Mental Health Nursing II NURS 2310 Unit 16 Psychiatric/Mental Health
advertisement

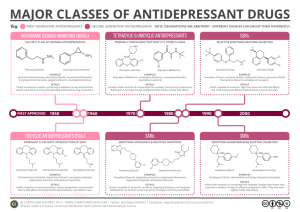
Mental Health Nursing II NURS 2310 Unit 16 Psychiatric/Mental Health Treatments and Interventions Key Terms Psychotropic medication = affects psychic function, behavior, or experience; effects the neuronal synapse, producing changes in neurotransmitter release and the receptors they bind to Neurotransmitter = a chemical that is stored in the presynaptic neuron and is released by an electrical impulse through the neuron Receptor = molecules situated on the cell membrane that are binding sites for neurotransmitters Antianxiety Agents Used for preoperative sedation and to treat anxiety disorders, acute alcohol withdrawal, muscle spasms, and convulsive disorders Depresses the CNS; all levels can be affected Classes of anxiolytics include antihistamines (hydroxyzine/Vistaril), benzodiazepines (alprazolam/Xanax, lorazepam/Ativan), and miscellaneous agents (buspirone/Buspar) Side effects include drowsiness, confusion, and lethargy; paradoxical excitement or blood dyscrasias may also occur with use Effects are increased when used with alcohol, narcotics, barbiturates, antipsychotics, and antidepressants; effects are decreased when used with nicotine and/or caffeine Physically and psychologically addicting Abrupt withdrawal may be life-threatening; withdrawal symptoms include depression, insomnia, increased anxiety, tremors, vomiting, sweating, convulsions, and delirium Exception is buspirone (Buspar), which does not depress the CNS and has no addiction potential; has a delayed onset of 10 days – 2 weeks, so cannot be used as a PRN Antidepressants Used to treat depressive disorders, alcoholism, schizophrenia, intellectual developmental disorder Elevates mood and alleviates other symptoms associated with depression May decrease the seizure threshold May increase suicide potential (watch for sudden lifts in mood) Side effects common to all antidepressants include dry mouth, sedation, and nausea; discontinuation syndrome may occur as a result of abrupt withdrawal (taper gradually) Tricyclics Blocks the reuptake of norepinephrine, serotonin, and/or dopamine Examples: amitriptyline (Elavil), clomipramine (Anafranil), imipramine (Tofranil), nortriptyline (Pamelor) Side effects specific to tricyclics include blurred vision, constipation, urinary retention, orthostatic hypotension, weight gain, tachycardia, and photosensitivity Effects are increased when taken with buproprion, Haldol, SSRIs, and Depakote Selective Serotonin Reuptake Inhibitors (SSRIs) Blocks the reuptake of norepinephrine, serotonin, and/or dopamine Examples: fluoxetine (Prozac), sertraline (Zoloft), citalopram (Celexa), paroxetine (Paxil), escitalopram (Lexapro) Side effects specific to SSRIs include insomnia, agitation, headache, and sexual dysfunction Interacts with alcohol (mental/motor skill impairment); use with buspirone, tryptophan, lithium, and amphetamines may result in serotonin syndrome (mental changes) Miscellaneous Agents Examples: bupropion (Zyban, Wellbutrin), mirtazapine (Remeron), trazodone (Desyrel), venlafaxine (Effexor), duloxetine (Cymbalta) Monoamine Oxidase Inhibitors (MAOIs) Inhibits the release of monoamine oxidase enzymes that inactivate norepinephrine, serotonin, and/or dopamine in the body Examples: isocarboxazid (Marplan), phenelzine (Nardil), tranylcypromine (Parnate) Use with narcotic analgesics may cause hyperor hypotension, convulsions, coma or death Concurrent use of antidepressants, amphetamines, vasoconstrictors, or foods containing tyramine may cause hypertensive crisis (marked increase in blood pressure, severe occipital headache, palpitations, coma) – Foods containing tyramine include aged cheese, smoked/processed meat, chicken, raisins, red wine, caviar, pickled herring, corned beef, beef liver, soy sauce, brewer’s yeast, and MSG Should not be used within 2 weeks of an adverse agent, or within 5 weeks of Prozac Mood-Stabilizing Agents Used to treat bipolar disorder Enhances reuptake of norepinephrine and serotonin, thereby decreasing their levels in the body (results in decreased hyperactivity) Classes of mood-stabilizing agents include antimanics (lithium carbonate/Eskalith), anticonvulsants (clonazepam/Klonopin, valproic acid/Depakote), calcium channel blockers (verapamil/Isoptin), and antipsychotics (olanzapine/Zyprexa, aripiprazole/Abilify, risperidone/Risperdal) Lithium Carbonate Very narrow margin between therapeutic and toxic levels Lithium toxicity can be life-threatening (symptoms include blurred vision, ataxia, persistent nausea/vomiting/diarrhea, psychomotor retardation, mental confusion, seizures, coma, and cardiovascular collapse) Fluoxetine, loop diuretics, and decreased salt intake can increase risk of lithium toxicity; carbamazepine, Haldol, and methyldopa can increase risk of neurotoxicity; verapamil may decrease serum lithium level or result in lithium toxicity Antipsychotic Agents Also called neuroleptics Used to treat psychosis and/or increased psychomotor activity Blocks postsynaptic dopamine receptors in the brain Reduces the seizure threshold Routine ECG should be completed prior to initiation due to potential for heart damage (prolonged QT interval) Categorized as typical and atypical Examples of typical antipsychotics: haloperidol/Haldol, chlorpromazine/Thorazine, fluphenazine/Prolixin, and thioridazine/Mellaril Examples of atypical antipsychotics: risperidone/Risperdal, clozapine/Clozaril, olanzapine/Zyprexa, quetiapine/Seroquel, ziprasidone/Geodon, and aripiprazole/Abilify Side effects common to all antipsychotic agents include extrapyramidal symptoms (EPS), dry mouth, blurred vision, constipation, nausea/GI upset, skin rash, sedation, orthostatic hypotension, photosensitivity, amenorrhea, and weight gain Extrapyramidal Symptoms (EPS) Pseudoparkinsonism = tremor, shuffling gait, drooling, rigidity Akinesia = muscle weakness Akathisia = continuous restlessness and fidgeting Tardive dyskinesia = bizarre facial and tongue movements, stiff neck, and difficulty swallowing; all long-term clients are at risk, and the symptoms are potentially irreversible even if the medication is discontinued Dystonia = involuntary muscular movements or spasms of the face, arms, legs, and neck Oculogyric crisis = uncontrolled rolling back of the eyes; may appear to be seizure activity *These are medical emergencies that are treated with IV or IM benztropine (Cogentin) Neuroleptic malignant syndrome = hyperpyrexia (up to 107 degrees), severe muscle rigidity, tachycardia, stupor/coma; potentially fatal; treated with Parlodel and immediate discontinuation of antipsychotic agent Use of atypical antipsychotics may cause hyperglycemia/diabetes; should assess BMI, blood glucose, and weight regularly Agranulocytosis, a potentially fatal blood disorder in which WBCs drop to extremely low levels) may occur with use of Clozaril; baseline WBC count must be completed before initiation of medication – WBC count done weekly for first 6 months, biweekly for next 6 months, and monthly thereafter – Supply only given until next test is due Sedative-Hypnotics Used to treat anxiety and insomnia Causes generalized CNS depression Potential for psychological and/or physical dependence, and may produce tolerance with chronic use Classes of sedative-hypnotics include barbiturates (secobarbital/Seconal), benzodiazepines (temazepam/Restoril), and miscellaneous agents (zolpidem/Ambien, zaleplon/Sonata, eczopiclone/Lunesta) Additive effect (CNS depression) when used with antihistamines, antidepressants, alcohol, or other CNS depressants Should not be used with MAOIs Use of barbiturates may decrease the effectiveness of drugs metabolized by the liver Attention-Deficit/Hyperactivity Disorder (ADHD) Agents Used to treat ADHD in children and adults Increases the levels of neurotransmitters in the body and stimulates the CNS Classes of ADHD agents include amphetamines (dextroamphetamine sulfate/Dexedrine), amphetamine mixtures (dextroamphetamine/Adderall), and miscellaneous agents (methylphenidate/Ritalin and Concerta, atomoxetine/Strattera, buproprion/Wellbutrin) Tolerance develops rapidly; should not be withdrawn abruptly Should not be used within 14 days of an MAOI Side effects common to all ADHD agents include overstimulation, restlessness, insomnia, palpitations, tachycardia, anorexia/weight loss, nausea/vomiting, constipation, and new/worsened psychiatric symptoms Buproprion is contraindicated in clients with seizure disorder Atomoxetine may cause severe liver damage Electroconvulsive Therapy Involves the induction of a grand mal seizure through the application of electrical current to the brain Appropriate for the following conditions: – Acute suicidality – Severe depression – Psychotic symptoms – Psychomotor retardation – Neurovegetative changes (disturbances in sleep, appetite, and energy) Only considered as a final treatment measure Side effects and risks: – Temporary memory loss that lasts approximately 30 minutes – Confusion – Mortality 2 : 100,000 Results from heart attack or stroke in already compromised clients – Permanent memory loss specific to the time surrounding treatment – Brain damage due to oxygenation issues Psychotherapy Takes place on a one-to-one basis between a client and a therapist (APRN, psychiatric social worker, psychiatrist, psychologist, or LMHP) Various modalities are used based on condition being treated – Psychoanalysis Client gains insight/understanding about current relationships/behavior patterns by confronting unconscious conflicts that surface in the transference relationship w/therapist Includes methods such as free association, dream analysis, hypnosis, and catharsis – Assertiveness training – Interpersonal psychotherapy Time-limited therapy developed for the treatment of major depression – Reality therapy Promotes the conviction that although an individual is a product of the past, he/she does not need to continue as its victim Based on power (self-empowering), belonging, freedom, fun, and survival Hope is instilled when therapy does not dwell on past failures, and client is able to look forward toward a change in behavior – Relaxation therapy Deep-breathing exercises Progressive relaxation Meditation Mental imagery Biofeedback – Cognitive therapy Individual is taught to control thought distortions that are considered to be a factor in the development and maintenance of mood disorders Goal is to provide symptom relief and identify dysfunctional patterns of thinking Behavior Modification Uses operant conditioning to replace undesirable behaviors with more desirable ones through positive or negative reinforcement Positive reinforcement – rewarding good behavior Negative reinforcement – punishing bad behavior Extinction – removing the response (i.e. “time-out”) Alternative/Complementary Medicine Alternative medicine = interventions that differ from the traditional or conventional biomedical treatment of disease; refers to an intervention that is used instead of conventional treatment Acupuncture Blue light/artificial light treatment Lifestyle/dietary changes Herbal medicine Chiropractic medicine Relaxation techniques Chelation therapy Complementary medicine = therapeutic intervention that is different from, but used in conjunction with, traditional or conventional medical treatment. Herbal medicine Acupressure/Acupuncture Diet/Nutrition Chiropractic medicine Massage Therapeutic touch Yoga Pet therapy