Ask yourself all these questions sequentially
advertisement

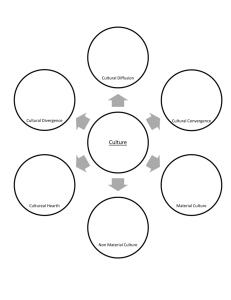
eEdE -29 Acquired Focal and Diffuse White Matter Pathologies -A Practical approach to Radiologist's Dilemma. Role of Multimodality Imaging, Histopathology and Laboratory correlation Prasad Hanagandi, Asim Bag, Lazaro do Amaral, Santanu Chakraborty Thanh Nguyen, Rafael Glikstein, John Woulfe, Gerard Jansen 1. 2. 3. The Ottawa Hospital, University of Ottawa, Canada University of Alabama at Birmingham, Birmingham, AL Medimagem &Hospital da Beneficência Portuguesa and Hospital São José- São Paulo ,Brazil No Disclosures Purpose: • In this education exhibit, we will describe • An image-based practical approach to acquired white matter abnormalities in adults. • A clinico-radiological algorithm demonstrating how to approach different white matter lesions in a day-to-day clinical practice. • Examples of how to use this algorithm in some common and rare diseases. Approach to the diagnosis: Ask yourself all these questions sequentially • • What is the clinical presentation? Careful evaluation of T2-weighted images is the key to the diagnosis: • – Is the lesion diffuse & confluent, nondiscrete or discrete? if discrete, how many are they? • – Where is/are the lesion(s)? • Periventricular/pericallosal • Subcortical – Is the adjacent cortex involved? • • Deep cerebral (in the centrum semiovale an in the corona radiata) • Brain stem (Is it central or periphery?) • • Cerebellum • Only callosal involvement?? • Multidistributional – Additional questions to ask: • Is it bilateral symmetrical? • Is temporal lobe white matter involved? – Is it periventricular? – Is it anterior temporal lobe? • Is there diffusion restriction? • • Is it holo-lesional? Is it at the periphery? Is there any enhancement? – – – Is it ring-like? Is it incomplete ring? Is it holo-lesional? No clue? – – How is the perfusion? How is the spectroscopy? Still no Clue?? – – What are the CSF findings? What is the serum chemistry Still no clue??? – Let’s consider for biopsy. Approach to the diagnosis: Ask yourself all these questions sequentially • • What is the clinical presentation? Careful evaluation of T2-weighted images is the key to the diagnosis: Look for – Periventricular/pericallosal Subcortical – • • • • • – Is there diffusion restriction? • Is it holo-lesional? • Is it at the periphery? Where is/are the lesion(s)? • • – • Is the adjacent cortex involved? Deep cerebral (in the centrum semiovale an in the corona radiata) Brain stem (Is it central or periphery?) Cerebellum Only callosal involvement?? Multidistributional Is the lesion diffuse or discrete? if discrete, how many are they? Additional questions to ask: • • Is it bilateral symmetrical? Is temporal lobe white matter involved? – – Is it periventricular? Is it anterior temporal lobe? • Is there any enhancement? – Is it ring-like? – Is it incomplete ring? – Is it holo-lesional? • No clue? – How is the perfusion? – How is the spectroscopy? • Still no Clue?? – What are the CSF findings? – What is the serum chemistry • Still no clue??? – Let’s consider for biopsy. Clinico radiological algorithm Small vessel disease Prior radiation treatment No neurologic symptoms HIV encephalopathy CADASIL Diffuse confluent white matter disease Infectious Asymmetric 1. HSV encephalitis 2. PML White matter disease of systemic causes 1. Gliomatosis Cerebri Tumor With neurologic symptoms CADASIL Symmetric White matter disease of systemic causes 2. Lymphomatosis cerebri Clinico-radiological algorithm PML Infection HSV encephalitis Asymmetric Metabolic 1. PRES Diffuse white matter diseases of systemic causes Autoimmune 1. Hashimoto encephalitis 1. Hyperammonemia Bilateral symmetrical Metabolic disturbances Toxic leukoencphalopathy PRES: Posterior reversible encephalopathy PML: Progressive multifocal encephalopathy 2. Hypoxic injury 3. Hypoglycemia 1. Methotrexate encephalopathy CADASIL: Cerebral autosomal dominant arteriopathy, subcortical infarct and leukoencephalopathy ARIA: amyloid related imaging abnormality ABRA: Amyloid beta related angiitis ADEM: Acute disseminated encphalomyelitis MELAS: Mitochondrial enchalopathy, lactic acidosis, stroke-like syndrome MS: Multiple sclerosis NMO: Neuromyelitis optica 1. PRES 2. Low grade glioma/cortical dysplasia 3. Vasculitis 4. ARIA, ABRA Subcortical 5. PML 6. ADEM 7. MELAS 8. Cerebral vein thrombosis 1. Small vessel disease 2. Infarct 3.PML Deep cerebral white matter 4. Vasculitis 5. Methotrexate encephalopathy 6. Angiocentric lymphoma Focal non-discrete Leukoencphalopathy Temporal lobe white matter CADASIL 1. Small vessel disease 2. MS Periventricular 3. CNS lymphoma Mesodiencephalic junction Behcet’s disease Brainstem 1. Small Vessel disease 2. Brainstem Glioma 3. Central variant of PRES 4. Osmotic demyelination 5. Rhombencephalitis 6. NMO 1. PML Cerebellum 2. Cerebrotendinous xanthomatosis 3. AV fistula Hypertensive emergency PRES Immunomodulator/cancer chemotherapy ±Focal mass effect History of seizure Low grade glioma No enhancement No diffusion restriction No mass effect ± ± H/O connective tissue disorder ±enhancement Cortical dysplasia Radiation band towards ventricle Vasculitis ±Hemorrhage ± diffusion restriction Vessel lumen irregularity Age >45-50 History of amyloid modifying drugs ARIA Micro- macrohemorrhage ABRA ± enhancement ± diffusion restriction H/O Immune deficiency Subcortical nonfluent white matter abnormalities NO mass effect PML Diffusion restriction at the advancing edge NO enhancement Prodromal history Lesions at other locations, particularly art basal ganglia ± Enhancement ±Diffusion restriction ADEM Multiple episodes of focal neurologic deficits Family history in the mother ‘s side MELAS Diffusion restriction Increased lactate peak FLAIR signal and T1 hyperintensity in the Adjacent cortical vein ± diffusion restriction Cortical vein thrombosis Asymptomatic Acute onset Holo-lesional Diffusion restriction Small vessel disease Infarct H/O Methotrexate therapy Subacute onset Methotrexate encephalopathy Holo-lesional diffusion restriction Focal non-discrete deep cerebral white matter lesion H/O immunodeficiency Sub acute onset PML Diffusion restriction at the margin H/O autoimmune disease (lupus, Sjogren etc. ) Headache Vasculitis Vessel wall irregularity on angiogram Subacute onset Diffusion restriction Nodular/Perivascular pattern of enhancement Angiocentric Lymphoma Granulomatous vasculitis Central pons NO symptoms Small vessel disease Central pons, sparing periphery H/O Hyponatremia or alcoholism ± Diffusion restriction Osmotic demylaination syndrome Involvement of the midbrain ± involvement of thalamus No overt mass effect Behcet disease No enhancement Non discrete brainstem white matter lesions Acute presentation Hypertensive urgency Immune modulator/chemotherapy Central variant of PRES Lupus Diffuse brainstem enlargement with increased FLAIR signal Subacute presentation Involvement of the floor of the 4th ventricle (Area prostrema) NMO 1. Brainstem glioma 2. Rhombencephalitis 1. Small vessel disease Subcortical 2. MS 3. Metastasis 4. Ganglioglioma/DNET 1. Small Vessel disease Deep cerebral 2. Lacunar infarct 3. MS 4. Border zone infarct 1. MS 2. Reversible splenial abnormality Callosal 3. Susac syndrome 4. Marchiafav-Bignami syndrome Discrete white matter lesion 1. Small vessel disease Periventricular/pericallosal 2. MS 3. Lacunar infarct Brain stem MS Cerebellum MS Examples Case: 1. 65 Year normotensive male presenting with headache and subacute onset (Over several days) visual field deficits. Image Analysis: Pattern: Patchy non-discrete Location: Subcortical Number: Multifocal Diffusion restriction: No Associated Clues: 1. Microhemorrhage 2. No appreciable enhancement Pertinent negative clues: NO sinus thrombosis NO arterial Ocllusion Low perfusion Case analysis: – Older patient, subacute etiology, no hypertensive urgency – Subcortical non-discrete lesions – Microhemorrhages – No diffusion restriction – No enhancement H and E stain and Beta Amyloid stain confirm the diagnosis of Amyloid Angiopathy Diagnosis: Amyloid Angiopathy Case 2: 24 Year female presenting with multiple episodes of headache seizures and right sided weakness. T1W , FLAIR and T2W images depict confluent area of T2-FLAIR signal abnormality in the left posterior frontal and parietal shite matter with no significant mass effect. T2W coronal, FLAIR sagittal images depict similar white matter changes.Multiple punctate foci of microhemorrhage are noted on the GRE sequence. Focal leptomeningeal and perivascular space enhancement is noted on the post gadolinium axial image. MR spectroscopy reveals Decreased peak heights of all metabolites. • Case analysis – – – – – – Young female patient (Unlikely to be ABRA) Non discrete subcortical white matter lesion Absence of other lesions (unlikely to be ADEM) Presence of microhemorrhage Leptomeningeal enhancement Lack of choline peak (Unlikely to be tumor or acute demyelination Internal elastic lamina Lumen H & E stain reveals thickening of the tunica media Media with inflammatory changes surrounding the adventia representing features of Primary CNS angiitis Diagnosis: Adventitia Primary CNS Angiitis Case 3. 63 Year male presenting with subacute onset seizures and left sided weakness. T2W and FLAIR images depict confluent area of hyperintense signal abnormality in the right frontal subcortical white matter with minimal mass effect and Diffusion restriction. Nodular and linear enhancement is predominantly centered around the perivascular spaces on the post gadolinium images. • Case Analysis – Subacute onset – Deep cerebral non-discrete white matter disease – No significant mass effect – Nodular and perivascular enhancement lymphocytes – Diffusion restriction Vessel lumen CD20 immunostaining positive for lymphoma H & E stain shows diffuse sheet of lymphocytes encasing the vessel ( arrows) . CD20 immunostaining positive for lymphoma. Diagnosis: Angiocentric Lymphoma Case 4: 65 Year male presenting with subacute onset of altered level of consciousness and seizures. T2W and FLAIR images depict confluent area of hyperintense signal abnormality in both cerebral hemispheres with nodular and linear enhancement on the post gadolinium images. Diffusion restriction is predominantly noted in the central deep white matter. • Case analysis – Subacute onset – White matter lesions are non discrete, multiple, involves subcortical, deep cerebral and periventricular white matter. – Positive diffusion restriction – Perivascular enhancement H & E stain showing sludging of the vessel lumen by lymphocytes (arrow) . CD45 immunostaining positive for lymphoma (arrow). Diagnosis Intravascular Lymphoma Case 5. 51 Year female HIV Positive and low CD4 count presenting with seizures and abnormal behavior T2W and FLAIR images depict confluent areas of hyperintense signal abnormality in both cerebral hemispheres extending into the parieto-occipital subcortical and deep white matter. Diffusion restriction is noted along the periphery of these lesions with no enhancement on the post gadolinium images. Generalized Volume loss is noted . Diffusion restriction ,lack of mass effect and no enhancement are the key features. • Case analysis – Immunodeficiency patient – Diffuse and confluent white matter lesions – Absence of mass effect – Absence of enhancement – Diffusion restriction at the advancing edge H & E stain showing enlarged oligodendrocyte infected with PML virus (arrow). PML virus probe stain demonstarting the viral inclsuion bodies within the infected oligodendrocyte (arrow). Diagnosis: PML Case 6. 46 Year male presenting with left sided weakness and facial paresthesia. T2W and FLAIR images depict confluent hyperintense signal abnormality in the right posterior frontal and parietal subcortical white matter. Please note the mainted morphology of the adjacent cortex. Incomplete ring enhancement is noted with peripheral diffusion restriction . MR spectroscopy shows elevated choline peak and reduced NAA. • Case analysis – Focal discrete subcortical lesion – Maintained morphology of the adjacent cortex – “Open- ring” or “C” type enhancement with the open end facing the the gray matter (Key finding) – Peripheral diffusion restriction – High choline peak, low NAA peak Normal Myelin Myelin pallor Zone of transition LFB stain (Luxol fast blue stain) demonstrates the myelin pallor corresponding to the demyelinating zone and the area of transition with normal myelin staining( arrow) Diagnosis: Tumefactive MS Case 7. 52 Year male presenting with seizures. T2W and FLAIR images demonstrate confluent areas of infiltrative pattern of hyperintense signal abnormality predominantly involving the right temporal lobe and insular cortex with extension across the midline. Focal diffusion restriction is noted in the right anterior putamen. There is minimal mass effect with effacement of cortical sulci. However there is no midline shift. Intense enhancement with elevated rCBV is noted in the right anterior putamen focus on perfusion study. Rest of the infiltrative white matter changes do not exhibit any obvious enhancement. • Case analysis – Older patient – Diffuse confluent involvement of >3 brain lobes associated with mass effect (Key finding) – Focal area of enhancement with increased rCBV (Key finding) Ki-67 proliferation marker showing high proliferation index. Diagnosis: Gliomatosis cerebri Conclusion • Pattern recognition of the T2 abnormality is the key to successful diagnosis of the white matter lesions – – – – Remember the clinical presentation Assess lesion morphology Assess lesion(s) distribution Look for suggestive clues from • • • • • Post contrast imaging Diffusion imaging Perfusion imaging Spectroscopy Angiography – If no clue: look for appropriate CSF and blood tests – If still no clue: Suggest biopsy