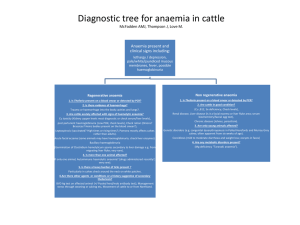
Classification of Anaemia By, Mosaab A. Omar
advertisement

Classification of
Anaemia
By,
Mosaab A. Omar
What is Anaemia?
Definition of Anaemia
Anemia is reduced Haemoglobin concentration in blood more than the
amount appropriate for that age, sex, race and physiological status.
Normal ranges of Hb
Men:
Hb 13.5 -17.5 g/dL
Women: Hb 11.5-16
g/dL
Infants : Hb 14 – 20
g/dL
Blood loss
On the basis of
cause
Inadequate production
of normal blood cells
Excessive destruction of
blood cells
Classification of
anaemia
Normocytic
On the basis
of
morphology
of RBC
Macrocytic
Microcytic
Classification according to Morphology
of RBC
• The average size of RBC (MCV) provides a convenient and
informative framework to categorize the various types of
anaemia
Normocytic Normochromic Anaemia
• The primary cause - reduction of number of RBCs.
Eg: Endocrine disorders (hypopituitarism, hypothyroidism
and hypoadrenalism)
Haematological disorders(aplastic anaemia ,haemolytic
anaemias)
Acute blood loss
Anaemia of chronic diseases
Normal
Put a normal
BP
Normocytic
Normocytic anaemia can be presented with elevation of
reticulocyte count or a reduction of reticulocyte count.
Elivated reticulocyte count
• Blood loss
anaemia
• Haemolytic
anaemia
Normal or low reticulocyte
count
• Bone marrow
disorders(Aplastic
anaemia)
• Chronic disease
• Kidney disease
Microcytic Anaemia
Many RBCs smaller than normal (MCV<80fL)
The RBCs are usually hypochromic (MCH<27pg)
Increased zone of central pallor
Cells are various in shape & size
Normal
Put a normal
BP
Try to find a
better picture
of microcytic
BP
Microcytic
Microcytic
Anaemia
Iron deficiency anaemia
Due to other reasons
Serum Ferritin level > 50µg/L
Serum Ferritin level > 50µg/L
Thalassaemia trait (α or β)
due to inadequate iron
for Hb synthesis)
Anaemia of chronic disease
Sideroblastic
anaemia(Inherited)
Lead poisoning
Sideroblastic anaemia
Bone Marrow Picture
Macrocytic Anaemia
• The average size of RBCs are larger than normal(>100fL)
• {MCHC is normal or high}
• Can be divided in to 2 types
Megaloblastic anaemia
Non megaloblastic anaemia
FL (femtoliters)
Normal
Macrocytic
Macrocytic Anaemia
A. MEGALOBLASTIC ANAEMIA
Vitamin B12 deficiency
Folate deficiency
Abnormal metabolism of folate and vit B12
B. Non megaloblastic anaemia
Liver disease
Alcoholism
Post splenoctomy
Neonatal macrocytosis
Stress erythropoiesis
Impaired production
(hypoproliferative)
Anaemia
Blood loss
(on the basis of cause)
(Haemorrhagic)
Increase destruction
(Haemolytic)
Reduced RBC Production
•
•
•
•
•
•
Stem cell defects
Nutritional deficiency
Erythropoietin deficiency
Hormone deficiency
Inhibitory effects of Cytokines
Unsuitable microenvironment
-
Aplastic anaemia
Fe deficiency anaemia
Chronic renal faliure
Hypothyroidism
Chronic diseases
Secondary deposits
Increased Loss
(Anaemia due to haemorrhage)
• Acute blood loss
• Chronic blood loss
Haemolytic
Anaemia
Inherited
Red cell
membrane
defects
Hb
abnormalities
Aquired
Metabolic
disorders of
RBC
immune
Non immune
Inherited haemolytic anaemia
1)Red cell membrane defects
Eg:
Hereditary spherocytosis
Hereditary Elliptocytosis
Hereditary Stomatocytosis
Eliptocytosis
Spherocytosis
Stomatocytosis
Inherited haemolytic anaemia
2)Hb abnormalities
Eg:
Thalassaemia
Sickle Cell Anaemia
Thalassaemia
Target cells
Sickle Cell Anaemia
Inherited haemolytic anaemia
3)Metabolic disorders of RBCs
Eg:
Glucose-6-phosphate
Dehydrogenase deficiency
Pyruvate Kinase deficiency
Aquired haemolytic anaemia
(Immune)
Eg:
Autoantibodies
Drug induced Antibodies
Allo Antibodies
Aquired haemolytic anaemia
(Non immune)
Eg:
MAHA – Micro Angiopathic Haemolytic
Anaemia(due to abnormal micro vessels)
Parasites – Malaria
Burns – Abnormal vessels
Malaria