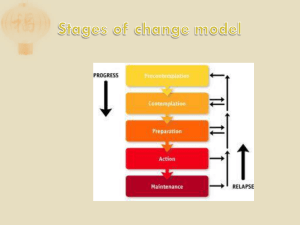
PDA Software for Patients - Faculty Virginia
advertisement

Innovative Approaches to Smoking Cessation Treatment Scott M. Strayer, MD, MPH Associate Professor University of Virginia, Dept. of Family Medicine Center for Information Mastery UVA Cardiology Grand Rounds, Feb 2008 Copyright© 2008 Scott Strayer Objectives • • • • • Review evidence-based smoking cessation guidelines and preview of 2008 guidelines to be published on May 1 Describe the latest evidence for treatments during smoking cessation, including the use of tricyclic anti-depressants in adults and patches in adolescents. Be able to describe the key components of “Motivational Interviewing” and the “Stages of Change” and how they are used in smoking cessation counseling. Identify web-based and computer resources that assist physicians with smoking cessation counseling. Identify web-based and computer resources that assist patients with smoking cessation. How well do we address smoking cessation? • Not very well!! – Only 35% of Physicians assist with smoking cessation attempts (Thorndike AN, Rigotti NA, Stafford RS, Singer DE. National patterns in the treatment of smokers by physicians. JAMA 1998; 279:604-608). Am J Public Health. 2007 Oct;97(10):1878-83. Epub 2007 Aug 29. The treatment of smoking by US physicians during ambulatory visits: 1994 2003. Thorndike AN, Regan S, Rigotti NA. Smoking Cessation is Effective! • Quitting at age 50, adds 6 years of life expectancy, quitting at 30 adds up to 10 years1 • Colorectal cancer screening adds 7.3 to 21.9 days of life depending on strategy2 • Mammography adds 9.8 days for women 60-69 and 11.7 days for women 50-593 1 Doll R, Peto R, Boreham J, Sutherland I. Mortality in relation to smoking: 50 years' observations on male british doctors. BMJ. 2004;328:1519. 2 Frazier AL, Colditz GA, Fuchs CS, Kuntz KM. Cost-effectiveness of screening for colorectal cancer in the general population. JAMA. 2000;284:1954-1961. 3 Kattlove H, Liberati A, Keeler E, Brook RH. Benefits and costs of screening and treatment for early breast cancer. development of a basic benefit package. JAMA. 1995;273:142-148. Examples in Cardiology Pignone M, Eamshaw S, Tice J, Pletcher M, Aspirin, Statins, or Both Drugs for the Primary Prevention Of Coronary Heart Disease Events in Men: A Cost-Utility Analysis. Ann Intern Med. 2006; 144:326-336 Explaining Declining CHD in England Unal B, Chitchley J, Capewell S, Explaining the Decline in Coronary Heart Disease Mortality in England And Wales Between 1981 and 2000 Circulation. 2004;109:1101-1107. What We Know… New Guidelines will be released in May 2008 • Tobacco dependence is a chronic condition that often requires repeated intervention. • Because effective tobacco dependence treatments are available, every patient who uses tobacco should be offered at least one of these treatments. • It is essential that clinicians and health care delivery systems (including administrators, insurers, and purchasers) institutionalize the consistent identification, documentation, and treatment of every tobacco user seen in a health care setting. • Brief tobacco dependence treatment is effective, and every patient who uses tobacco should be offered at least brief treatment. • There is a strong dose-response relation between the intensity of tobacco dependence counseling and its effectiveness. • Three types of counseling and behavioral therapies were found to be especially effective and should be used with all patients attempting tobacco cessation: • Provision of practical counseling (problem solving/skills training). • Provision of social support as part of treatment (intra-treatment social support). • Help in securing social support outside of treatment (extra-treatment social support). • Numerous effective pharmacotherapies for smoking cessation now exist. Except in the presence of contraindications, these should be used with all patients attempting to quit smoking. • Five first-line pharmacotherapies were identified that reliably increase long-term smoking abstinence rates: • Bupropion SR. • Nicotine gum. • Nicotine inhaler. • Nicotine nasal spray. Nicotine patch. • Two second-line pharmacotherapies were identified as efficacious and may be considered by clinicians if firstline pharmacotherapies are not effective: • Clonidine. • Nortriptyline. • Over-the-counter nicotine patches are effective relative to placebo, and their use should be encouraged. New Medications Since Guidelines Published • There are now 7 first-line medications – Nicotine Lozenges – Varenicline • Others are under development – Nicotine Vaccines---currently in Phase 2 and 3 trials New Drug Information for 2008 Guidelines Combination Therapies in 2008 Guidelines Caution with Varenicline • Post-marketing suicides (39), erratic behavior, mood changes (420) and sedation during medication use – Not all had quit smoking – Not all had previous psychiatric dz • Ongoing safety review at FDA • Close f/u, warn patients about possible side effects, caution with psychiatric patients Current FDA Warning • Tobacco dependence treatments are both clinically effective and costeffective relative to other medical and disease prevention interventions. New Counseling Interventions for 2008 Guidelines • Use of proactive telephone counseling (OR of quitting=1.6 [1.4,1.8], abstinence rates 12.7%, meta-analysis of 9 studies vs. minimal, no counseling or self-help) • Emphasis on counseling + meds • More on motivational treatments • Calls for innovative and more effective counseling strategies Is It Possible? • To deliver all the preventive services recommended by the USPTF to an average panel of patients, family physicians would need to spend 7.5 hours of every working day on prevention alone… Yarnell KS, Pollac KI, Ostbye T, Krause KM, Michener JL. Primary care: is there enough time for prevention? AM J Public Health 2003;93:635-41. Leveraging 1 Minute for Prevention 1 minute is the realistic average amount of time that primary care providers can devote to prevention during a typical office visit Stange, KC, Woolf, SH, Gjeltema K. One minute for prevention: The power of leveraging to fulfill the promise of health behavior counseling. Am J Prev Med, 2002; 22:320-323. Opportunities for Intervention • Most people visit their doctor about three times per year. • Even 2-3 minute interventions are effective, especially when followed up with telephone, e-mail, nurse calls, referrals, 1-800 numbers, etc. • Many primary care providers provide 2-3 minute health promotion/behavior interventions at every outpatient visit. Stange, KC, Woolf, SH, Gjeltema K. One minute for prevention: The power of leveraging to fulfill the promise of health behavior counseling. Am J Prev Med, 2002; 22:320-323. The other elements of brief health promotion • • • • Goal setting Specific Behavior Change Techniques Self-help Materials Regular Follow-up In the 1 minute devoted to preventive/behavioral issues, the doctor can either “plant the seed” for Interactive Behavioral Change Technology (IBCT) to cultivate after the visit, or “reap the fruit” of IBCT interventions that have taken place prior to the visit. Glasgow R, Bull S, Piette J, Steiner J. Interactive behavior change technology: A partial solution to the competing demands of primary care. Am J Prev Med 2004; 27:80-87. Glasgow R, Bull S, Piette J, Steiner J. Interactive behavior change technology: A partial solution to the competing demands of primary care. Am J Prev Med 2004; 27:80-87. Effective Behavioral Change Theories • Stages of Change----assess patient’s readiness to change and then deliver stage-appropriate interventions (Prochaska and DiClemente) • Motivational Interviewing (MI)---a nonconfrontational, patient-centered technique for helping patients change their health behavior (Miller and Rollnick) Stages of Change • Pre-contemplation-pt is not ready to initiate change. • Contemplation-pt is considering making change in next 6 months. • Preparation-pt is ready to make change in 30 days. • Action-pt is making change. • Maintenance-pt has made change. Assess • Are you thinking about quitting in the next 6 months? (No=Precontemplation) – If YES – Are you thinking about quitting in the next 30 days? (No=Contemplation, Yes=Preparation) • How important do you think it is for you to quit smoking? • How confident are you that you could quit smoking if you wanted to? Overview of MI • Directive, patient-centered counseling • Focus on user’s feelings, beliefs, ideas and values about using tobacco • Attempt to uncover ambivalence about tobacco use • Then elicit supports and strengthen “change talk” and “commitment talk” Techniques for MI • Precontemplation – Pros and cons of smoking – Personalizing risks – Re-assess after intervention • Contemplation – How long have they been considering? – What has worked in the past (if quit before)? – Pros and cons of quitting – Personalize risks and rewards Techniques for MI • Preparation – Clarify goal (quit entirely, cut down) – Get input on patient’s plans on how to do it – Discuss a “change plan”---use of medication, start date, what’s gone wrong in the past and how to avoid these things this time, social support – Summarize and next steps Techniques for MI • Action – IF patient has had a “slip” identify reasons and strategies for avoiding (e.g. cues, selfefficacy, assess confidence) – If no slips • Support self-efficacy (e.g. elicit confidence talk, personal strengths and supports, brainstorming, how will things be different?) • Refine or adjust action plan • Discuss coping skills (identify smoking triggers and ways of dealing with them) MI with Patient Motivational InterviewingDARES • Develop Discrepancy-between patient’s current behavior and their goals e.g. “It sounds like you are very devoted to your family, how do you think your smoking is affecting your children?” • Avoid Argumentation • “Roll with Resistance” • Express Empathy-use open-ended questions and reflective listening • Support Self-Efficacy-help patient identify and build on past experiences The 5 R’s of Motivational Interventions (NOT Interviewing) • Risks-have patient identify risks of smoking • Rewards-have the patient identify rewards of quitting • Relevance-how is quitting relevant to the patient and their dz status or risk, family or social situation • Roadblocks-barriers or impediments to quitting • Repetition-repeat at every visit Training in Motivational Interviewing • Motivational Interviewing Network of Trainers (MINT) • Motivational Interviewing by Miller and Rollnick Integrating the Behavioral Theories Programs for Physicians • Modular Lifestyle Intervention Tool (MLIT) (http://www.prescriptionforhealth.org/too lkit/index.html) • Calculators (www.statcoder.com and http://hin.nhlbi.nih.gov/atpiii/atp3palm.htm) • C-Tools 2.0 (http://www.cancer.org/docroot/COM/content/ div_TX/COM_5_1x_The_CTools_20.asp?SiteArea=) • Websites Development of the MLIT • • • • • • • Operationalize the Stages of Change Identify stage based interventions Scripted motivational interviewing Risk calculators Pharmacotherapy info Local and national resources Modular design Evaluation of MLIT • Pilot study (n=17) • VAPSRN academic physicians • Pretest Posttest survey (46 items) – Behavior – 5 A’s, TTM, MI, Rx – Comfort/Self-efficacy – Knowledge – TTM, PHS, OEI – Adapted from prior work • Intervention = MLIT on handheld with encouragement of use • Four month period Results: Counseling behaviors • More likely to advise patients to stop smoking (p = 0.049) • Increased overall use of the "5 A's" during patient encounters for smoking cessation (p = 0.031) • Increased general counseling behaviors – frequency of counseling, provision of behavior specific information, and use of pharmacotherapy and referrals for both smoking cessation (p = 0.047) Results: Comfort and Selfefficacy • Improved self-efficacy in counseling patients regarding smoking cessation (p = 0.006) • Increased comfort in providing follow-up to help patients sustain their efforts at smoking cessation (p = 0.042) Results: Knowledge • There was no change in physician knowledge either overall or within the four domains – stages of change classification – appropriate stage-based interventions – knowledge of PHS smoking cessation guidelines Technology Development • Silverchair’s staff adapted our platforms to create an IT Ecosystem: Technology Development C-Tools • Download at cancer.org (search on ctools) • Guidelines for smoking cessation • Pharmacotherapy Information • Websites • Quitline numbers InfoRetriever to help with treatment decisions • A 46 y/o male, smoker – PMH significant for hypertension treated with HCTZ. Most recent BP = 138/86. – FH: Both parents have HTN over age 70, no h/o CAD. – Lipids: Chol = 197; HDL = 41; LDL = 141. • Questions: – What is his risk of an AMI or sudden cardiac death in the next 10 years? – How much will lowering the SBP below 130 reduce the risk? – How much will stopping smoking affect his risk? Should his SBP be lowered to <130? What if he quit smoking instead? What if your patient asks about? • Smoking Cessation Quitlines – 1-800 QUIT NOW, available to all Virginians 18 and older, fax referrals coming soon • • • • Accupuncture Hypnotherapy Tricyclics Is the patch effective in adolescents? Websites for Physicians • Treating Tobacco Use and Dependence (http://www.surgeongeneral.gov/tobacc o/default.htm) • NCI website (www.smokefree.gov) • American Cancer Society (www.cancer.org) • American Lung Association (www.lungusa.org) Programs for Patients PinnacleHealth Hospitals Grand Rounds 2005 Copyright© 2005 Scott Strayer RWJ MyHealthyLiving Website • www.pubinfo.vcu.edu/myhealthyliving/ • Other RWJ resources (http://www.prescriptionforhealth.org/too lkit/index.html) American Cancer Society • www.cancer.org/quittobacco • Online resources for patients and providers • Localized resources • Tobacco Cessation Leadership Institute (UCSF) American Lung Association • Patient Resources • Freedom From Smoking Online Summary • Discussed evidence-based guidelines for smoking cessation counseling and treatment • Discussed MI and Stages of Change for counseling • Resources for physicians and patients