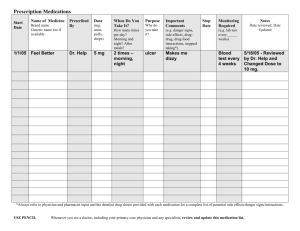
Medications. The nurse's role in dispensing, compounding and
advertisement

Medications The nurse’s role in dispensing, compounding and administering medications in British Columbia College of Registered Nurses of British Columbia 2855 Arbutus Street Vancouver, BC Canada V6J 3Y8 T: 604.736.7331 F: 604.738.2272 Toll-free: 1.800.565.6505 MEDICATIONS This document provides supplementary information and should be read in conjunction with the Scope of Practice for Registered Nurses: Standards, Limits and Conditions, Medication Administration Practice Standard Dispensing Medications Practice Standard Medication Inventory Management Practice Standard CRNBC resources referred to in this document as well as additional information on this topic are available from the CRNBC website www.crnbc.ca 2855 Arbutus Street Vancouver, BC V6J 3Y8 Tel 604.736.7331 or 1.800.565.6505 www.crnbc.ca Copyright CRNBC/Dec 2015 Pub. No. 3 College of Registered Nurses of British Columbia 2 MEDICATIONS Table of Contents L e gi sla t i on Legislation Affecting CRNBC Registrants and the Medication Process 4 4 Provincial 4 Federal 4 Administering Drugs With and Without an Order C on tr ol s on P r a c t ic e Examples of controls on practice applied to the medication process Or der s 5 6 7 8 Verbal/Telephone Orders 9 Pre-printed Orders 9 Abbreviations 9 Unacceptable Orders 9 Using Technology to Transmit Orders 9 P r e scr ib in g 10 C o mp o un d in g 10 D is p e n s in g 10 M ed i ca ti on I n v en to r y M a n a g e m en t 10 D r u g S ub s ti t u t io n b y P h a r ma c i st s 11 Ad m in is t er in g 11 Off-Label Medications 12 Investigational (Experimental) Medications 12 Narcotics and Controlled Drugs 12 Placebos 12 Complementary and Alternative Therapies 13 Withholding Medications 13 Administration by Others – The RN Role 13 R ol e o f th e C R N B C - C er ti fi e d P r a c t ic e R N 14 D oc u m en ta t i on 15 Medications Not Given 15 Medications Given by Other Staff 15 M ed i ca ti on S a fe ty 16 Medication Errors 16 R e so ur c es f or N ur s es College of Registered Nurses of British Columbia 17 3 MEDICATIONS Legislation LEGISLATION AFFECTING CRNBC REGISTRANTS AND THE MEDICATION PROCESS Provincial Nurses (Registered) and Nurse Practitioners Regulation Outlines the restricted activities of compounding, dispensing and administering Schedule I, IA and II drugs assigned to registered nurses. Drug Schedules Regulation Classifies drugs by categories called drug schedules Federal Controlled Drugs and Substances Act and Regulations Directs facilities licensed under the Hospital Act to maintain a count of narcotics, controlled drugs and medication wastage. College of Registered Nurses of British Columbia 4 MEDICATIONS ADMINISTERING DRUGS WITH AND WITHOUT AN ORDER B.C. PROVINCIAL DRUG SCHEDULES RN administers drugs following nursing diagnosis of a condition RN administers drugs following diagnosis of a disease or disorder Schedule I drugs require a prescription from an authorized health professional. with order with order Example: RNs require an order for antibiotics (Schedule I). Example: RNs require an order for antibiotics (Schedule I). Example: The Nurses (Registered) and Nurse Practitioners Regulation specifies certain conditions RNs may treat with Schedule I medications without an order. Example: RNs with CRNBC-Certified practices may give specific Schedule I medications without an order Schedule IA drugs in the Controlled Prescription Program. with order with order Example: RNs require an order Example: RNs require an order for narcotics (Schedule IA). for narcotics (Schedule IA). Schedule II drugs do not require a prescription, but are kept in an area of the pharmacy where there is no public access or opportunity for patient self-selection. without order with order Example: After assessing and diagnosing chest pain (a condition), RNs may administer sublingual nitroglycerin (Schedule II) without an order to treat the condition. Example: RNs require an order for insulin (Schedule II) for diabetes (a disease or disorder) or heparin (Schedule II) for a deep vein thrombosis (a disease or disorder). Schedule III drugs may be sold by a pharmacist from the selfselection area of the pharmacy. without order with order Example: After assessing and diagnosing uncomplicated pain (a condition), RNs may administer acetaminophen to treat the condition. Example: RNs require an order to administer cimetidine for a peptic ulcer (a disease or disorder). College of Registered Nurses of British Columbia 5 MEDICATIONS Controls on Practice The Nurses (Registered) and Nurse Practitioners Regulation sets out a broad scope of practice. Nursing practice is further controlled by: CRNBC – sets standards, limits and conditions Employer policies – may further restrict an activity in an agency or unit but cannot broaden scope Individual competence – nurses require the knowledge, skill, attitude and judgment to carry out the activity All four levels of control are necessary for nurses to provide safe, competent and ethical care. Each level successively narrows a nurse’s practice. For example: Schedule II, III and unscheduled medications do not require a prescription and a nurse may be competent to administer the medication, but agency policy may require an order before a nurse can administer these medications. A nurse may give a Schedule III or unscheduled medication after assessing and diagnosing a condition, but requires an order to give the same medication to treat a disease or disorder. College of Registered Nurses of British Columbia 6 MEDICATIONS EXAMPLES OF CONTROLS ON PRACTICE APPLIED TO THE MEDICATION PROCESS Application to the Medication Process Regulation RNs may compound, dispense or administer by any method a Schedule I or IA drug with an order (Section 7). An ER nurse gives Diazepam 5 mg. IV (Schedule I) to an adult with severe anxiety following a doctor’s order. RNs may compound, dispense or administer by any method a Schedule II drug without an order (Section 6). A residential care RN gives a nitroglycerin sublingual tablet (Schedule II) to a client who complains of chest pain. RNs may dispense or administer a Schedule I drug without an order for the purpose of treating: - anaphylaxis - hypoglycemia Standards, Limits, Conditions Example Parts 2 and 3 in CRNBC’s Scope of Practice for Registered Nurses: Standards, Limits and Conditions CRNBC Practice Standards Medication Administration, Dispensing Medications, Medication Inventory Management A camp RN assesses a 12-year-old with wheezing and shortness of breath after a bee sting, diagnoses anaphylaxis and gives epinephrine IM. A medical RN assesses a diabetic client with severe low blood glucose, diagnoses hypoglycemia and gives D50W IV. An RN reviews the CRNBC Standards of Practice and determines if she or he can manage the intended and unintended outcomes of giving a particular medication. The camp RN follows the CRNBC limits and conditions and uses an established DST when giving epinephrine without an order. The medical RN follows the CRNBC limits and conditions and uses an established DST when giving D50W without an order. Employer Policies RNs are familiar with employer policies related to medication. A surgical RN knows her agency policy requires patients with dopamine drips to be monitored in ICU. She consults with the ordering physician and arranges to have the patient transferred to ICU as soon as possible. Individual Competence RNs know and practise within their own level of knowledge, skill and judgment related to medications. An RN receives an unfamiliar drug order, checks the drug formulary and then calls pharmacy for more information. College of Registered Nurses of British Columbia 7 MEDICATIONS Orders Nurses1 can take orders from physicians, podiatrists, dentists, naturopathic doctors, midwives and nurse practitioners. An order is an authorization to carry out a restricted activity. The ordering professional (prescriber) must also be authorized to carry out the activity in British Columbia. Before carrying out a medication order: determine that the order is clear, complete, current, legible and appropriate, and verify that the order, pharmacy label and/or medication administration record (MAR) are complete A complete order includes: client name date prescribed medication name strength and dosage route dose frequency why the drug is prescribed (when it is a PRN medication) quantity to be dispensed (if appropriate) prescriber signature Clarify any incomplete order with the prescriber. Use the pharmacy dispensing label as an order if there is no alternative. Confirm that the label is current, accurate and appropriate. A pharmacist may produce a list of a client’s current prescribed medications. Once the prescriber reviews and signs the list, it becomes an order. 1 Nurse refers to the following CRNBC registrants: registered nurses, nurse practitioners, licensed graduate nurses. 1 College of Registered Nurses of British Columbia 8 MEDICATIONS VERBAL/TELEPHONE ORDERS Accept verbal/telephone orders only when circumstances require it and there are no other reasonable options. Follow agency policy for accepting and recording these orders. Record the time and date. Record the order as stated by the prescriber. Read the order back to the prescriber to confirm it is complete and accurate. Record the prescriber’s name and title. Sign your name and title on the order. PRE-PRINTED ORDERS Pre-printed orders set out the usual care for a particular client group or problem. Pre-printed orders should be accepted only when the prescriber has: added the client name, made any necessary changes to reflect the needs of the client, and signed and dated the order ABBREVIATIONS Abbreviations can be misused, misread and misinterpreted. Agencies should have a list of acceptable abbreviations. Clarify any unfamiliar or unclear abbreviations used in medication orders. Check the Institute of Safe Medication Practices at www.ismp-canada.org for a list of dangerous abbreviations, symbols and dose designations. UNACCEPTABLE ORDERS Orders that are not client-specific are unacceptable. These include standing orders or general orders protocols placed on client charts without the prescriber reviewing, individualizing and signing them. Orders that are not complete are unacceptable. Examples: medication as at home, resume medications post discharge. USING TECHNOLOGY TO TRANSMIT ORDERS Agency systems should be secure so that client information sent using technology cannot be changed in transit, is kept confidential and can be validated. College of Registered Nurses of British Columbia 9 MEDICATIONS When using fax or e-mail to transmit orders: locate fax machines and printers in secure areas away from public access, retrieve faxes and printed material immediately or ensure they are secure until collected, keep computer screens out of public view and log off when leaving, and use whatever means necessary to confirm the validity of the orders Refer to CRNBC’s Nursing Documentation booklet and Privacy and Confidentiality Practice Standard for more information. Prescribing Registered nurses cannot prescribe medications. Compounding Registered nurses may compound (mix a drug with one or more ingredients). Dispensing Nurses have the authority to dispense certain medications. Dispensing is preparing and giving medication for a client to take later. Nurses dispense with or without a pharmacist’s involvement. Nurses dispense only to clients under their care and only when it is in the client’s best interest. Dispensing with a pharmacist’s involvement When a pharmacist has already reviewed a medication’s suitability and dispensed it for the client, nurses take steps to ensure its proper use. Examples of dispensing with a pharmacist’s involvement may include: Providing a client, leaving a facility on a day pass, with medication to take while away. Giving a client, as part of an outpatient treatment program, medication supplied by a provincial agency (e.g. BC Renal Agency, BC Centre for Disease Control). Providing a health care worker, accompanying a client to an appointment outside the agency, with medication for the client to take while away. Giving a client, discharged from an inpatient unit, medication (e.g. antibiotic, inhaler) to take home with them. College of Registered Nurses of British Columbia 10 MEDICATIONS Dispensing without a pharmacist's involvement When a pharmacist has not reviewed the medication’s suitability (or it’s unclear if this was done), nurses take steps to ensure the medication’s pharmaceutical and therapeutic suitability for the client, as well as its proper use. Examples of dispensing without a pharmacist’s involvement may include: Providing a client, discharged from Emergency, with enough pain medication to manage until the pharmacy open the next morning. Giving a community health client an ‘over the counter’ (OTC) medication (e.g. acetaminophen, emergency contraceptive) to take later. Providing a client at a diagnostic and treatment centre with a course of antibiotics to treat an infection. When employers require nurses to dispense, employers provide the organizational supports necessary for safe dispensing. Dispense medications in accordance with CRNBC’s Dispensing Medication Practice Standard, Standards for Acting Without an Order and/or Standards for Acting With an Order. The Dispensing Medications resource page contains information and resources for dispensing. Medication Inventory Management A nurse may be responsible for managing a medication inventory if there is no pharmacist responsible for this function. The employer is responsible for providing the systems and infrastructure required for the safe management of medications. Refer to the Medication Inventory Management Practice Standard and CRNBC’s Nurse-Managed Medication Inventory: Information for Employers. Drug Substitution by Pharmacists Refer to Pharmacists’ Authority to Adjust, Interchange and Substitute Medication Orders Joint Statement in the CRNBC Standards section of the website www.crnbc.ca Administering When administering medications, registered nurses use knowledge, skill, attitude and judgment about the client and medication to assess, plan, administer, evaluate and document the care. Accountability and safe medication practice is supported when the nurse giving a medication carries out all the steps involved including preparing and documenting. Know about the effects, side effects and potential interactions. College of Registered Nurses of British Columbia 11 MEDICATIONS Educate your client about the medication. Follow the seven rights: right client, right medication, right dose, right time, right route, right reason and right documentation. Administer medication in accordance with CRNBC’s Medication Administration Practice Standard, Standards for Acting Without an Order and/or Standards for Acting With an Order. OFF-LABEL MEDICATIONS Off-label use is using a Health Canada-approved drug for a reason that is not listed on the package insert. It is the unapproved use of a legal medication. Nurses may receive orders for “off-label” use. Before giving any medication, make sure you are well informed about the medication, the reasons for its use and the risks and benefits to the client. INVESTIGATIONAL (EXPERIMENTAL) MEDICATIONS As part of a formal research program, you may receive an order for an investigational medication (not yet listed in a drug schedule or approved by Health Canada). Before administering make sure: the principal or co-investigator of the study (program?) has authorized the order, and a signed and dated consent form is in the client’s health record. As knowledge about reactions to the investigational medication may be incomplete, be particularly alert and document any the client experiences. Nurses do not give an investigational medication that is not part of a formal research program. Refer to the Scope of Practice for Registered Nurses, Standards, Limits and Conditions (p. 33) NARCOTICS AND CONTROLLED DRUGS Agencies must have policies and procedures about: who counts narcotics and controlled drugs, who has access to locked cupboards, what times drugs are counted, how the count is documented, and how to deal with discrepancies in the count PLACEBOS You may give a placebo if your client has consented (e.g., as part of a clinical trial). Clients must be informed they could receive a placebo as part of their treatment or participation in a trial. College of Registered Nurses of British Columbia 12 MEDICATIONS Administering placebos to clients without their knowledge and consent is unethical and unacceptable. COMPLEMENTARY AND ALTERNATIVE THERAPIES If you recommend or participate in these practices, you must: provide the client with evidenced-based information; make sure it is not of higher risk to the client than conventional treatment; and make sure it does not interfere with other current treatments Refer to Complementary and Alternative Health Care for additional information. WITHHOLDING MEDICATIONS If you believe a medication or dose is inappropriate or could harm a client, consult with a pharmacist or colleague, clarify the order with the prescriber and advocate for the client. If the prescriber is unavailable, consult with a manager or experienced colleague. If you still believe the order is unsafe or inappropriate, inform the prescriber you cannot give the medication. The prescriber may choose to give the medication independently. Make sure the issue is referred to an administrator or appropriate committee for resolution. Capable clients may choose not to take medications. All people are assumed capable of giving informed consent unless assessed to be incapable. Help clients understand their plan of care and explore other options. If a client refuses a medication, assess the client’s understanding and talk about potential consequences. Respect a client’s choice. Do not use force, coercion or manipulation to give medications. For issues relating to capacity to consent and substitute decision makers, refer to CRNBC’s Consent Practice Standard. ADMINISTRATION BY OT HERS – THE RN ROLE In some settings, unregulated care providers (UCPs) administer medications. For more information on working with UCPs, refer to the CRNBC Practice Standard Delegating Tasks to Unregulated Care Providers. College of Registered Nurses of British Columbia 13 MEDICATIONS Self-Administration of Medications In some settings, clients take their medications themselves or with help from their family. Examples: Clients who take oral medications kept at the bedside. Clients who come to the nurses’ station for their medications. Clients who use patient-controlled analgesia systems. Clients on pass who take their medications to self-administer. As the nurse, you are still responsible for the overall client care related to medications, including: educating clients about the medication’s actions and possible side effects, how to take them and monitor the effect (e.g., testing blood glucose), determining medications are taken as ordered, monitoring and evaluating client response and reactions, and following agency policy for documenting. Role of the CRNBC-Certified Practice RN Nurses with CRNBC-certified practice designation may diagnose and treat some diseases and disorders, including administering or dispensing specific Schedule I medications without an order. They must follow CRNBC-approved decision support tools (DSTs). CRNBC-certified practice nurses do not prescribe (i.e., write a prescription for a client to fill at a pharmacy). When treating a client, CRNBC-certified practice nurses must dispense the full course of medication as per the DST. For more information on certified practice activities and requirements, please see the Certified Practice page at www.crnbc.ca College of Registered Nurses of British Columbia 14 MEDICATIONS Documentation Nurses are responsible for maintaining timely and accurate records of all medications they give. Document on the agency record as soon as possible after giving medications. Include client name, drug name, date (and time if appropriate), dose, route, site, signature and title. When a record has room for initials only, sign the accompanying signature sheet (this should be filed with every client’s permanent record). If giving a PRN medication, document your assessment and the client’s response. When asked to double check or verify a medication, follow agency policy and document appropriately. Documenting by exception is never acceptable for medications. MEDICATIONS NOT GIVEN When you withhold or omit medications, document why, when and who was notified. MEDICATIONS GIVEN BY OTHER STAFF Document only the medications you give. Do not allow others to document medications for you and do not document medications that anyone else has given. The exception is in an emergency, such as a cardiac arrest when a nurse, designated as recorder, documents medications given by others. Those who gave the medications should countersign this record as soon as possible. If agency policy does not allow auxiliary staff to document on the health record, nurses record the medications given and any related observations reported to them. College of Registered Nurses of British Columbia 15 MEDICATIONS Medication Safety Medication safety is an important part of patient safety. Transparency and reporting are the most effective ways to reduce errors. Shaming, blaming and punishing do not prevent errors and may discourage reporting. MEDICATION ERRORS Medication errors are avoidable events that may happen during the process of prescribing, compounding, dispensing or administering a medication. They can result in a near miss injury or death. A near miss or close call is an event that could have resulted in unwanted consequences for a patient, but either by chance or timely intervention did not. These errors can involve the wrong client, medication, dose, time, reason, route or documentation. Medication errors often result from systems issues. Because of this, the best way to address a medication error is to use a just, multidisciplinary approach that focuses on why the error occurred. – ISMP Canada When a medication error occurs, take immediate steps to resolve and report it. Your primary concern is client safety. Assess the client promptly and notify the client’s practitioner so they can assess and treat the client if required. Document the facts of the error on the client’s chart, including what happened, interventions carried and client response. Follow agency policy for reporting errors. College of Registered Nurses of British Columbia 16 MEDICATIONS Resources for Nurses BC DRUG AND POISON INFORMATION SERVICES BC Drug and Poison Information Services’ mandate is to develop and implement centralized services to assist health professionals in providing optimal levels of drug therapy and poison management in the province and to provide poison information request services to the public. Twenty-four hour toll-free poison information is available for the public by calling 604.682.5050 or 1.800.567.8911. Health professionals can email info@dpic.bc.ca or call 604.682.2344 (ext. 62126). INSTITUTE FOR SAFE MEDICATION PRACTICES CANADA (ISMP CANADA) ISMP Canada is an independent national non-profit agency committed to the advancement of medication safety in all healthcare settings. It works collaboratively with the healthcare community, regulatory agencies and policy makers, provincial, national and international patient safety organizations, the pharmaceutical industry and the public to promote safe medication practices. More information at www.ismp-canada.org COLLEGE OF PHARMACISTS OF BRITISH COL UMBIA The College is responsible for registering pharmacists and pharmacy technicians and licensing pharmacies throughout the province. Their website contains information about and links to provincial and federal legislation and drug schedules. www.bcpharmacists.org SAFER HEALTHCARE NOW! (SHN) The SHN campaign offers Canadian health care organizations the opportunity to participate in and support a campaign dedicated to improving patient safety, through the implementation of six targeted interventions in patient care including medication reconciliation. For more information, email westernnode@saferhealthcarenow.ca or visit www.saferhealthcarenow.ca College of Registered Nurses of British Columbia 17