4 Bronchial Asthma
advertisement

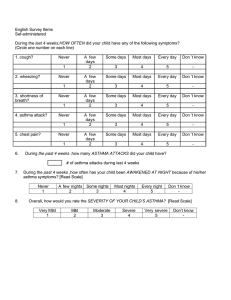
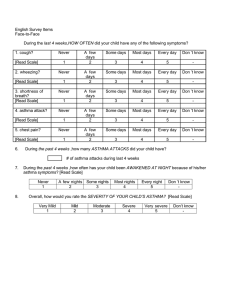
Asthma (bronchial asthma, BA) Asthma is a common chronic inflammatory disease of the airways characterized by: - variable and recurring symptoms - reversible airflow obstruction - bronchospasm. Hyper reactivity bronchus - a hypersensitivity of the bronchial tree, which manifests as bronchospasm, cough or difficulty in breathing in response to the stimulus. Morphological and biochemical basis of bronchial hyper reactivity is changing airway reactivity, resulting from chronic inflammation caused by prolonged exposure to environmental factors - specific (atopic) or nonspecific (viral and bacterial infections). Chronic inflammation at BA goes through a series of stages: 1. Acute obstruction - due to spasm of smooth muscles of bronchi. 2. Subacute obstruction – inflammation swelling of the mucous membranes of the respiratory tract. 3. Chronic obstruction - obstruction of terminal respiratory tract with viscous secret. 4. The progressive obstruction - an irreversible process, due to sclerotic changes in the bronchial wall. The first 3 types of obstruction can be return - bronchial lumen can return to normal on their own or under the influence of treatment. Asthma – is a disease that has allergic and inflammatory basis, as evidenced by the presence in the mucosa infiltrates, containing eosinophilic granulocytes (EG), mast cells and lymphocytes (even in mild flow). In the inflammatory process at BA participating 4 cell types: - Mast cells and inflammatory mediators released from them; - EG and mediators associated with them; - Lymphocytes; - Epithelial cells and related mediators. The pathogenesis of asthma: In the pathogenesis of asthma distinguish 3 stages: - First - immunological (under the influence of various allergens antibodies are produced or lymphocytes sensitization occurs); - The second - patochemical (at repeated actions of allergens mediators are released out of mast cells); - Third - pathophysiology (stage of clinical manifestations). Flow of an allergic reaction is immediate and delayed type. In the immediate type reactions leading role belongs to reagin that interact with antigen. This is particularly Ig E. It forms a complex with the antigen on the surface membrane of mast cells bronchial mucosa. This is followed by aggregation of membrane receptors and Ig E is a trigger of activation of mast cells. At patochemical stage due to allergen-antibody reactions in membranes of mast cells are released active substances - histamine, serotonin, bradykinin, leukotrienes, acetylcholine, prostaglandin F2α addition, bradykinin causing inflammation. Aspirin asthma - the development of an asthma attack while taking aspirin resembles an allergic reaction, but they are based on immune mechanism. Aspirin inhibits cyclooxygenase, which leads to the metabolism of arachidonic acid. The synthesis of prostaglandin E is suppressed, which has a bronchodilator effect, which enhances the action of prostaglandin F2α, as well as histamine and leukotrienes. Recently proved that a necessary condition for the development of atopic asthma is heredity. In the human genome are genes that induce disease control response to treatment. Investigated the following factors responsible for the development of asthma: 1) Interleukin (IL) 3, 4, 5, 9, 13. 2) Β2 - adrenergic receptor. 3) Lymphocyte specific glucocorticoid receptor. 4) Tumor necrosis factor (TNF). 5) Highaffine receptor Ig E, beta subunit. 6) Receptor 1 TNF. 7) Gamma-interferon. 8) Mast cell chymase. 9) T - cell receptor. However, a great role is assign to environmental risk factors. Risk factors Predisposing factors ▪ Atopy ▪ Heredity Triggers The factors are the cause of asthma 1. Household Allergens ▪ house dust ▪ pets and cockroach ▪ fungi 2. External alehreny ▪ fungi ▪ pollen 3. Acetylsalicylic acid 4. Professional allergens. 1. Respiratory infections. 2. Children age. 3. Food. 4. Air pollutants. 5. Smoking ▪pasive ▪ active Among the factors provoking or can modify the flow of asthma, select: 1. Inductors (inhaled allergens, some food allergens, dermatophytes, chemicals, heredity). ■ immune response (T-helper type 2, Ig E, Ig G) ■ inflammation (T-helper type 2, EG, basophilic granulocytes) 2. Amplifiers (rhinoviruses, endotoxins) 3. The triggers (exercise, cold air, histamine, methacholine, passive smoking, sharp smells) ■ difficulty in breathing. Inductors - foreign proteins and chemical particles with a small molecular weight, which can trigger an immune response. Amplifiers - agents that are in the environment and are not able to provoke an immune response. The triggers (provocateurs) - agents that are able to enhance bronchial hyper reactivity in a short period without development of inflammation in the airway wall. Today proved that the development of asthma associated with hyper reactivity of large and shallow bronchi, caused by chronic inflammation, which is coordinated by T-helper 2-type. T helper type 2 secretes IL-4 and IL-5. IL-4 is the main cytokine that switch B lymphocytes Ig synthesis in E. IL-5 selectively activates EG, which are two of the main effector cells of allergic inflammation. In EG activation also participate IL-3, platelet-activating factor. Mediators of the early phase of allergic reactions 1 - type and their biological effects. Mediators The biological effect From granules of basophilic granulocytes Histamine Vasodilation, increase vascular penetration, itching, bronchospasm Proteases The destruction of the basement membrane of blood vessels, increasing histamine release and migration of EG Heparin Formation of complex with proteases, extracellular matrix destruction, block of the mediators releasing Eosinophilic chemotactic factor A Chemotaxis of EG Neutrophilic chemotactic factor Chemotaxis of neutrophilic granulocytes (NG) With the destruction of cell membrane phospholipids formed: Prostaglandin Increase vascular penetration, bronchospasm Leukotrienes Increase vascular penetration, bronchospasm, increasing migration of EG Bronchospasm, attraction EG. Platelet-activating factor Cells and cytokines that are involved in the late phase of allergic inflammation in the mucosa of the respiratory tract Cells Cytokines Macrophages IL-1, IL-6, IL-8, IL-10, granulocyte macrophage colonystimulating factor (GM-CSF) T-helper cells type 1 IL, gamma interferon, GM - CSF, TNF T-helper cells type 2 IL-4, IL-5, IL-6, IL-9, IL-10, IL-13, GM-CSF Mast cells IL-4, IL-5, IL-10, GM-CSF EG GM-CSF, IL-3, IL-4, IL-5, IL-8 Epithelial cells of the respiratory tract IL-1beta, IL-6, GM-CSF IL - produced by macrophage cells, previously was called "endogenous pyrogens". Under the influence of IL-1 induced significant biological effects. IL-1 promotes early production of T-helper IL-2. IL-2 - a protein produced by T helper type 1 and influences the proliferation of lymphocytes. IL-4 - produced by T helper type 2. It’s main role - enhancement of humoral immune response and switching products Ig M to produce IgG, Ig E. IL-5 - eosinophilic factor - promotes activation of EG in the hearth of eosinophilic inflammation. IL-10 - interleukin suppressor produced by T-helper type 2. It inhibits the function of T-helper type 1. Leukotrienes are formed from arachidonic acid, which is part of the membranes. The synthesis of leukotrienes activates phospholipase A2, which selectively releases arachidonic acid from cell membranes. In the lungs contain several types of cells that have enzymatic systems necessary for the synthesis of cysteine leukotrienes, mast cells, EG, alveolar macrophages. Masts cells and EG are the main effector cells in the pathogenesis of asthma. Cysteine leukotrienes lead to airway obstruction at humans by stimulating specific receptors, called receptor cysteine leukotriene type 1 (TsysLT1receptors). Today managed to selectively block of only one ferment - 5 lipoxygenase that participates in the synthesis of leukotrienes. The inflammatory process has four mechanisms of bronchial obstruction: - Acute bronchospasm - Subacute edema - Chronic formation of mucous jams - Irreversible change bronchus Classification of asthma. According to the first division distinguished: ● Exogenous asthma (exogenous and known etiological factor) ● Endogenous asthma (endogenous factor not specified) ● mixed asthma. 45 J Asthma J 45.0 Predominantly allergic asthma ▪ Allergic bronchitis ▪ Allergic rhinitis with asthma ▪ Atopic asthma ▪ Exogenous allergic asthma ▪ Hay fever with asthma J 45.1 No allergic asthma ▪ Idiosyncratic asthma ▪ Exogenous No allergic asthma J 45.8 Mixed asthma J 45.9 unspecified asthma ▪ Asthmatic bronchitis ▪ Late asthma J 46. asthmatic status ▪ Acute severe asthma. Another classification is presented in the "Report on the international agreement on the diagnosis and treatment of asthma" (1992), based on a comprehensive assessment of symptoms and PEF changes. According to this classification, there are 4 stages of asthma. 1. Intermittent asthma ▪ Short symptoms occur at least 1 - 2 times a week ▪ Night asthma symptoms occurring at least 1 - 2 times a month ▪ Between exacerbations no symptoms ▪ PEF or FEV1 predictive value deviation of 20% 2. Easy persistent asthma ▪ Short symptoms occur more than 1 - 2 times a week ▪ Aggravation can cause sleep disturbances ▪ Night asthma symptoms occurring more than 2 times per month ▪ Chronic symptoms, that required agonist use almost every day ▪ PEF or FEV1 60- 80% predictive value deviation of 20% - 30% 3. Moderate persistent asthma ▪ Short symptoms occur more than 1 - 2 times a week ▪ Aggravation can cause sleep disturbances ▪ Night asthma symptoms occurring more than 2 times per month ▪ Chronic symptoms that require the use of agonists almost every day ▪ PEF or FEV1 60- 80% predictive value deviation of 20% - 30% 4. Severe persistent asthma ▪ Frequent exacerbations ▪ Permanent symptoms ▪ Frequent nocturnal asthma symptoms ▪ PEF or FEV1 60% predictive value ▪ Deviation of 20%. Degree of aggravation of asthma Symptoms Light severity The average severity Severe The activity of movements Patients walk, may lie Patients talk, try to sit Still, it is difficult to move Speech Sentence Phrases Words Consciousness Excitation is possible Typically, excitation Typically, excitation Accelerated Accelerated Accelerated more than 30 in 1 min Typically, there is no Typically, there is Almost always there is Paradoxical thoracoabdominal breathing Moderate, usually in the end of exhale Noisily Noisily Wheezing is absent Less than 100 in 1 min. 100 - 120 in 1 min. More than 120 in 1 min Bradycardia Breathing. Participation of supporting muscles in breathing Wheezing No wheezing Wheezing Heart rate The threat of respiratory failure Confusion The presence of a paradoxical pulse PEF after administration of bronchodilators Missing Missing Missing More than 80% of the appropriate values 60 - 80% of the appropriate values Less than 60% of the appropriate values ≥ 60 mm. Hg.c. ≥ 60 mm. Hg.c. РаО2, mm. Hg.c. Norm Ра СО2, mm. Hg.c. ≤ 45 mm. Hg.c. ≤ 45 mm. Hg.c. ≥ 45 mm. Hg.c. ≥ 90% 91 - 95 % ≤ 90% SаО2, % Missing in muscle fatigue Clinical features and investigation. Investigation of asthma is based on the data: 1) allergic reactions in history (food, medicines, chemicals, plants) 2) heredity 3) daily or seasonal variability of symptoms 4) expiratory dyspnea 5) feeling chest compression 6) respiratory discomfort 7) cough that occurs mostly at night or in the morning. The frequency of certain symptoms of asthma and its severity depends on the severity of the disease. First of all asthma patients concerned of tachypnea, cough, chest compression and sometimes wheezing, audible at a distance. During the attack the patient prefers sitting position, leaning forward, participates in respiration auxiliary muscles. Auscultation of the chest: prolonged expiratory, whistling dry rales throughout. In period without seizures abnormal respiratory noise does not auscultate. Investigation algorithm History - asthma symptoms + inducers, trigger, heredity, atopy Physical data - dry expiratory wheezing, prolonged expiratory, expiratory dyspnea The diagnosis of asthma is assumed FEV1, PEF and daily variability of these indicators The diagnosis of asthma is set (specification etiology: allergological tests, determination of Ig E in serum and others). FEV1, PEF below normal Bronchodilators test FEV1, PEF growth ≥ 15% Diagnosis was set (clarify etiology) FEV1, PEF growth≤ 15% Treatment with corticosteroids The diagnosis is unknown FEV1, PEF normal Bronchoconstrictive test Positive Diagnosis was set (clarify etiology) Negative The diagnosis was not confirmed Observation (possible morphological examination of bronchial mucosa and their contents) FEV1, PEF growth ≥ 15% Diagnosis was set FEV1, PEF growth ≤ 15% The diagnosis was not confirmed (continue investigation of bronchial obstruction syndrome). Laboratory and instrumental methods. Complete blood count in uncomplicated asthma is usually normal. Sometimes is observed slight eosinophilia. ESR - normal and its increasing evidence of infection accession. If you suspect a secondary infection requires a differential count. Investigation of sputum. Macroscopically sputum is viscous and whitish. At exogenous asthma in sputum cells determined by ciliated epithelium, NG, EG in large quantities and extended form crystals (Leiden’s), released from EG. At endogenous asthma EG number is much smaller than at exogenous, prevail NG. On chest X-ray in period without seizures in uncomplicated asthma any changes are absent. During the attack appears increased transparency of the lung fields, flattening of dome diaphragm. Due to blockage of bronchial mucous congestion may occur segmental and subsegmental atelectasis. The overall level of IgE in serum at exogenous asthma usually elevated. However, the definition of it at patients is usually not information and is not used. More often conduct skin tests or specific Ig E level determined. Additional methods determining lung function determine the allergic status and identify specific inducers and trigger of asthma. Important role in the diagnosis allocated to the respiratory function. Determination of bronchial obstruction and its reversibility and variability count is extremely important in the diagnosis of asthma. To assess the severity of airflow obstruction are used 2 methods: ● determination of forced expiratory volume in 1 second (FEV1). FEV1 - the maximum volume of air exhaled in the first second after a full inhale. ● determination of peak expiratory flow (PEF) - maximum flow rate, which is formed by the forced expiratory time. These findings correlated with FEV1. PEF is measured in liters in 1 sec. or 1 min. (l / s or l / min) and it is a parameter for assessing airway obstruction. To control the treatment of asthma is used measured daily variability index. The value of PEF and its variability characterizes everyday severity and stability of the disease. As normal PEF values most often used medium, the best indicator that was in remission or stable during the best of the patient. An important diagnostic and prognostic criterion is the determination of reversibility of bronchial obstruction (BO). The test is performed using PEF-index and β2 - agonist shortacting. The sequence of the test: ► determine the initial PEF (PEF 1) ► hold inhalation β2 - Short agonist action ► 15 minutes PEF measured (PEF 2) ► to calculate percentage of BO parameter that will display the reversibility of bronchial obstruction: BO = (PEF 2 - PEF 1) : PEF 1* 100 % Generally considered the following indicators of reversibility of bronchial obstruction: ► significant (25%) ► moderate (15 - 24%) ► small (10 - 14%) ► negative reaction (10%). To determine the oscillation of PEF, measurements should be taken weekly PEF, calculate their smallest and largest value from the formula: PEF max.- PEF min. -------------------------- * PEF max. 100% Daily performance PEF more than 20% is diagnostic feature of asthma, and the deviation is directly proportional to the severity of the disease. In some cases, the diagnosis of asthma can be confirmed by bronchoconstrictive (provocative) test. This test is for patients with normal (or with close to normal) indices of respiratory function in questionable physical and anamnesis. As bronchoconstrictive agents are used pharmacologic agents (acetylcholine, methacholine, and histamine), cold air, exercises, allergens. Most used in clinical practice tests with inhale pharmacological agents. They are standardized and harmless. Evaluating the data sample, determine the minimum threshold concentration (dose) of inhaled substance that is capable of reducing FEV1 by 20% compared with the original value. Normal value is 8 mg / ml. A lower value indicates the presence of asthma. All patients should assess allergic status. The most commonly used for this prick - test. Skin tests with allergens - the main method of diagnosis in patients with allergic asthma. Also important to determine specific Ig E in serum. However, this test does not replace the skin test. The diagnosis of asthma can be confirmed morphologically - the presence of typical asthmatic inflammation in the biopsy of mucosa of the bronchial tree. According to the Guidelines for the treatment of asthma of National Institute of Heart, Lung and Blood (USA) there are a number of diseases that should be excluded in the diagnosis of asthma: ■ chronic obstructive pulmonary disease ■ congestive heart failure ■ pulmonary embolism ■ diseases of the larynx ■ mechanical airway obstruction (including tumors) ■ eosinophilic pneumonia ■ cough caused by taking certain drugs (ACE - inhibitors) ■ diseases of vocal cords. Differential diagnosis of asthma with chronic obstructive pulmonary disease (COPD) Feature Allergy COPD Asthma There is no Typical Cough Permanent, severe intensity Stuffiness Permanent, without sharp fluctuations Expiratory dyspnea attacks Less than 10% More than 15% of Reversibility is not typical, progressive deterioration Typical reversible, progressive deterioration of missing Not typical Typical Daily measurement of FEV1 Bronchial obstruction Eosinophilia in blood and sputum Seizures Asthma attack Inspiratory or mixed Auscultation of the lungs No changes -Stenosis of the larynx -Hysteria Breathing weakened or absence of respiratory sounds in a particular part Spontaneous pneumothorax Expiratory Auscultation of the lungs Dry rales Moist rales No changes - PE (first 2 days) - Cardiac asthma (interstitial edema) Unilateral - PE Bilateral - Cardiac asthma -Stenosis of the larynx -Hysteria Dry rales - Foreign body of bronchi - Endobronchial tumors or bronchial compression outside - parasitosis - Mushroom or organophosphorus poisoning - Overdose of βblockers. - ARD - Asthma Status asthmaticus (SA) Status asthmaticus - a syndrome of acute respiratory failure, which occurs in patients with asthma due to bronchial obstruction resistant to sympathomimetic and aminophylline. Resistant bronchi-obstructive syndrome caused by delay accumulation of viscous mucus in the bronchi against the background of diffuse edema of the bronchial mucosa and / or total bronchospasm. There are three stages of asthma status: 1) Phase of compensation relative ventilation disorders. 2) The stage of decompensation ("silent lung"). 3) Hypercapnia coma. The main division in the stage picture of SA is auscultation of the lungs. In the first stage, breathing is hard, listened throughout lung, wheezes on auscultation of the lungs and on distance. At the second stage - breathing becomes impaired; there are areas of "silent lung", i.e. areas of the lung parenchyma, which completely eliminated due to obstruction of the ventilation mucus corresponding bronchi. The third stage - hypercapnia coma, requiring reanimation measures. Ventilation is only in the upper parts of lung, only there you can hear breathing. Dry rales in the lungs and they reduced, up to a total absence. Treatment of asthma. The highlights in the treatment of asthma: • Basic therapy aimed at maintaining asthma control and quality of life of patients; • Treatment is aimed at removing the direct attack asthma; • Treatment of status asthmaticus. The main objective of treatment is to achieve sustainable and possible long-term remission, to control symptoms of asthma that provides relatively normal life of the patient. Treatment of patients with asthma depends on: 1) The forms of the disease 2) The severity of the disease. Principles of treatment of patients with allergic asthma I. Etiological treatment: 1. Elimination of allergen if possible: - Appropriate employment; - Elimination diet; - Setting up life with the exception of the causal allergen; - "Air purifiers"; - Change of residence, etc. city. 2. Specific immunotherapy (SIT) with cause and significant allergen (made only in remission). II. Pathogenic treatment: 1. Anti-inflammatory therapy and nonspecific hyposensitization: a) antihistamines 1st, 2nd and 3rd generations (shown in combination with other asthma allergic diseases, their use is limited); b) stabilizing the membranes of mast cells (Cromoglycate sodium, zaditen, ketotifen); c) nedocromil sodium (bronchial hyperresponsiveness decreases). g) leukotriene modifiers (zafirlukast, montelukast); e) steroids (in severe disease parenteral in acute with subsequent transition to inhaled form, selecting a maintenance dose if necessary). g) anti Ig E preparations (Omalizumab-ksolar). 2. Bronchodilator therapy: a) sympathomimetic: - Selective 2 - short-acting agonists (salbutamol, berotek); - Selective 2 - long-acting agonists (salmeterol, formoterol); b) methylxanthines (inhibitors of phosphodiesterase): - Short-acting (aminophylline, theophylline) is used to relieve asthma attacks and symptoms of respiratory discomfort; - Prolonged theophylline (teopek, teotard) - used for long-term basic treatment to prevent asthma attacks; c) dose inhaled anticholinergics (ipratropium and tiotropium -ipravent, spiriva); d) combined inhaled bronchodilators dosage (Berodual - berotek + ipratropium bromide). 3. Improving drainage of bronchi: a) mucolytic (not desirable to use decoctions of herbs and herbal medications that increase bronchorea); b) inhalation (alkaline, mineral waters, etc.); c) vibratory massage the chest; d) physiotherapy (electrophoresis, laser therapy, electrical stimulation of the diaphragm, etc.); e) artificial rock salt spray (haloaerozolterapiya); g) exercises. 4. Plasmapheresis, hemosorbtion (in severe autoimmune variant of the disease). 5. Immunomodulatory therapy (if indicated after immunological examination, using relatively rare). 6. Fasting-diet therapy - when combined with food allergies asthma, chronic digestive diseases, hypertension, coronary heart disease, etc.). 7. Other non-drug methods increase nonspecific resistance of the organism: a) speleotherapy; b) artificial rock salt spra; c) spa treatment. Principles of treatment of patients with non-allergic asthma I. Etiological treatment 1. Eliminate chronic or acute inflammation in bronchi pulmonary system, upper respiratory tract, oral cavity, gastrointestinal tract etc. a) antibiotics (including sensitivity flora and hypersensitive); b) antiviral medications (if indicated); c) bronchi sanation (if purulent sputum); d) phytoncides (chlorofillipt and other herbs – during convalescence, often inhalation). 2. Correction of hormonal imbalance in women (if indicated). 3. Psychotherapy, acupuncture, sedatives (shown by to orders). II. Pathogenic treatment 1. Anti-inflammatory therapy (taking into account the severity of asthma): a) nedocromil sodium; b) fenspirid (erespal); c) leukotriene modifiers (montelukast, zafirlukast); d) stabilizing mast cell membranes (asthma in Physical efforts); e) glucocorticoids (mainly topical, an exacerbation - system). 2. Bronchodilator therapy (as in the treatment of allergic asthma). 3. Improving drainage of bronchi: a) mucolytic (not desirable to use decoctions of herbs and herbal medications that increase bronchorea); b) inhalation (alkaline, mineral waters, etc.); c) vibratory massage the chest; d) physiotherapy (electrophoresis, laser therapy, electrical stimulation of the diaphragm, etc.); e) artificial rock salt spray (haloaerozolterapiya); g) exercises. 4. Immunomodulatory therapy (if indicated after immunological examination, using relatively rare). 5. Increase of nonspecific resistance of the body (as in the treatment of allergic asthma). Basic treatment of asthma. Step 1. Intermittent asthma. Treatment is needed at the exacerbations.. Anti-inflammatory therapy (an exacerbation): - Generation antihistamines 2-3; - Kromons. Bronchodilators: - β2-agonists, anticholinergics and short-acting theophylline if necessary. Step 2. Easy persistent asthma. Basic anti-inflammatory therapy in low doses continuously combined with bronchodilators as needed. Anti-inflammatory therapy (continuous): - Kromons; - Nedocromil sodium; - Leukotrienes modifiers; - Topical corticosteroids in low doses (100-500mkh / day). Bronchodilators: - β2-agonists, inhaled anticholinergics and short-acting theophylline if necessary. Step 3. Persistent asthma moderate course. Anti-inflammatory therapy always possible in combination with bronchodilators: - Topical glucocorticoids in medium and high doses (> 400-500mkh / day); - A combination of topical glucocorticoids with β2-agonists long-acting (Seretide, asmoneks); - A combination of topical corticosteroids in low doses of leukotriene modifiers and β2-agonists prolonged action. Additionally, short-acting bronchodilators if necessary. Step 4. Severe persistent asthma. Basic anti-inflammatory and bronchodilator therapy regularly (a combination of two or more drugs): - A combination of topical corticosteroids in medium and high doses of β2agonists prolonged; - A combination of topical corticosteroids and long-acting β2-agonists, leukotriene modifiers and / or prolonged theophylline. If necessary, additional corticosteroids per os. When failure - sparring therapy (a combination of corticosteroids and immunosuppressive drugs - metotryksad, cyclosporine A). Removal asthma attack 1. Treatment in mild asthma attack. a) Ensure fresh air to calm the patient. You may have certain breathing exercises. b) Dosage β2-agonists (salbutamol, berotek) - 1-2 inspiration is stated. 2. Treatment for moderate asthma attack. a) Fresh air b) Dosage β2-agonists (2 inspirations are stated). c) If no effect, either immediately (depending on the basic treatment) is introduced i/v aminophylline 2.4% - 5,0-10,0ml. 3. The therapeutic approach in patients with severe asthma attack. 1) Provide fresh air. Oxygen therapy. 2) Theophylline 2,4% - 10 ml i/v on solution. 3) If no effect - glucocorticoids i/v (30-60mg prednisolone, dexamethasone 4-8 mg saline). In patients with asthma dose of glucocorticoid hormone can be increased. With little effect, putting of theophylline and prednisone can be repeated. The total dose theophylline no more than 15 ml of 2.4% solution. 4) In the absence of effect should consider developing asthmatic status and conduct appropriate treatment. Treatment of asthmatic status Treatment depends on the stage of the SA. At the first stage of the SA prescribed: 1) Glucocorticoids every 3-4 hours (60-90 mg prednisone, dexamethasone 8 mg) to improve the situation. In the second stage glucocorticoids are administered every 1.5 hours or without interruption. 2) Oxygen therapy, preferably moist oxygen, better oxygen or oxygen-air mixture gels. 3) 2.4% aminophylline first i/v bolus, followed i /v drip evenly throughout the day (up to 60-80ml per day). 4) Considering that most of the developing asthmatic status against the background of sympathomimetic overdose recommended complete cancellation of any sympathomimetic. At asthmatic status, emerged sharply as an allergic reaction, exposed to the allergen, there is possible use of sympathomimetic i/m or i/v (alupent, brykanil) with regard to the cardiovascular system. 5) Sodium bicarbonate 4% - 200.0 i/v drip (to eliminate acidosis and restore receptor sensitivity). Requires control of acid-base balance of the blood (maintain blood pH at 7.25). 6) Mucolytic: - Lasolvan i/v or i/m (2-3 amp. 2-3 times a day); - Sodium iodide 10% - 10.0 i/v drip to 30 ml per day, - Potassium iodide 3% per os - 1 tbsp. every 2 hours (in the absence of contraindications). - Steam-oxygen inhalation; - Vibrating chest massage. 7) The prescription of drugs that improve blood rheology: - Heparin 5000 units. i/v drip in saline solution (up to 20,000 units per day). 8) It is recommended hydration (hydrogenation) of the body to reduce haemoconcentration and improve expectoration. During the first day is recommended to give 3-3.5 liters of fluid i/v drip without giving diuretics under the control of the cardiovascular system and diuresis. Required diuresis 80 ml urine per hour without giving diuretics. By the second day administered to 2-2.5 liters of fluid without giving diuretics. 9) Antibiotic therapy is prescribed only when it is proven bacterial exacerbation (pneumonia). It is advisable to assign non-penicillin antibacterial agents (fluoroquinolones). In the second stage of asthma status conservative therapy may last 2-2.5 hours, if there is no effect - ventilation and bronchial lavage. In the third stage of asthma status mechanical ventilation and bronchial lavage carried out immediately and then attach conservative therapy. Criteria for improvement - discharge of phlegm, recovery ventilation (breathing) in "silent zones". If there are no effect and there is growth of phenomena of hypercapnia places - artificial ventilation, intubation and bronchial lavage (bronchi washing through the bronchoscope 1.4% solution of sodium content with suction bronchi).