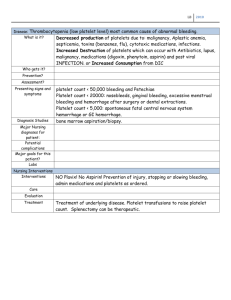
Hematologic Disorders Katherine Schafer, MSN, APRN, PCNS-BC, CNL, CCRN-K, CHSE Instructor Women, Children, & Family Nursing Anemias Iron Deficiency Aplastic Anemia Sickle Cell Disease Beta Thalassemia Let’s Begin with a Case Study M. is a 2 year-old male who was admitted to the inpatient pediatric unit for pneumonia. He is on Day 3 of antibiotic therapy and has been afebrile for 24 hours. T 98.8 axillary, HR 136, RR 22, BP 100/60, SaO2 95% on 1L O2 per NC. The night nurse reports he is drinking well, so his IVF were decreased to a KVO rate. His mother is at the bedside. You complete your 8 AM assessment. Significant Findings: Generally thin, but well-appearing child. Lethargic and uninterested in playing. Skin pale & cool to the touch. Pulses 3+, Cap refill 2 seconds. Lungs with adequate air exchange, bilateral coarse sounds. S1 & S2 heart sounds with splitting of S2. No appetite. What other information would you like? Additional Information Eats pasta, cheese, crackers, chicken nuggets, & “McDonalds” Drinks about 1 quart of cow’s milk per day Does not take a multivitamin Favorite activities: “video games” & “watching cartoons” Sleeps 16 hours per day. Falls asleep easily & “everywhere” Lives in a 70 year-old home with parents & 8 year-old sibling CBC Results WBC: 6.5 RBC: 4.1 HGB: 10.9 HCT: 29.5 MCV: 69 MCHC: 19 Retic: 0.8% Range: 5.5 – 15.5 Range: 3.1 – 4.5 Range: greater than 11.5 Range: greater than 33.5 Range: greater than 80 Range: 24-30 Range: 0.5% - 2.0% Iron Related Tests Serum Ferritin: 2 ng/ml Range: 7 – 142 ng/ml Total Iron: 30 mcg/dl Range: 50 – 120 mcg/dl Pb Level Lead level: 4 mg/dl Reference Range: greater than 5 mg/dl requires further investigation Iron Deficiency Anemia Most common cause of anemia Rare before 4 to 6 months of age Etiology AAP recommends screening during infancy, early/late childhood, and adolescence Decreased iron intake Increased iron or blood loss Increased growth rate (children) Can be associated with lead poisoning Family education is critical Collaborative Management Increase iron rich foods & assess milk weaning Administer iron (elemental iron) Hgb should increase within 2 weeks Administer iron on empty stomach in an acidic environment along with vitamin C Clean teeth after administration (stains—and yuck taste!) Black stools Therapy continued for at least 3 months after Hgb has normalized Food insecurity—social service referral IMPORTANT NOTE: Iron pills are number one pediatric ingestion – KEEP OUT OF REACH Aplastic Anemia Defined Incidence A rare condition in which the bone marrow ceases production of cells resulting in peripheral pancytopenia 2 cases per million per year in Europe and United States As a reference point: leukemia has an incidence of 50 cases per million per year Etiology Congenital Acquired Chemicals, drugs, viruses, radiation, autoimmune Idiopathic (70%) Collaborative Management Diagnosed through bone marrow aspirate and biopsy Discontinue exposure to causative agent, if found! Supportive Care Treatment Transfusions Platelet and RBCs Infection control Bleeding prevention Bone marrow/stem cell transplant Medication regimen of immune suppressants Psychosocial support Referral to transplant center http://www.aamds.org/aplastic/ Sickle Cell Disease Defined A group of hemoglobinopathies where normal Hb is partially or totally replaced by abnormal HbS Several varieties, though HgbSS (SCA) most “classic” Prevalence Particularly common among (but not exclusive to) those whose ancestors came from sub-Saharan Africa; Spanish-speaking regions in the Western Hemisphere (South America, the Caribbean, and Central America); Saudi Arabia; India; and Mediterranean countries such as Turkey, Greece, and Italy Etiology Inherited, autosomal recessive Genetic Transmission Father: Mother: HbS Hb Hb Hb (sickle cell trait) (unaffected) Offspring: HbSHb HbHb HbSHb HbHb 50% chance of child inheriting the trait Father: Mother: HbS HbS Hb Hb (sickle cell trait) (sickle cell trait) Offspring: HbSHbS HbSHb HbHbS HbHb 25% unaffected, 50% carry the trait, 25% affected Pathophysiology HbS Increased RBC destruction plus decreased RBC lifespan= chronic anemia High reticulocyte counts As new RBCs being made Microcirculation obstructions Brain, Heart, Kidney, Eye, Spleen Clinical Manifestations Often detected on newborn screen, but patient not symptomatic for 4-6 months due to fetal hemoglobin Stressful event results in sickling crisis Deoxygenation, acidosis, dehydration, infection Vaso-occlusive crisis Pallor, jaundice, fatigue Delayed growth/puberty Avascular necrosis or hips and shoulders Renal dysfunction Retinopathy Priapism Cerebral infarct Cardiomyopathy Acute chest syndrome (respiratory failure) Acute sequestration (hypovolemic shock) Collaborative Management Folate Prophylactic penicillin therapy by 2 months Invasive pneumococcal disease (10-fold risk over tha of general population/15-35% fatality rate) Hydroxyurea (if experiencing frequent VOC) Vaccines: influenza, pneumococcal, Hib, meningococcal PRBC transfusions (routine) Pain management (action plan) Can be “cured” by bone marrow or stem cell transplant (BMT/SCT) VOC Management Treat cause (often infection) Hydration Oxygen if hypoxemic Possible PRBC transfusions Pain management—opioids, NSAIDS, heat Be self-aware of bias/presumptions about how pain presents Challenges with vascular access Previous experiences with poorly managed pain can affect future healthcare encounters Monitor for signs of life-threatening complications (such as?) Patient/Family Education Fluid intake essential Expect frequent urination Caution against extremes in temperature Discuss risk of and monitoring for infection (primary cause of death under 5 years) Adequate rest Pain management (action plan) Fever greater than 101 requires evaluation Mental health assessment related to chronic pain Concerns for substance use disorder Baseline hemoglobin (action plan) Importance of primary care, especially dental Genetic counseling Pain Action Plan Beta-Thalassemia Thalassemia major or Cooley’s anemia Defined Prevalence A group of inherited disorders characterized by a Hb beta-polypeptide chain abnormality RBC destruction leads to compensatory overproduction Traits for thalassemia are more common (but not exclusive) among those whose ancestors came from Mediterranean countries, like Greece and Turkey, and from Asia, Africa, and the Middle East. Etiology Autosomal recessive Carrier state = “thalassemia minor” Clinical Manifestations Severe anemia Think of this as “worse” anemia than SCA Fatigue Frontal bossing Maxillary prominence Wide-set eyes Flat nose Hepatosplenomegaly Jaundice, pallor Growth retardation Increase risk of fractures Therapeutic Management RBC transfusions – a lot! Chelation therapy (deferoxamine) Alloimmunization Splenectomy Can be “cured” by BMT/SCT Nursing Interventions Monitor Hgb level, iron level Chelation therapy education Psychosocial support Vigilant primary care due to immunocompromise (immunizations, prompt treatment of infections) Genetic counseling Vascular access management Coagulation Disorders Hemophilia Von Willebrand’s Disease Immune Thrombocytopenia Hemophilia Factor VIII deficiency (hemophilia A) Factor IX deficiency (hemophilia B) Etiology X-linked recessive Clinical Manifestations Presents with bleeding Epistaxis Bleeding gums Hematuria Frequent bruising Muscle/joint bleeding (hemearthrosis--See next photo) Circumcision bleeding (excessive) Diagnostic Evaluation Quantitative immunoelectrophorectic assay Factors VIII and IX assays Platelet count Fibrinogen level PT PTT Management Administer intravenous factor (prophylactically) Administer clot stabilizing medication Avoid rectal temperature measurement or suppositories (but constipation increases bleeding risk…) Apply gentle pressure to superficial wounds Assess LOC – know why! Think about other signs/symptoms of bleeding. Measure the affected joint/extremity, immobilization Active range of motion after acute phase as patient can limit for pain as opposed to passive range of motion RICE NSAIDS with caution—acetaminophen preferred Family Teaching Safe environment/injury prevention (think growth and development) Appropriate activities (sports, etc.) Soft toothbrush/electric shaver Signs/symptoms of bleeding Administration of factor (may need a permanent vascular access device) prophylactically or emergently Genetic counseling Von Willebrand’s Disease Defined An underproduction or dysfunction of vonWillebrand’s protein Prevalence/Etiology Most common inherited bleeding disorder Autosomal dominant inherited Manifestations Carrier protein for coagulation factor VIII Co-factor for the binding of platelets to damaged endothelial tissue Prolonged bleeding Variable severity – often undiagnosed until menorrhagia, childbirth or after a surgical procedure (prolonged bleeding) Management DDAVP Releases endogenous stores of vonWillebrand’s protein Prophylactic factor infusions (HumateP) Family education: communication, bleeding prevention Immune Thrombocytopenia (ITP) Defined An acquired hemorrhagic disorder characterized by thrombocytopenia (platelet count less than 150,000, a purpuric rash, normal bone marrow, & the absence of other identifiable caused of thrombocytopenia) Acute = less than 6 months Chronic = more than 6 months Prevalence/Etiology Most common acquired bleeding disorder in children Unknown, often follows a viral illness, considered an autoimmune process Manifestations Sudden onset of bruising & petechiae Mucous membrane bleeding Nursing Interventions Management Watchful waiting Hmmm..maybe we need to do something? IVIG Platelet count below 10,000 or 20,000 with spontaneous bleeding Steroids, anti-D antibody Splenectomy Platelet Transfusion Soft toothbrush/electric shaver Gentle pressure to superficial wounds Vigilant follow up Monitor labs Discuss home environment/safety Appropriate play activities Steroid use education Risk for infection & tapering Avoid medications that affect platelet function Blood Product Transfusions “Whole blood” rarely used Packed Red Blood Cells (PRBC)* Fresh Frozen Plasma (FFP)* Platelets* Cryoprecipitate Granulocytes, AT3, Albumin, factor VIII, thrombin, etc. etc. PRBC Transfusions Intravenous access Consent: purpose, risks/benefits, alternatives Type/screen vs. type/crossmatch Identification of recipient and donor 2 LICENSED providers (MD, RN, transfusionist) This is the NUMBER 1 ERROR SOURCE Assess patient for S/S of reaction (RN!) VS at beginning, 15 minutes in, and end of infusion— most reactions are at start Review Harding TABLE 30-33 ACUTE TRANSFUSION REACTIONS Transfusion Reactions Acute reactions Hemolytic Febrile Allergic Transfusion-associated circulatory overload (TACO) Transfusion-related acute lung injury (TRALI) Temperature and electrolyte disturbances Delayed reactions Hemolytic Alloimmunization/antibody formation Questions?