Anatomy/Physiology Lecture Circulatory System ELEMENTS OF THE BLOOD:
advertisement

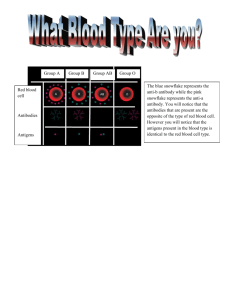
Anatomy/Physiology Lecture Circulatory System ELEMENTS OF THE BLOOD: I. Erythrocytes (RBC) a. Formation of blood = hemopoeisis; bone marrow i. Structure: biconcave disc (8 nm) ii. No nucleus or organelles iii. Semi-permeable membrane, cytoplasm, hemoglobin (carries O2) b. Function: combines with O2 and CO2 and transports them i. 4 heme groups (non-protein pigments) contain iron 1. Iron attaches to O2 ii. 4 globin groups (identical proteins) 1. Globin attach to CO2 c. General Information: i. There are approximately 700x more RBC than WBC 1. (4.8 million RBC/mm3 blood in females) 2. (5.4 million RBC/mm3 blood in males) ii. Life Span: ~120 days due to wear and tear experienced in the capillaries (very tight fit; nearly single file) 1. Broken down in liver, spleen and marrow 2. Heme groups are broken down in to iron and biliverden iii. Origin (production) 1. Erythropoeisis- formation of RBC 2. Occurs in red bone marrow 3. Rate of formation = rate of destruction a. If not, condition called anemia occurs (not enough RBC in the system) II. Leukocytes: White blood cells (WBC) a. Structure: i. Have a nuclei and lack hemoglobin 1. Either granular or a granular b. Function: i. Defense system; remove antigens (foreign particles) by either phagocytosis or initiating antibody (Ab) production ii. Immune response: eosinophils- pro-inflammatory releasing enzymes (histamine) causing inflammation: allergic reactions iii. Antibody response: block binding sites on cells, thus inhibiting antigen-cell interaction (no response) c. General Information: i. ~5,000 to 10,000 WBC/mm3 of blood ii. presence of more (10,000+) reflects the presence of infection iii. less than 5,000 cells = leukopenia; immunocompromization (can’t fight off infections) iv. Live only a few days (during infections live only hours) v. Produced in the white marrow of the bones III. Thrombocytes (platelets) a. General Information i. Disc-shaped; no nucleus; possess granules ii. Sole purpose: CLOT BLOOD iii. Live ~5-9 days iv. 250,000-400,000/mm3 blood v. Produced in the red bone marrow IV. Plasma- consists of “everything else” (water, hormones, proteins, nutrients, electrolytes, etc.) a. Primary Proteins: i. Albumen: 1. produced in liver 2. 55% of all plasma proteins 3. purpose: maintain water balance between blood and tissues ii. Globulins: 1. produced by B cells/plasma cells 2. 35% of plasma proteins 3. purpose: antibodies against foreign particles iii. Fibrinogen: 1. produced in the liver 2. 7% of plasma proteins 3. purpose: blood-clotting factors The Circulatory System: Part II Homeostasis: maintaining balance in the body; optimum levels the processes of the body that enable optimum conditions to be maintained for all cells, in spite of continual changes taking place both internally and externally. Whenever an imbalance occurs, regulatory systems become active to restore the optimum conditions, usually by a process known as negative feedback. When there is a break from the normal levels, the body is detects the variations and initiates changes which bring the level back to where it should be. MOMMY, WHY DON’T I BLEED TO DEATH? I. Mechanisms a. Vascular Spasms: contraction of smooth wall immediately following damage i. Primary response; reduces blood loss (between minutes and hours) until other mechanisms kick in ii. Induced by reflex mechanisms associated with pain receptors b. Platelet Plug Formation: swelling of platelets in damaged vessels i. Irregular shapes (more surface area; greater adherence to walls) ii. Become sticky and adhere to collagen fibers of wounded area; works well in small wounds iii. Tightens with coagulation (stretching of a scab) c. Coagulation: i. thickening and forming a gel (serum) that is different than plasma; forms the CLOT (reference page 314) d. Vascular Disorders: i. Plaque: cholesterol-containing mass found in the tunica media of the arteries ii. Thrombus: gel clot composed of insoluble protein fibers iii. Embolism: piece of debris (thrombi or plaque) breaks off and moves through vasculature until caught in small vessels 1. pulmonary embolism- occurs in the lungs iv. anti-coagulant: prevent clotting 1. heparin (mast cells/basophils) 2. inhibits prothrombin from maturing into thrombin THE FLAVORS OF OUR BLOOD II. Blood Typing: determined by surface molecules found on the RBC; contain genetically determined antigens called: *ethnicity plays a factor in blood types a. Agglutinogens: 14 types/systems but the top two are ABO and Rh i. ABO: based on agglutinogens called A and B ii. Blood plasma contains A or B (anti-A or anti-B) 1. A has A (plasma has anti-B antibodies) 2. B has B (plasma has anti-A antibodies) 3. AB has A and B (universal recipient; AB+ to be exact) a. (plasma has neither anti-A or B antibodies) 4. O has neither (universal donor; (O- to be exact) a. (plasma has both anti-A and B antibodies) b. Blood transfusions with different blood types is BAD i. Causes blood to clump ii. Cells swell and rupture (hemolysis = BAD) 1. 2. 3. 4. A gets A or O B gets B or O AB gets A, B or O O gets O only c. Rh Factor: named for Rhesus monkey (Macaca mulatto) i. Rh protein may be present or absent in individuals ii. Presence of Rh factor = Rh+ iii. Absence of Rh factor = Rhd. Understanding the Rh factor i. Mr. Hoefer is (A-); A blood type, lacking the Rh protein 1. Can donate to A+, A-, AB+, ABa. Application: from above, why is AB+ better than AB- when receiving blood? b. Why is O- better than O+ when donating blood? It is particularly important for expectant mothers to know their blood's Rh factor. Occasionally, a baby will inherit an Rh positive blood type from its father while the mother has an Rh negative blood type. The baby's life could be in great danger if the mother's Rh negative blood attacks the baby's Rh positive blood. If this happens, an exchange transfusion may save the baby's life. The baby's blood can be exchanged for new blood that matches the mother's.