node • cAMP accelerates the uptake of Ca2+ by the sarcoplasmic reticulum allowing the cardiocytes to relax more quickly • by accelerating both contraction and relaxation, norepinephrine and cAMP increase the heart rate as high as 230 bpm • diastole becomes too brief for adequate filling • both stroke volume and cardiac output are reduced Prof. Mark Andrews, Ph.D. 22 Cardiovascular Physiology • Chronotropic Effects of the ANS parasympathetic vagus nerves have cholinergic, inhibitory effects on the SA and AV nodes • acetylcholine (ACh) binds to cholinergic (muscarinic) receptors • opens K+ gates in the nodal cells • as K+ leaves the cells, they become hyperpolarized and fire less frequently • heart slows down • parasympathetics work on the heart faster than sympathetics • parasympathetics do not use a second messenger system. • without influence from the cardiac centers, the heart has a intrinsic “natural” firing rate of 100 bpm • vagal tone – holds down this heart rate to 70 – 80 bpm at rest • steady background firing rate of the vagus nerves Prof. Mark Andrews, Ph.D. 23 Cardiovascular Physiology Cardiac Rhythm • cycle of events in heart – special names • systole – atrial / ventricular contraction • diastole – atrial / ventricular relaxation • sinus rhythm = normal heartrate (HR) is triggered by the SA node • A regular resting HR = 60 to 100 bpm • < 60 bpm is bradycardia; > 100 bpm is tachycardia • adult at rest is usually 70 to 80 bpm (some vagal tone) • nodal rhythm – from AV node if SA node is damaged, 40 to 50 bpm • intrinsic ventricular rhythm – if both SA and AV nodes are not functioning, rate set at 20 to 40 bpm • this requires pacemaker to sustain life • ectopic focus - another part of heart fires before the SA node; visible on EKG • can be caused by hypoxia, electrolyte imbalance, or caffeine, nicotine, and other drugs Prof. Mark Andrews, Ph.D. 24 Cardiovascular Physiology SA Node Potentials • • • • SA node does not have a stable resting membrane potential (MP) MP starts at -60 mV and drifts upward with a slow inflow of Na+ without a compensating outflow of K+, a gradual depolarization is called pacemaker potential Membrane potential (mV) +10 0 –10 Fast K+ efflux Fast Ca2+–Na+ inflow –20 Action potential Threshold –30 –40 Pacemaker potential –50 –60 Slow Na+ inflow (If current) –70 0 .4 .8 Time (sec) 1.2 1.6 At a threshold of -40 mV, voltage-gated fast Ca2+ and Na+ channels open, with a faster depolarization occurring and peaking at 0 mV K+ channels then open and K+ efflux occurs as the cell repolarizes, K+ channels close, and pacemaker potential starts over Prof. Mark Andrews, Ph.D. 25 Cardiovascular Physiology Electrical Behavior of Myocardium • ventricular myocytes have a stable resting potential of -90 mV • depolarize only when stimulated • depolarization phase (very brief) • stimulus opens voltage regulated Na+ gates, (Na+ rushes in) membrane depolarizes rapidly • action potential peaks at +30 mV • Na+ gates close quickly • plateau phase lasts 200 to 250 msec, sustains contraction for expulsion of blood from heart • Ca2+ channels are slow to close and SR is slow to remove Ca2+ from the cytosol • repolarization phase - Ca2+ channels close, K+ channels open, rapid diffusion of K+ out of cell returns it to resting potential • has a long absolute refractory period of 250 msec compared to 1 – 2 msec in skeletal muscle • prevents wave summation and tetanus which would stop the pumping action of the heart Prof. Mark Andrews, Ph.D. 26 Cardiovascular Physiology Prof. Mark Andrews, Ph.D. Fast-Type Myocardial Action Potential 27 Cardiovascular Physiology Action Potential of a Cardiocyte 3 Membrane potential (mV) +20 2 Na+ inflow depolarizes the membrane and triggers the opening of still 4 0 3 Na+ channels close when the cell depolarizes, and the Myocardial relaxation voltage peaks at nearly +30 mV. 4 Ca2+ entering through slow Ca2+channels prolongs depolarization of 2 membrane, creating a plateau. Plateau falls slightly because of some K+ leakage, but most K+ channels remain closed until end of plateau. Myocardial contraction –60 –80 more Na+ channels, creating a positive feedback cycle and a rapidly rising membrane voltage. 5 Action potential –20 –40 1 Voltage-gated Na+ channels open. Plateau Absolute refractory period 5 Ca2+ channels close and Ca2+ is transported out of cell. K+ channels 1 open, and rapid K+ outflow returns membrane to its resting potential. 0 .15 Time (sec) .30 1) Na+ gates open 2) Rapid depolarization 3) Na+ gates close 4) Slow Ca2+ channels open 5) Ca2+ channels close, K+ channels open (repolarization) Prof. Mark Andrews, Ph.D. 28 Cardiovascular Physiology Normal Electrocardiogram (EKG) • P wave SA node depolarizes and atria undergo systole atrial systole begins about 100 msec after SA signal 0.8 second • PR interval Atrial systole until ventricular sytole starts Normal range is from 120-210 msec R • R ventricles depolarize under 80 msec specific shape of the complex is due to direction of wave of depolarization and the shape of the two ventricles +1 Millivolts PQ segment ST segment T wave P wave 0 PR interval Q Prof. Mark Andrews, Ph.D. ST segment ventricular systole plateau in myocardial action potential • T wave QRS interval –1 Atria contract • S QT interval Ventricles contract Atria contract Ventricles contract QRS complex ventricular repolarization and relaxation; shape and duration differ from QRS complex 29 Cardiovascular Physiology Electrical Activity of Myocardium Wave of depolarization Wave of repolarization 1 Atria begin depolarizing. 4 Ventricular depolarization complete. T P Prof. Mark Andrews, Ph.D. 2 Atrial depolarization complete. Ventricular repolarization 5 begins at apex and progresses. Ventricular depolarization begins 3 at apex and progresses superiorly; atria repolarize. 6 Ventricular repolarization complete; heart is ready for the next cycle. 30 Cardiovascular Physiology Integration in the Medullary Cardiac Center § higher brain centers such as the cerebral cortex, limbic system, hypothalamus (ANS) affect heart rate (sensory / emotional stimuli) § medulla also receives input from muscles, joints, arteries, and other brainstem nuclei • proprioceptors in the muscles and joints • inform cardiac center about changes in activity: HR increases before metabolic demands rise • baroreceptors signal cardiac center • pressure sensors in aorta and internal carotid arteries • blood pressure decreases, signal rate drops, cardiac center increases heart rate • if blood pressure increases, signal rate rises, cardiac center decreases heart rate • chemoreceptors • • • • • in aortic arch, carotid arteries and medulla sensitive to blood pH, CO2 and O2 levels more important in respiratory control than cardiac control hypercapnia and acidosis stimulate the cardiac center to increase heart rate also respond to hypoxemia – oxygen deficiency in the blood • usually slows down the heart if hypercapnia / acidosis are not concomitant. Prof. Mark Andrews, Ph.D. 31 Cardiovascular Physiology Properties of Blood • viscosity - resistance of a fluid to flow, resulting from the cohesion of its particles – whole blood 4.5 - 5.5 times as viscous as water – plasma is 2.0 times as viscous as water • important concept in circulatory function – important parameter determining turbulent flow – best understood as “stickiness” • Oncotic pressure of blood - the total molarity of proteins dissolved in plasma, that cannot pass through the capillary walls – – – – affect transit of fluid across of capillary walls by draws water to them if too high, there will be too much fluid, increasing the blood pressure if too low, fluid leaks into tissues, edema occurs and blood pressure drops optimum oncotic pressure is achieved by regulation of protein production in the liver. – liver damage will greatly affect oncotic pressure – a component of Starling Forces Prof. Mark Andrews, Ph.D. 32 Cardiovascular Physiology Starling Forces Net filtration pressure: 13 out Forces (mm Hg) 33 out Net reabsorption pressure: 7 in 13 out 20 in Capillary 20 in Blood flow Venule Arteriole Arterial end • fluid filters out of the capillary and osmotically reenters at the venous end, delivering materials to the cell and removes metabolic wastes • opposing forces • hydrostatic pressures drives fluid away • high BP on arterial end of capillary • colloid oncotic pressure (COP) draws fluid towards the protein (20 mmHg) capillaries reabsorb 90% of the fluid they filter other 10% is absorbed by the lymphatic system and returned to the blood • • Prof. Mark Andrews, Ph.D. Venous end 33