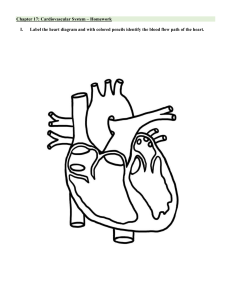
Biosignal Analysis Part 2 ECE 4923: Mar 14, 2022 (Lec 15) Last Updated: Mar 13, 2022 Administrative Matters • Assignment 1 – Due March 25, 2022 (5 pm) • Lab 3 – Mar 21, 2022 - CircuitLab – registration • Quiz 2 – Date (Mar 23?) and Syllabus? • Seminar presentations - Mar 25 to April 11 - Any no-go days for your team? • Assignment 2 – will be open this Friday (Mar 18) 2 Quick Recap • MES> MUAPT> SFAPT • Innervation point or innervation zone? • EMG amplitude measurement – MAV, RMS 3 Outline (Mar 14, 2022) • ECG • Review of Mechanical and electrical activity • Clinical ECG- Standard lead configurations • Diagnosis with ECG • EEG • • Frequency bands Diagnosis – Useful indicators and sleep patterns • EMG • Generation of muscle force • Muscle Force Twitch • Force and MES estimation of force 4 Autonomic Nerve Amplitude (mV) Electrocardiography (ECG) 1 0.5 0 -0.5 1 2 Time (sec) 3 ECG References: Chapter 5- Richard Normann, Principles of Bioinstrumentation, https://ecgwaves.com/topic/ekg-ecg-leads-electrodes-systems-limb-chest-precordial/ 5 Let’s recall (1) • ECG = surface level measurement of the electrical activity of cardiac muscles. • Also known as EKG • Cardiac electrogram – when electrodes are placed on or in the heart to measure the electrical activity. • Self excitation property (don’t need a nerve to initiate the firing) • The muscle fibres fire more or less synchronously 6 Let’s recall (2) – Mechanical activity Image Source: Saladin, Anatomy and Physiology : Unity of Form and Function, McGraw Hill Publication, 2017 7 Let’s recall (3) – Electrical activity • Pacemaker cells: - Those groups of cells that have the ability to pace the heart. - 3 such groups - SA node, AV node, Bundle of His & Purkinjee fibres • Diastole and systole phases (the rest and the active phase) 8 Let’s recall (4) – Electrical Activity • Rest phase – atria fill with blood. There is no electrical activity. • 2) The SA node depolarizes spontaneously, and waves of depolarization move from the SA node across the atria – causing a mechanical contraction pushing the blood into the ventricles 9 Let’s recall (5) – Electrical Activity 3) AV node then delays the depolarization spread to ensure that the ventricles are filled 4) Purkinjee fibres conduct the depolarization wave very rapidly – causing the ventricles to contract from the bottom upwards. (Ventricular depolarization) 5) Ventricles repolarize (T wave) and return to the rest phase. 10 GENERATION OF ECG Amplitude (mV) FORMATION OF THE ECG SIGNAL 1 0.5 0 -0.5 1 2 Time (sec) 3 Sources: adapted from Bioelectromagnetism - Principles and Applications of Bioelectric and Biomagnetic Fields by Malmivuo and Plonsey, Oxford University Press, 1995. 11 Clinical Electrocardiography • Clinicians observe the shape, duration, amplitude, etc of the ECG as compared to the normal ECG to detect diseases. • But these parameters all depend on the electrode configuration used in the measurement. So standard “lead” configurations are used. • ECG lead – is a graphical description of the electrical activity and is computed by analysing electrical currents detected by several electrodes. 12 Standard 12 Lead configuration • 12 lead display – has 12 curves derived from 10 electrodes that are placed on standard location. • 6 leads come from 4 electrodes placed on the limbs. • 6 leads come from the 6 electrodes placed on the chest. 13 Limb Leads • All the limb leads use the electrode on the RL to be the ground electrode. • Standard electrode leads are (1) RA – LA (2) RA – LL (3) LA - LL 14 Augmented Limb leads • Augmented limb leads use stand limb electrode configuration, but the electrodes are connected through resistors to a common node. • This decreases the noise level and increases the size of the apparent signal. Image source: https://ecgwaves.com/topic/ekg-ecg-leads-electrodes-systems-limb-chest-precordial/ 15 Einthoven's Triangle (1) • Leads I, II and III form the original leads constructed by Wilhelm Einthoven. • Their spatial orientation forms a triangle in the chest. 16 Einthoven's Triangle (2) • Based on Kirchoff’s current law: 𝐿𝑒𝑎𝑑 𝐼 + 𝐿𝑒𝑎𝑑 𝐼𝐼𝐼 = 𝐿𝑒𝑎𝑑 𝐼𝐼 • So we only need information from two leads to calculate the exact appearance of the remaining lead. 17 Einthoven's Triangle (3) – Augmented Leads 𝐿𝑒𝑎𝑑 𝐼 − 𝐿𝑒𝑎𝑑 𝐼𝐼𝐼 𝑎𝑉𝐿 = 2 𝐿𝑒𝑎𝑑 𝐼 + 𝐿𝑒𝑎𝑑 𝐼𝐼 𝑎𝑉𝑅 = − 2 𝐿𝑒𝑎𝑑 𝐼𝐼 + 𝐿𝑒𝑎𝑑 𝐼𝐼𝐼 𝑎𝑉𝐹 = 2 18 Chest Leads 19 Presentation of ECG 20 ECG signal processing specs • Bandwidth: 0.1 – 100 Hz • Gains: between 100 to 5000 (usually much smaller than EMG as the signal is larger) • CMRR: 100 dB or above • Input resistance: >100 MΩ 21 Diagnosis with ECG (1) Hate Rate: 60-100bpm 1 p-wave for each QRS-complex (0.06-0.1 sec) Normal ECG Sinus Brachacardia Sinus Tachacardia HR<60-100bpm HR>60-100bpm Source: figures extracted from http://courses.cs.washington.edu/courses/cse466/13au/pdfs/lectures/ECG_filtering.pdf 2015 Asystole 22 Diagnosis with ECG (2) Abnormal Ventricular Conditions Abnormal Atrial Conditions Ventricular Tachycardia Atrial Flutter Sawtooth appearance resulting from a focused irritation in atria causing too many but regular P-waves Regular plateaued appearance resulting from a focused irritation in the ventricles Atrial Fibrillation Ventricular Fibrillation chaotic appearance within irregular QRScomplexes resulting from a unfocused irritation causing fibrillatory atrial reaction Chaotic appearance void of QRScomplex resulting from unfocused irritation in the ventricles causing fibrillatory ventricular reaction Source: figures extracted from http://courses.cs.washington.edu/courses/cse466/13au/pdfs/lectures/ECG_filtering.pdf 2015 23 Markers for a Myocardial Infarction (Aka Heart Attack) • ECG measurements can carry tell-tale signs that a heart attack has taken place, even if the patients themselves didn’t notice it. • The ST segment acts as a marker. 24 Source: figures extracted from immflife.com/Heat-attack.html