DOCX ENG
advertisement

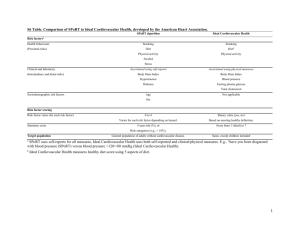
E-01 : primitive hypertension E- 01 : hypertension with renal disease B-CRF : cardiovascular complications Prevention of Cardiovascular Disease in Women: Highlights for the Clinician of the 2011 American Heart Association Guidelines Nanette K. Wenger Advances in Chronic Kidney Disease. Volume 20, Issue 5 , Pages 419-422, September 2013 Emory University School of Medicine, Emory Heart and Vascular Center, Atlanta, GA ABSTRACT The 2011 Update to the American Heart Association Effectiveness-Based Guidelines for the Prevention of Cardiovascular Disease in Women is designed to assist women and health professionals in understanding the cardiovascular disease risk for women and undertaking the most effective preventive interventions. Although coronary heart disease remains the leading cause of mortality for women in the United States, cardiovascular mortality among U.S. women has decreased dramatically each year since 2000, with the decline in mortality being steeper for women than for men. Nonetheless, since 1984, more women than men continue to die annually from cardiovascular disease. Half of the decrement in cardiovascular mortality for women since 2000 reflects the improved management of their established cardiovascular disease; the other half is attributable to reductions in their major coronary risk factors, hence the importance of this prevention guideline. Key Words: Prevention, Cardiovascular disease, Women, AHA guidelines COMMENTS Use of the traditional Framingham Risk Score is acknowledged to underestimate cardiovascular risk in women, likely because of its focus on 10-year risk, in that women develop cardiovascular disease later in life. This likely underlies the problem that physicians and other healthcare providers characteristically underestimate the cardiovascular risk for women, leading to underprescription and underutilization of preventive therapies. The 2007 American Heart Association prevention guideline promulgated an algorithm designed to reflect women's increased lifetime risk for cardiovascular disease; This simplified approach to cardiovascular risk assessment in women classifies them as “high risk,” “at risk,” and as at “ideal cardiovascular health.” Characteristics of high-risk status include •Clinically manifest coronary heart disease •Clinically manifest cerebrovascular disease •Clinically manifest peripheral arterial disease •Abdominal aortic aneurysm •End-stage kidney disease or CKD •Diabetes mellitus •10-year predicted cardiovascular risk ≥ 10% At-risk women are characterized by having at least 1 of the following major risk factors: •Cigarette smoking •Systolic blood pressure of 120 mmHg or greater, diastolic blood pressure of 80 mmHg or greater, or being treated for hypertension •Total cholesterol of 200 mg/dL or greater, high-density lipoprotein cholesterol (HDL-C) less than 50 mg/dL, or being treated for dyslipidemia •Obesity, particularly central obesity •Poor diet •Physical inactivity •Family history of premature cardiovascular disease occurring in first-degree relatives in men younger than 55 years of age or in women younger than 65 years of age •Metabolic syndrome •Evidence of advanced subclinical atherosclerosis (eg, coronary calcification, carotid plaque, or increased intima-media thickness) •Poor exercise capacity on treadmill test and/or abnormal heart rate recovery after stopping exercise •Systemic autoimmune collagen-vascular disease (eg, lupus or rheumatoid arthritis) •History of preeclampsia, gestational diabetes, or pregnancy-induced hypertension Ideal cardiovascular health is characterized by all of the following: •Total cholesterol less than 200 mg/dL (untreated) •Systolic blood pressure less than 120 mmHg/diastolic blood pressure less than 80 mmHg (untreated) •Fasting blood glucose less than 100 mg/dL (untreated) •Body mass index (BMI) less than 25 kg/m2 •Abstinence from smoking •Physical activity at goal for adults older than 20 years of age: 150 minutes/week or more of moderate intensity, 75 minutes/week or more of vigorous intensity, or a combination •Healthy (Dietary Approaches to Stop Hypertension (DASH)-like) diet Newly added to the at-risk characteristics since 2007 is the evidence of systemic autoimmune collagen vascular disease, particularly lupus or rheumatoid arthritis; because of the increased relative risk for cardiovascular disease in these women, they should be screened for cardiovascular risk factors. Also newly added are complications of pregnancy, which appear to be early indicators of cardiovascular risk, mandating the appropriate referral of women with these pregnancy complications for cardiovascular risk assessment and surveillance. Highlighted is that a detailed history of pregnancy complications should be part of the routine cardiovascular risk assessment for all women. Thus, the recommended evaluation for cardiovascular risk in women encompasses a medical history that includes a family history and a history of pregnancy complications, assessment of symptoms of cardiovascular disease, and depression screening for women documented to have cardiovascular disease. Physical examination for risk assessment should include measurements of blood pressure, BMI, and waist circumference; laboratory tests should include fasting lipoprotein and glucose levels; and a Framingham Risk assessment should be performed if there is no evidence for cardiovascular disease, CKD, or diabetes mellitus. Pr. Jacques CHANARD Professor of Nephrology