Myocardial Infarction: Causes, Symptoms, Diagnosis & Treatment
advertisement

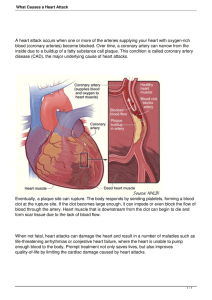
Clot is formed, and this leads to the arteries being blocked. This is a bit like a pipe that has a blockage, which causes limited amount of water to go through it. In this case there is limited amount of blood flow. Myocardial infarction What is myocardial infarction? Myocardium: this is the heart muscle. This is like any muscle, where of you do not get enough oxygen to it, you get a cramp. Infarction: Obstruction of the blood supply to an organ or region of tissue, typically by a thrombus or embolus, causing local death of the tissue. This starve the muscles of the nutrients and oxygen Myocardial Infarction happens when there is a sudden loss of blood flow to a part of your heart muscle, usually caused by a clot. This can be found when cardiologists do angiograms. The angiogram will show which artery is occluded and by how much percent. This will allow the cardiologist to use stents to open the artery depending on how occluded it is. The diagram on the left shows the arteries/areas of the heart the angiogram looks at. The angiogram look at what percentage the artery is occluded and allows treatment, such as putting stents in. What causes a myocardial infarction? MI is a heart attack! HCP call it an MI. Why?!! A wide range of conditions that can cause a reduction in blood blow to the coronary arteries-these are known as acute coronary syndromes. 1. Nearly always coronary heart disease- condition where the inside of one or more of the coronary arteries becomes narrowed 2. Why?- fatty deposits (atheroma) build up within the artery walls 3. The fatty area of atheroma in the artery wall is called a plaque 4. If a plaque cracks- a blood clot forms to try to repair the damaged artery wall. This causes platelet accumulation and so the size of the plaque increases causing the artery to be occluded. This is where you get 60%/40% flow through the artery. 5. This blood clot can totally block your coronary artery, causing part of your heart muscle to be starved of blood. PY6030 De Silva- 5th October 2018 This is when you experience angina 6. If this happens, the affected part of your heart muscle will begin to die, because it is not getting oxygen. This is a heart attack Other causes: Ø Inflammation of the coronary arteries (rare). Ø A stab wound to the heart. Ø A blood clot forming elsewhere in the body (for example, in a heart chamber) and travelling to a coronary artery where it gets stuck. Ø Taking cocaine, which can cause a coronary artery to go into spasm. Ø Complications from heart surgery. Atheroma formation is the primary cause Ø Some other rare heart problems- congenital heart defects Acute coronary syndromes (ACS): Two main subtypes of ACS can be diagnosed by what is seen on your heart tracing (electrocardiogram, or ECG). ST-elevation MI (STEMI) and non-ST-elevation MI (NSTEMI). NSTEMI can also include unstable angina, happens when sitting. Most people with angina chest pains only have pain with a certain amount of exertion. This is called stable angina. If the pattern of your pain changes suddenly and the pains develop after minimal exertion, or while you are resting, this is called unstable angina. NSTEMI, the artery is only partly blocked, so only part of the heart muscle supplied by the affected artery is affected STEMI, the artery supplying an area of the heart muscle is completely blocked Your treatment and management can depend upon which type you have - STEMI or NSTEMI. Who is more likely to get ACS? • • • • Most occur in people aged over 50 years and then increases with age-can happen at a young age A heart attack is three times more common in young men than in young women (This is from 45 years old onwards.) However, after the menopause, the female hormones no longer protect the heart (as the cardio-protective hormones are no longer produced) so the risk is then the same for men and women. A heart attack may occur in people known to have heart disease, such as people with chest pain called angina. It can also happen suddenly in people with no previous symptoms of heart disease. This is because fatty patches or plaques (atheroma) often develop without any symptoms at first Family history- Your risk is increased if there is a family history of heart disease or a stroke that occurred in your father or brother aged below 55, or in your mother or sister aged below 65. PY6030 De Silva- 5th October 2018 • • • • • • • This shows that it has to be your primary relative, so not your grandparents, unless this has affected your parents. Ethnic group- Certain ethnic groups - for example, British Asians - have a higher risk of developing cardiovascular diseases Smoking High blood pressure Overweight- Losing weight will reduce the amount of workload on your heart and also help to lower your blood pressure. High Cholesterol Inactive lifestyle- According to the NICE guidelines you should be doing 150 minutes of exercise every week. This is moderate exercise that increase your heart rate and makes you sweat. Poor Diet • Saturated fats may also contribute to the build-up of plaque in the coronary arteries. Saturated fats are found mostly in meat and dairy products, including beef, butter, and cheese. These fats may lead to an arterial blockage • Another type of fat that contributes to clogged arteries is trans-fat, or hydrogenated fat. Trans-fat is usually artificially produced (processed) and can be found in a variety of processed foods. Trans-fat is typically listed on food labels as hydrogenated oil or partially hydrogenated oil • Also patients with high salt intake may be at higher risk Patient can improve their diet by: Reducing their salt intake Increasing their intake of unsaturated fats Decrease saturated/trans fats Increasing intake of pulses/brown rice/brown flour in bread Increasing portions of fruit and veg. This should be five portions (a handful) of different ones (different colours) do not overcook them as it takes out the nutrients and value in them. You need to mindful of fruits as they have high sugar content, may lead to diabetes, which is a risk factor for MI Û Avoid mango juice/cranberry juice as it may be problematic with medication Û Kale can also be problematic with mediation Û Eat fish Û Û Û Û Û • Diabetes- this can lead to a silent MI, where the typical symptoms of MI are not seen. For example Dr Silva’s dad is diabetic and had a silent MI, where he experienced a flutter in his heart and flu like symptoms. Other symptoms that may be experienced include; chest pain or shortness of breath. What are the symptoms of MI? v Pressure or tightness in the chest, then radiating down left arm. Chest pain can be dismissed as being, dyspepsia, which is GI disturbances. When people get acid. PY6030 De Silva- 5th October 2018 v Pain in the chest, back, jaw, and other areas of the upper body that lasts more than a few minutes or that goes away and comes back v Shortness of breath v Sweating v Nausea v Vomiting v Anxiety (clammy) v A cough v Dizziness v A fast heart rate (tachycardia) Diagnosis: • • • • • § ECG Evaluation of history and symptoms (SOB/chest pain/ clammy in extremities) Blood test called a troponin test (proteins inside heart cells, which are released very slowly when the heart cells are damaged.) Physical examinations (blood pressure and monitoring your heart rhythm and heart rateirregular as there has been an artery that has been occluded.) Troponin levels- Troponins are proteins that are normally found within the cells of the heart. If your heart muscle is damaged, troponins leak into your blood, where they can be detected by a blood test. They are released into your bloodstream quite slowly, so the level of troponin in your blood rises gradually over a few hours. This means that the troponins may only be detected several hours after the start of the symptoms of a heart attack. This is why the troponin test is not used as a way to decide on immediate treatment. A troponin test can help show if there is damage to your heart muscle. If your troponin test is positive – that is, if you have a high level of troponins in your blood – it means that you have had a heart attack. If the troponin test is negative several hours after your symptoms first started – that is, if you don’t have a high level of troponins in your blood – it means that your heart muscle was not damaged. This would confirm a diagnosis of unstable angina What are the treatment aims when someone has had an MI? 1. Relieve pain 2. Relieve anxiety- you would be stressed and worried if you knew you were having a heart attack 3. Relieve nausea 4. Prevent further damage to myocardium- sooner treat patient the better 5. Re-vascularize coronary artery/ies- this means that there is blood perfusion as soon as possible, to the relevant artery/ies. PY6030 De Silva- 5th October 2018 6. Prevent/treat complications 7. Stop it happening again Treatments: You use oxygen if the saturations is less than 94%, it can help with perfusion as you have no oxygen going to the myocardium as you have had a vessel cut off. This means that saturating and putting oxygen into the body will improve things and help things. Also for patients it does calm the down to have an oxygen mask on. • If you have a heart attack, you need to have treatment as soon as possible. This will be to get the blood flowing to the damaged part of the heart muscle again as quickly as possible, and to limit the amount of permanent damage to your heart. • Emergency treatment to unblock the coronary artery: o Either you will have a treatment called primary angioplasty (sometimes called primary PCI), which is a procedure to re-open the blocked coronary artery. (PCI stands for percutaneous coronary intervention.) o Or you will have thrombolysis, which means giving you a ‘clot-busting’ medicine to dissolve the blood clot that is blocking the coronary artery. 1. Pain-IV Morphine/Diamorphine Ø Diamorphine 2mg IV(Can use Morphine) Ø Increase in increments until pain free Ø Don’t give by any other route – onset too slow. If it is given orally (patient may be nauseous) or intramuscularly it can cause complications with reperfusion Ø IM can cause reperfusion problems The treatment of the pain also relieves Ø Outcome – relieve pain/ relieve anxiety anxiety. This is as the cause of anxiety is Ø Side effects/ reactions: Makes feel sickthe pain. The diamorphine ttakes away Treatment of the already nauseated, respiratory depression pain hence reduces fear. This means that nausea. Parenteral – (high doses.) it acts as an anxiolytic/euphoric effect IV if possible. Ø Morphine equally effective as diamorphine Cyclizine if LVF not When choosing the pain relief avoid Ø Should be given as early as possible compromised. sedatives if possible Ø No real point in other analgesia as Metoclopramide Diamorphine/morphine should work. It is otherwise. Both not ideal to use sedatives. written up on drug chart, you choose which one is better. 2. Glyceryl trinitrate (GTN spray/IV GTN). This allows vasodilation and relieves ischemic pain 3. For revascularization: NICE- The sooner the blood flow can be restored, the better the chances of avoiding death of the heart muscle.’ Death if heart muscle is long ter, this will compromise PY6030 De Silva- 5th October 2018 left ventricular function. This will lead to heart failure as heart is not strong enough to push blood around the body. Use on thrombolytic: they do not treat or break the 4. Thrombolysis (also aids with revascularization) clot but prevent a further clot from being formed. • PTCA/PCI (PCI is percutaneous coronary intervention) – treatment of ¨ Bleeding complications main risk choice unless contra indicated (if patient very unstable such as very ¨ Haemorrhagic stroke 0.5 – 1% elderly patients) and if available as ¨ Risk increases with age & raised BP research shows best outcomes. Patients must consent and relatives ¨ Bleeding at injection site, GI tract or elsewhere can consent on their behalf, this is as ¨ Hypotension hemorrhaging is a risk and bleeding is side effect. Interventional methods ¨ Risks and benefits assessed more effective. PTCA +/- Glycoprotein IIb/IIIa inhibitor. PTCA needs specialist ¨ C/I. Hx of bleeding disorders. Recent facilities + interventional cardiologist. haemorrhage, trauma, surgery or CVA Abciximab only one indicated for use with PTCA. PTCA + Glycoprotein IIb/IIIa inhibitor (e.g. Abciximab, Eptifibatide, Tirofiban. These reduce risk of immediate vascular occlusion and are used for intermediate/high risk patients) + heparin/ LMWH. There are mobile cath labs that allow this to happen quickly. (You can also use Bivalirudin instead of Glycoprotein IIb/IIIa inhibitor, but there is risk of bleeding) • • Anti-platelets: Aspirin (unless allergic or already had). This will prevent further coagulation, this is long term. Has independent improvement in mortality. It is an additive to thrombolysis. Unless C/I give 150-300mg. It is chewable or in water. It is given ASAP, with Clopidogrel 300mg, (600mg if prior to PTCA, so there’s really thin blood flow for when they go in).Other ones are heparin and LMWH such as foundaparinux. Anticoagulants: Clopidogrel or alike. Not streptokinase. How is angioplasty performed? à Usually, angioplasty is performed while the patient is under local anesthesia. à An incision is made in the patient's arm or groin to insert a flexible tube called catheter. à A thin wire called the guidewire is passed across the narrow segment of the blocked artery-Supports vessel à Then the catheter with a small uninflated balloon is inserted inside on the end of the artery. PY6030 De Silva- 5th October 2018 à Using iodine dye and X-ray camera the catheter with the balloon is threaded to the blockage of the artery over the guidewire. à Once the position is set, the inflatable balloon is inflated to remove the blockage and widen the artery. This happens because the plaque or fatty deposits gets pushed against the wall of the artery due to the inflation. à The balloon may be inflated several times to flatten the plaque against the wall of the artery. This way, the plaque that extends into the wall of the artery may crack or tear. This is necessary and normal. à Once this is done, the balloon is deflated. X-ray pictures are taken to make sure that the blockage is gone. Then the balloon is removed along with the catheter. à In some cases, a stainless steel mesh called stent may also be attached to the catheter. This stent holds the blood vessel open. The stent may be drug eluting which have antiplatelet effect. This can remain in the artery after the balloon is deflated and removed. à The procedure of angioplasty ends with the closure of the incision site where the catheter was inserted Cost of thrombolytics: Streptokinase is the cheapest as it is the oldest and has been on the market longer so more pharmaceutical companies are making it. It was carried by paramedics, but it’s an half an hour infusion so there’s risk of hemorrhaging. Choice based on: a. Effectiveness b. Safety c. Cost – hospital costs d. Convenience to give – time to give, complexity of infusion, weight based doses 5. Beta-blockers: • Early treatment shown to be of benefit • Common one is atenolol • No C/I • IV Atenolol 5mg over 5 minutes • Repeat after 10-15 minutes • IV Metoprolol alternative • Timolol also in studies PY6030 De Silva- 5th October 2018 This takes 30-60 seconds to work. The locality will depend which hospital pays for which one. All hospitals will have streptokinase. Long-term management: Ø Aspirin + Clopidogrel, after a heart attack, keep after 12 months only. Ø Statins, to lower cholesterol. The dose you start on is 80mg Ø ACE inhibitors you start and then titrate up. This is done every one to two week providing that your blood pressure allows it. PY6030 De Silva- 5th October 2018