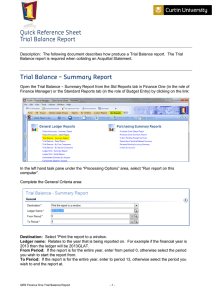
CARDIAC TERMS CARDIAC OUTPUT (CO) ↓ CO = ↓ perfusion to the body Total volume pumped per minute • ↓ LOC • • Shortness of breath • Skin will be cold & clammy • ↓ UOP • Weak peripheral pulses Normal 4 - 8 L/min Less volume = ↓ CO More volume = ↑ CO CO = HR x Stroke Volume Cardiac Output Heart Rate STROKE VOLUME CONTRACTILITY Amount of blood pumped out of the ventricle with each beat or contraction Force / strength of contraction of the heart muscle EJECTION FRACTION (EF) % of blood expelled from the left ventricle with every contraction Normal EF: 50 - 70% EXAMPLE: If the EF is 55%, the heart is pumping out 55% of what’s inside of the left ventricle PRELOAD AFTERLOAD Amount of blood returned to the right side of the heart at the end of diastole Pressure that the left ventricle has to pump against (the resistance it must overcome to circulate blood) Clinically measured by systolic blood pressure! Hemodynamic Parameters Cardiac output (CO) Total volume pumped per minute Cardiac Index Cardiac output per body surface area Central Venous Pressure Pressure in the superior vena cava. Shows how much pressure from the blood is returned to the right atrium from the superior vena cava. (CI) (CVP) Mean Arterial Pressure CI = CO surface area (MAP) Average pressure in the systemic circulation (your body) through the cardiac cycle Systemic Vascular resistance The resistance it takes to push blood through the circulatory (SVR) © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. Normal 4 - 8 L/min 2.5 – 4.0 L/min/m2 2 – 8 mmHg 70 – 100 mmHg At least 60 mm Hg is require to adequately perfuse the vital organs 800 – 1200 dynes/sec/cm 101 FLOW OF BLOOD THROUGH THE HEART RIGHT SIDE LEFT SIDE Deoxygenated Blood Oxygenated Blood Carries oxygen poor blood from the body back to the right side of the heart Oxygenated blood from the lungs 1. Superior / Inferior Vena Cava 7. Pulmonary Vein 2. Right Atrium 8. Left Atrium 3. Tricuspid Valve 9. Bicuspid / Mitral Valve 4. Right Ventricle 10. Left Ventricle 5. Pulmonic Valve 11. Aortic Valve 6. Pulmonary Artery 12. Aorta Deoxygenated blood to the lungs Oxygenated blood to the body VASCULAR SYSTEM FACTS ARTERIES - Carry oxygenated blood to tissues → (think Away from the heart) VEINS - Carry deoxgenated blood back to the heart Electrical Conduction of the Heart MNEMONIC Send A Big Bounding Pulse © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. SA Node ↓ AV Node ↓ Bundle of His ↓ Bundle Branches ↓ Purkinje Fibers 102 AUSCULTATING HEART SOUNDS 5 Areas for Listening to the Heart All People Enjoy Time Magazine Aortic Right 2nd intercostal space Pulmonic Left 2nd intercostal Space ERB’s Point (S1, S2) Left 3rd intercostal space Tricuspid Lower left sternal border 4th intercostal Mitral Left 5th intercostal, medial to midclavicular line TIP NORMAL Tricuspid & mitral valve closure S2 Aortic & pulmonic valve closure LUB ↓ Closing of the valves Valve opening does not normally produce a sound S3 Early Diastole in rapid ventricle filling S4 Late Diastole & high atrial pressure (forcing blood into a stiff ventricle) ↓ SYSTOLE: Ventricle pump / ejection = LUB (S1) DIASTOLE: M S1 DUB ABNORMAL M DUB (S2) © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. ry Memo Trick Extra q sounds “COZY RED” CO (contract) ZY (systole) RE (relax) D (diastole) 103 EKG WAVEFORMS SIGNS & SYMPTOMS PQRST P Atrial contraction (squeeze) DE-polarization DE-compressing QRS Ventricle contraction (squeeze) DE-polarization P COMPLEX DE-compressing T T Ventricles RE-laxing RE-polarizing PR INTERVAL QRS ST SEGMENT Movement of electrical Time between ventricular deactivity from atria to ventricles polarization and repolarization (ventricular contraction) QT INTERVAL Time take from ventricles to depolarize, contract, and repolarize 5-LEAD PLACEMENT WHITE ON RIGHT RA CHOCOLATE IN MY HEART GREEN GOES LAST la SMOKE OVER... v rl © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. ll FIRE 104 6 STEPS TO INTERPRETING EKG’S BASIC RHYTHMS #1 P WAVE NORMAL SINUS 60 - 100 bpm SINUS TACHYCARDIA > 100 bpm SINUS BRADYCARDIA < 60 bpm Identify & examine the P waves • Should be present & upright • Comes before QRS complex • One P wave for every QRS complex #2 PR INTERVAL Measure PR interval #3 QRS WAVE Is every P wave followed by a QRS complex? 1 sec. Normal PR interval: 0.12 - 0.2 seconds Normal QRS complex: 0.06 - 012 0.04 sec. • Should not be widened or shortened W iden is ofte n – this may indicate problems! seen in PV C’s, Electrolyte imbalances #4 R-R 0.20 sec. 1 large box = 0.20 seconds 5 large boxes = 1 second Are the R to R intervals consistent 1 small box = 0.04 seconds • Regular or irregular? #5 DETERMINE THE HEART RATE 6 SECOND METHOD Be sure and chec k th the strip is 6 seco at nds! Count th e boxes Count the number of R’s in between the 6 second strips & multiply by 10 BIG BOX METHOD 300 divided by the number of big boxes between 2 R’s 1 2 3 4 5 6 R’s X 10 = 60 beats per minutes 300 / 5 = 60 BPM #6 IDENTIFY THE EKG FINDING! © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. 105 EKG’S NORMAL SINUS RHYTHM RATE RHYTHM P WAVE PR INTERVAL QRS COMPLEX 60 - 100 bpm Regular Upright & uniform before each QRS Normal R Normal T P QS SINUS BRADY KEY The sinus node creates an impulse at a slower-than-normal rate RATE RHYTHM P WAVE PR INTERVAL QRS COMPLEX < 60 bpm Regular Upright & uniform before each QRS Normal Normal CAUSES TREATMENT q Lower metabolic needs • Sleep, athletic training, hypothyroidism q Correct the underlying cause! q Vagal stimulation q Medications • Calcium channel blockers, beta blockers, Amiodarone q ↑ the heart rate to normal SINUS TACHY KEY The sinus node creates an impulse at a faster-than-normal rate RATE RHYTHM P WAVE PR INTERVAL QRS COMPLEX > 100 bpm Regular Upright & uniform before each QRS Normal Normal CAUSES TREATMENT q Physiologic or psychological stress • Blood loss, fever, exercise, dehydration q Identify the underlying cause! q Certain medications • Stimulants - caffeine, nicotine • Illict drugs - cocaine, amphetamines • Stimulate sympathetic response - epinephrine q ↓ the heart rate to normal q Heart failure q Cardiac tamponade q Hyperthyroidism © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. 106 EKG’S VENTRICULAR TACHYCARDIA (VT) ick: Memory tr e lik s ok lo s tombstone RATE RHYTHM P WAVE PR INTERVAL QRS COMPLEX 100 - 250 bpm Regular Not visible None Wide (like tombstones) > 0.12 seconds Irregular, coarse waveforms of different shapes. The ventricles are quivering and there is no contractions or cardiac output which may be fatal! CAUSES MANIFESTATIONS q Myocardial ischemia / infarction q q Electrolyte imbalances q Digoxin toxicity q Stimulants: caffeine & methamphetamines q q q q Chest pain Lethargy Anxiety Syncope q Palpitations No Card iac Outp = Low Oxy g ut en TREATMENT UNSTABLE CLIENTS WITHOUT A PULSE STABLE CLIENT WITH A PULSE Also called PULSLESS V-TACH q Oxygen q Antidysrhythmics (ex. Amiodarone...stabilizes the rhythm) q Synchronized Cardioversion • Synchronized administration of shock (delivery in sync with the QRS wave). q CPR q q Possible intubation q Drug therapy SHOCK! • Epinephrine, vasopressin, amiodarone • Cardioversion is NOT defibrillation! (defibrillation is only given with deadly rhythms!) UNTREATED VT CAN LEAD TO ↓ VENTRICULAR FIBRILLATION ↓ DEATH © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. 107 EKG’S VENTRICULAR FIBRILLATION (V-FIB) Rapid, disorganized pattern of electrical activity in the ventricle in which electrical impulses arise from many different foci! RATE RHYTHM P WAVE PR INTERVAL QRS COMPLEX Unknown Chaotic & irregular Not visible Not visible Not visible CAUSES MANIFESTATIONS q Cardiac injury q Loss of consciousness q Medication toxicity q May not have a pulse or blood pressure q Electrolyte imbalances q Respirations have stopped q Untreated ventricular tachycardia q Cardiac arrest & death! No Card Outputiac no Ox to the ybgen ody = TREATMENT q CPR q Drug Therapy • Vasoconstriction: Epinephrine q Oxygen q Defib (follow ACLS protocol for defibrillation) q Possible intubation TIP • Antiarrhythmic: Amoidaraon, lidocaine • Possibly magnesium “Defib the Vfib” Cardioversion vs. Defibrillation CARDIOVERSION DEFIBRILLATION q Synchronized shock q Asynchronous q Lower amount of energy q Higher amount of energy q Not done with CPR q Resume CPR after shock q Stable clients q Unstable clients q Ex. A-fib © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. KEY q Example: pulseless VT or VF 108 EKG’S ATRIAL FIBRILLATION (A-FIB) irregular r-r intervals ↓↓ ↓ ↓ ↓ RATE RHYTHM P WAVE PR INTERVAL QRS COMPLEX Usually over 100 BPM Irregular Visible Normal Uncoordinated electrical activity in the atria of the muscles in the atrium. The atri a is quiverin g! CAUSES MANIFESTATIONS q Open heart surgery q Most commonly asymptomatic q Heart failure q Fatigue q COPD q Malaise q Hypertension q Dizziness q Ischemic heart disease q Shortness of breath q Tachycardia All due to low 02 q Anxiety q Palpitations TREATMENT STABLE PT. UNSTABLE PT. q Oxygen q Oxygen q Drug therapy! q Cardioversion • Synchronized administration of shock (delivery in sync with the QRS wave). • Beta blockers • Calcium channel blockers • Digoxin • Amiodarone defibrillation • Anticoagulant therapy to prevent clots Risk for clots! Defibrillation is only given with deadly rhythms! The atria quiver causes pooling of blood in the heart which increases the risk for clots = increased risk for MI, PE, CVA’s, & DVTs! © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. 109 EKG’S PREMATURE VENTRICULAR CONTRACTIONS (PVCS) RATE Depends on the underlying rhythm RHYTHM Regular but interrupted due to early P waves P WAVE Visible but depends on timing of PVC (may be hidden) PVC PR INTERVAL Slower than normal but still 0.12 - 0.20 seconds QRS COMPLEX Sharp, bizarre, and abnormal during the PVC Early “premature” conduction of a QRS complex CAUSES BIGEMINY: every other beat TRIGEMINY: every 3rd beat QUADRAGEMINY: every 4th beat q Heart failure q Myocardial ischemia / infarction q Drug toxicity q Caffeine, tobacco, alcohol q Stress or Pain Exercise Fever Hypervolemia Heart failure Tachycardia R-ON-T PHENOMENON: PVC arises spontaneously from the repolarization q Increased workload on the heart TREATMENT MANIFESTATIONS q May be asymptomatic *TX based on underlying cause* q Feels like your heart... q May not be harmful if the client has a healthy heart • “Skipped a beat” q Oxygen • “Heart is pounding” q Decrease caffeine intake q Chest pain q Correct the electrolyte imbalances q D/C or adjust the drug causing toxicity q Decrease stress or pain Chest pain Notify the healthcare provider if the client complains of chest pain, if the PVC’s increase in frequency or if the PVC’s occur on the T wave (R-on-T phenomenon). ASYSTOLE RATE RHYTHM P WAVE PR INTERVAL QRS COMPLEX CAUSES q Myocardial ischemia/infarction q Heart failure q Electrolyte imbalances (common: hypo/hyperkalemia) q Severe acidosis q Cardiac tamponade Flatline TREATMENT q High quality CPR • Heel of hand on the center of the chest • Arms straights • Shoulders aligned over hands • Compress at 2 - 2.4 inches at a rate of 100 - 120 min • 30 compressions to 2 rescue breaths • Minimal interruptions q Cocaine overdose © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. 110 EKG’S ATRIAL FLUTTER Sawtooth RATE 75-150 BPM RHYTHM Usually regular P WAVE “Sawtooth PR INTERVAL Unable to measure QRS COMPLEX Usually normal & upright signals spread through the atria. The heart’s upper chambers (atria) beat too quickly but at a regular rhythm. CAUSES MANIFESTATIONS q Coronary artery disease (CAD) q May be asymptomatic q Hypertension q Fatigue / syncope q Heart failure q Valvular disease q Hyperthyroidism q Chronic lung disease q Chest pain q Shortness of breath q Low blood pressure q Pulmonary embolism q Cardiomyopathy TREATMENT STABLE PT. UNSTABLE PT. q Drug therapy! q Cardioversion • Calcium channel blockers • Antiarrhythmics • Synchronized administration of shock (delivery in sync with the QRS wave). • Anticoagulants Risk for clots! defibrillation Atrial flutter causes pooling of blood in the atria = risk for clots Defibrillation is only given © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. 111 HEART FAILURE TOMS SIGNS & SYMP LEFT SIDED HF RIGHT SIDED HF Left Side Think Lungs Fluid is backing up into the lungs = pulmonary symptoms d yspnea OTHER S& S r ales (crackles) ↑ UOP Hypote nsion S3 Gall op o rthopnea w eakness / fatigue Fluid is backing up into the venous system s welling of the legs & hands w eight gain e dema (pitting) l arge neck veins (JVD) l ethargy / fatigue n octurnal paroxysmal dyspnea i rregular heart rate i ncreased HR n agging cough (frothy, blood tinged sputum) g aining weight (2 -3 lb's a day) n octuria g irth (Ascites) OTHER S& S Hepato megaly Spleno megaly Anorex ia SYSTOLIC HF VS. DIASTOLIC HF SYSTOLIC HF DIASTOLIC HF Weakened heart muscle Stiff & non-compliant heart muscle The ventricle does not EJECT properly The ventricle does not FILL properly EF Reduced Normal EF © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. EJECTION FRACTION (EF) Amount of blood pumped out Amount of blood in the chamber % EF Normal Ejection Fraction 50% - 70% 112 HEART FAILURE: DIAGNOSIS & INTERVENTIONS DIAGNOSIS BNP CHEST X-RAY ECHOCARDIOGRAM B-TYPE NATRIURETIC PEPTIDE Secreted when there is ↑ pressure in the ventricle Looks at ejection fraction, Enlarged heart & EF is ↓ in most types of HF BNP ↑ in HF INTERVENTIONS Diet Modifications Monitor Fluid restrictions ↓ Sodium ↓ Fat ↓ Cholesterol Strict I&O’s Daily weights Edema Same time Same scale Same clothes Report S&S of fluid retention Rep ort w (2-3 t. gai lbs) n Spread fluids out during the day Suck on hard candy to ↓ thirst Elevate hob (Semi-Fowler’s position) Balance periods of activity & rest Edema Weight gain © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. 113 CORONARY ARTERY DISORDERS (CAD) PATHO RISK FACTORS Non-modifiable Age Gender Race Family history Modifiable Diabetes Obesity Hypertension Physical inactivity Smoking High cholesterol Metabolic Syndrome SIGNS & SYMPTOMS ISCHEMIA Inadequate blood supply to the heart = ↓ O2 to the heart. Ischemia: ↓ O2 Infarction: Death ANGINA PECTORIS Chest pain that is caused by myocardial ischemia • Chest pain w/ activity • Shortness of breath • Fatigued Cholesterol Called atherosclerosis ↓ Restriction of blood flow to the heart • Management of hypertension • Management of diabetes • Smoking cessation • Diet • Exercise TREATMENT blood test • LDL • HDL • Total Cholesterol • Triglycerides ECG • Assess for changes in ST segments or T waves! Low Density Lipoprotein ↓ PREVENTION DIAGNOSIS LDL Fatty plaques develop Want LOW Levels (<100 mg/dL) BAD CHOLESTEROL © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. • Lipid-lowering medications “Statins” • Heart-healthy diet WEEKL • Physical activity EXERCISE GOY ALS Moderate • Smoking cessation : 75 min Vigorous: 150 min • Stress management • Hypertension management • Diabetes management • Coronary stent / angioplasty • Coronary Artery Bypass Graft (CABG) HDL High Density Lipoprotein Want HIGH Levels (>60 mg/dL) HAPPY CHOLESTEROL 114 PERIPHERAL VASCULAR DISEASE is an umbrella term for... PERIPHERAL VENOUS DISEASE (PVD) PERIPHERAL ARTERIAL DISEASE (PAD) Narrow artery (atherosclerosis) where oxygenated blood can’t get to the distal extremities (hands & feet). Deoxygenated blood can’t get back to the heart. Pooling of oxygenated blood in the extremities. Dull, constant, achy pain! Pulse ? May not be palpable due to edema Edema ? TE AR ART RY IN VE VEI N x po of boling lood Ischemia & necrosis of the extremities ER Y pain ? Think “BAD” lood no bo O 2 n Sharp pain: Gets worse at night “rest pain” pain ? Intermittent claudication Pulse ? Very poor or even absent x Edema ? Blood is POOLING the leg No blood in theinextremities No blood in the extremities Temp ? Warm legs (Blood is warm) Temp ? Cool No blood = cool leg Color ? Stasis dermatitis (Brown/yellow) Color ? Pale, hairless, dry, scaly, thin skin due to lack of nutrients (↓ O2 ) Wounds ? Venous STASIS ulcers, Irregular shaped wounds, shallow Wounds ? Regular in shape, red sores round appearance “punched out” Gangrene ? Elevate Veins Tissue death caused by a lack of blood supply Gangrene ? We have too much blood! Gangrene is caused by insufficient amounts of blood. Positioning ? (blood is warm) Positioning ? Positions that make it worse: dangling, sitting/standing for long periods of time Dangle arteries CAUSES OF BOTH Smoking • Diabetes • High cholesterol • Hypertension DX: Doppler Ultrasound or Ankle Brachial Index (ABI) TREAMENT • Elevate KEEP VEIN OPEN! Veins • Medications TREAMENT A GET BLOOD MOVING! • D ngle Arteries (Dependent position) • Perform daily skin care with moisturizer - Aspirin or Clopidogrel • Stop smoking - Cholesterol lowering drugs “statin” • Avoid tight clothing (vasoconstriction) • Surgery - Angioplasty • • Medications - Bypass (CABG) - Vasodilators - Endarterectomy - Antiplatelets © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. 115 ANGINA PECTORIS Chest pain that is caused by myocardial ischemia TYPES OF ANGINA STABLE UNSTABLE PRINZMETAL’S / VARIANT “Predictable” “Preinfarction” “Coronary artery vasospasm” Occurs with Occurs at Pain at rest with reversible ↑ myocardial demand for oxygen & more frequently st-elevation rest exertion MANIFESTATIONS INTERVENTIONS Goal: • Chest pain (heavy sensation) may radiate to neck, jaw, or shoulders • Unusual fatigue • Weakness • Shortness of breath • Pallor • Diaphoresis ↓ oxygen demand Reperfusion Procedures PCI Percutaneous Coronary Interventions CABG Coronary Artery Bypass Graft DRUG THERAPY nitrates Calcium Channel Blockers beta blockers • Vasodilators • Relaxes blood vessels • ↓myocardial oxygen • Prevents platelet • ↓ischemia = ↓pain • ↑oxygen supply to the consumption aggregation & • Usually administered heart sublingually • ↓workload of heart © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. Antiplatelet / Anticoagulant thrombosis 116 MYOCARDIAL INFARCTION (MI) angina Coronary arteries become narrow due to plaque build-up ↓ artherosclerosis SIGNS & SYMPTOMS Sudden, crushing, radiating chest pain that continues despite rest & medications • Shortness of breath • Nausea & vomiting • Sweating • Pale & dusty skin WOMEN PRESENT WITH DIFFERENT SYMPTOMS Due to ischemia (low O2) ↓ PATHO Complete blockage in one or more arteries of the heart Pain felt in the... • Left arm • Mid back/shoulder • Heartburn • Fatigue • Shoulder blade discomfort • Shortness of breath Myocardial Infarction (mI) Plaque rupture become a blood clot that blocks arteries of the heart DIAGNOSIS - ECG • ST-Elevation (no O2) • ST-Depression (low O2) T-wave inversion - Troponin - Stress test • Chemical & excercise TREATMENT immediate m MORPHINE o OXYGEN n a ↓workload of the heart & ↓ pain ↑O2 to the heart NITROGLYCERIN opens up the vessels ASPRIN Prevents platelets from sticking together cath lab or clot buster Medications • Thrombolytics (clot busters) Prevention & Rest -teplase -ase prevent / stabilize clot • Heparin IV • Example: Streptokinase Rest the heart with... Surgery • Nitro • PCI “Percutaneous • Beta-Blockers Coronary Intervention” • Calcium channel blockers • CABG • Endarterectomy ANY TIM E YOU GI - Cut out the blockage V © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. E A THROM BOLYTIC, WATCH F OR SIGNS BLEEDING OF ! 117 CARDIAC BIOMARKERS TROPONIN Protein released in the blood stream when the heart muscle is damaged. There are 3 isomers of troponin Troponin C: binds calcium to activate muscle contraction Troponin I & T: TROPONIN I RANGE PEAK 0 - 0.4 ng/mL > 0.4 = Heart attack! Can remain elevated for as long as 3 weeks BEST indicator of an acute MI CK-MB Creatine Kinase - MB An enzyme released in the bloodstream when the heart, muscles or brains are damaged! Cardiac-specific isoenzyme BUT less reliable than Troponin MYOGLOBIN Myoglobin is found in cardiac & skeletal muscle but a (-) sign is good for ruling out an acute MI Myoglobin Think Muscle BNP Brain Natriuretic peptide RANGE PEAK RANGE PEAK RANGE 0 - 5 ng/mL 24 Hours 5 - 70 ng/mL 12 hours Normal: <100 pg/mL Mild HF: 100 - 300 Moderate HF: 300 - 700 Severe HF: >700 Indicates heart failure (HF) © 2021 NurseInTheMaking LLC. Sharing and distributing this copyrighted material without permission is illegal. 118