STATE OF PALESTIN
دولــــــــة فلســــــــطين
Ministry of Health
وزارة الصحـــــــة
Palestinian Pediatric Emergency Guidelines
بروتوكوالت طوارئ األطفال
MAY 2022
FORWARD
It is a known fact that deaths of children in hospital often occur within the first
24 hours of their admission to the facility. Many of these deaths could be
prevented if very sick children were identified, and proper treatment was
initiated immediately upon their arrival at the emergency departments.
This can be facilitated and achieved by rapid triage of all children presenting
to the hospital for provision of appropriate emergency treatment accordingly.
Therefore, the Ministry of Health in Gaza has adopted guidelines and training
materials for Pediatric Emergency Triage, Assessment and Treatment
(PETAT). The guidelines and training materials were developed by a local
group of consultant pediatricians and clinical pharmacists from different
hospitals.
Pediatric Emergency Guidelines aims at identifying children presenting with
airway obstruction and other breathing problems, circulatory impairment or
shock, severely altered coma or convulsive seizures (CNS) function, or severe
dehydration, as those children are the ones who require urgent interventions
and proper medical care to prevent death. The urgency categorization and
waiting time definition are considered quality indicators in patient care,
especially in situations when there is a large volume of patients.
Since the first edition of the PETAT, many new evidences in emergency
services have become available and number of international guidelines have
been updated. These updates included recognition of the importance of
cardiac pulmonary resuscitation in children, use of mask ventilation during
resuscitation, new oxygen delivery methods, use of oxygen titration to limit
the risk for hyperoxaemia, especially in preterm neonates, and many others.
The use of this guideline that was developed to improve triage and emergency
care of children presenting with signs of severe illness would certainly
contribute substantially to reducing morbidity and mortality indicators of
infants and young children brought to hospital.
Deputy Minister
Dr Yousef Abu Al Reesh
ACKNOWLEDGEMENTS
The MoH expresses its gratitude to the following Palestinian experts, who
participated in the technical review, revision and adaptation of these
Pediatric Emergency Guidelines.
Dr/ Nabil M.A. Albarqouni (Senior Consultant Pediatrician and Neonatologist)
Dr/ Ziyad Al masri (Chief of PICU Dorrha hospital)
Dr/ Raid Mahdi (Medical Director of Dorrha hospital)
Dr/ Bushra Lobbad (Chief of PICU Rantisi Specialized Pediatric Hospital)
Clinical Pharmacist / Enas Al Gharably (Chief of Pharmacy in Dorrha hospital)
Dr/ Ayman Al Zahar (Chief of PICU in EGH)
Dr/ Essa Myziad (Chief of Pediatric department Aqsa Hospital)
Dr/ Tareq Al Daghma (Chief of Pediatric department Tahreer Hospital)
Clinical Pharmacist / Noor Al Zahar (Chief of Pharmacy in EGH)
Special thanks also to General Director of Hospitals in Gaza Strip
Dr. Mohammed K. Zaqout, and Dr. Ahmed Shatat for their valuable
contribution and support.
Deputy Minister
Dr Yousef Abu Al Reesh
Anaphylaxis
Sever life threatening generalized or systemic hypersensitivity reaction
(acute onset +one of the following criteria)
Criteria 1
Criteria3
Criteria 2
Mucocutanesous
manifestation+ 1of the
following systems
involvement:
-Respiratory system
-CVS (decrease BP )
Exposure to
known allergen
to that patient +
decrease BP
Exposure to likely allergen to
that patient +2 or more of the
following involvement
-Mucocutaneous manifestation
-Respiratory system
-CVS )decrease BP
-GIT system
ABC
Airway : Immediate intubation If evidence of impending airway
obstruction (due to angioedema)
If not Intubated
Consider Cricothyroidotomy, When Intubation Is Difficult
Epinephrine IM(1:1000)0.01mg/kg (max0.5ml) no absolute contraindiction
In mid anterolateral thigh
Can repeat every 5-15min as needed
Plus
Hemodynamic monitoring (HR,SPO2, BP)
Place in recumbent position , if tolerate and elevate lower extremities
Administer 100%O2, 2 large bore IV access 3 attempts within 5mint if
not . insert I.O line
IF Intubated Give
I.M Epinephrine
Quick emergency
doses of Epinephrine
IM (1:1000)
<6yrs→0.15ml
6-12yrs →0.3ml
>12yrs→0.5ml
Treat poor perfusion
Bolus of 0.9% NS 20 ml/kg (rapid infusion), reevaluate ,repeat as
needed (observe urine output )up to 60ml/kg. reassess every 10mint.
For bronchospasm (not responding to epinephrine )
Nebulized albuterol 0.15mg/kg (minimum 2.5mg) +3 mlNS
,repeat as needed+/-IPRATROPIUM. reassess every 10mint.
Consider :
Promethazine (IM.IV) 0.1-0.2 mg/kg.
Ranitidine IV (H2 antihistamine ) 1mg/kg (max 50mg)
Methylprednisolone IV 1mg /kg(max 125mg)
Call PICU
(FOR EPINEPHRINE
INFUSION +/- DOPAMINE).
Note PICU protocol
Cases refractory to Epinephrine , patients taking beta-blocker ,Consider : Glucagon IV 20-30mcg/kg over
5min(max cumulative dose of 1mg) followed by infusion 5-15mcg /kg (titrate to clinical effect(
Acute asthma exacerbations
HR/RR/O2Sat/accessory muscle usage/alertness/color/chest auscultation &grade the severity
mild
Moderate
Neb salbutamol 20min interval up to
3times
Assessment after 1 hr
Good response
observation for 1hr
Sever /life threaten
O2 by facemask (if o2 sat<95%)
Neb salbutamol + ipratropium 20min interval up to 3times
Assessment after 1 hr
Good response
observation for 1hr
O2 by facemask (if o2 sat<92%)
Neb salbutamol + ipratropium Br
continuously or hourly
I.M or SC epinephrine (0.01 mL/kg of
1 mg/mL solution; maximum dose of
0.4 mg or 0.4 mL) for patient with
poor aeration instead of
inhaled salbutamol and ipratropium
Poor response
IV. mag sulphate 25mg-75mg
Poor response
IV. mag sulphate 25mg-75mg
Discharge on
salbutamol
±oral prednisolone
+ the controller
treatment
Discharge on salbutamol
±oral prednisolone
+ the controller treatment
c
Poor respons
Poor response
Good response
observation for 1hr
Admission ICU
admission
Discharge on salbutamol
±oral prednisolone
+ the controller treatment
Aminophylline: 5mg/kg, IV (loading dose over 20 min at least) , then 0.7- 1mg/kg/hour .IV .infusion
Acute asthma exacerbations (classification):
PARAMETERS
MILD
MODERATE
SEVERE
LIFE THREATENING
Breathless
When walking
dyspnea
At rest
At rest
Talks In
Normal speak (sentences)
phrases
words
Unable to speak
(Infant stop feeding).
Alertness
Conscious
Usually, agited
Drowsy
confused/coma
(collapse)
Respiratory Rate
Normal –
mild increased
increased
Marked increased
Poor respiratory effort
Accessory Muscle No
Usage/Retractions muscle Retractions
muscle Retractions are
present
Intercostal-subcostalsuprasternal
retractions.
Paradoxical
thoraco-abdominal
movement
Wheeze
Mild respiratory Wheeze
Loud expiratory wheeze
bilateral
Usually
loud-biphasic
inspiratory
&Expiratory wheeze.
Silent chest
(Sever wheeze due to airway
obstruction).
PO2
>95% on R.A.
92-95%
<92%
Marked hypoxia Cyanosis
< 92%
Pulse/Min
<100 Normal HR.
100-120
( >160 in infant)
(>120 in > 5yrs)
Bradycardia due to sever
hypoxia
Bleeding
•
•
•
•
ABC's, O2
Assess hemodynamic status (HR, BP+ Orthostatic changes ,capillary refilling time(CRT )+ temp)
IV access (2 large bore cannulas) or IO
Lab CBC coagulation, RFT, LFT, Electrolytes & glucose ,group & cross matching
Hypovolemic shock
•
•
•
Iv fluid bolus of crystalloid (0.9% NS) or Ringer lactate ,20ml/kg over5-20min
May be repeated up to 3 times if no improvement and no signs of fluid overload
Not improved
Improved
Evidence of hemorrhagic shock and unidentified source
of bleeding (should undergo immediate further
assessment):
• Give 10ml /kg PRBC and definite treatment of cause
or give another bolus PRBC untill HB above 10g
• Source of bleeding: Sonography if hemodynamically
unstable, CT if hemodynamically stable
• Extent of bleeding: serum Hct, lactate, base deficit
- Monitor
Central & peripheral
Pulse, skin
Perfusion, BP
Mental status, urine
out put
Continue IV fluid (0.45%NS, D5%W
+/- KCL, guided by electrolytes)
Maintenance +deficit
•
Other Specific Managment
Upper GI Bleeding
•
•
•
•
•
•
NPO, NG tube insertion +/- gastric
Levage 3-5ml/kg of room temp NS
Stop NSAIDs or any ppt drugs
PPI omeprazole 1.5-2mg/kg /day
divided 6-8 hrly
Consult Gastroenterologist
+/- Octreotide if known or suspected
esophageal varices : initial IV bolus1-2
mcg/kg then continuous infusion 12mcg/kg/hr (taper dose by 50%
every 12hrs when no active bleed for
24hrs
Endoscopy within 24-48hrs, if
acute/ sever upper GI bleeding
requiring blood transfusion (after
patient stabilized)
Coagulopathy
•
•
•
•
•
•
•
•
Consult hematologist +/- Surgeon
Replacement therapy indicated if active bleeding ,invasive
procedure or at risk of bleeding complication
Red blood cells: 10-20ml/kg
Plt transfusion ( for plt < 50x109 or plt function disorder )
< 15kg→1UNIIT/5kg B.Wt
≥ 15kg→ single apheresis unit/ stander pool
FFP( for non-specific hemostatic failure , coagulation
deficiencies where no specific factor available)
→10-15 ml/kg infusion can be repeated every 12-24hrs
Cryoprecipitate (to correct clotting defect induced by
massive transfusion or DIC and hypofibrinogenemia
≤ 100 mg/dl →10ml/kg/infusion can be repeated 6 hrly
Vitamin K (for oral anticoagulation warfarin over dose or
prolonged PT/INR) → if significant bleeding non-life
threatening 0.5-2mg IM or IV
→If life threatening 5mg IV
Protamine sulphate: for heparin over dose →depends on
time since last heparin administration 0.25-1mg of IV
protamine may given
Avoid NSAIDs, IM injections & arterial punctures
Bronchiolitis
Risk factors sever disease
Prematurity (GA<37 wks)
Age < 3months
BPD patient
Congenital and anatomic
defects of the airways
CHD
Immunodeficiency
Neurological disease
Definition it is an inflammatory disease of terminal
bronchioles most commonly due to viral disease
Occur in children < 2yrs
Check for risk factor for sever +/- complicated bronchiolitis
Assess Severity
Mild
None or end exp .wheeze
Normal feeding
No oxygen requirement
No/mild chest indrawing
Normal behavior
No apnea
Moderate
Entire expiration wheeze
Less than usual,
frequently
stops feeding , or more than half
normal feed volume
May require oxygen
Intercostal / supraclavicular
retraction
Some intermittent irritability
No apnea
Trial of Nebulized 3% Saline or Salb. Neb
Meets discharge criteria :
RR< 60 breaths/min
SpO2>94% on RA
Adequate oral intake
(at least >75%of
usual intake(
Sever
-Inspiration & expiratory
wheeze
-Feeding : not interested , less
than half normal Feeds
-gasping / coughing
-Require oxygen
-Sever with nasal flaring
-Irritability /lethargy /toxic
-Possible apnea
<3 MONTHS
NO RESP.
YES
Discharge home
saline nasal drops
with nasal bulb
suction prior to
feeding
Admit
ABGS
Monitor HR,RR,BP,SpO2
Blood gas analysis
Urine test if febrile
Supplemental O2 (Maintain
SpO2 > 92%)
Saline nasal drops with nasal
suction prior to feeding
e
(external OR bulb)
Feeding:
-Assess level of hydration
-Hold oral feed if RR> 60/min, swallow ing
dysfunction, copious oral secretion
-Consider NGT feeding
-Consider I.V fluid D.S
with regular assessment every 4 hrs
Hypoxemia (despiteO2)
Hypercapnea ( pCO2
>55 mmHg ,<7.33 Kpa )
Apnea
Consider
PICU
Salbutamol Neb.(Trial)
- 2.5mg<20kg
- 5mg>20kg
- Dilute in 2.5-3ml NS Over 5-15 mints
Trial hypertonic Saline 3% ( 3ml ) Neb .
Evaluate after 1 hour
1-1000 Epinephrine (Trial of 1 dose):
2.5 mg / dose (diluted in ml NS )by o2
mask
Evaluate after 1hr
D/C if NO response
NOT Responded
Continue Salbutamol Neb OR
HTS 3% Neb. According to
response
Pediatric Cardiac Arrest
Shout for help – Activate Emergency Response
1
Start CPR
Give oxygen , Attach monitor/ Defiblrilator
Rhythm Shockable ?
yes
2
No
9
VF (ventricular fibrillation)
VT )ventricular tachycardia(
Asystole / PEA )plusless
electrical activity(
3
1st
Shock 2-4kj/kg
10
4
CPR (2 min)
•IO /IV acess
•Epinephrine every 3-5 min
•Consider Advance Airway
CPR (2min)
IO /IV access
Rhythm Shockable ??
Rhythm shockable
?
Yes
No
5
yes
11
CPR (2 min)
Treat reversible
cause
2nd Shock ≥ 4J /kg
6
NO
Subsequent shocks : 4J /kg
Rhythm shockable ?
CPR (2 min)
•Epinephrine every 3-5 min
•Consider Advance Airway
yes
Go to 5 or 7
12
Rhythm Shockable ?
7
No
yes
Subsequent shocks ≥ 4 J /kg
❖
❖
❖
8
CPR (2 min)
•Amiodarone or lidocain
•Treat reversible causes
Reference, Nelson 20, Up to date 2021
❖
❖
NO
•Asystole /PEA → GO TO 10 OR 11
•Organized Rhythm → Check pulse
•Pulse present ROSC (retain of spontaneous
circulation) POST cardiac arrest care
Epinephrine IO/IV: 0.01mg/kg (0.1 ml /Kg OF 1:10000)
Endotracheal dose 0.1 mg /kg (0.1 ml /kg 1:1000)
Amiodarone IO/IV:5 mg/kg bolus during cardiac arrest
may repeat up to 2 times for refractory VF/ pulse less VT
Lidocaine IO/IV initial 1mg/kg as loading dose then
maintenance 20-25 mg/kg/mint
Reversible causes(H& Ts) hypovolemia,
hypoxia,hydrogen ion (acidosis) hypoglycemia ,hypohyperkalemia ,hypohermia, tension pneumothorax,
Tomponade,toxins,thrombosis ,(coronary ,pulmonary )
Comatose Child
Definition :Profound state of alteration of consciousness in which a person appears to be a sleep
and cannot be aroused , it implies bilateral hemispheric ,cortical dysfunction or brain stem ,
reticular activating system dysfunction.
Stabilize C-spine
(if suspected trauma) Neck Collar
• Ensure ABCS 100% Oxygen
• (Intubation if GCS <8 or Resp. failure )
• PULSE Oximetry – Monitor BP
• Check bedside blood glucose
• IV. access
• Control temperature
Urgent investigation
• CBC , ABGS
• Electrolytes (Ca ,K ,Na ,Mg)
• RFT, LFT
• Cultures
• Metabolic screen tests (ammonia level)
• Drug screen (Toxicology screen )
If suspecting seizures
(convulsive or non convulsive)
-Give Midazolam, 0.2mg/kg
IV(Max 5mg / Dose )
OR
-Phenytoin 15 - 20 mg/kg loading
over 20 min
-Refer to Status Epilepticus
algorithm
Indication for CT brain
Suspected trauma
Fever / bleeding disorder
Focal neurological deficit / ICP
Suspected intracranial mass
Consider rapid MRI if available
If Hypoglycemia (RBS<50 mg/L in
Comatose child :
Collect critical sample(insulin
cortisone ,GH ,C peptide , ketone
in urine )
Immediately give bolus Dextrose
10%: 2.5 ml/kg IV over 5-10 mint
DO NOT delay treatment
Waiting for results
Refer to hypoglycemia: algorithm
IF known or strongly suspecting
Opioid Toxidrome (Miosis,
Respiratory depression
,hypotonia )
Give Naloxone 0.1mg /kg in
children <20kg
or < 5yrs(Max 2mg)
If suspecting ICP
• Treat the fever
• Elevate head of the bed 30◦
• moderate hyperventilation
( Target PaCO2 30-35 mmHg
Arterial)
Dexamethasone 0.6mg/kg
/day ÷6hrs
• IV Mannitol 0.25-1g /kg
Or IV 3% NS 3-5 ml/kg over
20-30min )
Consider CT if patient is in
stable condition .
Neurosurgery
If Suspecting
Meningitis/Encephalitis
• Give Ceftriaxone100mg/kg
day in 1 or 2divided doses
(max4 g/day ) OR
Cefotaxime(250-300 mg)/kg
/day in 4 divided doses
• Vancomycin 60mg/kg
/day in 4 divided dose
Dexamethasone
0.6mg/kg / day in 4
divided dose
• +/- Acyclovair 60mg/ kg/
day in 3 divided doses
• DO NOT delay antibiotics
waiting LP
Adjunctive therapy
• Correct acid- base imbalance
• Thermal regulation(35˚-36˚c)
• H2 blockers (for Stress Ulcer )
• Ophthalmic lubricant (protect cornea)
• Mouth care
Protocol of Dehydration
Indications for Admission (2)
Signs of Dehydration
Mild
(1)
Degree of Dehydration
Severe
(3)
Moderate
• ORS 100 ml/ kg over 4 hours.
• Replace ongoing losses: 10
ml/kg after each episode.
• Continue age-appropriate diet.
Note: If ORS is not tolerated, IV 10
cc/Kg/hr/ for 4 hours should be given
as:
- infant: ½ NS glucose 5%
- Older child: NS glucose 5%
• and reassess and treat accordingly.
Isonatremic
1. Shock therapy 20cc/kg Normal saline
over 20m.
Can be repeated till signs of shock resolve.
2. Calculate the deficit:
Degree of dehydration x10x weight.
3. Subtract the shock therapy.
The remaining amount should be given over
the1st8hours.
Type of fluid:
• Infant: ½ normal saline glucose 5%.
• Older child: normal saline glucose 5%.
Check k level and manage accordingly.
4. Maintenance fluid should be given over
next-16hours.
Type of fluid 0.18 glucose saline
5. Replace ongoing losses by ORS 10cc/kg.
Note: Reevaluate every 4-6 hours. (Clinical
and lab).
Hyponatremic
Hypernatremia (4)
• The same as isonatremic dehydration.
• Na level measurement should be done
after giving the deficit.
• More Na should be added to
maintenance (using 23.4% NaCl) or
normal saline according to this
equation:
(Na desired – Na level) x 0.6 x weight.
• Or the maintenance fluid should be
given an glucose NS.
Note: In symptomatic hyponatremia:
4ml/kg NaCl 3% is given over 15 mins
and can be repeated to maximum
(12ml/kg/24hrs)
Signs of Dehydration (1)
INFANT
Child
Mild dehydration
(<5%)
(<3%)
Skin color
Unchanged
Unchanged
Extremities
Eyes
Warm
Not sunken
Warm
Sunken
Cold
Sunken
Moist
Dry
Very dry
Breathing
Normal
Fast
Deep and rapid
Peripheral pulse
Normal
Normal
Weak
Skin turgor
Blood pressure
Urine out put
Normal
Normal
Normal
Reduced
Normal
Oliguria
Lost
Hypotension
Anuria
Heart rate
Capillary refill
Consciousness
Normal
Normal
Alert
Fast
Normal
Irritable
Very fast
Prolonged
Unresponsive
Mucous Membranes
•
•
•
(3)
ORS 50 ml/ kg over 4 hours.
Replace ongoing losses: 10
ml/kg after each episode.
Continue age-appropriate diet.
Note: If ORS is not tolerated, IV 10
cc/Kg/hr/ for 4 hours should be given
as:
- infant: ½ NS glucose 5%
- Older child: NS glucose 5%
and reassess and treat accordingly.
Moderate dehydration
(5-10%)
(3-6%)
Severe dehydration
(>10%)
(>6%)
Pale/ mottled
(2)
❖ Age < 6 months.
❖ Prematurity or chronic illnesses
❖ Fever > 38 c if younger than 3
months or > 39 if the age 3-36
months.
❖ Persistent vomiting or bloody
diarrhea.
❖ Evidence of severe dehydration.
❖ Metabolic acidosis or electrolyte
imbalance.
• Normal blood pressure in presence of
other signs of hypoperfusion doesn’t
rule out severe dehydration
(4)
• Restore intravascular volume: 20 ml/kg over 20 minutes can be repeated.
• Give the typical fluid Dextrose 5 % ½ N. Saline
Typical Rate 1¼ 1 ½ times maintenance according to Na level:
Na level: 158170: 1 ½ maintenance
171183: 1 ⅓ maintenance
183196: 1 ¼ maintenance
• Repeat Na level measurement after 4 hours
▪ If rapid drop in Na level (> ½ meq/h) :
Either ↓ the rate or ↑ the concentration to N.S glucose 5%
▪ If slow drop in Na level (< ½ meq/h) :
Either ↑ the rate or ↓ the concentration to 0.18 saline glucose 5%
Note : How to prepare ½ NS glucose 5 % either by:
• 6 cc hypertonic saline 23.4% is added to 500cc glucose saline.0.18 OR
• Mix glucose 10% with Normal saline (equal volumes) .
Note : If convulsion occurred during infusion 4 ml Kg Nacl 3% over 15 Minutes.
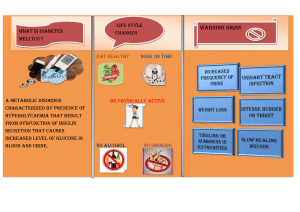
ALGORITHM FOR THE DIABETIC KETOACIDOSIS MANAGEMENT IN PEDIATRICS
Assess dehydration
Smell of Ketones
Lethargy , drowsiness
Deep sighing respiration
Polyuria
Polydipsia
Weight loss
Abdominal Pain
Weakness
Vomiting
Confusion
1st hour
Biochemistry :
Clinical signs
Clinical history
Confirm diagnosis = DKA
(inform senior staff immediately)
Elevated blood glucose > 200mg/dl
Acidemia (PH< 7.3)
HCO3 < 15 mmol /L
Ketone in urine or blood
Electrolytes
True Na+ level (1)
Calculate Anion gap.
Serum Osmolality.
Perform other investigation if
indicated ( sepsis?)(7)
Resuscitation
keep NPO, Airway ± NG tube (if vomiting / unconscious)
Breathing (100%O2 ), (if necessary).
Circulation (10ml/kg 0.9% NS over 30 minute, can be repeated
2 doses until circulation restored).
Admission to PICU
Next hours till resolution
I.V fluid : ( calculate fluid requirement)
Fluid requirement/hour = 85ml/kg + maintainance – bolus
23 hours
Give calculated fluid using two bag system. (2)
0.9 % NaCl for 12 hour unless hypernatremia (consult call), then 0.45 % NaCl .
Add KCl (3)
Insulin by I.V continuous infusion (4)
No
improvement
Deterioration
Observation
Vital signs
ECG- monitoring
Blood sugar, neurological status, fluid input/ output (
hourly).
Electrolytes 2 hour after starting I.V therapy, then 4 hourly
Amount of administered Insulin/Hour
Re-evaluate :
Fluid balance + I.V-therapy(8)
Check insulin dose delivery
system
If continued acidosis, may
require further resuscitation
fluid(9)
??Hyerchloremic metabolic
acidosis. (10)
Consider sepsis
Blood sugar < 300 mg /dl
Neurological
Deterioration (5)
Exclude
Hypoglycemia.
Is it
I.V- Therapy
IV fluids therapy by two bag system
Consider reducing insulin, ( only when pH≥7.3,
or blood sugar < 150 mg /dl, despite addition of
Glucose 10%).
Insulin :
- Start SC. Insulin then
stop IV insulin after:-
Resolution of DKA
Clinically well, tolerating food.
No emesis.
PH ≥ 7.3
Na =135-145 meq/l
HCO3 ≥ 15 meq/l
30 minutes with rapid
acting insulin
1 hr with regular Insulin
3/2023
النصر-مستشفى الرنتيسي لألطفال
Cerebral oedema ??
Management
Give mannitol (6)or 3%
hypertonic saline
Call senior staff .
Restrict I.V fluids by half.
CT- scan when stabilized
ALGORITHM FOR THE DIABETIC KETOACIDOSIS MANAGEMENT IN PEDIATRICS
1- True Na+ level
2-
= Measured Na + 2 x
serum glucose - 100
100
Two bag system:
Bag 1 “ saline bag “ contains only saline ± KCl .
Bag 2 “ Glucose Bag” contains dextrose 10% with the same electrolyte composition as bag 1
Table 1 . Two bag system protocol applied for fluid management in DKA.
Blood glucose
(mg/dl)
%O hourly IVF rate from
bags without dextrose
%O hourly IVF rate from the
bags with D 10
Final dextrose
Concentration
More then 300
250-299
200-249
150-199
100-149
a
Less than 100
100% of hourly rate
75% of hourly rate
50% of hourly rate
25% of hourly rate
0% of hourly rate
0% of hourly rate
0% of hourly rate
25% of hourly rate
50% of hourly rate
75% of hourly rate
100% of hourly rate
100% of hourly rate
0% dextrose
2.5% dextrose
5% dextrose
7.5% dextrose
10% dextrose
10% dextrose
3- KCI infusion rate
Serum K level
KCl dose in infusion fluid
meq /Kg body wt. over one hour
<2.5 meq /L
2.5 – 3.5 meq /L
3.5 - 5 meq /L
5 -6 meq /L
10 meq /L
Over 6 meq /L
4- Regular insulin dose: (continuous IV. Infusion) : 0.1 u/kg/hour for all patients, except patient ≤ 2 years
old ( 0.05 u/kg/hour).How to prepare: R.insulin 50U/50ml NaCl 0.9% in syringe pump then flush the tube before
administration).
5- Neurological deterioration (Warning signs):
Headache, Irritability, Slowing heart rate, Reduced conscious level, Incontinence, Depressed respiration,
Rising blood pressure, Decreased O2 saturation, Apnea, Seizure, Rapidly increasing of serum Na level
6- Mannitol dose:
0.5-1.0 g/kg stat ( 2.5-5 ml/kg of mannitol 20% ) I.V over 20 min. A repeated dose may be required after 2
hour if there is no response.
7 -Start antibiotics in febrile patients after obtaining the appropriate septic workup.
8- Urinary losses may be replaced with equal volumes for urinary output exceeding (5ml/kg / hr) and there is negative
balance of input output .
9- Sodium Bicarbonate (NaHCO3) :
Administration of NaHCO3 is not recommended except for treatment of life threatening hyperkalemia or
unusual severe acidosis (venous pH<6.9) with evidence of compromised cardiac contractility.
10- Hyperchloremia :
If ratio of Chloride: sodium > 0.79
Base excess due to chloride = (sodium – chloride) – 32
Chloride load can be reduced by: Not giving K+ as KCl and Using fluids like R. Lactate
3/2023
النصر-مستشفى الرنتيسي لألطفال
Drowning
Drowning : Primary respiratory impairment from immersion in a liquid medium .
Symptomatic (pre-hospital OR ER)
Asymptomatic
Observe for 8 hrs , then
Remove from water and resuscitate (ABCD)
o Open airway and give 2 rescue breaths
o If no response to delivered breaths , immediately begin high – quality
CPR
o In hypothermic(check for pulse for at least 1 minutes) before starting
compression
o Continue CPR according to BLS/PALS algorithm
o C spine immobilization NOT routine unless suspect injury (teens, diving
in shallow water ,motor vehicle crash)
o High flow supplemental O2 by face mask if victim is breathing ; Intubate
if apneic
o Wet clothing should be removed and wrapped in a warm blanket
o Continue resuscitation until temp 32-35◦C
o Avoid abdominal thrusts
o Obtain details of incident ,submersion time ,symptoms if possible
discharge if stable vital signs
and normal initial investigation
Serial monitoring of :
Vital signs, spO2, GCS
Respiratory and CNS Examination
Investigation:
Initial : BGAs, blood glucose ,
electrolyte , CXR, ECG
Secondary : CBC,BUN, Creatinine,
coagulation profile, C.K , troponin+/drug levels (according to
circumstances)
Addmition pt if has significant hypoxia ,apnea, still need O2 Support, arrhythmia , CPR, moderate to sever
hypothermia , abnormal chest x -ray or arterial blood gasses .
Airway and breathing
-Consider CPAP
-Intubate if (apnea, cyanosis, inability to
protect the airway due to altered mental status
hypoventilation or labored respiration persists
despite the administration of 100% O2 by bag
mask SpO2< 90% or PaO2<60 mmHg despite
supplemental O2 , or PaCO2>50mmHg )
-If you intubate ,insert an NGT or OGT ( if
facial injuries) to decompress the stomach
-Neb Salbutamol for bronchospasm
-Antibiotics if pneumonia or submersion in
grossly contaminated water
Circulation
-Obtain large pore IV access
-Cardiopulmonary monitor(long
QT interval)
-Asses pulse BP, CRT
-Fluid bolus if hypovolemic 20
ml/kg ( N.S )
-Inotropic support IF need
according to ECHO .
Hypothermia (temp <35◦C )
-Remove wet clothes
-Passive rewarming (temp > 32◦C)by dry blankets or any
insulators, warm environment (up to35◦C)
-Active external rewarming (temp <32◦C ) warm blankets, heat
lamps ,forced warm air (goal 32-35◦C)
-Active internal rewarming (temp<32◦ intact circulation ) by
heated humidified O2 ,, warm IVF (shortest I.V tubing to assure
efficacy) ,,gastric or bladder lavage, pleural & peritoneal
irrigation with warm saline ,hemodialysis
-Cardiopulmonary bypass ,ECMO if absent circulation ( if
available)
-Warm trunk first if using active rewarming
Neurology
-AVPU , GCS, Pupillary response
-Continuous reassessment CNS
-monitor cerebral edema or increase ICP
(elevate head of bed at
30%,hyperventilation arterial PCO2(3035),fluid restriction to 75%of
maintenance)
-Treat seizures ( phenytoin 10-20mg/kg.
loading dose , levels should be
monitored )
-Maintain euglycemia (80-110mg/dl)
Poor prognosis
-Submersion> 5 min
-time to effective BLS > 10 min
-Resuscitation > 30 min
-Water temp> 10 C
- Age < 3 years
-GCS < 5
-Persistent apnea and need of CPR in
ER
-Arterial blood PH < 7.1 on
presentation
Febrile Convulsions protocol
History
Examination
➢
➢
➢
➢
ABC.
O2 support.
Vascular access.
Termination according to
protocol of convulsion.
Counsel parents about risk of
recurrence and how to provide first
aid and manage fever.
MAJOR:
➢ Age < 1year(X8).
➢ Duration of fever <24 hr (X17).
➢ Fever 38-39 Co (100.4- 102.2 Fo)
(X17)
MINOR:
➢ Family history of febrile
seizures (X7).
➢ Family history of epilepsy.
➢ Complex febrile seizure.
Lab. Test
Manage:
*LP??
Determine risk factor epilepsy
High Risk
➢ Neurodevelopmental
abnormalities 33%
➢ Complex focal
febrile seizures 29%
➢ Family history 18%
of epilepsy
Low Risk
➢ Fever <1 hr before
febrile seizure.
➢ Complex no focal
➢ >1 complex feature
➢ Recurrent febrile
seizures.
➢ Simple febrile seizure
➢ Late onset febrile
seizure > 3 years old
➢ Consider EEG
➢ Consider Imaging
No further management.
Definition:
A convulsion associated with temperature 38⸰C or higher.
Age between (6 months. – 5 years).
Absence of central nervous system infection or inflammation.
Absence of acute metabolic abnormality that may produce convulsion.
No history of previous a febrile seizure.
Simple
Brief ( < 15 minutes )
one attack/24hours.
Generalized tonic – clonic convulsion.
Brief post ictal state.
Complex
Long (>15 minutes)
Repeated convulsions within 24 hours.
May be focal, or generalized.
Long post ictal state.
History:
Seizure characteristics (type, recurrence, post- ictal state) duration, and presence
of focal findings.
History of neurological problems or developmental delay.
Family history of seizures.
Physical examination:
General examination, vital signs.
Complete detailed neurological examination.
Laboratory test:
1. CBC, serum electrolytes, blood sugar, calcium, and urea should be measured.
2. LP should be done for:
Infants (<1 year age)
Clinical features suggest a possible meningitis or intracranial infection.
3. LP to be considered for (clinical judgment, senior decision):
If febrile seizures occur after 24hr of illness.
The patient is on antibiotics.
Infants 12-18 months.
Febrile status epilepticus
Imaging:
Focal convulsion.
Any neurological defect.
Signs of increased intracranial pressure
EEG:
Patient with high risk of epilepsy
Febrile infant (29-90 days)
Axillary temp ≥ 38◦c
Ill appearing
Admit
Well appearing
(previously healthy term infant without prenatal
complications)
Signs of
Septic shock
✓
✓
✓
✓
✓
✓
✓
✓
ABCS
CBC, BLOOD C/S ,CRP
ABG & chemistry
Urine routine & C/S(by
catheter/suprapubic)
CSF examination
CXR if any Respiratory
Symptoms
Stool C/S if diarrhea
Ammonia ,lactate ,DIC
screen
Referred to
septic shock
algorithm
✓
✓
✓
To streptococcus pneumonia
H .influenza Neisseria
Meningitidis
✓
✓
✓
✓
✓
✓
✓
CBC, blood C/S
Urine routine & C/S (By
catheter / suprapubic) if
available
CXR if any Respiratory
Symptoms
CRP
Stool C/S if diarrhea
Low risk
✓
Antibiotics coverage
✓
✓
Cefotaxime or ceftriaxone
Add Ampicillin (if < 60days)
Add VANCOMYCIN (IF soft
tissue infection or CSF
pleocytosis
WBC 5000 TO
15000/microl
Absolute band
count <1,500/microl
UA <10WBC/hpf +
No bacteria seen
Others if obtained
No infiltrate in CXR
if done
Stool < 5WBC/ hpf
if diarrhea
High risk
✓
✓
✓
✓
✓
WBC < 5000 OR
>15000/microl
Absolute band
count ≥ 1500/
microl
UA >10 WBC/ hpf
or bacteria seen
Other if obtained
Infiltrate in CXR IF
DONE
STOOL >5 WBC
/hpf
F/U cultures & clinical
status within 48hrs
Admit
LP (collect CSF sample)
Discharge after 72 hrs if :
A febrile , all Cultures –ve, good general
condition, good feeding & CRP -ve
Cefotaxime or
ceftriaxone
Febrile Neutropenia Low risk
Transient isolated Febrile Neutropenia in otherwise healthy child
1,000 to 1,500/mcL
500 to 1,000/mcL
<500/mcL
(1.0 to 1.5x109/L) Mild
(0.5 to 1.0x109/L) Moderate
(0.5x109/L) Severe
Viral
Viral
Bacterial pneumonia,
Bacterial: URI
systemic
(sinusitis, purulent
systemic
rhinitis), otitis
symptoms, GU
rhinitis), otitis
symptoms, GU
media, local skin
infections,
media, local skin
infections,
lymphadenitis
infections
lymphadenitis
Bacterial: URI
(sinusitis, purulent
Supportive
Assume bacterial
Bacterial pneumonia,
infections
Supportive
Blood cultures
PO antibiotics
- Blood cultures
And
-specific cultures,
according to clinical course
Follow up
- Best estimated antibiotics
Blood culture
CRP
Urine culture
LP if CNS INFECTION
SUSPECTED
Parenteral broadspectrum antibiotics
-Blood cultures
Specific cultures
**
-specific cultures,
according to clinical course
parenteral broadspectrum
mono-duotherapy
±
vancomycin
- Best estimated antibiotics
antibiotics
Acceptable empiric monotherapy regimens include one of the following(**)
•
•
•
•
Cefepime 50 mg/kg (to a maximum of 2 g per dose) intravenously (IV) every eight hours
Meropenem 20 mg/kg IV every eight hours (maximum of 1 g per dose)
Piperacillin-tazobactam (dosed according to the piperacillin component 100mg/kg every 6 hours)
Ceftazidime 50 mg/kg IV every eight hours (maximum dose 2 g) AND amikacin 15 mg/kg once daily,
amikacin can be stopped once cultures results negative.
• Ceftriaxone 75 – 100 mg /kg
• Reasses after 3 days , follow Blood culture result
Vancomycin indications , to be used in severe neutropenia if one of the following present :
•
•
•
•
•
Severe mucositis
Quinolone prophylaxis
Colonized with Methicillin – resistant staphylococcus aureus
Obvious catheter related infection
Hypotension
Reassess after 3 days
Prepared by : scientific committee , Al- Ranteesy –Nassr hospital
Fever without focus (3-36months)
This algorithm for children who are Immunocopmpetent , with
fever ≥ 39◦c ( rectal )of duration <7 days and NO focus
Ill appearing
Well appearing
Admit
Full history and careful examination
(previously healthy term )
Full septic work
DO NOT delay antibiotics
Incomplete vaccination
Complete Vaccination
(Hib+ pneumococcal vaccines)
3-6months
(at least 2doses Hib vaccines +3 doses
pneumococcal vaccines) 3-6months
Risk of bacteremia <1%
Risk of Occult bacteremia 5%
5%5%
Investigations
–CBC with differential
–urine routine(UA)and culture
NO Routine blood labs are recommended
UA
Treat as
UTI
Positive
Low risk
Normal investigations
Follow up after
24hrs (if follow up
uncertain , admit
the infant)
High risk IF:
WBC ≥ 15000/microl
Collect Blood culture If :
WBC ≥15000/microl (practical: you can
collect blood c/s with CBC and to send
it if WBC ≥15000)
-CXR if
WBC >20000
abnormal CRX
Give ceftriaxone IV,IM 50 mg/Kg
pending culture results
If allergic to cephalosporine
-Clindamycine IV 10mg/kg follow
by oral clindamycin 8hrs later
References
Nelson 20
Up to date 2021
Kuwaiti guideline 2018
Risk of UTI
Indication of urine analysis and C/S :
•
•
•
•
•
•
Girls ≤ 2 years
Boys (uncircumcised) ≤ 12month
Boy (circumcised) ≤ 6month
Fever > 48hrs
Previous history of UTI
Urogenital anomalies
Yes
Do urine R/M&C/S
Bag specimen Should
NOT be sent for culture
Not indicated
Follow –up after
48hrs
If still persist fever
reevaluate to
identify the fever
focus
Fever without focus (3-36months)
This algorithm for children who are Immuno-competent , with
fever ≥ 39◦c ( rectal )of duration <7 days and NO focus
Ill appearing
Well appearing
Admit
Full history and careful examination
(previously healthy term )
Full septic work
DO NOT delay antibiotics
Incomplete vaccination
Complete Vaccination
(Hib+ pneumococcal vaccines)
3-6months
(at least 2doses Hib vaccines +3 doses
pneumococcal vaccines) 3-6months
Risk of bacteremia <1%
Risk of Occult bacteremia 5%
5%5%
Investigations
–CBC with differential
–urine routine(UA)and culture
Low risk
Normal investigations
Follow up after
24hrs (if follow up
uncertain , admit
the infant)
UA Positive
Treat as
UTI
High risk IF:
WBC ≥ 15000/microl
Collect Blood culture If :
WBC ≥15000/microl (practical: you can
collect blood c/s with CBC and to send
it if WBC ≥15000)
-CXR if
WBC >20000
abnormal CRX
Give ceftriaxone IV,IM 50 mg/Kg
pending culture results
If allergic to cephalosporine
-Clindamycine IV 10mg/kg follow
by oral clindamycin 8hrs later
NO Routine blood labs are recommended
Risk of UTI
Indication of urine analysis and C/S :
Girls ≤ 2 years
Boys (uncircumcised) ≤ 12month
Boy (circumcised) ≤ 6month
Fever > 48hrs
Previous history of UTI
Urogenital anomalies
Yes
Do urine R/M & C/S
Bag specimen Should
NOT be sent for culture
Not indicated
Follow –up after
48hrs
If still persist fever
reevaluate to
identify the fever
focus
PAEDIATRIC PARENTERAL FLUID THERAPY (1 month-12 yrs)
ADMINISTER RAPID FLUID BOLUS
Monitoring & Observations Essential
Admission
Weigh.U&E
ALL
CHILDREN
12 Hourly : Assess In /Out put, plasma glucos
➢
➢
➢
➢
Yes
Is shock
present?
s
Give 20 ml/kg sodium chloride 0.9% IV or intraosseous over 20 minute ………. Reassess
Repeat bolus if needed(up to 60-80 ml/kg) __ Consider third bolus in ICU area
Call for senior help
Colloids may be needed
Daily-Clinical reassessment:.
No
U&E(more often if abnormal;4-6 hourly if
Na+< 130 mmol/L
Prescribe O.R.S ( orally or by NG tube) According to level of dehydration and
tolerance
Can child be managed
with oral Fluids?
Severly ill children may need :
•
•
•
•
Hourly-HR. RR .BP, GCS
Fluid IN/Output(urine osmolarity if
volume cannot be assessed)
2-4 hourly –glucose, U&E,+/- blood gas
Daily-weight is mandatory
•
•
•
Yes
YES
Mild dehydration 30-50ml/kg over 4hr
Mod dehydration 50-100ml/kg over 4hrS
If not improved or not tolerated give I.V fluid
Yes
s
Is there a fluid
deficit?
Each shift : Handover and review of fluid
management plan
No
If plasma Na+ < 130 mmol/l or > 16mmol/L
or plasma Na + changes> 5 mmol/L in 24
hours ask for senior advice
•
•
•
•
•
•
•
Prescribe Maintenance
fluids
•
(Estimate deficit +maintenance) – shock bolus /24hrs
Fluid deficit= (%dehydration x kg x10) as mls of sodium chloride 0.45% + D5%
Estimate IV maintenance fluid see table CALCULATION OF 100% MAINTENANCE RATE
Fluid choices: sodium chloride 0.45% with D5 % (if not available can prepare)
Give over 24 hours (If Na < 135 or >145 mmol/l give over 48 hours )
Ongoing losses: calculate at least 4 hourly. Give (ORS or 0.45% + D5%) as 10ml/ kg for each diarrheal stool
or vomiting
Sodium chloride 0.45% (with or without pre-added potassium):can be prepared to change fluid type and
volume according to clinical reassessment, electrolyte losses and test results
Commence oral fluid & discontinue IV fluids as soon as possible
CALCULATION OF 100% MAINTENANCE RATE
➢
Weigt (kg)
daily
hourly
•
a
For first 10
100ml/kg/day
4ml/kg/hr
kg
b For second
50ml/kg/day
2ml/kg/hr
10 kg
c
For each kg
20 ml /kg /day 1 ml / kg /hr
over 20 kg
For 100% daily maintenance add together
(a)+(b)+(c)
➢
Patients particularly at risk of
hyponatremic complications:
Gastric losses; CNS infection; Sever sepsis;
Hypotension; Intravascular volume
depletion; Bronchiolitis; Gastroenteritis with
dehydration; Abnormal plasma sodium,
particularly if less than 138 mmol/L but also
when gets than 160 mmol/L salt wasting
syndromes
Alter fluid rate according to clinical
assessment. Change electrolyte and glucose
content of fusion fluid according
If risk of hyponatraemia is high consider
initially reducing maintenance Volume to
two thirds of maintenance
➢
➢
➢
➢
Hypokalaemia(<3.5 mmol/L): Check for initial deficit
.Maintenance up to 40 mmol/L, IV potassium usually need after
good urine output .
Oral intake and Medications: Volumes of intake, medications&
drug infusions must be considered in the fluid prescription.
Hypoglycaemia(<50mg/ dl): Medical Emergency give 4 ml/kg
bolus of glucose 10%. Review maintenance fluid, (consult with
senior and recheck level after 15-30 mins.,)
Symptomatic Hyponatraemia: check U&E if patient develops
nausea, vomiting, headache,irritability, altered level of
consciousness, seizures or apnea. This is a Medical Emergency and
must be corrected : Commence infusion of 3% sodium chloride
(4-6ml/kg) in a rate of 1ml /min and get senior advice immediately.
Guidelines for Inpatient Management of pneumonia
Community acquired pneumonia
1-3 months
Cefotaxime
+
Ampicillin
3-6 months
Cefotaxime
OR
Ceftriaxone
> 6 months
❖ Ampicillin,
Or
❖ Penicillin G,
Aspiration pneumonia
Hospital acquired pneumonia
pneumonia (Noscomia)
Aminoglycosides (Gentamycin or Amikacin)
Clindamycin
+
or
Ceftazidime
Aminoglycosides
If on response mecopenem
Cefotaxime ,
Or
Ceftriaxone .
❖ If there is only tachypnea.
If there are other signs of resp.distress.
Severe Pneumonia
3r d generation cephalosporin +
Azithromycin +
Vancomycin +
Oral zinc.
MEDICATION DOSES
❖
❖
❖
❖
❖
❖
❖
❖
❖
Duration of treatment IV antibiotic till a febrile for 2-3 days The total duration is 10 days.
Cefotaxime 150 mg /kg /day in 4 divided doses.
Ceftriaxone 50 – 100 mg / kg / day in 1-2 divided doses.
Ampicillin 150-200 mg /kg/ day in 4 divided doses.
Penicillin G 200.000 to 250.000 IU /kg in 4 divided doses.
clindamycin 40 mg / kg in 4 divided doses.
Azithromycin 10 mg/kg in the 1st day then 5 mg/kg for 4 days.
Vancomycin 40-60 mg / kg in 3-4 divided doses.
Zinc 10 mg/day < 12m, 20 mg/ kg>12m.
Indication of admission:▪
▪
▪
▪
▪
▪
▪
▪
Age < 6m.
Multiple lobe involvement.
Immune compromised.
Toxic appearance.
Mod to severe resp distress.
O2 sat < 92 %. On room air
Complicated pneumonia .
Failure of oral antibiotics.
Criteria of severe pneumonia:
✓ nonresolving symptoms after 48 hours.
✓ Resp failure.
✓ Complicated pneumonia.
Hydrocarbon Ingestion
Signs & symptoms:
Vital : fever at time of presentation 38 to 40ºC pyrogenic effect . If Persistence beyond 48 hours suggests
bacterial super infection
Respiratory : Choking , cough , wheeze ,↓SpO2,cyanosis , respiratory compromise & chemical pneumonitis
CNS: CNS depression, seizure ,euphoria , disorientation, hallucinations & coma
Cardiac: arrhythmia 2ry to ↑sensitization to endogenous ( + exogenous) catecholamine leading to VF
GI: Irritation of esophagus → causing GI bleeds& haematemesis
If symptoms presents admitt
presents
✓ External
decontamination remove
✓
✓
✓
✓
contaminated clothes ,cleanse
affected hair and skin, copious
water irrigation of eyes as
indicated
Ensure ABCs ,100% oxygen
Salbutamol if clinically indicated
Continuous cardiac monitor
NPO & IV fluids maintenance
Investigations
•
•
•
•
•
•
CBC (↑WBCs)
RFT , Mg , K , glucose , LFT (↑ ALT
,AST)
ABG (metabolic alkalosis , hypoxia ,
later acidosis)
Urine analysis
Serial CXR at presentation & ≥ 4 hrs
post exposure
ECG if (arrhythmia ,VF)
If Seizures
Give Diazepam or
Midazolam 0.1-0.2
mg/kg IV (max 5mg/
dose)
If no symptoms
Immediate
admission if:
• Symptomatic
• Suicidal intent
• Massive ingestion
AVOID active charcoal
and AVOID induce
emesis
(Risk of aspiration )
External decontamination remove
contaminated clothes ,cleanse affected hair
and skin, copious water irrigation of eyes as
indicated
Observe for 6 hours in the ED & repeat
CXR : IF
• Asymptomatic & normal CXR :
Discharge , appropriate instructions to
return if fever , tachypnea or cough
develop
• Asymptomatic & abnormal CXR : OPD
follow –up after 24 hours
• Symptomatic or cannot guarantee close
follow –up Admit to ward for
observation & supportive management
If Respiratory failure / CNS depression
Intubation with cuffed tube admit to PICU
consider nasogastric decontamination
If arrhythmia /VF
Correct electrolytes ( Mg ,K )
-If VF : refer to CPR algorithm
( CPR/Defibrillator)
Lidocaine 1mg/kg infusion
rate20-50mcg /min or use
ß -blocker
If Pneumonitis
Antibiotics if fever or leukocytosis 48
hrs post exposure or ↑CXR infiltrates
or positive sputum /tracheal bacterial
culture
Antibiotics should NOT be used
prophylactically
AVOID Epinephrine (cardiac
sensitization to catecholamine
→ arrhythmias
NB : corticosteroid should NOT be
used (has been associated with
↑morbidity )
Hyperammonemia
Clinical feature : Poor feeding ,lethargy , tachypnea, hypothermia, irritability
,vomiting, ataxia, seizures , hepatomegaly ,coma, hypotonia ,dehydration
+ Respiratory
alkalosis
consider UCD
Hyperammonemia
-Neonate >150 micg/dl
-Infant / Child >80 micg/dL)
+ Metabolic
acidosis
consider
organic
acidemia
-ABC, 100% O2,ventilator support as needed,
Cardiopulmonary monitoring , IV access, check RBS.
-Contact metabolic specialist, consider PICU
Confirm diagnosis : repeat immediately if S. ammonia >100 micg/dL)
Critical investigation :BGA, LFT, RFT,S/E ,LACTATE ,pyruvate ,plasma aminoacid +
acyclcarnitines, urine organic and oritic acid, culture ( blood, urine ,CSF as indicated)
Stop all protein intake (avoid withholding protein >48hrs)
IVF :D10% at 1.5xmaintenance rate+ intralipid 1-3 g/kg/day (via
central line ) to give 120- 130kcal /kg/day)
-IV Ammunol (phenylacetate + Sodium benzoate):
Loading dose (over 90min) : 250 – 500 mg/kg
Maintenance infusion : 250-500mg/kg/day (Loading & maintenance should be diluted in
25-35ml/kg D10% (IV maintenance used until oral form can be tolerated)
• DO NOT administer sodium in IVF while on IV ammunol
-Available Oral Sodium benzoate: Oral sodium benzoate (if patient tolerated)
Initially 250mg/kg … maintenance 250mg/kg/day divided 6-8hrs
-If suspected U.C.D added Arginine 250mg/kg/day once daily
-Cover the patient with broad spectrum antibiotics( as precipitation factor could be infection)
-Conceder Neomycin oraly 100mg/kg /day divided into 4doses
Monitor glucose , keep level around 100-145 mg/dl. if hyperglycemia ,DO NOT stop or ↓ D10%
If needed start IV insulin infusion at 0.01U/kg/hr , with adjustment to avoid hypoglycemia
Check serum ammonia 3 hrly
Ammonia rapidly ↑or resistant to initial treatment or>300-400 mic g/l→ hemodialysis or peritoneal dialysis
-Avoid glucocorticoids in immediate Mx Avoid depakine (valproic acid) if seizure
-Monitor for signs of brain edema &↑ ICP, Mannitol ineffective if case of urea cycle defect
Hyperkalemia( K>5.5)
•
•
•
•
•
Serum K+ 5 - 7mEq/L → patient Asymptomatic
> 7 mEq/L→ Muscles weakness , paralysis , cardiac changes on
ECG ,arrhythmias ,sudden arrest
stop all k supplements or drug that induce hyperkalemia
confirm true hyperkalemia (rapid analysis of venous or arterial non-hemolyzed
sample )
Obtain ECG, connect to cardiac monitor
CARDIAC MONITORING
Normal
ECG K =3.55.5
+
Abnormal
ECG K ≥ 6
mmol/L
Abnormal
ECG K> 7
mmol/l
Abnormal ECG
K >8 mmol/l
IF cardiac changes admitted to PICU
ECG changes ( Not tall T wave only)
•
Widening QRS complex
•
Loss of P waves
•
Sever arrhythmias
True K+ level > 7 mEq/L
Calcium gluconate 10% IV /IO 0.5 ml
/kg over 5 min (max 20ml)
• Onset of effect : Immediate
• If ECG Changes persist ,
Repeat the dose 1-2 times
every 10 mints
• Use large vein or central line
• Consider furosemide and
Sodium polystyrene sulfonate
plus
Regular insulin 0.1U/kg (max10units) +0.5g/kg
dextrose over 30 min ( 5ml/kg D10%)
• Onset effect :10-20 min
• Repeat the dose after 30 min if no
improvement
• Observe RBS ,if hypoglycemia↑ dextrose
• If arrhythmias or impending arrest ,use
larger doses(insuline0.2U/kg(+ dextrose
1g/kg)
Sodium bicarbonate 8.4%IV 1ml/kg (=1mmol/kg)
over 10-15min
• Onset of effect 15min
• Max single dose 50 mmol
• AVOID to administrate with the same Ca gluconate line
(potential for precipitation)
IF NO cardiac changes
Nebulized salbutamol x Q 20min
• Neonate 0.4mg +2ml NS
• <25kg : 2.5mg +2 ml NS
• 25-50 kg : 5mg + 2ml NS
• Onset of effect : 20-30min
Or use MDI 4-8 puffs with spacer
Furosemide (lasix )IV 1 mg /kg (max
single dose 40mg)
• Onset of effect 1-2 hours
• Replace fluid losses unless
patient is volume expanded
• May be repeated after 6 hours
Sodium polystyrene sulfonate (without
sorbitol) 1g/kg(max 30g)
• PO ,by NGT or Retention enema
• Onest: 1-2 hours
• May repeat dose 4-6 hours
• Contraindicated in preterm ,term infant
with intestinal hypo-motility,( if risk of
NEC ,post –op ,bowel obstruction or
ileus)
• Use Lactulose (to prevent colonic
impaction )
Hemodialysis
(+/-sever renal dysfunction)
Hypernatremia
Hypernatremia: Is defined as serum level Na >150mEq/L
Hypernatremia occurs when too much salt is ingested or too much free water is lost
It is essential to correct hypernatremia slowly over 48-84hrs .Most recommendations are to lower
serum sodium value no more than 0.5 mEq/L/hr or 12mEq/L/day.
D5%+1ൗ2NS with 20mEq/L KCL is an excellent choice of replacement fluid(as urine output is
adequate )( Add 9.6ml Nacl 23.4% to 500ml DW5% to prepare D5%+1ൗ2NS)
Sign and Symptoms:
•
•
•
Irritable, high-pitched cry, lethargy, seizures, fever, renal failure and rhabdomyolysis.
In infant, these symptoms mimic those of infections and sepsis.
BP could be normal early
Complication of condition: Cerebral hemorrhage
Complication of therapy : Cerebral edema and hyponatremic seizure
Management
•
•
•
•
In the child with hypernatremic dehydration, as in any child
with dehydration, the first priority is restoration of intravascular
volume with isotonic fluid
IF shock bolus used substract from total fluid
Typical rate = 125-150 ml/kg of ( D5% ,1/2 NS / 24hrs) _ shock bolus /24hrs
Monitor Na level Q 4 hr to check for targeted drop
Hypertension Crisis
Systolic and /or diasystolic BP ≥ 95th percentile adjusted For age
gender , and height measured on 3 or more occasions
History :
❖ Identify symptoms of end organ damage seizure or encephalopathy
papilledema and retinal hemorrhage or exudates , heart failure , renal insufficiency
❖ Identify symptoms suggestive of primary or secondary causes of HTN
❖ Exclude causes of HTN for which rapid reduction of BP might be harmful
(sever pain , intracranial injury or mass lesion causing raised ICP , coarctation of
aorta or ingestion of sympathomimetic agents)
Examination :
❖ Confirm BP by auscultation with proper cuff size and placement, take 4 limbs BP
❖ Examine for acute signs of end organ damage
❖ look for underlying causes of high BP
Investigation :
ECG, CXR , lab( CBC , Retics, RFT ,Electrolytes),urine microscopy
For specific cases : urine toxicology screen , CT head , ECHO, U/S Abd.
NB: for RX of HTN
emergencies and HTN
urgencies 2nd to an acute
underlying condition , the
goal is : to↓ BP by no more
than 25% over the first 8 hrs
to avoid irreversible end
organ damage.
Further BP reduction should
be gradual over 48 hrs
NB: for HTN
urgencies 2nd to a
chronic underlying
condition the goal is
to↓ BP over 1-2 days
Is there is evidence of end –Organ
damage??
NO
YES
HYPERTENSIVE EMERGENCY:
An acute severe symptomatic elevation in BP WITH
evidence of potentially life-threatening symptoms or
target organ damage
• ABC, IV lines 2x ,Admit to PICU for close obs,&
Monitoring , consider ped Nephrologists consult
• Give Hydralazine 0.2-0.4 mg/kg; max single dose
20mg q 4–6 hr and titrate to effect (max: 3.5
mg/kg/24 hr).
• OR : IV bolus labetalol 0.2-1mg; max single dose
40mg ( note : contraindicated in asthma ,BPD,HF
& may mask symptoms of hypoglycemia )
• After bolus, start IV infusion : labetalol 0.25 3mg/kg/hr
• OR Nicardpine 0.5-1mcg/kg/min titrate the dose
according to BP , increase infusion rate q 1530min
( max dose= 4 -5mcg/kg/min)
• Consider adding IV furosemide 1mg/kg bolus for
pts with volume overload
HYPERTENSIVE URGENCY: An acute severe
elevation in BP WITHOUT severe symptoms or
evidence of acute target organ damage
1. ABC , IV line, Admit to ward , Close
obs. , and Monitoring , consider peds
Nephrologists consultation .
2. Start Antihypertensive
For HTN urgency 2 nd to
an acute condition or for
pts who cannot tolerate
PO:
Give IV bolus of labetalol
OR hydralazine
Follow with PO
Antihypertensive (no IV
infusion needed)
For HTN urgency 2nd
to a chronic
condition and who
can tolerate PO:
Hydralazine
0.25mg/kg/dose(max
single dose =25mg)
every six to eight hrs.
HYPOCALCEMIA
Total serum Ca < 7.5 mg/dl
Ionized Ca < 3 mg/dl
Symptoms: lethargy ,poor feeding , vomiting ,abdominal
distension, twitching , tetany, seizures, apnea ,stridor,
laryngospasm
Investigations:
Total Ca ,ionized Ca ,Mg , phos, RFT,Albumin,ALP,PTH,
25-OH Vitamin D ,urine
Ca/ creatinine ratio, wrest X ray (if indicated)
ECG: Prolonged QT interval (>0.45 s)
Symptomatic
Correct hypomagnesaemia(Mg
< 1.6mg/dl )if persist give Mg
sulphate 50% IV /IM
0.2ml/kg/dose slowly {max
2ml/dose of (50% Mg
sulphate)= 1g /dose }
Hypocalcaemia may NOT be
corrected unless you correct
Mg level
Consider starting VitaminD
alfaclacidol one alpha drops
0.05mcg /kg/day (1
drop=0.1mcg)
Asymptomatic
(Seizure , laryngospasm, Cardiac ,dysrhythmia,
muscle spasm /cramp, tetany, carpopedal spasm )
10 % Ca gluconate IV (initial ) :
Oral Calcium
50-150mg/kg/day elemental Ca
divided in 4-6 hr (max 1000mg/day)
1 ml/kg 10 % Ca gluconate diluted to 2% solution (by mixing
each 10ml of 10 %Ca gluconate in 40ml NS or D5% ) Over 1015min
If symptoms persist can repeat the dose once .
NB: ( Max dose 20ml 10% Ca gluconate /dose)
Connect the patient on cardiac monitor
Must check the integrity of IV site
Consider central line if intractable
hypocalcemia and high dose calcium
needed to prevent local injury
Regimen 1 (boluses)
Regimen 2 (continuous infusion)
1-2ml/kg/dose 10 % Ca gluconate over 1hr XQ46hrs , diluted to 2% solution (as previous step)
( Max dose20ml 10%Ca gluconate /dose)
5-8ml/kg/24hrs of 10%Ca gluconate dilute
to 20% solution
Always connect to cardiac monitor
Always check the integrity of IV site
If HR <70 b/min persistently stop Ca gluconate
infusion and assess your patient
Check Ca level every 6 hrs
Titer the infusion according to Ca level
Check Ca level every 6hrs
Always connect to cardiac monitor
Always check the integrity of IV site
If HR < 70 b/min persistently stop Ca
gluconate infusion and assess your patient
لج
Hypoglycemia
RBS <60mg/dl in symptomatic patient
RBS ≤ 40mg/dl in asymptomatic patient
Clinical features:
Any patient with acute lethargy or coma
need immediate RBS checking
Infant irritability jitteriness, poor feeding , hypothermia, hypotonia ,tachypnea Cyanosis
,Apnea ,seizure
Older children
Autonomic response ,sweating ↑ HR palpitation ,tremor ,hunger, parasthesia,
ABC, 100%O2
Cardiopulmonary monitoring
If unexplained cause ,Recurrent & child is not known to have DM on Rx
obtain CRITICAL SAMPLE before treatment
5-10 ml blood for FFA's , pyruvte ,B –hydroxybutyrate , lactate , total / free
carnitine, acylcarnitine ,insulin, C-peptide , GH ,cortisol
Urine for ketones + reducing substances
But DO NOT delay treatment
Consciousness/ able to drink & swallow
safely
Rapidly absorbed oral carbohydrates :
0.3 g/kg (10-20g,max 25g)
120 ml of sweetened juice or non-diet soda
Teaspoon of honey or table sugar
Check BS in 10-15min
Corrected
Not corrected
↓Consciousness/unable to drink &
swallow
IV ACCESS/ IO
Available
IV initial glucose:
0.25 g/kg max single dose25g
infusion rate 2-3 ml/min
Infant & children <12y
2.5ml/kg of D.W 10%
NO
Glucagon
IM/SC: 0.03
mg/kg (max
1mg)
observation
IV Maintenance glucose at rate 6-8mg/kg/min
Monitor BS every 30-60min;alter dextrose accordingly until BS 70-120mg/dl then BS 2-4 hourly
Hyponatremic seizures
Hyponatremia is defined as seum Na level <135mEq/L
Signs and symptoms :
• Irritability ,poor feeding ,nausea and vomiting ,lethargy, seizures and
eventually coma and death
• A change in mental status and other neurological signs are important clues to
the need for emergent treatment
Complication of the condition : cerebral edema
Complication of therapy : osmotic demylination syndrome ( irreversible diffuse
demylination in the brain with dysarthia , confusion ,obtundation & coma )
Step 1: acute correction until seizure stop (ideal calculation )
The goal is to raise the serum Na level to 125mEq/L or until seizure stop
Amount of Na = 0.6 x wt in kg x (desired Na level – actual Na level) =… mEq Na
OR 1.2 x wt in kg x (desired Na level – actual Na level) = …ml of 3% NaCL over 15-20min
* Another (fast calculation)
• 3-5 ml/kg of 3% NaCL over 15-20min
• Repeat same fluid as needed in the same duration until seizures stop then recheck
Na level and go to step 2 (slower correction)
TO prepare 3% NaCL = add 1 ml of NaCL 23% + 7 ml 0.9 N.S = 8 ml 3%
Step 2 : Slower correction ( target correction 6-8mEq/L/day )
Amount of Na = 0.6x wt in kg (target Na level –actual Na level)= ….mEq Na over
24hrs( can use 0.9% NS or 0.45% NS+ D5% )
Example
A 10kg child presented with seizures and found to have Na level of 115mEq /L
Management after ABCs
Step 1 (acute correction)
Amount of Na = 1.2x 10 x(125 - 115) = 120ml of 3% NaCL over 15-20min
Step 2( slower correction after seizure stopped )-" target increase Na by 8mEq/L/ day as an example " &
actual Na level become 125 after step 1)
Amount of Na = 0.6x 10 x (133-125) =48mEq Na
" By using 0.9%NS ( each 1L had 154 mEq Na )'
= 310ml of 0.9%NS over 24hours
Immune thrombocytopenia (ITP)
Immune thrombocytopenia (ITP) of childhood is characterized by isolated thrombocytopenia (platelet
count <100,000/microL with normal white blood cell count and hemoglobin)
Un remarkable history except from bleeding symptoms
Un remarkable examination particularly of sings of hereditary bone marrow failure, malignancy,
collagen vascular disease.
✓ CBC, Isolated Thrombocytopenia, Normal WBCS Total and Differential
✓ No Blasts In Peripheral Blood Film
Assess the severity of patient's bleeding symptoms
Sever
Bleeding symptoms
Grade IV
non Sever
bleeding symptoms
Grade I-III
Is bleeding potentially life-threatening?
Yes
Treatment includes all of the
following
PLT transfusion at a dose of
10 to 30 mL/kg (1 unit/4kg
BW), generally followed by a
continuous infusion)
IV. methylprednisolone
30 mg/kg per day (up to 1 g)
for 3-4 days
IVIG 1 g/kg per day for 1-3
days +/- anti -D
75 micg/kg IV as a single
dose
Urgent splenectomy may be
required if rapid
improvement in PLT count is
not achieved. additional
therapies can be added if
these treatments do not
suffice to rapidly control the
bleeding
Is the patient at moderate to high risk of
sever bleeding complications based on one
NO
or more of the following:
Treatment includes
• Head trauma without ICH
either or both of the
• Sever unexplained headache
following
• Planned surgery or procedure that is
IVIG or anti -D
likely to induce blood loss
IV.
• Grade III bleeding symptoms
methylprednisolone
• PLT <30,000/microl PLUS any of the
additional therapies
following risk factors
may be necessary in
o Use of antiplatelet or
some cases
anticoagulant medications (e.g
NSAIDs, heparin)
o Concomitant bleeding disorder
(e.g von Willebrand disease)
o Very active lifestyle subjecting
the patient to frequent trauma
(that cannot be controlled with
activity constriction)
o Close follow up and /or other
required parental supervision
Yes
no
cannot be assured and /or
therapy
is
Is a rapid increase in platelet
accessPharmacologic
to medical care
is
Generally not indicated
count desired ?(e.g urgent
limited
Most patients are
surgery ,head trauma )
managed with watchful
Yes
no
waiting
Treat with IVIG or IV anti-D
Treat with oral glucocorticoids
Grade
Bleeding severity
(international
consensus report)
Minor/minimal
Grade I
Clinical symptoms
Few petechiae (≤100 total) and/or ≤5
small bruises (≤3 cm in diameter)
Grade II
Mild
Many petechiae (>100 total) and/or
>5 large bruises (>3 cm in diameter)
Grade III
Moderate
Grade IV
Severe
Mucosal bleeding ("wet purpura")
that does not require immediate
medical attention or supervision,
such as brief epistaxis, intermittent
gum bleeding, menorrhagia, and/or
a lifestyle that increases bleeding
risks
Mucosal bleeding or suspected
internal hemorrhage that requires
immediate medical attention (eg,
severe GI bleeding, severe
prolonged epistaxis, pulmonary
hemorrhage, muscle or joint
hemorrhage)
Hematology
Specialty
Immunology
Medical Condition / Prerequisite / Comments
Primary and secondary immune deficiency conditions
Hypogammaglobulinemia (reduced total IgG or IgG subclasses and/or inadequate response to immunization) with
recurrent bacterial infection. Not to be given to IgA deficiency
Fetal-Neonatal alloimmune thrombocytopenia (F/NAIT)
Previous affected pregnancy or family history of F/NAIT or mother found on screening to have platelet alloantibodies.
IVIG is first-line treatment of F/NAIT.
In newborn with NAIT the provision of radiated platelets should be first-line therapy and IVIG adjunctive
Treatment should be under the direction of a high-risk obstetrical center with expertise in F/NAIT
Hemolytic disease of the newborn (HDN)
IVIG is indicated only in HDN infants with severe hyperbilirubinemia; i.e. TSB rising despite intensive phototherapy or
TSB level within 34 – 51 micromol/L of the exchange level (TSB=total serum bilirubin)
Idiopathic thrombocytopenic purpura (ITP)-pediatric
REFER TO ITP PROTOCOL
Guillain-Barré syndrome (GBS), including Miller-Fisher syndrome and other variants Symptoms of grade 3 severity
(able to walk with aid) or greater or symptoms less than grade 3 severity that are progressing. Treatment should be
given within 2 weeks of symptom onset. Diagnosis of GBS variants should be made by a specialist.
Neurology
Chronic inflammatory demyelinating polyneuropathy (CIDP): IVIG is considered a first line treatment for initial
treatment of CIDP. Some patients may respond fully to IVIG alone. Other CIDP patients may have a limited or
incomplete response to IVIG and then alternate treatments and immunosuppressants may be considered. Maintenance:
All patients receiving IVIG for chronic treatment of CIDP should be followed by a neurologist specialist.
Multifocal motor neuropathy (MMN)
Diagnosis should be made by a neurologist specialist, as very specific electrodiagnostic expertise is required
Myasthenia gravis (MG)
Severe exacerbations of MG or myasthenic crises, or to stabilize patients before surgery
IVIG not recommended as maintenance therapy for patients with chronic MG
Dose and Duration
0.3-0.6 g/kg every 4
weeks. Monitor IgG
trough level.
Maternal Dose 1 g/kg
every week Neonatal
Dose 1 g/kg, with a
second dose within 48
hrs if required
0.5 – 1 g/kg. If necessary
dose can be repeated in
12 hours
Pediatric: 2 g/kg over 2
days or 0.4g/kg/day for
5 days .Adults. 2 g/kg
over 2-5 days
Initial treatment: 2 g/kg
over 2-5 days.
Maintenance: tailor to
the lowest effective dose
usually 0.5-1g/kg q 4-8
weekly. Or according to
patient follow up
Initial treatment:
2 g/kg over 2-5 days.
Maintenance: tailor to
the lowest effective dose,
0.5-1 g/kg q 3-6 weekly
Initial treatment: 2 g/kg
over 2-5 days or
0.4g/kg/day for 5days
Maintenance: if short
term maintenance
therapy is required
0.5-1 g/kg q 3-4 weekly.
ADEM (Acute Disseminated Encephalomyelitis) syndrome:
For patients Who have an insufficient response to I.V glucocorticoid treatment
Infectious
Diseases
Staphylococcal toxic shock or Invasive Group A streptococcal fasciitis with associated toxic shock. Evidence of systemic
inflammation and end organ hypoperfusion with fever, tachycardia, tachypnea and hypotension
Consult with a medical microbiologist or infectious disease specialist before treatment
Rheumatology
Juvenile dermatomyositis: Lack of response or contraindication to corticosteroids, Methotrexate and/or Azathioprine
therapy. Maintenance therapy: a systematic approach should be taken to determine minimum effective dose. Continued
use should be based on objective measures of sustained effectiveness.
Kawasaki disease:
➢ IVIG is recommended and preferred to be administered within the first 10 days of illness before aneurysms
typically develop.
➢ IVIG should be administered even beyond these 10-day window in patients with evidence of persistent vasculitis or
systemic inflammation (e.g. persistent fever).
Resistant dermatomyositis & polymyositis
IVIG is used as a second line therapy for Patient not responding adequately to glucocorticoids plus azathioprine or
methotrexate.
Dermatology
•
•
Sever toxic epidermal necrolysis.
Sever Stevens – Johnson syndrome.
2g /kg divided in doses
over 2 day-5 days as
alternative therapy to
methylprednisolone
1 g/kg on day one, and
0.5 g/kg per day on days
2 & 3 OR 0.15 g/kg per
day over 5 days.
Initial treatment:2 g/kg
over 2 days.
Maintenance: Maximum
dose per treatment
course should not exceed
2 g/kg.
2 g/kg x 1 day. Second
dose can be given for
patients who fail to
respond the first time.
1 gm/kg for 2
consecutive days then
0.4gm/kg every month
generally for 6 months
course.
1gm/kg/day for
3consecutive days
Hemolysis is an uncommon but well described adverse event of IVIG therapy & has been characterized & reported most often in patients:
•
•
•
Non-Group O (highest risk in Group A or AB),
Inflammatory conditions,
& receiving a high total dose of IVIG(~ 2 grams/kg).
Following IVIG therapy patients should be monitored for 1 to 2 weeks for this adverse event.
Monitor for new onset fever, pallor, jaundice, or changes in urine color (outpatients should be advised to monitor themselves for the above symptoms and alert their physician if
these occur),Changes in Hgb; increased RBC ;increased LDH; low haptoglobin; unconjugated hyperbilirubinemia; hemoglobinuria and presence of significant spherocytosis.
Perform additional testing to confirm the hemolysis if the Hgb has dropped significantly: RBC, Direct antiglobulin test, LDH & Bilirubin.
All IVIG requests that do not correlate with the list above must have hematopathologist approval.
IVIG Is Not Recommended Or Is Contraindicated For Use In The Following Conditions:
Hematology: Aplastic Anemia, Heparin-Induced Thrombocytopenia
Neurology: Adrenoleukodystrophy, A Myotropic Lateral Sclerosis, Autism,
Critical Illness Polyneuropathy, Inclusion Body Myositis, Intractable Childhood Epilepsy, Paraproteinemic Neuropathy (Igm Variant), POEMS.
السلطة الوطنية الفلسطينية
Palestinian National Authority
Ministry of Health
وزارة الصحة
اإلدارة العامة للمستشفيات
Hospitals General Administration
تم مراجعة وتحديث البرتوكول بواسطة لجنة طب األطفال المركزية باإلدارة العامة للمستشفيات وفريق العمل النرويجي المتخصص برعاية
12/01/2016 منظمة الصحة العالمية
Meningitis flow Chart
Patient with Suspected Meningitis
L
Can not do L.P.
•
•
Contraindication for L.P
Treat as high risk
Meningitis until L.P done
Can do L.P
Low risk
High risk
• C.S.F Cells <500 cells/microl
• Protein < 80mg/dl
• Sugar Normal
• Gram stain (– ve )
• NO Seizure or toxic look
All of previous criteria should be present
•
•
I.V. Ceftriaxone 100 mg /kg
/24h or Cefotaxime 225-300
C.S.F Cells >500 cells/microl
• Protein more than 80mg/dl
• Sugar low
• Gram stain (+ ve )
• Seizure or toxic look
If one of previous criteria is present
Full vaccinated for strep.
•
mg/kg/24 hr divided q6h
Don not add Dexamethasone.
•
If C.S.F culture –ve , continue
treatment for 2-5 days
according to response of pt.
and clinical improvement.
•
If after 48 hrs of treatment pt.
Improving and( no available
beds , crowded pediatric ward)
Pt. can be go out on pass and
given treatment as outpatient.
•
I.V Ceftriaxone 100 mg
/kg/24 h or Cefotaxime
225-300/kg/24 h divided
q6h
Add Dexamethasone
(0.15 mg/kg per dose) i.v.
every six hours for (2) days
Partial or not vaccinated for
strep.
• I.V. ceftriaxone, or
Cefotaxime + Vancomycin
60mg/kg. q6h time
•
Add Dexamethasone
(0.15 mg/kg per dose) i.v.
every six hours for (2) days
•
If C.S.F C/S +ve : Most sensitive single Antibiotics can be
used according to causative organism and sensitivity & clinical
response Duration (7-10-14 ) days.
•
•
If CSF culture is neg. with poor
clinical response continue AB
and send CSF for PCR
I.f C.S.F C/S -ve : And pt. improved , Vancomycin can be
stopped after 5 days of treatment and continue Ceftriaxone only
for ( 7-10 ) days according to patient response and clinical
improving as out on pass and given treatment outpatient if no
available beds, and crowded pediatric ward .
•
If PCR is +ve for EV stop AB
•
•
N.B. :
•
•
If Pt. allergic to cephalosporine alternative is
chloramphenicol
If CSF culture is neg. with poor clinical response send CSF
for PCR
ALL cases of suspected bacterial meningitis to be regular follow up as outpatient for
assessment of hearing loss and other complications for at least 6 months.
ALL cases on outpatient management must be under supervision of specialist
Palestinian National Authority
Ministry of Health
السلطة الوطنية الفلسطينية
Hospitals General Administration
وزارة الصحة
اإلدارة العامة للمستشفيات
Meningitis
Neonate ( < 28 days)
(28 days- 2 monthes)
•
Same protocol in Neonate.
•
Vancomycin can be Added
> (2) monthes
•
•
C.S.F Cells > 22
•
Protein or normal
if C.S.F analysis is
pediatric
•
Sugar or normal
suggestive high risk group
Meningitis
•
Gram stain +ve or -ve
meningitis.
Same protocol of
Treatment
• I.V. Ampicillin and Cefotaxime
• C.S.F C/S + ve : According to organism continue for 2-3
weeks.
• C.S.F C/S - ve : Continue for (2) weeks , send CSF for
PCR , IF confirmed virus STOP antibiotics and assess pt.
❖ N.B
L.P To be repeated after (5) days if C.S.F C/S → +ve and for Suspected Bacterial
Meningitis or clinically Not responded for neonatal period.
Metabolic emergency (1st presentation )
Metabolic emergency
(Disorder of carbohydrate, protein & fat metabolism)
Investigations
Blood ( CBC ,differential
,culture), blood glucose
ABG, Anion gap, U/ E,RFT
,LFT ,coagulation profile ,
Ammonia, lactate , CK , uric
acid , lipase ,plasma
aminoacids, pyruvate ,
acylcarnitine profile
Urine : ketones ,RM ,PH,
C/S myoglobin (dipstick
for blood),reducing
substances ,organic acids
CSF ( If indicated ): glucose ,
aminoacids, lactate
Hyperammonemia
Refer to
hyperammonemia
algorithm
Signs of acute decompensation
Vomiting ,anorexia ,shock , dehydration,
lethargy ,seizure, dystonia ,coma, rapid
deep breathing , apnea ,rhabdomyolysis.
Hypoglycemia ( late sign).
Triggers
Acute infection , surgery
, Trauma, fasting,
Increased consumption of
food component(protein)
Monitor BP &vital signs,
GCS, fluid balance
Follow up
ammonia BG , ABG, U/E ,
RFT, LFT,plasma aminoacids
Admit to hospital
▪ Correct hypoglycemia :2 ml/kg
D10%over few minutes
▪ Start antibiotics
▪ FFP( if indicated)
Hypoglycemia
Refer to
Hypoglycemia
algorithm
Shock
Metabolic acidosis
IVF resuscitation : 20ml/kg Normal saline bolus (avoid ringers
lactate ),repeated as indicated
PICU admission
Ventilator support
Fluid
D10% for hypoglycemia
Dext . saline if not hypoglycemia 1.5 x maintenance (glucose
infusion rate 7-8 mg/min)
Rate of infusion: 5ml/kg/hr
Keep BG ( 60-120 mg /dl)
If BG>150mg/dl , start insulin infusion as per DKA protocol at
rate 0.05-0.1unit/kg/hr
Watch for hypernatremia
Cofactors
B12 1mg IM in MMA
Biotin 10mg OD PO in PPA
L –glycine 300mg /kg/day in
Isovaleric acidemia
L-carnitine IV200mg/kg/day in 4
divided doses or PO 100mg /kg/day
Stop carnitine in FAOD &
argininosuccinic aciduria
Nutrition
TPN : intralipid 2g /kg/day (avoid
in FAOD)
Stop protein for 24-36 hrs in UCD
Gradual introduction of protein &
essential amino-acids after 24hrs
Treat constipation(avoid lactulose)
Metabolic acidosis( if persistent
after correction of perfusion)
IV NaHCO3(8.4%)
If PH <7.2,BE >10mmol/l ,or
HCO3 <14mmol/l
Dose : {0.15 X WT X base deficit}
, over30min ,dilute 1ml of
NaHCO3 in 5ml of D5%
NaHCO3 maintenance as
required
Dialysis
Intractable metabolic acidosis
Unresponsive
Hyperammonemia
Coma
Sever electrolyte disturbance
Metabolic emergency (1st presentation )
Metabolic emergency
(Disorder of carbohydrate, protein & fat metabolism)
Investigations
Blood ( CBC ,differential
,culture), blood glucose
ABG, Anion gap, U/ E,RFT
,LFT ,coagulation profile ,
Ammonia, lactate , CK , uric
acid , lipase ,plasma
aminoacids, pyruvate ,
acylcarnitine profile
Urine : ketones ,RM ,PH,
C/S myoglobin (dipstick
for blood),reducing
substances ,organic acids
CSF ( If indicated ): glucose ,
aminoacids, lactate
Hyperammonemia
Refer to
hyperammonemia
algorithm
Signs of acute decompensation
Vomiting ,anorexia ,shock , dehydration,
lethargy ,seizure, dystonia ,coma, rapid
deep breathing , apnea ,rhabdomyolysis.
Hypoglycemia ( late sign).
Triggers
Acute infection , surgery
, Trauma, fasting,
Increased consumption of
food component(protein)
Monitor BP &vital signs,
GCS, fluid balance
Follow up
ammonia BG , ABG, U/E ,
RFT, LFT,plasma aminoacids
Admit to hospital
▪ Correct hypoglycemia :2 ml/kg
D10%over few minutes
▪ Start antibiotics
▪ FFP( if indicated)
Hypoglycemia
Refer to
Hypoglycemia
algorithm
Shock
Metabolic acidosis
IVF resuscitation : 20ml/kg Normal saline bolus (avoid ringers
lactate ),repeated as indicated
PICU admission
Ventilator support
Fluid
D10% for hypoglycemia
Dext . saline if not hypoglycemia 1.5 x maintenance (glucose
infusion rate 7-8 mg/min)
Rate of infusion: 5ml/kg/hr
Keep BG ( 60-120 mg /dl)
If BG>150mg/dl , start insulin infusion as per DKA protocol at
rate 0.05-0.1unit/kg/hr
Watch for hypernatremia
Cofactors
B12 1mg IM in MMA
Biotin 10mg OD PO in PPA
L –glycine 300mg /kg/day in
Isovaleric acidemia
L-carnitine IV200mg/kg/day in 4
divided doses or PO 100mg /kg/day
Stop carnitine in FAOD &
argininosuccinic aciduria
Nutrition
TPN : intralipid 2g /kg/day (avoid
in FAOD)
Stop protein for 24-36 hrs in UCD
Gradual introduction of protein &
essential amino-acids after 24hrs
Treat constipation(avoid lactulose)
Metabolic acidosis( if persistent
after correction of perfusion)
IV NaHCO3(8.4%)
If PH <7.2,BE >10mmol/l ,or
HCO3 <14mmol/l
Dose : {0.15 X WT X base deficit}
, over30min ,dilute 1ml of
NaHCO3 in 5ml of D5%
NaHCO3 maintenance as
required
Dialysis
Intractable metabolic acidosis
Unresponsive
Hyperammonemia
Coma
Sever electrolyte disturbance
Minor Head Injury (<2 years)
Definition : infant who are alert or awaken to voice or light touch but has
history or physical signs of blunt trauma to scalp , skull or brain
Low risk
✓
✓
✓
✓
✓
✓
✓
Normal mental
status , normal
behavior per routine
care giver
No LOC
No severe
mechanism of injury
(fall >0.9m
,acceleration and
deceleration injury ,
death of another
passenger ,etc)
No Vomiting
No evidence of skull
fracture , no
nonfrontal scalp
hematoma
No suspicion of
child abuse
Reliable care givers
Intermediate risk
✓
✓
✓
✓
✓
High risk
LOC< 5 min
Headache, lethargy
Irritability ,confusion
Vomiting <3 times
Non acute skull
fracture >24 hrs
✓
✓
✓
✓
✓
✓
✓
✓
✓
✓
✓
Observe
4-6hours
Witnessed LOC>5min
≥ 3 Vomits
Suspicion of child abuse
GCS< 14( <15 if <1year)
Post –traumatic seizure(focal
or generalized)
Bulging / tense fontanels
Severe mechanism of injury
Signs of basal skull fracture
Fall >1.5m in height
Depressed skull injury
+ve focal neurological exam
Persistent or
worsening
Improved
(symptoms
resolved GCS
15/15)
signs and
symptoms
CT Head Immediately
& Admit
CT Head &
Admit
Discharge with
providing
written
instruction** to
care giver
Additional risks
• High force trauma
• Unwitnesed trauma
• Hematoma
• Vague history(
suspicious of child
abuse)
If normal or
Simple skull
Fracture.
Observation
24hr
Negative
Skull X –ray
(R/o fracture)
positive
Written instruction
1. Immediate medical attention is required when :
• Inability to awaken the child as instructed
• Persistent or worsening headache
• Continued vomiting that begin /continues 4-6 hours post trauma
• Change in mental status or behavior
• Unsteady gait or clumsiness / in coordination
• seizure
2. where is the nearest place to seek medical advice if needed
+ve ct
Neurosurgical
consultation
Consider Manitol if
suspecting
↑ICP (Dose :0.25-1gm
/kg/dose
Over 20-30min) ,may
repeat as needed
Minor Head Injury (>2 years)
Definition : Children who have sustained head trauma but have GCS 14-15
with normal physical examination & no evidence of skull fracture
Low risk
✓
✓
✓
✓
✓
✓
✓
Normal mental status
No LOC
No severe mechanism
of injury (fall >0.9m,
acceleration and
deceleration injury ,
death of another
passenger ,etc)
No vomiting or severe
headache
No signs of basal skull
fracture
No suspicion of child
abuse
No Coagulopathies
✓ Reliable care givers
Intermediate risk
✓ LOC<5 min
✓ Headache, lethargy
✓ Irritability ,confusion
✓ Vomiting <3 times
✓ Unreliable care giver
✓
Observe
4-6 hours
✓
✓
Improved
(symptoms
resolved GCS
15/15)
Discharge with
providing written
instruction to care
giver
✓
✓
✓
✓
✓
Persistent or
worsening
signs and
symptoms
✓
✓
High risk
Witnessed LOC>5min
≥ 3 Vomits
Suspicion of child abuse
GCS< 14
Post –traumatic
seizure(focal or
generalized)
Positive focal
neurological
examination
Severe mechanism of
injury
Signs of basal skull
fracture
Fall >3m in height
Depressed skull injury
C T Head
Immediately& Admit
+ve CT
CT Head &
Admit
Consider other diagnosis
(may need F/U CT, fundoscopy)
Neurosurgical
consultation
Consider Manitol if Suspecting
↑ICP (Dose :0.25-1gm /kg/dose
Over 20-30min) ,may repeat as
needed
Written instruction
1. Immediate medical attention is required when :
• Inability to awaken the child as instructed
• Persistent or worsening headache
• Continued vomiting that begin /continues 4-6 hours post trauma
• Change in mental status or behavior
• Unsteady gait or clumsiness / in coordination
• seizure
2. where is the nearest place to seek medical advice if needed
Organophosphate & Carbamate poison
Acute onset + "DUMBELS" +/-CNS
Diarrhea ,Urination, Miosis ,Bradycardia, Bornchorrhea, Bronchospasm ,Emesis ,
Lacrimation, Salivation
ABC
O2 maske 100% , cardiopulmonary monitoring
Early Intubation often required , AVOID succinylcholine
Decontamination
If ingestion < 1hr→give Activated charcoal 1g /kg (max 50g), unless airway not protected or other
contraindications
Aggressive skin & ocular irrigation
Bag /Discard clothing
NB: Health care workers must take precautions as they may get exposure
Atropine IV 0.05 mg/kg
If No effect DOUBLE the dose every 3-5min
Therapeutic end point is until clearance of respiratory secretions & cessation of
bronchospasm NOT tachycardia or mydriasis
Atropine overdose
•
•
•
Fever
Muscular
Fibrillation
Agitation
Treat poor perfusion
-Bolus of 0.9% NS 20 ml/kg (rapid infusion) ,repeat as needed (observe
urine output)
For Bronchospasm
Inhaled ipratropium bromide 0.5mg (repeated as needed)
Pralidoxime (use in conjunction with Atropine)
IV bolus 25-50mg/kg slowly over 30min
May be repeated after 30min
If sever, give continuous infusion pralidoxime 10-20mg/kg/hr
AVOID rapid bolus administration → may cause cardiac arrest
Diazepam (valium) IV 0.1-0.2mg/kg(max 10mg)
Prophylactic for organophosphate agent –induced seizure
Repeat as necessary if seizure occur. AVOID Phenytoin
Call PICU
Atropine
infusion
10-20% of the
total loading
dose/hr
PAEDIATRIC PARENTERAL FLUID THERAPY (1 month-12 yrs)
Initial management guideline
ADMINISTER RAPID FLUID BOLUS
Monitoring & observations
12 Hourly : Assess In /Out put,
plasma glucose
➢
➢
➢
➢
YES
Admission
WeighT.U&E
ALL
CHILDREN
Is shock
present
?
Give 20 ml/kg sodium chloride 0.9% IV or intraosseous over 20 minute ………. Reassess
Repeat bolus if needed(up to 60-80 ml/kg) ) consider third bolus in ICU area
Call for senior help
Colloids may be needed
Daily-Clinical reassessment:.
U&E(more often if abnormal;4-6
hourly if Na+< 130 mmol/L
No
Can child be
managed with oral
Fluids?
PRESCRIBE ORS ( orally or by NG tube):According to level of
dehydration and tolerance
YES
SEVERLY ILL CHILDREN
MAY NEED
➢
➢
➢
Mild dehydration 30-50ml/kg over 4hr
Mod dehydration 50-100ml/kg over 4hrS
If not improved or not tolerated give I.V fluid
Hourly-HR. RR .BP, GCS
.Fluid IN/Output(urine osmolarity
if volume cannot be assessed)
2-4 hourly –glucose, U&E,+/blood gas
Daily-weight is mandatory
Is there a
fluid
deficit?
No
Each shift : Handover and review
of fluid management plan
If plasma Na+ < 130 mmol/l or >
160 mmol/L or plasma Na +
changes> 0.5 mmol/L in hours
ask for senior advice
YES
o
(estimate deficit +maintenance )– shock bolus /24hrs
o
fluid deficit= (%dehydration x kgx10)as mls of sodium chloride 0.45% + D5%
o
o
o
estimate IV maintenance fluid
o
give over 24 hours(but over 48 hours if Na < 135 or>150 mmol/l)
ongoing losses: calculate at least 4 hourly. give (ORS or 0.45%saline + D5%) as 10ml/ kg for
each diarrheal stool or vomiting
sodium chloride 0.45% (with or without pre-added potassium: be prepared to change fluid
type and volume according to clinical reassessment, electrolyte losses and test results
o
o
Prescribe
Maintenanc
e fluids
Fluid choices: Sodium chloride 0.45% with D5 % (if not available can prepare)
How to calculate maintenance( fluid see the table )
Commence Oral Fluid & Discontinue Iv Fluids As Soon As Possible
PAEDIATRIC PARENTERAL FLUID THERAPY (1 month-12 yrs)
Initial management guideline
CALCULATION OF 100% MAINTENANCE RATE
➢ (a) For first 10 kg: 100ml/kg/day= 4ml/kg/hr
➢ (b) For second 10 kg 50ml/kg/day = 2ml/kg/hr
➢ (c ) For each kg over 20 kg : 20 ml /kg /day = 1 ml / kg /hr
➢ For 100% daily maintenance add together (a)+(b)+(c)
➢
•
Patients particularly at risk of hyponatremic complications:
Gastric losses; CNS infection; severs sepsis; hypotension; intravascular volume depletion; Bronchiolitis; gastroenteritis with dehydration; abnormal
plasma sodium, particularly if less than 138 mmol/L but also when gets than 160 mmol/L salt wasting syndromes
Alter fluid rate according to clinical assessment. Change electrolyte and glucose content of fusion fluid according
➢ If risk of hyponatraemia is high consider initially reducing maintenance Volume to two thirds of maintenance
➢ Hypokalaemia(<3.5 mmol/L): Check for initial deficit .Maintenance up to 40 mmol/L, IV potassium usually need after good urine output .
➢ Oral intake and Medications: Volumes of intake, medications& drug infusions must be considered in the fluid prescription.
➢ Hypoglycaemia(<50mg/ dl): Medical Emergency give4 ml/kg bolus of glucose 10%. Review maintenance fluid, (consult with senior and recheck level after
15-30 mins.,)
➢ Symptomatic Hyponatraemia: check U&E if patient develops nausea, vomiting, headache,irritability, altered level of consciousness, seizures or apnea. This is
a Medical Emergency and must be corrected : Commence infusion of 3% sodium chloride(4-6ml/kg) in a rate of 1ml /min and get senior advice immediate
Rapid Sequence Intubation( RSI )
1-
Preoxygenation (5 minutes before intubation)
- Administration O2 at highest concentration available
-For spontaneously breathing child ,use non-rebreathing mask for at least 3min
-If apneic or desaturating insert NG tube , use bag –mask ventilation >7L/min +/- Cricoid
pressure to prevent gastric insufflation which reduces the risk of regurgitation and aspiration
2-Preparation (AMPLE)
• Identify conditions that will affect choice of medications
• Identify conditions that will predict difficult intubation or
bag- mask ventilation
• Assemble equipment & check function
• Develop contingency plan for failed intubation
• If cardiac arrest or deeply comatose child , sedation
&paralytic agents are unnecessary prior to intubation
AMPLE
•
•
•
•
•
A = Allergy
M = Medication
P = Past medical
L = last medical
E = Events
3- Pretreatment
•
•
Atropine IV 0.02mg/kg (min 0.1mg-max 0.5mg)
o All infant <1yr
o 1-5 yrs receiving succinylcholine , and >5yrs with2nd dose succinylcholine
Lidocaine IV optional for ↑ ICP,2-3min. before intubation
o 1-2mg/kg (max dose 100mg)
Hx of asthma
Bronchospasm
,↓BP OR septic
shock
- Ketamine
(>3months)
o IV: 1-2mg/kg
o IM: 3-7mg/kg
Status epilepticus
*(stable BP)
o -Midazolam
IV:0.2-0.3mg/kg
(max2mg)
↑ICP or head injury
(if stable or↓BP)
Etomidate
IV :0.3mg/kg
Uncomplicated
child
Etomidate
IV :0.3mg/kg
IF Etomidate NOT available use
Midazolam 0.2-0.3 mg /kg Max 2 mg
4- paralytic
-Succinylcholline:
o IV: infant & younger children 2mg/kg , older children 1-1.5mg/kg
o IM :3-5mg/kg
o Avoid in :Neuromuscular disease , Organophosphate poisoning,48-72hrs after burn
,Crush or denervation injury , Malignant hyperthermia , Pre –existing ↑K+
-Pancronium ( if succinylcholine contraindicated) dose IV 0. 1mg/kg
5-Protection & Positioning
o
o
Sniffing position
Cricoids pressure
6-Placement
&
confirmation
7- Post –intubation
CXR, Infusion Midazolam .
Infusion Fentanyl (1micg /kg/ hr)
Septic shock
Define as sepsis with CVS dysfunction (i.e BP, reliance on vasoactive drugs to maintain a
normal BP ,or 2 of the following:
• prolonged capillary refill, oliguria , metabolic acidosis, lactic acedemia that
persists despite the administration of > 40 ml /kg NS in 1 hr
•
•
•
Recognize altered mental status and perfusion
ABC ,O2 and support ventilation ,establish vascular access
Consider CBC ,ABG ,lactate , glucose, ionized calcium , electrolytes,cultures
Consider PICU
Within First hour
▪ push repeated 20 ml / kg 0.9% NS to treat shock , give up 60-80ml boluses
▪ Correct hypoglycemia , hypocalcaemia , electrolytes
▪ Give 1st dose antibiotics STAT Ceftriaxone or Cefotaxime
▪ Consider ordering vasopressor drip
▪ Establish 2nd vascular access site if vasoactive infusion anticipated
Continue PICU
monitoring
YES
fluid responsive (i.e normalized perfusion/hemodynamic
)?
NO
Begin vasoactive drug therapy and titrate to correct hypotension
/poor perfusion : consider establishing central venous access
Normotensive
Hypotensive vasodilated
(worm)shock
Begin Dopamine 2-20
mcg/kg/min IV/IO
Infusion ,titrate to
desired effect
Begain Norepinephrine 0.1-2
mcg/kg/min IV/ IO infusion titrate
to desire effect
Hypotensivevasoconstricted
(cold) shock:
Begin Epinephrine :0.1-1mcg
/kg/min IV/IO infusion (consider
higher doses if needed(
Evaluate Scvo2 :goal Scvo2 sat >70%?
Scvo2 sat ≥ 70%decrease BP
(WARM SHOCK)
Additional fluid boluses
Norepinephrine +/Vasopressin (0.2-2
milluints/kg/min)
•
•
•
Scvo2 sat< 70 % normal BP but poor
perfusion
▪ Transfuse to Hgb>10g/dl
▪ Additional fluid boluses
▪ Optimize arterial oxygen Sat
▪ Consider dobutamine 2-20 mcg/kg/min
IV/IO :titrate to desire effect(
▪ Consider Milrinone or Nitroprusside
Scvo2 sat <70 % decreased BP &
poor perfusion (Cold SHOCK)
▪ Transfuse to Hgb>10g/dl
▪ Additional fluid boluses
▪ Optimize arterial oxygen
sat
▪ Consider Epinephrine or
Dobutamie+Norepinephrine
Fluid-refractory and Dopamine-or Norepinephrine dependent shock defines pt at risk for adrenal
insufficiency (AI)
Draw baseline cortisol ; consider ACTH stimulation test if unsure of need for steroids
If adrenal insufficiency is suspected , give Hydrocortison 2mg/ kg bolus IV (max100mg)
Reference Nelson 20, Uptodate2018,kwuaiti guideline2015
Sever Croup
-Croup (laryngotracheitis,), primarily is viral (parainfluenza 60%) respiratory tract illness. most patients have
an URTI, the child then develops the characteristic barking, cough, hoarseness and inspiratory stridor and a
variable degree of RD. Symptoms are characteristically worse at night .Significant respiratory compromise is
present when the PO2 rises over 45mm Hg and PaO2 falls below 70mm Hg in room air .
-Signs suggestive of impending respiratory failure include: hypotonicity, noticeable retractions ,↓or
absent respiratory breath ,depressed level of consciousness, tachycardia out of proportion , cyanosis.
-Sever croup : stridor at rest ,cyanosis SO2 <92% in air ,moderate to severe recession , apathetic/ restless
Moderate - sever croup
Westley score >3
•
•
•
•
•
•
ABC
100% O2, maintain SPO2 >92%
Cardiac monitor / pulse oximeter
Instruct parents to hold and comfort the child
Treat the fever (use antipyretic)
If IV access obtained, consider IV fluids
Nebulized Epinephrine (1: 1000)
•
0.5ml/kg/dose (max 2.5ml for age <4yrs 5ml for >4 yrs ) over 15
min
•
Can be repeated every 15- 20min
C and
Corticosteroids
•
Dexamethasone 0.6mg/kg (max 16mg)*by the least invasive route
(PO , IV,IM ) or
•
Nebulized Budesonide 2mg over 10-15 min. (if vomiting or
couldnot administer corticosteroid
toxic / ill looking child
Consider bacterial
infection
Call PICU
Consider
intubation with
ETT 0.5-1mm
smaller than
normally used for
age OR
tracheostomy
Observe for 3-4 hrs
Repeat Nebulized
Epinephrine
Yes
Worsening symptoms
No
May discharge
home
Yes
Are discharge criteria
met
Clinical feature
Assigned score
Level of consciousness
Normal, including sleep = 0
Disoriented = 5
None = 0/With agitation = 4/At rest = 5
None = 0/With agitation = 1/At rest = 2
Normal = 0/Decreased = 1/Markedly decreased = 2
None = 0/ Mild = 1/ Moderate = 2/ Severe = 3
Cyanosis
Stridor
Air entry
Retractions
References :Nelson 20,Up todate 2018,Kuwaiti guide line
No
Admit to
pediatric ward
Westly croup score
≤2 mild
3 to 7 moderate
8 to 11 sever
≥12 Impending respiratory failure
Status Epilepticus
SE as a single unremitting seizure lasting longer than five minutes or frequent clinical seizures
without an interictal return to the baseline clinical state. This corresponds with the time at which
urgent treatment should be initiated
Manage ABC
0-5MINT
1.
2.
3.
4.
5.
6.
Cardiac pulmonary Monitor including BP ,Pulse Oximeter, temp
Establish IV Access
Place in the recovery lateral decubitus position
bedside, glucometer
cbc ,electrolytes
Measure blood level if on Phenobarbital, phenytoin carbazepine or valproate
IV access attempts should be limited to 3
min
-5mint-10mint
IV Diazepam 0.2mg/kg
over 2min (max 5mg in
infants and10mg in child)
OR Midazolam I.V.
0.2mg/kg
Benzodiazepine can be
repeated once after 5min
2nd dose
BUCCAL OR INTRANASAL
YES
NO
Rapid IV
access
Midazolam 0.2-0.5MG /KG
OR Rectal Diazepam
0.5mg/kg(max20mg)
Benzodiazepine can be
repeated once after 5min
Insert intraosseous IO needle if
seizure is not stopped with other
routes benzodiazepines
IS child
on
YES
NO
15-50 MINTN
IV/ IO Phenobarbital
20mg/kg over 20min
Max 1gm) OR IV,IO
phenytoin 10mg/kg in NS
over 20min(max 500mg)
IV/IO PHENYTOIN 20mg/kg in NS
over 20 min(max1000mg)
If no response Then
IV Phenobarbital 20mg/kg over 20min
phenobarbital can be repeated up to
40mg maximum 1 g, (10 mg/kg if
phenobarbital already given)
Seizure
Stopped?
Admit to
hospital ,
investigate and
treat potential
causes of status
epilepticus
YES
No→ Call PICU
IV /IO Midazolam 0.1mg/kg loading dose (max of 8mg)over 2-3min then
120mcg/kg/hr infusion increase by 120mcg/kg/hr every 5min if the
seizure contagious (max 1440 mcg/kg/hr)
Consider rapid sequence intubation, Consider high dose phenobarbital,
لجنة الصيدلة و العالجيات بمستشفى الدرة
thiopental infusion, propofol.
Reference
Nelson 20
Upto date 2018
AMERICAN EPILEPSY SOCITY
Important toxicology mnemonics
•
•
•
•
Miosis causes : COPS
Cholinergic , Clonidine
Opiates, Organohosphate
Phenothiazine , Pilocarpine
Sedatives , Barbiturates
•
•
•
•
Mydriasis causes : AAAS
Antihistamines
Antidepressant
Anticholinergic
Sympathomimetics
(amphetamines ,cocaine ,PCP: Phenylcyclophenedine)
•
•
•
•
•
•
•
•
•
•
•
•
•
•
•
•
•
Diaphoretic skin causes SOAP
Sympathomimetics
Organophosphates
Aspirin
PCP (Phenylcyclophenedine)
Blue skin causes
Cyanosis
Methemoglobinemia
Seizure toxins: OTIS CAMPBELL
Organophosphates
TCA
INH
Sympathomimetics
Camphor
Amphetamines
Methylxzanthines
PCP, Propranonlol ,Phenol
Bzp (benzodiazepines) withdrawal
Lithium ,lead
Lidocaine ,lindane
↑Anion Gap Causes : MUDPILE CATS
• Methanol
• Uremia
• DKA
• Paraldehyde, Phenoformin
• Iron , INH
• Lactic acidosis
• Ethylene glycol
• Aspirin , Alcohol
• Toluene
• Solvents
•
•
Red skin causes
Carbonmonoxide
Boric acid
•
•
•
•
↓HR,↓BP causes
B – Blockers
Calcium channel blockers
Digoxins
Narcotics
Coma toxins : LETHARGIC
•
•
•
Lwad, Lithium
Ethanol, Ethylene glycol
TCAs (tricyclicantidepressent) ,Toluene
•
Heroin , HEAVY metals ,Hypoglycemiacs
•
•
•
•
•
Antidepressents, antihistamin
Respiridone
GHB gamma- hydroxybutyrate
INH,INSULIN
Carbon monoxide, Cyanide, Clonidine
" One Pill Can Kill"
•
•
•
•
•
•
•
Cardiovascular drugs (ß- blocker, Cachannel antagonist)
Antidepressents
Antipsychotics
Antiarrhythmic
Salicylates
Oral hypoglycemic agents
Opioids