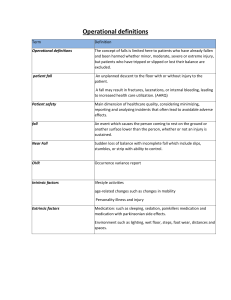
Administering Medications Introduction An adverse drug event (ADE) is defined as harm to the patient, including mental harm, physical harm, or loss of function, that results from a medication error. A medication error refers to a mistake that occurs during the medication administration process. If a mistake occurs, it doesn't matter whether the patient was harmed or whether there was a potential for injury it's still considered a medication error. An ADE is a more direct measure of harm to the patient than a medication error. ADEs can be further defined as preventable or nonpreventable. A preventable ADE results from a clinician error or a systematic error and could, therefore, have been prevented. A nonpreventable ADE results from a drug's pharmacologic properties. Avoid distractions and interruptions when preparing and administering medications to promote a culture of safety and prevent medication errors. Adhere to the "five rights" of medication administration: Identify the right patient by using at least two patient-specific identifiers, select the right medication, administer the right dose, administer the medication at the right time, and administer the medication by the right route. Recent literature identifies nine rights of medication administration, which in addition to the five rights includes the right documentation, the right action (or appropriate reason for prescribing the medication), the right form, and the right response. Oral drug administration Introduction Because oral administration is usually the safest, most convenient, and least expensive method of drug delivery, it's the most common administration route. Drugs for oral administration are available in many forms: tablets, enteric-coated tablets, capsules, syrups, oils, liquids, suspensions, powders, and granules. Some require special preparation before administration, such as mixing them with juice to make them more palatable; oils, powders, and granules most commonly require such preparation. Sometimes oral drugs are prescribed in higher dosages than their parenteral equivalents because, after absorption through the GI system, they are immediately broken down by the liver before they reach the systemic circulation. Elder alert: An oral dosage normally prescribed for adults may be dangerous for elderly patients because of their decreased hepatic and renal clearance. 2 Oral drug administration is contraindicated for unconscious patients. It may also be contraindicated in patients with nausea and vomiting and in those who can't swallow. Nurses are responsible for understanding the pharmacology behind the drugs they administer to prevent potential error and patient harm. Equipment • Patient's medication record • Prescribed drug • Medication cup • Water • Optional: personal protective equipment, appropriate vehicle (such as pudding or applesauce) for crushed pills (commonly used for elderly patients), preferred beverage, pill-crushing device Implementation • Avoid distractions and interruptions when preparing and administering the drug to prevent medication errors. • Verify the order on the patient's medication record by checking it against the practitioner's order. • Reconcile the patient's medications when the practitioner prescribes a new medication to reduce the risk of medication errors, including omissions, duplications, dosing errors, and drug interactions. • Perform hand hygiene. • Gather and prepare the necessary equipment and supplies. • Compare the drug label to the order in the patient's medical record. • Check the patient's medical record for an allergy or contraindication to the prescribed medication. If an allergy or contraindications exist, don't administer the medication and notify the practitioner. Clinical alert: Cardiovascular agents, antibiotics, antifungals, antiretrovirals, diuretics, anticoagulants, antidiabetics, steroids, opioids, anticholinergics, benzodiazepines, and nonsteroidal anti-inflammatory drugs are the most common drugs that cause drug interactions. To avoid drug interactions, review with the patient all current prescribed and over-the-counter drugs, dietary supplements, and herbal preparations. Notify the patient's practitioner and your facility's pharmacy of any potential interactions. • Check the expiration date on the medication (as shown below). If the medication is expired, return it to the pharmacy and obtain new medication. • Visually inspect the medication for loss of integrity; don't administer the medication if integrity is compromised. • Discuss any unresolved concerns about the medication with the patient's practitioner. • Perform hand hygiene. • Confirm the patient's identity using at least two patient identifiers. • Provide privacy. • Explain the procedure to the patient and family (if appropriate) according to their individual communication and learning needs to increase their understanding, allay their fears, and enhance cooperation. • If the patient is receiving the medication for the first time, teach the patient and family (if appropriate) about potential adverse reactions and other concerns related to the medication. • Assess the patient's condition to determine the need for the medication and • Observe the patient carefully for a rash, pruritus, cough, and other signs of an adverse reaction to a previously administered drug. • Verify that you're administering the medication at the proper time, in the prescribed dose, and by the correct route to reduce the risk of medication errors. • If your facility uses bar-code technology, use it, as directed by your facility. • Administer the medication to the patient (as shown below) along with an appropriate vehicle or liquid, as necessary, to aid swallowing, minimize adverse effects, and the effectiveness of previous therapy. promote absorption. • If the patient can't swallow a whole tablet or capsule, ask the pharmacist whether the medication is available in liquid form or can be administered by another route. If not, request a crushed tablet (if appropriate). Alternatively, discuss whether you can crush the tablet yourself or open the capsule and mix it with food. Keep in mind that many enteric-coated and time-release drugs and gelatin capsules shouldn't be crushed to prevent possible adverse effects. If necessary, contact the practitioner for an order to change the administration route. • Stay with the patient until the patient has swallowed the drug. If the patient seems confused or disoriented, check the mouth to make sure that the patient has swallowed the drug. • Monitor the patient for adverse reactions and respond appropriately. • Discard used supplies in appropriate containers. • Perform hand hygiene. • Document the procedure. Special Considerations • Notify the practitioner about any medication that the patient refuses or that you withhold. • Evaluate appropriate current laboratory test results (including potassium and digoxin levels), as necessary and ordered, before administering a medication affected by these values. • Don't administer a medication from a poorly labeled or unlabeled container. Don't attempt to label or reinforce medication labels yourself. This action must be done by a pharmacist. • Never administer a medication poured by someone else. • Never return unwrapped or prepared medications to stock containers. Instead, dispose of them or return them to the pharmacy. Keep in mind that another nurse must witness and cosign the disposal of a controlled substance, as mandated by law. • If the patient questions you about a medication or dosage, check the medication record again. If the drug is correct, reassure the patient. Explain any changes in the drug or dosage. Teach the patient and family (if appropriate), about possible adverse effects. Ask the patient to report anything perceived as a possible adverse effect. • Administer unpleasant-tasting liquids through a straw, if possible, to minimize • When tablets must be split, request that the pharmacy split and repackage them before dispensing the medication to prevent medication errors. their contact with the taste buds, making them more palatable. Complications Complications of oral drug administration include aspiration, adverse effects of the prescribed drug, and medication administration errors. Documentation Document the medication strength, dose, administration route, and date and time of administration. Record pertinent assessment data you obtained before administration, such as the heart rate or symptoms that warranted the use of an as-needed medication. Record any adverse reactions to the prescribed medication, the date and time you notified the practitioner, prescribed interventions, and the patient’s response to those interventions. 41 If the patient refuses a medication, document the refusal and the name of the practitioner you notified. Also note whether you omitted or withheld a medication for other reasons, such as for radiology or laboratory tests or if, in your judgment, the drug was contraindicated at the ordered time. Verify and sign out all controlled substances according to your controlled substance documentation system. Document teaching you provided to the patient and family (if applicable), their understanding of that teaching, and any need for follow-up teaching. Eyedrop administration Introduction Practitioners may prescribe eyedrops for a variety of diagnostic and therapeutic purposes, including dilating the pupil, staining the cornea to detect abrasions or scars, anesthetizing or lubricating the eye, and treating such disorders as glaucoma and infection. Understanding the ocular effects of medications is important, because certain drugs can cause eye disorders or have serious ocular effects. For example, anticholinergics, which are commonly in use during eye examinations, can exacerbate acute glaucoma in patients with a predisposition to the disorder. Equipment • Prescribed eye medication • Gloves • Warm water or normal saline solution • Gauze pads • Facial tissues • Optional: ocular dressing, personal protective equipment Preparation of Equipment Inspect all equipment and supplies. If a product is expired, is defective or has compromised integrity, remove it from patient use, label it as expired or defective, and report the expiration or defect, as directed by your facility. Make sure the medication is labeled for ophthalmic use. Date the medication container the first time you open it because you should use the medication within the time specified by the manufacturer once you've opened the container to prevent contamination. 34 Follow your facility's directions or the manufacturer's instructions on when to discard an opened eye medication. Implementation • Avoid distractions and interruptions when preparing and administering the medication to prevent medication errors. • Verify the practitioner's b. • Reconcile the patient’s medications when the practitioner prescribes a new medication to reduce the risk of medication errors, including omissions, duplications, dosing errors, and drug interactions. • Gather and prepare the necessary b and supplies. • Compare the medication label to the order in the patient's medical record. . • Confirm which eye requires treatment. Clinical alert: Make sure you know which eye to treat, because the practitioner may order different medications and doses for each eye. • Check the patient's medical record for an allergy or contraindication to the prescribed medication. If an allergy or contraindications exist, don't administer the medication and notify the practitioner. • Check the expiration date. If the medication is expired, return it to the pharmacy and obtain new medication. • Visually inspect the medication for particles or discoloration or other loss of integrity; don't administer the medication if integrity is compromised. • Discuss any unresolved concerns about the medication with the patient's practitioner. • Warm the medication to room temperature, as necessary. • Perform hand hygiene. • Confirm the patient's identity using at least two patient identifiers. • Provide privacy. • Explain the procedure to the patient and family (if appropriate) according to their individual communication and learning needs to increase their understanding, allay their fears, and enhance cooperation. 24 • If the patient is receiving the medication for the first time, teach the patient and family (if appropriate) about potential adverse reactions or other concerns related to the medication. 78910 • Verify that you're administering the medication at the proper time, in the prescribed dose, and by the correct route to reduce the risk for medication errors. 78910 • If your facility uses bar-code technology, use it, as directed by your facility. • Raise the bed to waist level before providing care to prevent caregiver back strain. 25 • Have the patient sit or lie in the supine position. • Perform hand hygiene. • Put on gloves to comply with standard precautions. • If the patient is wearing an eye dressing, remove it by pulling it gently down and away from the patient's forehead to prevent skin shearing or tearing. 30 Take care not to contaminate your hands. • Assess the patient's eye, noting any redness, edema, or discharge; note the appearance and amount of discharge. • Remove any discharge by cleaning around the eye with gauze pads moistened with warm water or normal saline solution. With the patient's eye closed, clean from the inner to the outer canthus. Use a fresh gauze pad for each stroke. • To remove crusted secretions from around the eye, take these steps: • Moisten a gauze pad with warm water or normal saline solution. • Ask the patient to close the eye. • Place the gauze pad over it for 1 to 2 minutes. • Remove the pad. • Repeat the steps with new moist gauze pads, as necessary, until the secretions are soft enough to be removed without traumatizing the mucosa. • Remove and discard your gloves. • Perform hand hygiene. • Put on new gloves. • Instruct the patient to tilt the head back and toward the side of the affected eye so that excess medication can flow away from the tear duct, minimizing systemic absorption through the nasal mucosa. • Remove the bottle cap from the medication container and place it on a clean, dry surface. Be careful to avoid contaminating the dropper tip or bottle top. • Before instilling the eyedrops, instruct the patient to look up and away. This • If necessary, steady the hand holding the dropper by resting it against the patient's forehead. 1 With your other hand, pull down the lower lid of the affected position moves the cornea away from the lower lid and minimizes the risk of touching the cornea with the dropper if the patient blinks. eye gently and instill the drops in the conjunctival sac. Try to avoid placing the drops directly on the eyeball to prevent the patient from experiencing discomfort. (See Instilling eyedrops.) INSTILLING EYEDROPS To instill eyedrops, pull the lower lid down to expose the conjunctival sac (as shown below). Have the patient look up and away, and then squeeze the prescribed number of drops into the sac. Then release the patient's eyelid. • After instilling the eyedrops, instruct the patient to close the eyes gently without squeezing the lids shut. • If necessary, press your thumb or a gauze pad gently on the inner canthus for 2 to 3 minutes while the patient closes the eyes to prevent systemic absorption of medication. • Use a clean tissue to remove any excess solution leaking from the eye. Remember to use a fresh tissue for each eye to prevent cross-contamination. • Apply a new ocular dressing if necessary. • Return the bed to the lowest position to prevent falls and maintain patient safety. 32 • Discard used supplies in appropriate receptacles. • Return the medication to the storage area, storing it according to the label's instructions. • Remove and discard your gloves. • Perform hand hygiene. • Document the procedure. Special Considerations • Never touch the dropper tip to the patient's eyeball, eyelids, or eyelashes to maintain the drug container's sterility. 1 If the dropper tip becomes contaminated, discard the medication and obtain another sterile medication bottle. Complications Instillation of some eye medications can cause transient burning, itching, and redness. Although rare, systemic effects can also occur. Documentation Document your assessment of the eye. Record the medication you administered, eye or eyes you treated, and date, time, and dose, according to your facility's documentation format. Note the patient's response to the procedure. Document any adverse effects that occur, the date and time you notified the practitioner, prescribed interventions, and the patient's response to those interventions. 38 Document teaching you provided to the patient and family (if appropriate), their understanding of that teaching, and any need for follow-up teaching. Eye ointment application Introduction An ointment formulation helps keep an eye medication in contact with the treatment area of the eye for as long as possible. Eye ointments treat eye diseases, prevent or treat infection or inflammation, relieve discomfort, provide lubrication, and prevent damage. Equipment • Prescribed eye ointment • Gloves • Warm water or normal saline solution • Sterile gauze pads • Facial tissues • Optional: ocular dressing, personal protective equipment Preparation of Equipment Inspect all equipment and supplies. If a product is expired, is defective, or has compromised integrity, remove it from patient use, label it as expired or defective, and report the expiration or defect, as directed by your facility. Implementation • Avoid distractions and interruptions when preparing and administering medication to prevent medication errors. • Verify the practitioner's order. • Reconcile the patient’s medications when the practitioner prescribes a new medication to reduce the risk of medication errors, including omissions, duplications, dosing errors, and drug interactions. • Gather and prepare the necessary equipment and supplies. • Compare the medication label to the order in the patient's medical record to • Confirm which eye requires treatment. • Check the patient's medical record for an allergy or contraindications to the prescribed medication. If an allergy or contraindications exist, don't administer the medication and notify the practitioner. verify the correct medication, indication, dose, route, and time of administration. • Check the expiration date on the medication. If the medication is expired, return it to the pharmacy and obtain new medication. • Visually inspect the medication for discoloration or other loss of integrity; don't administer the medication if integrity is compromised. • Discuss any unresolved concerns about the medication with the patient's practitioner. • Warm the medication ointment tube in the palm of your hand, as necessary, to bring • Perform hand hygiene. • Confirm the patient's identity using at least two patient identifiers. • Provide privacy. • Explain the procedure to the patient and family (if appropriate) according to their individual communication and learning needs to increase their understanding, allay it to body temperature. Warming the ointment facilitates administration into the eye. Keep the cap on the tube to avoid spillage. their fears, and enhance cooperation. • If the patient is receiving the medication for the first time, teach the patient and family (if appropriate) about potential adverse reactions or other concerns related to the medication. • Verify that you're administering the medication at the proper time, in the prescribed dose, and by the correct route to reduce the risk for medication errors. • If your facility uses bar-code technology, use it, as directed by your facility. • Perform hand hygiene. • Raise the bed to waist level before providing care to prevent caregiver back strain. 23 • Have the patient sit or lie in the supine position. • Perform hand hygiene. • Put on gloves to comply with standard precautions. • If the patient is wearing an eye dressing, remove it by gently pulling it down and away from the patient's forehead. Take care not to contaminate your hands. • Assess the condition of the eye, noting redness, edema, or discharge. • Remove any discharge by cleaning around the patient's eye with sterile gauze pads moistened with warm water or normal saline solution. With the patient's eye closed, clean from the inner to the outer canthus, using a fresh sterile gauze pad for each stroke. • To remove crusted secretions from around the eye, follow these steps: • Moisten a sterile gauze pad with warm water or normal saline solution. • Ask the patient to close the eye. • Place the moistened gauze pad over the eye for 1 to 2 minutes. • Remove the pad. • Repeat the procedure, as necessary, until the secretions are soft enough to remove without traumatizing the mucosa. • Remove and discard your gloves. • Perform hand hygiene. • Put on new gloves. • Instruct the patient to tilt the head back. • Remove the medication tube cap and place it on a clean, dry surface. • Squeeze a small ribbon of medication on the edge of the conjunctival sac, beginning at the inner canthus (as shown below) and continuing to the outer canthus. 2 If necessary, steady the hand holding the medication tube by bracing it against the patient's forehead or cheek, taking care not to touch the tip of the tube to the eye or any other surface. Cut off the ribbon of ointment by turning the tube. • Instruct the patient to close the eyes gently without squeezing the lids shut and to roll the eyes behind the closed lids to help distribute the medication over the surface of the eyeball. Tell the patient that the eye ointment may cause momentary blurring of the vision. 1 • Use a clean facial tissue to remove any excess solution or ointment leaking from the eye. Remember to use a fresh tissue for each eye to prevent cross- contamination. 2 • Apply a new ocular dressing if necessary. • Reapply the cap to the medication tube and then return the tube to the storage area. Make sure that you store the medication according to the label's instructions. • Return the bed to the lowest position to prevent falls and maintain patient safety. • Discard used supplies in appropriate receptacles. • Remove and b your gloves. • Perform hand hygiene. • Document the procedure. Special Considerations • To maintain the drug container's sterility, never touch the tip of the tube to the patient's eyeball, lids, or lashes. • To prevent cross-contamination, never use the same container of eye medication for more than one patient. • If you're administering eyedrops and an eye ointment, administer the drops before applying the ointment, because the ointment may inhibit the action of the eyedrops. Wait times between applications vary; follow the medications' prescribing information. • Treat only the affected eye unless otherwise ordered. Complications Instillation of some eye medications can cause transient burning, itching, and redness. Although rare, systemic effects can also occur. Documentation Document your assessment of the eye before medication administration. Record the medication you applied, the eye or eyes you treated, and the date, time, and dose, according to your facility's documentation format. Eardrop instillation Introduction Eardrops may be prescribed for various conditions, including infection and inflammation. They may also be used to soften cerumen for removal, produce local anesthesia, and facilitate removal of an insect or other foreign body trapped in the ear. Instillation of eardrops is usually contraindicated if the patient has a perforated eardrum but may be permitted with certain medications and adherence to sterile no-touch technique. Equipment • Prescribed eardrops • Light source • Facial tissues • Optional: gloves, cotton balls, cotton-tipped applicator, personal protective equipment Preparation of Equipment Inspect all equipment and supplies. If a product is expired, is defective, or has compromised integrity, remove it from patient use, label it as expired or defective, and report the expiration or defect as directed by your facility. Allow the ear medication to reach room temperature before administration or warm the solution by rotating the container gently in your hands. Instilling cold eardrops can cause dizziness and nausea. Implementation • Avoid distractions and interruptions when preparing and administering the medication to prevent administration errors. • Verify the practitioner's order. • Reconcile the patient's medications when the practitioner prescribes a new medication to reduce the risk of medication errors, including omissions, duplications, dosing errors, and drug interactions. • Gather and prepare the medication and the necessary equipment and supplies. • Compare the medication label to the order in the patient's medical record. • Check the patient's medical record for an allergy or a contraindication to the prescribed medication. If an allergy or contraindication exists, don't administer the medication and notify the practitioner. • Check the expiration date on the medication. If the medication is expired, return it to the pharmacy and obtain new medication. • Visually inspect the medication for particles, discoloration, or other loss of integrity; don't administer the medication if integrity is compromised. • Perform hand hygiene. • Confirm the patient's identity using at least two patient identifiers. • Provide privacy. • Explain the procedure to the patient and family (if appropriate) according to their individual communication and learning needs to increase their understanding, allay their fears, and enhance cooperation. • If the patient is receiving the medication for the first time, teach the patient and family (if appropriate) about potential adverse effects or other concerns related to the medication. • Verify that the medication is being administered at the proper time, in the prescribed dose, and by the correct route to reduce the risk of medication errors. • Confirm the ear in which you must administer the medication. • If your facility uses bar-code technology, use it as directed by your facility. • Raise the bed to waist level before providing care to prevent caregiver back strain. 22 • Perform hand hygiene. Clinical alert: If your facility’s hazardous drug list contains the drug you’re about to administer, put on personal protective equipment as directed. • Put on gloves, as needed, to comply with standard precautions. • Have the patient sit or lie with the head turned to the unaffected side. • Straighten the patient's ear canal by pulling the auricle (pinna) of the ear up and back. • Using a light source, examine the ear canal for drainage. If you find any, clean only the outer ear with a tissue or cotton-tipped applicator. • To avoid damaging the ear canal with the dropper, support the hand holding the dropper gently against the patient's cheek or head, keeping the dropper above the ear canal and being careful not to contaminate it. • Squeeze the dropper slowly and firmly to instill the ordered number of drops on the side of the ear canal. • Massage the tragus (the fleshy part in front of the ear canal) gently with your finger, unless contraindicated because of pain. Doing so facilitates entry of the medication into the ear canal. • Have the patient remain supine with the head turned for the time specified by the medication's prescribing information (usually 1 to 5 minutes) to allow absorption of the medication. • Place a cotton ball in the ear, if needed, to prevent medication leakage. 28 • Clean and dry the outer ear with a tissue. • Repeat the procedure on the other ear, if ordered. • Assist the patient into a comfortable position. • Return the bed to the lowest position to prevent falls and maintain the patient's safety. • Remove and discard your gloves, if worn. • Perform hand hygiene. • Document the procedure. Complications Complications of eardrop instillation may include local reactions, such as redness and swelling of the ear canal, as well as systemic reactions. The patient may report dizziness, nausea, or discomfort if the medication is given while it's cold. Documentation Document the color and amount of ear drainage, if present. Document the medication strength, dose (number of eardrops instilled), administration route, ear(s) treated, and date and time of administration. Record any adverse reactions to the prescribed medication, the date and time the practitioner was notified, prescribed interventions, and the patient’s response to those interventions. 35 Document teaching provided to the patient and family (if appropriate), their understanding of that teaching, and any need for follow-up teaching. Rectal suppository administration Introduction A rectal suppository is a small, solid, medicated mass that is usually cone-shaped with a cocoa butter or glycerin base and is intended as a singledose rectal application. It can help stimulate peristalsis and defecation or relieve pain, vomiting, and local irritation. Rectal suppositories commonly contain drugs to reduce fever and induce relaxation that can't be administered orally because they interact poorly with digestive enzymes or have an offensive taste. They may also help when a patient can't take medications orally because of nausea, vomiting, or another GI condition. Rectal suppositories melt at body temperature and are absorbed slowly by the rectal mucosa. Because insertion of a rectal suppository may stimulate the vagus nerve, this procedure is contraindicated in patients with potential cardiac arrhythmias. It may also be contraindicated in patients with active rectal bleeding or recent rectal or prostate surgery because of the risk of local trauma and discomfort during insertion. The rectal route for medication administration isn't recommended for use in patients with immunosuppression or thrombocytopenia because of the risk of infection and bleeding. Equipment • Prescribed rectal suppository • Patient's medication administration record • Gloves • Water-soluble lubricant • Optional: bedpan, other personal protective equipment Preparation of Equipment Inspect all equipment and supplies. If a product is expired, is defective, or has compromised integrity, remove it from patient use, label it as expired or defective, and report the expiration or defect as directed by your facility. Implementation • Avoid distractions and interruptions when preparing and administering medication to prevent medication errors. • Verify the practitioner's order. • Reconcile the patient's medications when the practitioner prescribes a new medication to reduce the risk of medication errors, including omissions, duplications, dosing errors, and drug interactions. • Gather and prepare the medication and the necessary equipment and supplies. • Compare the medication label to the order in the patient's medical record. • Check the patient's medical record for an allergy or a contraindication to the prescribed medication. If an allergy or a contraindication exists, don't administer the medication and notify the practitioner. • Check the expiration date on the medication. If the medication is expired, return it to the pharmacy and obtain new medication. • Visually inspect the medication for discoloration or other loss of integrity; don't administer the medication if integrity is compromised. • Discuss any unresolved concerns about the medication with the patient's practitioner. • Perform hand hygiene. • Confirm the patient's identity using at least two patient identifiers. • Provide privacy. • Explain the procedure to the patient and family (if appropriate) according to their individual communication and learning needs to increase their understanding, allay their fears, and enhance cooperation. • If the patient is receiving the medication for the first time, teach the patient and family (if appropriate) about potential adverse reactions or other concerns related to the medication. • Verify that the medication is being administered at the proper time, in the prescribed dose, and by the correct route to reduce the risk of medication errors. • If the medication is not being used to stimulate peristalsis or defecation, ask whether the patient needs to defecate. Assist with toileting, as needed. • If your facility uses bar-code technology, use it as directed by your facility. • Raise the bed to waist level before providing care to prevent caregiver back strain. • Perform hand hygiene. • Put on gloves to comply with standard precautions. • Position the patient on the left side in the Sims position. • Drape the patient with the bed linens to expose only the buttocks. • Remove the suppository from its packaging. • Lubricate the suppository with water-soluble lubricant. • Lift the patient's upper buttock with your nondominant hand to expose the anus. • Instruct the patient to take several deep breaths through the mouth to help • Using the index finger of your dominant hand, insert the suppository—tapered end first—about 1" (2.5 cm), until you feel it pass the internal anal sphincter to prevent expulsion. 31 Ensure that the suppository is in contact with the rectal wall. • Direct the tapered end toward the side of the rectum so that it contacts the membranes. (See How to administer a rectal suppository.) relax the anal sphincter and reduce anxiety and discomfort during insertion. HOW TO ADMINISTER A RECTAL SUPPOSITORY When inserting a suppository, direct its tapered end toward the side of the rectum so that it contacts the membranes, encouraging medication absorption (as shown below). • Ensure the patient's comfort and make sure that the patient can reach the call light. Encourage the patient to lie still and, if applicable, to squeeze or hold the buttocks together to retain the suppository for the appropriate time. The patient should retain a suppository administered to relieve constipation as long as possible (at least 20 minutes) to be effective. If appropriate, keep a bedpan close by to place under the patient in case the patient has difficulty retaining the suppository. • Return the bed to the lowest position to prevent falls and maintain the patient's • Remove and discard your gloves and, if worn, other personal protective equipment. • Perform hand hygiene. • Document the procedure. safety. Special Considerations • Store suppositories in a cool, dry place to avoid melting. Refrigerate them if directed by the medication label. • Be sure to inform the patient that the suppository may discolor the next bowel movement. For example, hydrocortisone suppositories can give feces a silver-gray, pasty appearance. Patient Teaching Some rectal suppositories are available over the counter. Teach the patient how to selfadminister the suppository, if appropriate. A patient experiencing constipation may need further teaching about proper diet, hydration, daily exercise, and proper use of laxatives. Complications Complications related to the medication's action may occur. Vagal nerve stimulation may occasionally occur, causing a vagal reaction. Defecation can cause early expulsion of the suppository, resulting in incomplete absorption. 38 Other potential complications include local reactions, such as tissue irritation and rectal bleeding. Documentation Document the medication strength, dose, administration route, and date and time of administration. Record any adverse reactions to the prescribed medication, the date and time that the practitioner was notified, prescribed interventions, and the patient’s response to them. 39 Document the patient's tolerance of the procedure and response to therapy. Document teaching provided to the patient and family (if applicable), their understanding of that teaching, and any need for follow-up teaching.