Nursing Care of the Child with
GU disorders
External Defects in the Urinary
System
Extrophy of the bladder
Hypospadias vs epispadius
Cryptorchidism
Extrophy of the bladder
Posterior bladder wall
extrudes through the
lower abd wall.
Failure of the abd to
close
Pre-op focus of nsg
care
– Prevent trauma
– Prevent infection of
exposed
bladder
Post-operative care with surgical
care of extrophy of bladder
Care of the surgical
site with meticulous
wound care
Positioning:
immobilization and
avoidance of
abduction of legs
Neurovascular
assessment of lower
extremities
Monitoring renal
function and
obstruction of tubes
Promoting comfort
Discharge teaching
Hypospadias vs Epispadias
Hypospadias
– Congenital urethral
defect
– Uretheral opening
on VENTRAL (lower)
aspect of the penis
Epispadias
– Congenital urethral
defect
– Urethral opening is
on the DORSAL
aspect of the penis
Treatment for hypospadias
DO NOT circumcise infant; may need
the foreskin for reconstruction
Surgery: reconstructive to reposition the meatus at the tip
Usually done before one year of age
Post-op care:
Post-op management
Care of the catheter (may be foley,
suprapubic or urethral stent.
Use double diapering
Management of bladder spasms
Prophylactic abx
No bath until stent removed
Increase fluid intake
No play on straddle toys
Call physician for temp > 101º
Cryptorchidism
Therapeutic interventions for
cryptorchidism
Orchiopexy done via laproscopy
Nursing care post-op:
– Minimal activity for few days
– Allow opportunity to express fears about
mutilation or castration
Critical thinking for client
undergoing urinary tract surgery
David is 5 years old and scheduled for ureter
reimplantation surgery. In addition to discussion
of post-op pain, tubes and dressings, the most
significant other topic would be which of the
following?
– A. Need to reassure David his genitals are
intact and will function normally when the
catheters are removed
– B. Importance of monitoring the urine
drainage from stents and urethral catheter
– C. The need to assess the surgical site for
bleeding or excessive drainage
– D. The home care regimen that can be
anticipated when David is discharged
Obstructive Uropathy
Stenosis of uteropelvic valve
Stenosis of posterior urethral valve
Stenosis of the uterovesicular
junction otherwise known as
“vesicoureteral reflux”
Hydronephrosis the main problem
with reflux of urine
What is vesicoureteral reflux?
Therapeutic management
Corticosteroids (prednisone)
Dietary management
Restriction of fluid intake
Prevention of infections
Monitoring for complications:
infections, severe GI upset, ascites,
or respiratory distress
Physiologic changes r/t
hydronephrosis
Cessation of glomerular filtration and
cell death
Metabolic acidosis result
Impairment of kidney’s ability to
concentrate urine
Obstruction results in stasis and
infection
Can lead to chronic renal failure
Diagnostic tests for renal/bladder
function
Urine culture and
sensitivity: done
every 2-3 months
VCG: voiding
cystourethrogram
Renal/bladder
ultrasound
IVP
Renal biopsy
Cystoscopy
Nursing responsibilities with testing
Responsible for preparation and
collection of urine or blood
Maintains careful intake and output
Recognizes that renal disease can
diminish the glomerular filtration
rate(the amt of plasma from which a
given substance is totally clear in
one minute)
Treatment for vesicoureteral reflux
Directed toward preventing UTIs
Managed by time or surgery if a
lower grade
Single doses each day of abx as long
as reflux lasts
Urine cultures done q 6 wks up to 3
months to make sure no “silent
infection”
Treatment and nsg care for
obstructive uropathy
Drug therapy
– Penicillin
– Cephalosporins
– Urinary antiseptics
(Furadantin)
Surgery:
– Repair of anatomical
anomalies/pyeloplasty
Follow up VCG after
few months post op
Nsg care:
– Teach prevention of UTI
– Teach imp of taking all
abx
– Monitor urinary
drainage from catheters
– Assess for pain
– Teach parents how to
change dressings,
double-diaper
– s/s obstruction or
infection
Differences between adult s/s UTI
and pediatric patient
In children:
– Unexplained fever
– Failure to thrive
– Vomiting
– Diarrhea
Urinary tract infections
Most common type of bacterial
infections occurring in children
Bacteria passes up the urethra into
the bladder
Most common types of bacteria are
those near the meatus…staph as well
as e.coli
Contributing factors
Those with lower resistance,
particularly those with recurrent
infections
Unusual voiding and bowel habits
may contribute to UTI in children
“forget to go to bathroom”
Symptoms:
Therapeutic management
Eliminate the current infections
Identify contributing factors to
reduce the risk of re-infection
Prevent systemic spread of the
infection
Preserve renal function
FYI
The single most important host
factor influencing the occurrence of
UTI is urinary stasis
What is the chief cause of urinary
stasis?
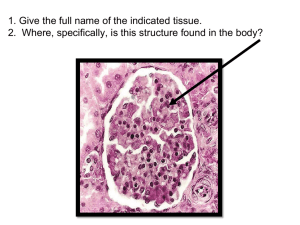
Nephrotic syndrome
Nephrotic syndrome, cont
Child with nephrotic syndrome
Treatment of nephrotic syndrome
Varies with degree of severity
Treatment of the underlying cause
Prognosis depends on the cause
Children usually have the “minimal
change syndrome” which responds
well to treatment
Nursing interventions to manage
nephrotic syndrome
Administer corticosteroids
(prednisone) as ordered
Dietary management
Restriction of fluid intake
Prevention of infections
Monitoring for complications:
infections, severe GI upset, ascites,
or respiratory distress
Glomerular diseases
Acute glomerulonephritis (AGN)
Nephrotic syndrome (MCNS) or
minimal-change nephrotic syndrome
AGN
Immune-complex disease causing
inflammation of glomeruli of kidney
Usual organism is group A betahemolytic strep
Decreased glomerular filtration
Common in children (boys > girls)
Assessment/diagnostic tests:
AGN
Treatment and nursing care:
Bed rest may be recommended during
acute phase
Record of daily weight is the most useful
means for assessing fluid
balance
Nursing diagnosis for the child with
glomerulonephritis
Fluid volume excess r/t to…
Activity intolerance r/t….
Altered patterns of urinary
elimination r/t …
Altered family process r/t…
Nursing care specific to the child
with AGN
Allow activities that do not expend
energy
Diet should not have any added salt
Fluid restriction, if prescribed
Monitor weights
Education of the parents
 0
0