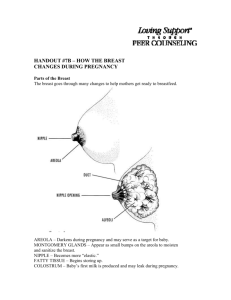
Breast inflammatory lesion
advertisement

A: Mammogram of young women – dense white (opaque) B: Young women’s breast – density due to fibrous interlobular stroma & paucity of adipose tissue C: During pregnancy – undergo lactational changes D: Old women’s breast – small ducts & atrphic lobules in adipose tissue E: Mammogram – more radiolucent in elder’s breast Enumerate different types of inflammatory breast lesions. Enumerate the causes of inflammatory breast lesions. Describe clinical picture and management of inflammatory breast lesion. Describe the differentiation of the inflammatory breast lesion from breast cancer. Uncommon – less than 1% of women with breast symptoms- 1- Acute Mastitis 2- Periductal Mastitis. 3- Mammary Duct Ectasia (plasma cell mastitis). 4- Traumatic fat necrosis. Systemic Breast Disease 5- Lymphocytic Mastopathy (autoimmune basis- scelrosing lobulitis) 6- Granulomatous Mastitis \ 7- Radiation Cuases - Infectious agents: 1- Staph – localized area,single or multiple abscesses Acute inflammation, usually small-start at one duct Occasionally large abscess – heals by palpable scar. 2- Strep – generally spread to entire breast Pain, marked diffuse, spread of infection, swelling and tenderness Resolution rarely leaves areas of indurations. Access of bacteria to the breast 1-Through ducts- start at one duct, then spread. 2- Fissures in nipple- lactation or nipple dermatitis. is known as, subareolar abscess, squamous metaplasia of lactiferous ducts, Zuska disease. 1)Vitamin A deficiency in associated with toxic substances in tobacco smoke or smoking ↓↓ Altere the differentiation of ductal epithelial Note:- Not association with lactation Histologic feature is keratinizing squamous metaplasia of the nipple ducts, chronic granulomatous response to keratin, +\- bacterial infections occur in the 5th or 6th decade of life, in multiparous women Chronic mastitis (non-bacterial) - inspissation of secretions in main excretory ducts Morphology: Ductal dilatation (ectasia) with ductal rupture. Dilated ropelike ducts with thick cheesy secretions Reactive changes in the surrounding breast tissue+ calcification (nipple retraction and palpable mass). Ducts filled by granular debris, sometimes containing WBCs mainly fat-laden macrophage (nipple discharge) The striking feature is prominent lymphocytic and plasma cell infiltration with occasional granulomas Mistaken for carcinoma by– retraction of overlying skin or nipple, palpable mass (even on mammogram)- nipple discharge- calcificaftion Define as foamy macrophages infiltrating partially necrotic adipose tissue- involve adipose tissue, occ. parenchyma Traumatic fat necrosis: A) Post-traumatic fat necrosis, often in pendulous large breast (1-2 WEEKS) B) Prior surgery - Central necrotic fat cells surrounded by PMNs & mononuclear infiltrates and fatladen macrophages. - This is enclosed later by fibrous tissue and Replaced by scar tissue or cyst + Calcification. - Skin retraction Probably immune-mediated pathogenesis (Autoimmune diseases- e.g.):- a) Type 1 (insulin-dependent) diabetes mellitus. b) Autoimmune thyroid disease Microscopy: -Diffuse dense lymphocytic infiltrates. (lobules& Small blood vessels) - Lobular atrophy.- Sclerosis: collagenized stroma surrounding atrophic ducts and lobules. - The epithelial basement membrane is thickened. Immune-mediated pathogenesis, can simulate malignancy in presentation.= (granulomatous lobulitis) 1- Systemic granulomatous diseases (e.g., Wegener granulomatosis, SLE, amyloidosis or sarcoidosis). 2- Infections- (e.g. mycobacteria or fungi, actinomycosis, Histoplasmosis)- common in immunocompromised patients. 3 4- Foreign objects such as breast prostheses. Hypersensitivity reaction to antigens expressed by lobular epithelium during lactation (Granulomatous lobular mastitis )- uncommon. 1- Mastitis – development of cracks and fissures in the nipples, erythematous and painful, and fever single or multiple abscesses. 2- Periductal Mastitis- painful erythematous subareolar mass+ a fistula tract of the smooth muscle of the nipple and opens onto the skin 3- Mammary Duct Ectasia (plasma cell mastitis). poorly defined palpable periareolar mass,+ a\w thick, white nipple secretions and sometimes with skin retraction + No pain or erythematous 4- Traumatic fat necrosis- painless palpable mass, skin thickening or retraction, a mammographic density or calcifications. 5- Lymphocytic Mastopathy- LOBULAR (autoimmune basis), single or multiple hard palpable masses, may be bilateral, so hard lesion. 6- Granulomatous Mastitis- immunocompromised patients or adjacent to foreign objects + hypersensitivity reaction Diagnosis: clinical examination, US, MG, FNAC, tissue biopsy Management: according to the type and etiology Acute mastitis, Mammary duct ectasia and breast abscess A)- ;Frequent nursing and massaging of the breast(keep it empty) B) - Appropriate antibiotics. C) Incision and drainage. Fat necrosis A) Using warm compresses B) Analgesics (ibuprofen,aspirin) C) FANC drainage of oil d) Lumpectomy if mass persist. LYMPHOCYTIC MASTOPATHY Surgery (often recur) Granulomatous mastitis systemic antibiotics, anti TB, steroids, immunosuppressive methotrexate, surgery Age, sex, clinical presenting symptoms, signs& durations. Nipple bloody discharge, Nipple pain. Examination Breast findings: mass (localized, involve X quadrants, size), firm\hard, with irregular margins Skin: irritation, dimpling, redness, pseduo-orange, ulcer. Nipple:retraction, Corresponding depression, irritations, redness scaling. axilla- enlarged lymph nodes, accessory. Examination of other breast Asymmetrical & distortion Breast ca- skin changes A: Mammogram of young women – dense white (opaque) B: Young women’s breast – density due to fibrous interlobular stroma & paucity of adipose tissue C: During pregnancy – undergo lactational changes D: Old women’s breast – small ducts & atrphic lobules in adipose tissue E: Mammogram – more radiolucent in elder’s breast Supernumerary nipples or breast: Mildline remnants – extends from axilla to perineum Axillary breast: Normal ductal system extends into chest wall & axilla. Congenital Nipple Inversion: Failure to evert during development, may be unilateral; may be confused with acquired causes that may give rise to inversion sometimes – like in cases of invasive breast cancer or inflammatory diseases of nipple (recurrent subareolar abscess or duct ectasia). Macromastia: One cause is an unusual tissue response to hormonal changes during puberty massive rapid breast growth (Juvenile hypertrophy)