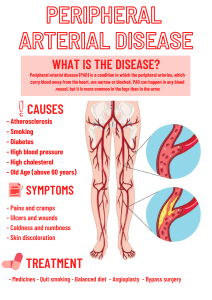
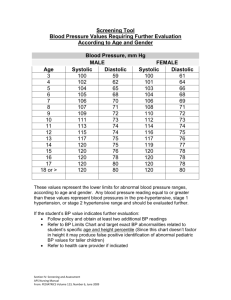
BLOOD PRESSURE Dr. Arifa Begum Associate professor, Dept of Physiology, Gazi Medical College Khulna, Bangladesh. Definition: Blood pressure is the lateral pressure exerted by blood on the vessel walls while flowing through it. • B.P= cardiac output X total peripheral resistance. • Systolic pressure is the measure of Cardiac output • Diastolic pressure is the measure of peripheral resistance Types :Arterial blood pressure is expressed in four different terms: 1. Systolic blood pressure 2. Diastolic blood pressure 3. Pulse pressure 4. Mean arterial blood pressure Systolic and diastolic blood pressure are measured blood pressure and remaining two are calculated pressure. SYSTOLIC BLOOD PRESSURE: Systolic blood pressure (systolic pressure) is defined as the maximum pressure exerted in the arteries during systole of heart. Normal systolic pressure: 120 mm Hg (110 mm Hg to 140 mm Hg). Significance of Systolic pressure undergoes The height of systolic pressure indicates: (1) The extent of work done by heart (2) The force with which the heart is working. (3) The degree of pressure which the arterial walls have to withstand. DIASTOLIC BLOOD PRESSURE: Diastolic blood pressure (diastolic pressure) is defined as the minimum pressure exerted in the arteries during diastole of heart. Normal diastolic pressure: 80 mm Hg (60 mm Hg to 80 mm Hg). Increase of diastolic pressure indicates that the heart is approaching towards its failure. Consequently, variations of diastolic pressure are of greater prognostic importance than those of systolic. PULSE PRESSURE: Pulse pressure is the difference between the systolic pressure and diastolic pressure. Normal pulse pressure: 40 mm Hg (120 – 80 = 40). MEAN ARTERIAL BLOOD PRESSURE: Mean arterial blood pressure is the average pressure existing in the arteries. It is the diastolic pressure plus one third of pulse pressure. To determine the mean pressure, diastolic pressure is considered than the systolic pressure. It is because, the diastolic period of cardiac cycle is longer (0.53 second) than the systolic period (0.27 second). Normal mean arterial pressure: 93 mm Hg (80 + 13 = 93). Mean arterial blood pressure = Diastolic pressure + 1/3 of pulse pressure = 80 + 40/3 = 93.3 mm Hg Factors controlling arterial blood pressure: 1. Pumping action of the heart: Effectual contraction of the heart is the main factor for controlling the cardiac output, blood pressure and flow within the blood vessels 2.Cardiac output: Alterations of cardiac output will alter blood pressure. Cardiac output depends upon venous return, force and frequency of heart beat. Blood volume affects blood pressure directly, by mainly modifying the cardiac output. 3. Elasticity of the arterial walls: 4.Blood volume: Increase in blood volume will raise both the systolic and diastolic blood pressure. 5. Viscosity of the blood: Alteration in blood viscosity will affect the diastolic pressure by its effect on the peripheral resistance. .6. Peripheral resistance: It is the resistance which blood has to overcome while passing through the periphery. The chief seat of peripheral resistance is the arterioles and to a smaller extent the capillaries Peripheral resistance depends on the following: (a) Velocity of blood (b) Viscosity of blood (c) Elasticity of arterial walls (d) Lumen of the blood vessels. The seat of peripheral resistance is found to be chiefly in the arterioles, where the velocity is fairly high and the lumen is narrow. Cardiac output Arterial system Total peripheral resistance Peripheral runoff to capillaries The arterioles are the smallest branches of the arteries. Their walls have an extensive development of smooth muscle, and they are the site of highest resistance to blood flow. It is extensively innervated by sympathetic adrenergic nerve fibers. α1-Adrenergic receptors are found on the arterioles of several vascular beds (e.g., skin and splanchnic vasculature). When activated, these receptors cause contraction, or constriction, of the vascular smooth muscle. Constriction produces a decrease in the diameter of the arteriole, which increases its resistance to blood flow Poiseuille's law: In 1841 the French Physician J . L. M. Poiseuille studied the factors regulating the flow of viscous fluids through the capillary tubes. He showed that: Resistance to blood flow in any blood vessel proportionally varies directly with the viscosity of the blood and also with the length of the blood vessel and inversely with the fourth power of the radius of the blood vessel. It can be represented by the following formula: where R stands for resistance to blood flow, n for viscosity of blood, L for length of blood vessels, r for radius of the blood vessel, 8 for Hagen's integration and 𝝅 factor for a cylindrical tube. • Factors Affecting Peripheral Resistance: Peripheral resistance is determined by two main factors: • 1. Radius of Blood Vessel: The radius of the blood vessel significantly affects peripheral resistance. This is called vascular hindrance. • 1. Vasoconstriction increases and vasodilation decreases • peripheral resistance. • 2. Decrease in radius of vessels to half increases peripheral • resistance by 16 times. Viscosity of Blood: Viscosity of blood also affects peripheral resistance. Viscosity mainly depends on the factors like hematocrit, composition of plasma, resistance of red cells to deformation and temperature. • Hematocrit: Hematocrit is the single most factor that greatly affects viscosity of blood. Hematocrit is the packed cell volume, which depends mainly on the number of red cells in the blood. Viscosity increases in polycythemia and decreases in anemia. In anemia, circulation is hyperdynamic due to decreased peripheral resistance. • Composition of Plasma: In plasma, it is mainly the concentration of plasma proteins that affects viscosity. Viscosity increases in conditions in which concentration of plasma protein is more, Viscosity decreases in hypoproteinemia. • Resistance of Red Cells to Deformation: When the red cells become rigid as seen in hereditary • spherocytosis, viscosity increases. • Temperature: increase temperature decreases viscosity, decrease temperature increases viscosity. Blood Pressure Cardiac output Stroke volum e Preload E.D.V Venous return Total peripheral resistance Heart rate Contr actilit y After load Filling time Filling pressure Veno motor tone Blood volume Measurement and recording of blood pressure: Indirect method: very convenient clinically in human being. Riva-Roci (1896) first introduced this indirect method and afterwards Korotkoff (1905) introduced a convenient method by which the systolic and diastolic pressure could be ascertained only through listening to a sound. This is the standard method of recording blood pressure all throughout the world. The instrument used is known as Sphygmomanometer. Auscultatory method: The instrument is kept at the level of the heart and the cuff is tied round the upper arm. Pressure is raised to 200 mm of Hg and then gradually released. Variations of sounds are heard with a Stethoscope placing its chest piece on the brachial artery, a little below the cuff. the sounds are heard due to occurrence of turbulence in the flow of blood through the narrowed blood vessels when the manometric pressure just coincides with the systolic blood pressure. When the pressure is further released, normal streamline flow sets in and the sound is no longer heard. At this point manometric pressure coincides with the diastolic blood pressure. as the pressure is released the following variations of sounds are heard: : First phase—sudden appearance of a clear tapping sound. This indicates systolic pressure. Second phase—the tap sound is replaced by a murmur persisting for another 15 mm of Hg. Third phase- the murmur is replaced by a clear loud gong sound Fourth phase—the loud sound suddenly becomes muffled and rapidly begins to fade. This point indicates diastolic pressure. fifth phase— absence of all sounds. REGULATION OF ARTERIAL BLOOD PRESSURE: Arterial blood pressure varies even under physiological conditions. However, immediately it is brought back to normal level because of the presence of well organized regulatory mechanisms in the body. The regulatory mechanisms are: A. Nervous mechanism or short term regulatory mechanism B. Renal mechanism or long term regulatory mechanism C. Hormonal mechanism D. Local mechanism or intermediate - term mechanism Short term regulation mechanism: 1. Baroreceptor reflex mechanism • 2. chemoreceptor mechanism • 3. CNS ischemic response Long term mechanism: 1. renal body fluid mechanism 2. Renin angiotensin mechanism • Intermediate term mechanism: • 1. vasoconstrictor mechanism • 2.capillary fluid shift mechanism • 3. Stress relaxation changes in vasculature • Hormonal mechanism: 1. Epinephrin-nor epinephrin mechanism • 2. Vasopressin vasoconstrictor mechanism • Cardiovascular centers are mainly located in the medulla. • These centers primarily control the autonomic output on heart and blood vessels, which is the major cardiovascular regulatory pathway. Nervous control of arterial pressure, beginning within seconds and often increasing the pressure to two times normal within 5 to 10 seconds. Conversely, sudden inhibition of nervous cardiovascular stimulation can decrease the arterial pressure to as little as one-half normal within 10 to 40 seconds. Therefore, nervous control of arterial pressure is by far the most rapid of all our mechanisms for pressure control. . Baroreceptor Mechanism: Baroreceptors are the receptors, which give response to change in blood pressure. Location: The baroreceptors are located in the walls of the carotid sinus, where the common carotid artery bifurcates into the internal and external carotid arteries, and in the aortic arch. The baroreceptors are mechanoreceptors, which are sensitive to pressure or stretch. Increases in arterial pressure cause increased stretch on the baroreceptors and increased firing rate in the afferent nerves. Decreases in arterial pressure cause decreased stretch on the baroreceptors and decreased firing rate in the afferent nerves. Brain stem cardiovascular centers: are located in the reticular formations of the medulla and in the lower onethird of the pons. These centers function in a coordinated fashion, receiving information about blood pressure from the baroreceptors and then directing changes in output of the sympathetic and parasympathetic nervous systems to correct the blood pressure as needed. Mechanism: blood pressure is sensed by baroreceptors in the carotid sinus and aortic arch. Afferent information about blood pressure is then sent to the medulla via the glossopharyngeal (CN IX) and vagus (CN X) nerves. This information is integrated in the nucleus tractus solitarius, which then directs changes in the activity of several cardiovascular centers The parasympathetic outflow is the effect of the vagus nerve on the SA node to decrease the heart rate. The sympathetic outflow has four components: an effect on the SA node to increase heart rate, an effect on cardiac muscle to increase contractility and stroke volume, an effect on the arterioles to produce vasoconstriction and increase TPR. An increase in Pa is detected by baroreceptors in the carotid sinus and in the aortic arch. The glossopharyngeal and vagus nerve fibers synapse in the nucleus tractus solitarius of the medulla increase in parasympathetic outflow to the heart and a decrease in sympathetic outflow to the heart and blood vessels • The increase in parasympathetic activity to the SA node (via the vagus nerve) results in a decrease in heart rate • The decrease in sympathetic activity to the SA node decrease HR and also decreases cardiac contractility. • the decreased heart rate and decreased cardiac contractility produce a decrease in cardiac output • decrease in sympathetic activity also affects the tone of the blood vessels, decreased constriction of arterioles, decreases TPR these coordinated reflexes reduce Pa back to the setpoint pressure (i.e., to 100 mm Hg) How BP is regulated in a person when stand suddenly from lying position: the carotid sinus baroreceptors are not stimulated at all by pressures between 0 and 50 to 60 mm Hg, but above these levels, they respond progressively more rapidly and reach a maximum at about 180 mm Hg. Note especially that in the normal operating range of arterial pressure, around 100 mm Hg. Chemoreceptor reflex: that operates in much the same way as the baroreceptor reflex except that chemoreceptors. The chemoreceptors are chemo sensitive cells sensitive to oxygen lack ,carbon dioxide excess, and hydrogen ion excess. this chemoreceptor reflex is not a powerful arterial pressure controller until the arterial pressure falls below 80 mm Hg Location: Peripheral chemoreceptors are situated in the carotid body and aortic body. Mechanism: Whenever blood pressure decreases, blood flow to chemoreceptors decreases Resulting in decreased oxygen content and excess of carbon dioxide and hydrogen ion Excite the chemoreceptors, which send impulses to stimulate vasoconstrictor center. Blood pressure rises and blood flow increases. Chemoreceptors play a major role in maintaining respiration rather than blood pressure. Central nervous system (CNS) ischemic response: the baroreceptors, the chemoreceptors, and the lowpressure receptors, all of which are located in the peripheral circulation outside the brain. when blood flow to the vasomotor center in the lower brain stem becomes decreased Cause cerebral ischemia the vasoconstrictor and cardioaccelerator neurons in the vasomotor center become strongly excited Stimulating the sympathetic vasomotor nervous control areas in the brain's medulla. The systemic arterial pressure often rises to a level as high as the heart can possibly pump. This arterial pressure elevation in response to cerebral ischemia is known as the central nervous system (CNS) ischemic response. The ischemic effect on vasomotor activity can elevate the mean arterial pressure dramatically, sometimes to as high as 250 mm Hg for as long as 10 minutes he CNS ischemic response is one of the most powerful of all the activators of the sympathetic vasoconstrictor system. It is sometimes called the "last ditch stand" pressure control mechanism. Cushing Reaction: Cushing reaction is a special type of CNS ischemic response that results from increased pressure of the cerebrospinal fluid around the brain in the cranial vault. It occurs when ICP raises. Long term mechanism for blood pressure control: Kidneys play an important role in the long term regulation of arterial blood pressure. Kidneys regulate arterial blood pressure by two ways: 1. By regulation of ECF volume or renal body fluid mechanism. 2. Through renin angiotensin mechanism. Long term mechanism for blood pressure control: Renal body fluid mechanism: when body contains too much extra cellular fluid blood volume Arterial pressure The rising pressure in turn has a direct effect to cause the kidney to excrete the excess ECF, thus returning pressure back toward normal. So, When the blood pressure increases, kidneys excrete large amounts of water and salt, particularly sodium, by means of pressure diuresis and pressure natriuresis. This is the mechanism for decreasing blood pressure. Renin angiotensin aldosterone mechanism: