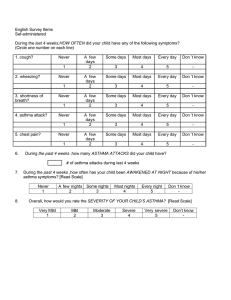
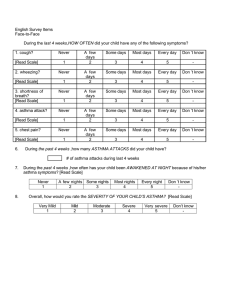
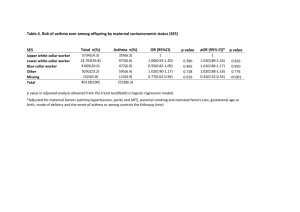
حساسية
advertisement

ASTHMA: DIAGNOSIS AND MANAGEMENT Asthma Clinical Quality Team NMCSD 2004 Burden of Disease General • 26 million adults and children in the USA have received a diagnosis of asthma sometime during their lifetime – 8.6 million were under 18 years of age • 10.6 million individuals experienced an asthmatic episode during the previous 12 months – 3.8 million were children • Hospitalizations increased 6.7% between 1988 and 1997 National Center for Health Statistics. Raw Data from the National Health Interview Survey, US, 1997-1998. (Analysis by the American Lung Association Best Practices Division, Using SPSS and SUDAAN software) Burden of Disease Death Rate, 1979 to 1997 1.8 1.6 Deaths per 100,000 Population Female Male + Female Male 1.4 1.2 1 0.8 '79 '80 '81 '82 '83 '84 '85 '86 '87 '88 '89 '90 '91 '92 '93 '94 '95 '96 '97 Year National Center for Health Statistics. Raw Data from the National Health Interview Survey, US, 1997-1998. (Analysis by the American Lung Association Best Practices Division, Using SPSS and SUDAAN software) Asthma definition • Inflammatory airways disorder involving mast cells, eosinophils, PMN’s, epithelial cells, macrophages and T cells. • This inflammation leads to clinical sequelae of episodic bronchospasm (wheezing), breathlessness, chest tightness and cough • Episodes are usually associated with variable airflow obstruction that is reversible Pathophysiology (inflammation) • Allergens (or other inciting agents) in the airway trigger local inflammation which exists chronically (multiple cell types) • Leads to airway hyperresponsiveness to various precipitants (cold air, exercise). • In addition to smooth muscle spasm, see mucosal edema and mucus hypersecretion of the airways Clinical presentation • Episodic wheezing, shortness of breath, coughing paroxysms • Often related to specific triggers (cold air, exercise, post-viral URI) • Patients will sometimes relate a history of frequent “bronchitis” as a child • Often have a personal or family history of atopic disorders (AR, asthma,eczema) Diagnosing asthma • Asthma is a clinical diagnosis. Historical and objective data must be combined to arrive at the diagnosis. • History: Cough, recurrent wheeze, SOB. Symptoms worsen with triggers such as allergen exposure, exercise, pollutants. Sx occur or worsen at night, resulting in awakening. • Physical exam: wheezing is not always asthma; asthma pts don’t always wheeze. Diagnosis • Objective lung studies: To document clinically suspected reversible airways obstruction, spirometry is used. There are 3 ways to document reversible obstruction. • (1) Spirometry, pre- and post- inhaled bronchodilator therapy (eg, albuterol) • (2) Spirometry before and after a course of sytemic or inhaled steroids. • (3) Bronchoprovocation studies Spirometry diagnosis • Classically, see a low FEV1 (amount of air expired in one second with maximal effort) with a decreased FEV1/FVC ratio (FVC is a rough measure of lung capacity) in an asthmatic with active disease. • To document asthma, must see a greater than or equal to 12% increase in FEV1 post bronchodilator or after a course of steroids. • Failure to see 12% increase or greater does not mean asthma excluded Bronchoprovocation • Bronchoprovocation studies include cold air challenge, histamine challenge, exercise challenge, and methacholine challenge. • All of these studies attempt to demonstrate the airway hyperresponsiveness seen in asthma. Useful in individuals where the diagnosis of asthma is uncertain. • Methacholine challenge done by inhaling increasing doses of the agent, then performing spirometry. Asthmatics will have a decline in their FEV1 and FEV1/FVC ratio after this challenge. Methacholine challenge • Looking for a drop of 20% or greater in FEV1 from baseline as a positive test. The dose that causes this drop is called the PD20. • The lower the PD20 dose, the more supportive the result is of asthma diagnosis. Generally, a PD20 of 8 mg/ml or less is considered positive. A higher PD20 could represent a false positive. • A negative full dose challenge is strongly suggestive that the patient is not asthmatic. Positive methacholine challenge at 5mg/ml dose Precipitating/sustaining factors for asthma • • • • • Allergen exposure Exercise Viral URI’s Rhinosinusitis GERD Viral respiratory infections • The vast majority (~80%) of acute asthma exacerbations are secondary to viruses • Most common agent is rhinovirus • Mechanism is poorly understood. Most plausible is that existing airway inflammation is up-regulated. • Frequent handwashing and routine influenza vaccination can prevent viralinduced asthma exacerbations. Allergen exposure • Estimated that 50% or so of asthmatics are atopic. In these individuals, allergens are believed to be a major driving factor in chronic inflammation. • Most significant are indoor allergens dust mite and cat. Also important in some environments is cockroach. Outdoor aller-gens can also sustain airway inflammation. • Elimination of indoor allergens mentioned above can result in disease improvement. Exercise-induced bronchospasm • Probably not a distinct disease entity, but rather a subset of asthma. • Those with symptoms exclusively during exercise are probably mild asthmatics who only get symptoms at the extremes of exertion. • Classically, see worst symptoms and airway obstruction 5 to 10 minutes after exercise. • Possibly due to cool,dry air inspiration that results in drying/irritation of bronchial mucosa GERD and asthma • GERD has been proposed by many authors as a chronic and acute driving factor for asthma, likely via a vagal reflex. • Role is controversial, but evidence mounting: perfusion of acid into the esophagus leads to an increase in cough response and increased airways hyperresponsivess. • Studies show medical treatment with PPI can improve asthma symptom control, but not objective lung studies (PEF,FEV1). Some studies suggest a 70% improvement in symptoms. • Fundoplication may provide even better results than medical management. GERD and asthma • Spivak et al (1999) looked at 39 pts who had fundoplication for GERD aggravating asthma. Sx improved overall, and 7 of 9 steroid dependent asthmatics able to d/c steroids • GERD is probably worth investigating in asthmatic who is on multiple meds, poorly controlled, and has no other driving factors. • Certainly, significant asthmatic with reflux symptoms should be started on empiric therapy Rhinosinusitis and asthma • NIH guidelines recognize an association between asthma and rhinosinsitis that was first noted hundreds of yrs ago • By unkown mechanism (neural?), inflammation of nose and sinuses appears to drive or worsen asthma in some individuals • Most marked in those with opacified/ infected sinuses. Curing the sinus/nasal disease often markedly improves the asthma. Rhinosinusitis and asthma • Rhinitis/asthma link supported by studies which show lower airway dynamics (FEV1, methacholine challenge) are affected by nasal allergen challenge. Also, exhaled lower airway NO (a marker of lower airway inflammation) is decreased by nasal steroid use. • 2002 Harvard Pilgrim study (Adams et al) of all asthmatics in a managed care organization over a 5 year period. Regular use of nasal steroids reduced ED visits for asthma by 30-50%, depending on rate of use. Asthma classification • NIH guidelines classify asthmatics into 4 groups based on severity • Classification is important for physician communication and so appropriate therapy can be used based on published guidelines. • NHLBI/NIH guidelines for the diagnosis and management of asthma available online: www.nhlbi.nih.gov/guidelines/asthma Classification of Asthma Severity: Clinical Features Before Treatment Step 4 Days With Symptoms Continuous Nights With Symptoms Frequent PEF or FEV1 60% PEF Variability 30% Severe Persistent Step 3 Daily 5/month 60%-<80% 30% Moderate Persistent Step 2 3-6/week 3-4/month 80% 20-30% Mild Persistent Step 1 2/week 2/month 80% Mild Intermittent Footnote: The patient’s step is determined by the most severe feature. 20% Stepwise Approach to Therapy for Adults and Children >Age 5: Maintaining Control STEP 4 Multiple long-term-control medications, include oral corticosteroids STEP 3 > 1 Long-term-control medications STEP 2 1 Long-term-control medication: anti-inflammatory STEP 1 Quick-relief medication: PRN Step down if possible Step up if necessary Patient education and environmental control at every step Recommend referral to specialist at Step 4; consider referral at Step 3 Asthma therapy • One goal of asthma therapy is to prevent symptoms that limit activity and/or result in missed school/work days • Avoid hospitalizations/ER visits • Avoid asthma deaths (3,000 - 5,000/year) • Another goal: Prevent “unchecked” inflammation that may lead to airway remodeling and irreversible damage Asthma therapy • Obvious triggers, drivers of the airway inflammation should be treated and/or avoided if possible. • Treat sinusitis, GERD. • Full physical activity should not be discouraged. • Allergen avoidance may be useful adjunct to meds (for identified indoor allergens). Pharmacotherapy (long-term control meds) • • • • Inhaled steroids Long-acting beta agonists Anti-leukotriene agents Theophylline Mild intermittent • NIH guidelines dictate that patients may be treated with prn bronchodilators as long as symptoms continue to occur two or less times weekly and spirometry is normal (at baseline) Mild persistent • Most easily remembered as patients with symptoms more than twice weekly (but not daily) who have normal baseline spirometry • Require anti-inflammatory medication • Vast majority of experts/clinicians use inhaled steroids as first line. • Some advocate use of anti-leukotrienes Mild persistent • Concern is that anti-LT drugs only attack one arm of the inflammatory process, while inhaled steroids have broader activity. So steroids preferred. • Low dose inhaled steroids (e.g., Flovent 44 mcg/puff 2 puffs BID or Azmacort 4 puffs BID) usually sufficient in this group. • If not controlled with the above, pt is behaving more like a moderate persistent patient Moderate persistent • Patient with daily symptoms/need for albuterol, or baseline FEV1 60-80% pred • Three choices at this point: • (1) Going from low to medium dose steroids (eg, Flovent 110 2 puffs bid) • (2) Add a long-acting bronchodilator • (3) Add an anti-leukotriene agent (eg, Singulair) All are reasonable options. Which is correct? Moderate persistent • Studies suggest that if pt not controlled on this, adding Serevent is the next best option (Busse et al, 1999: Kelsen et al, 1999). This is reflected in recently updated NIH guidelines, where the addition of a longacting B-agonist is recommended prior to using higher dose inhaled steroids or leukotriene receptor antagonists. • Therefore, option 2 is the most correct choice. Long-acting beta agonists (Serevent) • If needed, these agents should only be used in conjunction with an anti-inflammatory medication (act synergistically). • Serevent is available in combination with Flovent as Advair (100/50, 250/50, or 500/50). • Therapy with Serevent alone may just be bronchodilating without any effect on the underlying inflammation. This can result in undesirable clinical outcomes. Severe persistent • These are pts with contiual sx, baseline FEV1 under 60%, frequent nighttime awakenings, multiple hospitalizations and intubations. • Need high dose inhaled steroid,Serevent, and possibly Singulair as well. • Theophylline, and finally oral steroid may be needed to fully control such patients. • A detailed investigation for causes of difficult to treat asthma should be undertaken Monitoring asthma therapy • Patient self-reporting of asthma symptoms is variably reliable in assessing control. • Important sx: exercise tolerance, nighttime awakenings, prn albuterol use, missed school/work days • NIH guidelines suggest that objective monitoring (periodic peak flow and/or spirometry) should be performed at regular intervals. This data should be combined with patient symptoms to direct therapy. Monitoring asthma • Spirometry should be repeated at least every 1 to 2 years to assess the maintenance of airway function (NIH guidelines). • Peak flow meter use is recommended for moderate and severe asthmatics, especially those who perceive obstruction poorly. • Patients should be given instructions on how to proceed depending on peak flow results (asthma action plan). Written asthma action plans specifically have been shown to improve outcomes. The Effect of a Peak Flow-Base Action Plan • 150 asthmatics randomized to 1 of 3 groups – No action plan – Symptom-based plan – Peak flow-based plan • All received asthma education No plan # urgent care visits #admissions 55 12 PF plan 5 2 Symptom plan 45 6 Cowie RL, et al. Chest 1997;112:1534-38 Peak Flow & Symptom-Based Home Action Plan Managing exacerbations in ED • Supplemental O2. Repeat albuterol/atrovent nebs (3). The practice of adding atrovent to albuterol improves outcomes • If exacerbation initially seems severe, or pt not responding, systemic steroids are indicated (several hour effect time). • Magnesium use is controversial – little evidence of effect except possibly in very severe exacerbations • If impending or actual respiratory failure occurs, pt may require intubation first. • If patient fails to improve (doesn’t reach 70% of predicted or best PEF as a general guideline), hospitalization needed. High dose systemic steroids and frequent nebs the usual treatment course, with slow taper of steroids as an outpatient.