Safe Motherhood
advertisement

Safe Motherhood: 2005 - 2008
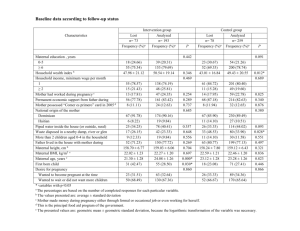
Access and barriers to measures targeted to prevent malaria in
pregnancy in rural Kenya.
Author:
Gikandi PW; Noor AM; Gitonga CW; Ajanga AA; Snow RW
Source:
Tropical Medicine and International Health. 2008 Feb;13(2):208-217.
Abstract:
The objectives were to evaluate barriers preventing pregnant women
from using insecticide-treated nets (ITN) and intermittent presumptive
treatment (IPT) with sulphadoxine-pyrimethamine (SP) 5 years after the
launch of the national malaria strategy promoting these measures in
Kenya. All women aged 15-49 years were interviewed during a
community survey in four districts between December 2006 and January
2007. Women pregnant in the last 12 months were asked about their age,
parity, education, use of nets, ITN, antenatal care (ANC) services and
sulphadoxine-pyrimethamine (SP) (overall and for IPT) during
pregnancy. Homestead assets were recorded and used to develop a
wealth index. Travel time to ANC clinics was computed using a
geographic information system algorithm. Predictors of net and IPT use
were defined using multivariate logistic regression. Overall 68% of
pregnant women used a net; 52% used an ITN; 84% attended an ANC
clinic at least once and 74% at least twice. Fifty-three percent of women
took at least one dose of IPT-SP, however only 22% took two or more
doses. Women from the least poor homesteads (OR = 2.53, 1.36-4.68) and
those who used IPT services (OR = 1.73, 1.24-2.42) were more likely to
sleep under any net. Women who used IPT were more likely to use ITNs
(OR = 1.35, 1.03-1.77), while those who lived more than an hour from an
ANC clinic were less likely (OR = 0.61, 0.46-0.81) to use ITN. Women with
formal education (1.47, 1.01-2.17) and those who used ITN (OR: 1.68, 1.202.36) were more likely to have received at least one dose of IPT-SP.
Although the use of ITN had increased 10-fold and the use of IPT
fourfold since last measured in 2001, coverage remains low. Provider
practices in the delivery of protective measures against malaria must
change, supported by community awareness campaigns on the
importance of mothers' use of IPT. (author's)
Language:
English
Keywords:
KENYA | RESEARCH REPORT | KAP SURVEYS | PREGNANT
WOMEN | WOMEN IN DEVELOPMENT | RURAL POPULATION |
PROGRAM ACCESSIBILITY | PREGNANCY COMPLICATIONS |
BED NETS | ANTENATAL CARE | PARITY | EDUCATIONAL
STATUS | PESTICIDES | MALARIA PREVENTION |
SOCIOECONOMIC STATUS | DEVELOPING COUNTRIES |
AFRICA, EASTERN | AFRICA, SUB SAHARAN | AFRICA |
SURVEYS | SAMPLING STUDIES | STUDIES | RESEARCH
1
Safe Motherhood: 2005 - 2008
METHODOLOGY | POPULATION CHARACTERISTICS |
DEMOGRAPHIC FACTORS | POPULATION | ECONOMIC
DEVELOPMENT | ECONOMIC FACTORS | PROGRAM
EVALUATION | PROGRAMS | ORGANIZATION AND
ADMINISTRATION | DISEASES | PARASITE CONTROL | PUBLIC
HEALTH | HEALTH | MATERNAL HEALTH SERVICES |
MATERNAL-CHILD HEALTH SERVICES | PRIMARY HEALTH
CARE | HEALTH SERVICES | DELIVERY OF HEALTH CARE |
FERTILITY MEASUREMENTS | FERTILITY | POPULATION
DYNAMICS | SOCIOECONOMIC FACTORS | INGREDIENTS AND
CHEMICALS | MALARIA | PARASITIC DISEASES
Document Number: 324984
Child nutritional status and maternal factors in an urban slum in
Nairobi, Kenya.
Author:
Thuita FM; Mwadime RK; Wang'ombe JK
Source:
East African Medical Journal. 2005 Apr;82(4):209-215.
Abstract:
The objective was to assess the relationship between maternal factors and
child nutritional status among children aged 6-36 months. Design: Cross
sectional descriptive survey. Setting: Urban slum settlement in Nairobi,
Kenya. Subjects: This study included a random sample of 369 households
of mothers with children aged 6-36 months at the time of the study.
Maternal factors which showed a positive significant association with at
least one of the three child nutritional status indicators (height for age,
weight for age and weight for height) were birth spacing, parity, maternal
education level and mothers marital status. Child spacing and parity
emerged as the most important predictors of stunting among study
children. Maternal nutritional status was also shown to be positively
associated with child nutritional status. Maternal ill health had a negative
effect on child nutritional status. Maternal factors are an underlying cause
of childhood malnutrition. (author's)
Language:
English
Keywords:
KENYA | RESEARCH REPORT | CROSS SECTIONAL ANALYSIS |
URBAN POPULATION | SLUMS | MOTHERS | CHILD |
MATERNAL HEALTH | CHILD HEALTH | CHILD NUTRITION |
MALNUTRITION | AFRICA, EASTERN | AFRICA SOUTH OF THE
SAHARA | AFRICA | DEVELOPING COUNTRIES | RESEARCH
METHODOLOGY | POPULATION CHARACTERISTICS |
DEMOGRAPHIC FACTORS | POPULATION | URBANIZATION |
2
Safe Motherhood: 2005 - 2008
URBAN POPULATION DISTRIBUTION | POPULATION
DISTRIBUTION | GEOGRAPHIC FACTORS | PARENTS | FAMILY
RELATIONSHIPS | FAMILY CHARACTERISTICS | FAMILY AND
HOUSEHOLD | SOCIOCULTURAL FACTORS | YOUTH | AGE
FACTORS | HEALTH | NUTRITION | NUTRITION DISORDERS |
DISEASES
Document Number: 293567
Seroprevalence of hepatitis B markers in pregnant women in
Kenya.
Author:
Okoth F; Mbuthia J; Gatheru Z; Murila F; Kanyingi F
Source:
East African Medical Journal. 2006 Sep;83(9):485-493.
Abstract:
Objective:
To evaluate hepatitis B serological markers in pregnant women from
various geographical sites in Kenya. Design: A cross-sectional
observational study of women attending antenatal clinics. Setting: The
Kenyatta National Hospital and eight hospitals from five provinces in
Kenya. Subjects: All women in their third trimester of pregnancy
attending the antenatal clinic over the period June 2001 to June 2002.
Main outcome measures: For each pregnant woman age and gestation
were documented. Hepatitis serological markers were evaluated. Results:
A total of 2,241 pregnant women were enrolled. Among them 205 women
(9.3%) were positive for HbsAg and from these 18 (8.8%) were found to
have HbeAg. Protective antibodies (anti-HbsAg) were detected in 669
(30.2%) of the women. There were notable significant regional differences
for HbsAg rates. Conclusions: These results confirm the presence of high
disease carrier rate and the corresponding previously reported low level
of HbeAg suggesting questionable low rate of perinatal transmission but
high rate of horizontal transmission. (author's)
Language:
English
Keywords:
KENYA | RESEARCH REPORT | CROSS SECTIONAL ANALYSIS |
PREGNANT WOMEN | PREGNANCY, THIRD TRIMESTER |
HEPATITIS | ANTIBODIES | LABORATORY PROCEDURES |
TRANSMISSION | RISK FACTORS | DEVELOPING COUNTRIES |
AFRICA, EASTERN | AFRICA, SUB SAHARAN | AFRICA |
RESEARCH METHODOLOGY | POPULATION CHARACTERISTICS
| DEMOGRAPHIC FACTORS | POPULATION | PREGNANCY |
REPRODUCTION | VIRAL DISEASES | DISEASES |
IMMUNOLOGIC FACTORS | IMMUNITY | IMMUNE SYSTEM |
3
Safe Motherhood: 2005 - 2008
PHYSIOLOGY | BIOLOGY | LABORATORY EXAMINATIONS AND
DIAGNOSES | EXAMINATIONS AND DIAGNOSES | MEDICAL
PROCEDURES | MEDICINE | HEALTH SERVICES | DELIVERY OF
HEALTH CARE | HEALTH | INFECTIONS
Document Number: 308848
Caesarian section rates and perinatal outcome at the Aga Khan
University Hospital, Nairobi.
Author:
Wanyonyi S; Sequeira E; Obura T
Source:
East African Medical Journal. 2006 Dec;83(12):651-658.
Abstract:
There has been a persistent rise in the rate of Caesarean sections over the
years. Whether this rise is the cause of the decline in infant mortality and
improved neonatal outcome still remains debatable. The objective was to
compare the Caesarian section rate and the perinatal outcome at the Aga
Khan University Hospital for the years 2001 and 2004. The design used
was a retrospective study. The Aga Khan University Hospital, Nairobi
was used for the setting of the study. Main outcome measures: The total
Caesarian section rates, their indication and the perinatal outcome. The
overall Caesarian section rate was 20.4% in 1996, 25.9% in 2001 and 38.1%
in 2004. The rate among patients managed by their private obstetricians
was 27.1% in 1996, 30.8% in 2001 and 41.7% in 2004. Whilst among
general patients, it was 14.7%, 21.5% and 34.5% over the same period. The
main indication for emergency Caesarian section was foetal distress,
while that for elective Caesarian section was a previous uterine scar. The
overall perinatal mortality rate improved from 25.2 per 1,000 births in
2001 to 14.0 per 1,000 births in 2004 (P< 0.001, 95%CL 8.58-30.62). The
early neonatal mortality rate was 12.8 per 1,000 live births in 2001
compared to 10.8 per 1,000 live births in 2004 (p=0.08, 95%CI 9.84-13.76).
There has been a significant increase in Caesarian section rate over the
years. Being a referral unit dealing with many high-risk patients some of
whom are supervised elsewhere and with a significant ratio of private
patients, the high rate of Caesarean section at the Aga Khan University
Hospital is expected. The rise could also be due to early detection of
foetal compromise and improved diagnostic facilities leading to timely
intervention. However, there has been a significant improvement in the
neonatal outcome over the same period of time. Whether this is an effect
of the high Caesarean section rate is debatable and calls for further
research to correlate the two. (author's)
4
Safe Motherhood: 2005 - 2008
Language:
English
Keywords:
KENYA | RESEARCH REPORT | RETROSPECTIVE STUDIES |
INFANT | PREGNANT WOMEN | INFANT MORTALITY |
PERINATAL MORTALITY | CHILDBIRTH | LOW BIRTH WEIGHT
| CESAREAN SECTION | PREGNANCY COMPLICATIONS |
DEVELOPING COUNTRIES | AFRICA, EASTERN | AFRICA, SUB
SAHARAN | AFRICA | STUDIES | RESEARCH METHODOLOGY |
YOUTH | AGE FACTORS | POPULATION CHARACTERISTICS |
DEMOGRAPHIC FACTORS | POPULATION | MORTALITY |
POPULATION DYNAMICS | PREGNANCY OUTCOMES |
PREGNANCY | REPRODUCTION | BIRTH WEIGHT | BODY
WEIGHT | PHYSIOLOGY | BIOLOGY | OBSTETRICAL SURGERY |
SURGERY | TREATMENT | MEDICAL PROCEDURES | MEDICINE
| HEALTH SERVICES | DELIVERY OF HEALTH CARE | HEALTH |
DISEASES
Document Number: 319530
Low use of skilled attendant's delivery services in rural Kenya.
Author:
Cotter K; Hawken M; Temmerman M
Source:
Journal of Health, Population and Nutrition. 2006 Dec;24(4):467-471.
Abstract:
The aim of the study was to estimate the use of skilled attendants'
delivery services among users of antenatal care and the coverage of
skilled attendants' delivery services in the general population in Kikoneni
location, Kenya. Data collected from the registers at the Kikoneni Health
Centre (KHC) from March 2001 through March 2003 were retrospectively
reviewed. Antenatal care attendance, deliveries by skilled attendants, and
the percentage of antenatal care attendees who delivered in a healthcare
facility were assessed. Deliveries at the KHC were compared with
expected births in the population to estimate the coverage of deliveries
assisted by skilled attendants in the community. Of 994 women who
attended the antenatal care clinic, 74 (7.4%) presented for delivery
services. 5.4% of expected births in the population occurred in health
facilities. The coverage of deliveries assisted by skilled attendants was far
below the national and international goals. The use of institutional
delivery services was very low even among antenatal care attendees.
Targeted programmatic efforts are necessary to increase skilled
attendant-assisted births, with the ultimate goal of reducing maternal
mortality. (author's)
5
Safe Motherhood: 2005 - 2008
Language:
English
Keywords:
KENYA | RESEARCH REPORT | ESTIMATION TECHNICS |
RETROSPECTIVE STUDIES | MIDWIVES AND MIDWIFERY |
PREGNANT WOMEN | WOMEN IN DEVELOPMENT | DELIVERY
OF HEALTH CARE | ANTENATAL CARE | CHILDBIRTH |
UTILIZATION OF HEALTH CARE | AFRICA, EASTERN | AFRICA
SOUTH OF THE SAHARA | AFRICA | DEVELOPING COUNTRIES
| RESEARCH METHODOLOGY | STUDIES | HEALTH
PERSONNEL | HEALTH | POPULATION CHARACTERISTICS |
DEMOGRAPHIC FACTORS | POPULATION | ECONOMIC
DEVELOPMENT | ECONOMIC FACTORS | MATERNAL HEALTH
SERVICES | MATERNAL-CHILD HEALTH SERVICES | PRIMARY
HEALTH CARE | HEALTH SERVICES | PREGNANCY OUTCOMES
| PREGNANCY | REPRODUCTION
Document Number: 315576
The effect of health care worker training on the use of intermittent
preventive treatment for malaria in pregnancy in rural western
Kenya.
Author:
Ouma PO; Van Eijk AM; Hamel MJ; Sikuku E; Odhiambo F
Source:
Tropical Medicine and International Health. 2007 Aug;12(8):953-961.
Abstract:
In 1998, Kenya adopted intermittent preventive treatment (IPTp) with
sulphadoxine-pyrimethamine (SP) for malaria prevention during
pregnancy. We conducted a survey in 2002 among women who had
recently delivered in the rural neighbouring areas Asembo and Gem and
reported coverage of 19% of at least one dose and 7% of two or more
doses of SP. Health care workers (HCW) in Asembo were retrained on
IPTp in 2003. The objectives were to evaluate if IPTp coverage increased
and if the training in Asembo led to better coverage than in Gem, and to
identify barriers to the effective implementation of IPTp. Communitybased cross-sectional survey among a simple random sample of women
who had recently delivered in April 2005, interviews with HCW of
antenatal clinics (ANC) in Asembo and Gem. Of the 724 women
interviewed, 626 (86.5%) attended the ANC once and 516 (71.3%)
attended two or more times. Overall IPTp coverage was 41% for at least
one dose, and 21% for at least two doses of SP. In Asembo, coverage
increased from 19% in 2002 to 61% in 2005 for at least one dose and from
7% to 17% for two doses of SP. In Gem, coverage increased from 17% to
28% and 7% to 11%, respectively. Interviews of HCW in both Asembo
6
Safe Motherhood: 2005 - 2008
and Gem revealed confusion about appropriate timing, and lack of direct
observation of IPTp. Training of HCW and use of simplified IPTp
messages may be a key strategy in achieving Roll Back Malaria targets for
malaria prevention in pregnancy in Kenya. (author's)
Language:
English
Keywords:
KENYA | RURAL AREAS | RESEARCH REPORT | HEALTH
PERSONNEL | MALARIA PREVENTION | PREGNANCY | DRUGS
| ADMINISTRATION AND DOSAGE | ANTENATAL CARE |
CLINIC ACTIVITIES | TRAINING ACTIVITIES | DEVELOPING
COUNTRIES | AFRICA, EASTERN | AFRICA, SUB SAHARAN |
AFRICA | GEOGRAPHIC FACTORS | POPULATION | DELIVERY
OF HEALTH CARE | HEALTH | MALARIA | PARASITIC
DISEASES | DISEASES | REPRODUCTION | TREATMENT |
MEDICAL PROCEDURES | MEDICINE | HEALTH SERVICES |
MATERNAL HEALTH SERVICES | MATERNAL-CHILD HEALTH
SERVICES | PRIMARY HEALTH CARE | PROGRAM ACTIVITIES |
PROGRAMS | ORGANIZATION AND ADMINISTRATION |
TRAINING PROGRAMS | EDUCATION
Document Number: 320316
Quality of record keeping in the intrapartum period at the
Provincial General Hospital, Kakamega, Kenya.
Author:
Wamwana EB; Ndavi PM; Gichangi PB; Karanja JG; Muia EG
Source:
East African Medical Journal. 2007Jan;84(1):16-23.
Abstract:
The objective was to assess the quality of recording critical events in the
intrapartum period in Kakamega Provincial General Hospital (PGHK). A
retrospective comparative study was used as the design. The setting of
the study was the Provincial General Hospital, Kakamega, the referral
hospital for Western Province, Kenya. Two hundred women admitted at
the labour ward during the six-month period between 1st September 2000
and 28th February 2001 were compared to two hundred women admitted
between 1st July 2001 and 31st December 2001. The Safe Motherhood
Demonstration Project (SMDP) was introduced in four districts of
Western Province, Kenya, in which PGHK is located. It included on job
training in Safe Motherhood which emphasised, among others, collection
and utilisation of maternal health care services data. Comprehensiveness
of recording of biodata, history taking and examination findings were
assessed for women in labour before and during the implementation of
the SMDP. The proportion of cases in labour managed by use of
7
Safe Motherhood: 2005 - 2008
partograph and its appropriate use were also determined. Retrieval rate
of patients' notes was 86.9% and 89.6% before and during SMDP
respectively. Information on socio demographic characteristics, history
taking, general and obstetric examination had a near universal recording
in both groups but data on alcohol consumption, smoking, menarche,
previous pregnancies and contraceptive use was poorly recorded. There
was a significant improvement in recording of diagnosis and plan of
management during the SMDP (p=0.037). The partograph was used in
only 11% of patients before SMDP as compared to 85% during SMDP
(p=0.000). Record on foetal condition and progress of labour were
significantly improved during the SMDP (p=0.000). Records on summary
of labour likewise significantly improved during the SMDP (p=0.02). The
quality of record keeping in the intrapartum period at the PGHK greatly
improved during the implementation of the SMDP. It would be
worthwhile to assess the sustainability of quality of intrapartum records
and care a year or so after the SMDP ended. (author's)
Language:
English
Keywords:
KENYA | RESEARCH REPORT | RETROSPECTIVE STUDIES |
COMPARATIVE STUDIES | PROGRESS REPORT | PREGNANT
WOMEN | MATERNAL HEALTH SERVICES | CHILDBIRTH |
RECORDS | HOSPITALS | INTERVENTIONS | EVALUATION |
DEVELOPING COUNTRIES | AFRICA, EASTERN | AFRICA, SUB
SAHARAN | AFRICA | STUDIES | RESEARCH METHODOLOGY |
POPULATION CHARACTERISTICS | DEMOGRAPHIC FACTORS |
POPULATION | MATERNAL-CHILD HEALTH SERVICES |
PRIMARY HEALTH CARE | HEALTH SERVICES | DELIVERY OF
HEALTH CARE | HEALTH | PREGNANCY OUTCOMES |
PREGNANCY | REPRODUCTION | INFORMATION PROCESSING
| INFORMATION | HEALTH FACILITIES | PROGRAMS |
ORGANIZATION AND ADMINISTRATION
Document Number: 319298
The effects of maternal helminth and malaria infections on motherto-child HIV transmission.
Author:
Gallagher M; Malhotra I; Mungai PL; Wamachi AN; Kioko JM
Source:
AIDS. 2005;19:1849-1855.
8
Safe Motherhood: 2005 - 2008
Abstract:
Objective:
To investigate the effect of helminth and/or malaria infection on the risk
of HIV infection in pregnant women and its transmission to their
offspring.
Design:
A retrospective cohort study of pregnant Kenyan women and their
offspring from term, uncomplicated vaginal deliveries (n = 936) with a
nested case–control study.
Methods:
We determined the presence of HIV, malaria, schistosomiasis, lymphatic
filariasis, and intestinal helminthes in mothers and tested for HIV
antibodies in 12-24 month-old offspring of HIV-positive women. We
related these findings to the presence of cord blood lymphocyte
activation and cytokine production in response to helminth antigens.
Results: HIV-positive women (n = 83, 8.9% of all women tested) were 2fold more likely to have peripheral blood and/or placental malaria (P <
0.025) and a 2.1-fold greater likelihood of lymphatic filariasis infection (P
< 0.001) compared to location- and- parity matched HIV-negative women.
Women with HIV and malaria tended to show an increased risk for
mother-to-child-transmission (MTCT) of HIV, although this difference
was not significant. MTCT of HIV, however, was significantly higher in
women co-infected with one or more helminthes (48%) verses women
without helminth infections (10%, P < 0.01; adjusted odds ratio, 7.3; 95%
confidence interval, 2.4–33.7). This increased risk for MTCT of HIV
correlated with cord blood lymphocytes production of interleukin5/interleukin-13 in response to helminth antigens (P < 0.001). Conclusion:
Helminth co-infection is associated with increased risk for MTCT of HIV,
possibly by a mechanism in which parasite antigens activates
lymphocytes in utero. Treatment of helminthic infections during
pregnancy may reduce the risk of MTCT of HIV. (author's)
Language:
English
Keywords:
KENYA | RESEARCH REPORT | COHORT ANALYSIS |
PREGNANT WOMEN | INFANT | HIV POSITIVE PERSONS |
MALARIA | SCHISTOSOMIASIS | MOTHER-TO-CHILD
TRANSMISSION | FILARIASIS | DEVELOPING COUNTRIES |
AFRICA, EASTERN | AFRICA SOUTH OF THE SAHARA | AFRICA
| RESEARCH METHODOLOGY | POPULATION
CHARACTERISTICS | DEMOGRAPHIC FACTORS | POPULATION
| YOUTH | AGE FACTORS | PERSONS LIVING WITH HIV/AIDS |
HIV INFECTIONS | VIRAL DISEASES | DISEASES | PARASITIC
DISEASES | TRANSMISSION | INFECTIONS
Document Number: 292082
9
Safe Motherhood: 2005 - 2008
Jill Sheffield: Nurturing safe motherhood.
Author:
Das P
Source:
Lancet
Abstract:
One day when Jill Sheffield was working as a volunteer for a family
planning clinic at the Pumwani Maternity Hospital in Kenya, a woman
walked into the clinic carrying a newborn baby on her front, and an older
baby on her back. She had had 11 pregnancies, had six living children,
and was just 27 years old. It was the mid-1960s and Kenya was one of
only two African countries that had a national family planning
programme, but to get contraceptives a woman had to have her
husband's signature. This woman had not sought her husband's
permission. Sheffield still remembers her response to this woman's plight:
"I was the same age and had no children; I thought holy smoke, stuff the
rules. I made sure she got contraceptives, and thought: I have to change
this. From that day on I wanted to make sure that women everywhere
had as much choice as they could because if you can't plan your fertility,
you can't plan your life." Sheffield went on to become the co-founder and
President of Family Care International (FCI), a non-profit organisation
that has made impressive contributions to maternal health and adolescent
sexual and reproductive health. This year is the 20th anniversary of FCI
and the Safe Motherhood Initiative-a global campaign to reduce maternal
mortality that Sheffield has championed since its inception. (excerpt)
Language:
English
Keywords:
KENYA | CRITIQUE | EVALUATION | POLICYMAKERS | SAFE
MOTHERHOOD | NONGOVERNMENTAL ORGANIZATIONS |
LEADERSHIP | MATERNAL HEALTH | CONTRACEPTIVE
AVAILABILITY | FAMILY PLANNING POLICY | DEVELOPING
COUNTRIES | AFRICA, EASTERN | AFRICA, SUB SAHARAN |
AFRICA | ADMINISTRATIVE PERSONNEL | ORGANIZATION
AND ADMINISTRATION | HEALTH | ORGANIZATIONS |
POLITICAL FACTORS | SOCIOCULTURAL FACTORS |
CONTRACEPTION | FAMILY PLANNING | POPULATION POLICY
| SOCIAL POLICY | POLICY
Document Number: 321870
10
Safe Motherhood: 2005 - 2008
Editor's Comment; Lessons and accomplishments 20 years after the
Safe Motherhood Conference in Nairobi.
Author:
Fortney JA
Source:
International Journal of Gynecology and Obstetrics. 2007 Sep
Abstract :
It is 20 years since the Safe Motherhood Conference in Nairobi. What
have we learned and what have we accomplished since then? Our
knowledge base is a good deal more solid than it was 20 years ago. While
we might wish that the nature of the evidence were more rigorous
(though it is rarely practical or ethical to conduct randomized control
trials of most programs), we have more than enough evidence to proceed.
We have learned to focus our attention and resources on two
complementary approaches - skilled attendance at delivery and access to
emergency obstetric care (EmOC) for when complications arise. While
Graham et al. have shown that skilled attendance at delivery and the
maternal mortality ratio are closely correlated, they found, too, that this is
truer when the skilled attendants are physicians than when they are
midwives. Some have wondered if this means we should be promoting
hospital deliveries, and we need more data on this. The important lesson
is that skilled attendance means midwives and physicians and not semiskilled workers (such as community health workers) with only a few
weeks of training, and definitely not traditional birth attendants whether trained or not. Unfortunately some countries, especially in south
Asia, are going the semi-skilled worker route. (Excerpt)
Language:
English
Keywords:
KENYA | CRITIQUE | SAFE MOTHERHOOD | MATERNAL
HEALTH | PREGNANCY COMPLICATIONS | REPRODUCTIVE
HEALTH | OBSTETRICS | MATERNAL HEALTH SERVICES |
QUALITY OF HEALTH CARE | EMERGENCY SERVICES |
KNOWLEDGE | INTERVENTIONS | DEVELOPING COUNTRIES |
AFRICA, EASTERN | AFRICA, SUB SAHARAN | AFRICA |
HEALTH | DISEASES | MEDICINE | HEALTH SERVICES |
DELIVERY OF HEALTH CARE | MATERNAL-CHILD HEALTH
SERVICES | PRIMARY HEALTH CARE | HEALTH SERVICES
EVALUATION | PROGRAM EVALUATION | PROGRAMS |
ORGANIZATION AND ADMINISTRATION | SOCIOCULTURAL
FACTORS
Document Number: 319404
11
Safe Motherhood: 2005 - 2008
Delivering safer motherhood: Sharing the evidence.
Author:
Fikree FF; Worley H; Sines E
Source:
Washington, D.C., Population Reference Bureau [PRB], 2007.
Abstract :
Every year an estimated half a million women die in childbirth.
Unfortunately, this global figure has changed little since the problem was
first highlighted in 1987 at the Safe Motherhood Conference in Nairobi,
Kenya. These deaths, mostly in developing countries, are primarily from
haemorrhage, infection, and complications of abortion. Progress has been
meagre in the poorest countries due to weak health systems, substandard
quality of care, inadequate human resources, insufficient political
commitment and funds, and lack of data to inform and monitor
intervention strategies. In response, safe motherhood experts have
proposed a variety of strategies over the last 20 years to help reduce
maternal deaths, based on care in health facilities, as well as at home and
in the community. Some strategies focus on increasing skilled attendants
at delivery to ensure that more women deliver their babies with health
care providers with midwifery skills. Other strategies focus on
eliminating delays when complications arise by improving, for example,
family awareness of danger signs, referral systems, or emergency
obstetric services at health centres and district hospitals. (excerpt)
Language:
English
Keywords:
KENYA | INDONESIA | GHANA | SUMMARY REPORT |
MOTHERS | MATERNAL MORTALITY | CHILDBIRTH | DEATH
RATE | SAFE MOTHERHOOD | MATERNAL HEALTH |
MATERNAL HEALTH SERVICES | QUALITY OF HEALTH CARE |
EMERGENCY SERVICES | GOALS | FEES | MEASUREMENT |
PROGRAM DEVELOPMENT | DEVELOPING COUNTRIES |
AFRICA, EASTERN | AFRICA, SUB SAHARAN | AFRICA | ASIA,
SOUTHEASTERN | ASIA | AFRICA, WESTERN | PARENTS |
FAMILY RELATIONSHIPS | FAMILY CHARACTERISTICS |
FAMILY AND HOUSEHOLD | SOCIOCULTURAL FACTORS |
MORTALITY | POPULATION DYNAMICS | DEMOGRAPHIC
FACTORS | POPULATION | PREGNANCY OUTCOMES |
PREGNANCY | REPRODUCTION | HEALTH | MATERNAL-CHILD
HEALTH SERVICES | PRIMARY HEALTH CARE | HEALTH
SERVICES | DELIVERY OF HEALTH CARE | HEALTH SERVICES
EVALUATION | PROGRAM EVALUATION | PROGRAMS |
ORGANIZATION AND ADMINISTRATION | PLANNING |
FINANCIAL ACTIVITIES | ECONOMIC FACTORS | RESEARCH
METHODOLOGY
Document Number: 320061
12
Safe Motherhood: 2005 - 2008
Reproductive health issues in rural western Kenya.
Author:
van Eijk AM; Lindblade KA; Odhiambo F; Peterson E; Sikuku E
Source:
Reproductive Health. 2008
Abstract :
We describe reproductive health issues among pregnant women in a
rural area of Kenya with a high coverage of insecticide treated nets (ITNs)
and high prevalence of HIV (15%). We conducted a community-based
cross-sectional survey among rural pregnant women in western Kenya. A
medical, obstetric and reproductive history was obtained. Blood was
obtained for a malaria smear and haemoglobin level, and stool was
examined for geohelminths. Height and weight were measured. Of 673
participants, 87% were multigravidae and 50% were in their third
trimester; 41% had started antenatal clinic visits at the time of interview
and 69% reported ITN-use. Malaria parasitemia and anaemia
(haemoglobin less than 11 g/dl) were detected among 36% and 53% of
the women, respectively. Geohelminth infections were detected among
76% of the 390 women who gave a stool sample. Twenty percent of
women were underweight, and sixteen percent reported symptoms of
herpes zoster or oral thrush in the last two months. Nineteen percent ofall
women reported using a contraceptive method to delay or prevent
pregnancy before the current pregnancy (injection 10%, pill 8%, condom
0.4%). Twenty-three percent of multigravidae conceived their current
pregnancy within a year of the previous pregnancy. More than half of the
multigravidae (55%) had ever lost a live born child and 21% had lost their
last singleton live born child at the time of interview. In this rural area
with a high HIV prevalence, the reported use of condoms before
pregnancy was extremely low. Pregnancy health was not optimal with a
high prevalence of malaria, geohelminth infections, anaemia and
underweight. Chances of losing a child after birth were high. Multiple
interventions are needed to improve reproductive health in this area.
(author's)
Language:
English
Keywords:
KENYA | RESEARCH REPORT | COMMUNITY SURVEYS | CROSS
SECTIONAL ANALYSIS | PREGNANT WOMEN | REPRODUCTIVE
HEALTH | MALARIA | HIV | BODY WEIGHT | CONDOM USE |
CONTRACEPTIVE USAGE | ANTENATAL CARE | BED NETS |
DEVELOPING COUNTRIES | AFRICA, EASTERN | AFRICA, SUB
SAHARAN | AFRICA | SURVEYS | SAMPLING STUDIES |
STUDIES | RESEARCH METHODOLOGY | POPULATION
CHARACTERISTICS | DEMOGRAPHIC FACTORS | POPULATION
| HEALTH | PARASITIC DISEASES | DISEASES | HIV
INFECTIONS | VIRAL DISEASES | PHYSIOLOGY | BIOLOGY |
RISK REDUCTION BEHAVIOR | BEHAVIOR | CONTRACEPTION
13
Safe Motherhood: 2005 - 2008
| FAMILY PLANNING | MATERNAL HEALTH SERVICES |
MATERNAL-CHILD HEALTH SERVICES | PRIMARY HEALTH
CARE | HEALTH SERVICES | DELIVERY OF HEALTH CARE |
PARASITE CONTROL | PUBLIC HEALTH
Document Number: 325394
Pharmacokinetics of sulfadoxine-pyrimethamine in HIV-infected
and uninfected pregnant women in western Kenya.
Author:
Green MD; van Eijk AM; van ter Kuile FO; Ayisi JG; Parise ME
Source:
Journal of Infectious Diseases. 2007 Nov
Abstract :
Sulfadoxine-pyrimethamine (SP) is among the most commonly used
antimalarial drugs during pregnancy, yet the pharmacokinetics of SP are
unknown in pregnant women. HIV-infected (HIV+) women require more
frequent doses of intermittent preventive therapy with SP than do HIVuninfected (HIV-) women. We investigated whether this reflects their
impaired immunity or an HIV-associated alteration in the disposition of
SP. Seventeen pregnant HIV- women and 16 pregnant HIV+ women
received a dose of 1500 mg of sulfadoxine and 75 mg of pyrimethamine.
Five HIV- and 6 HIV+ postpartum women returned 2-3 months after
delivery for another dose. The pharmacokinetics of sulfadoxine and
pyrimethamine were compared between these groups. HIV status did not
affect the area under the curve (AUC/or8) or the half-lives of sulfadoxine
or pyrimethamine in prepartum or postpartum women, although partum
status did have a significant affect on sulfadoxine pharmacokinetics.
Among prepartum women, the median half-life for sulfadoxine was
significantly shorter than that observed in postpartum women (148 vs 256
h; P < .001), and the median AUC/or8 was ~40% lower (22,816 vs 40,106
microg/mL/h, P < .001). HIV status and partum status did not show any
significant influence on pyrimethamine pharmacokinetics. Pregnancy
significantly modifies the disposition of SP, whereas HIV status has little
influence on pharmacokinetic parameters in pregnant women. (author's)
Language:
English
Keywords:
| RESEARCH REPORT | COMPARATIVE STUDIES | PREGNANT
WOMEN | POSTPARTUM WOMEN | HIV POSITIVE PERSONS |
HIV INFECTIONS | ANTIMALARIAL DRUGS | DEVELOPING
COUNTRIES | AFRICA, EASTERN | AFRICA, SUB SAHARAN |
AFRICA | STUDIES | RESEARCH METHODOLOGY |
POPULATION CHARACTERISTICS | DEMOGRAPHIC FACTORS |
POPULATION | PUERPERIUM | REPRODUCTION | PERSONS
14
Safe Motherhood: 2005 - 2008
LIVING WITH HIV/AIDS | VIRAL DISEASES | DISEASES |
MALARIA | PARASITIC DISEASES
Document Number: 321164
Deep Dive: An Exploration of Innovation Improving Quality in the
Private Sector. Case study: Scaling Up Post Abortion Care Services.
Contributed by IntraHealth International.
Author:
IntraHealth International. PRIME
Source:
Bethesda, Maryland, Abt Associates, Private Sector Partnerships One
[PSP-One], 2005 May 24. 6 p.
Abstract:
Building on a successful pilot, PRIME II dramatically scaled up a
program in three of Kenya's seven provinces to create accessible, high
quality primary-level PAC services by trained private sector nursemidwives. This initiative has been continued and expanded under the
ACQUIRE Project. The pivotal role these nurse-midwives can play in
treating emergency complications, increasing use of family planning, and
providing or making referrals for other reproductive health services
holds promise for reducing maternal mortality and decreasing the
chances of repeat abortion among PAC clients, many of whom are
adolescents. Complications from unsafe abortion account for more than a
third of all maternal mortality in Kenya. Starting in 1999, PRIME
collaborated with the Kenya MOH and key stakeholders - including the
Nursing Council of Kenya (NCK) and the National Nursing Association
of Kenya (NNAK) - to train private and NGO sector nurse-midwives in
PAC. To implement the pilot program in 1999, PRIME introduced a
partnership approach to ensure stakeholder buy-in, create training and
supervision structures within the private sector, and strengthen links
between the private and public sectors. The pilot established PAC
services by trained nurse-midwives at 44 private sector facilities in six
districts, serving both urban and rural populations. The success of the
program convinced the MOH, NCK, and NNAK that nurse-midwives are
capable of providing quality PAC services and that this care increases the
accessibility and use of FP services. The key stakeholders worked first
with PRIME II then starting in 2004, with ACQUIRE and other agencies in
the scale-up of the program. (excerpt)
Language:
English
Keywords:
KENYA | ADMINISTRATIVE DISTRICTS | EVALUATION REPORT
| CASE STUDIES | PILOT PROJECTS | NURSE-MIDWIVES |
15
Safe Motherhood: 2005 - 2008
NONGOVERNMENTAL ORGANIZATIONS | USAID |
PERFORMANCE IMPROVEMENT | PRIVATE SECTOR |
ABORTION | TECHNICAL ASSISTANCE | TRAINING
PROGRAMS | PROGRAM ACCESSIBILITY | CAPACITY
BUILDING | DEVELOPING COUNTRIES | AFRICA, EASTERN |
AFRICA, SUB SAHARAN | AFRICA | GEOGRAPHIC FACTORS |
POPULATION | EVALUATION | STUDIES | RESEARCH
METHODOLOGY | HEALTH PERSONNEL | DELIVERY OF
HEALTH CARE | HEALTH | ORGANIZATIONS | POLITICAL
FACTORS | SOCIOCULTURAL FACTORS | GOVERNMENT
AGENCIES | MANAGEMENT | ORGANIZATION AND
ADMINISTRATION | MACROECONOMIC FACTORS |
ECONOMIC FACTORS | HEALTH FACILITIES | PROGRAMS |
EDUCATION | PROGRAM EVALUATION | PROGRAM
SUSTAINABILITY
Antenatal care and perinatal outcomes in Kwale district, Kenya.
Author:
Brown CA; Sohani SB; Khan KS; Lilford RJ; Mukhwana W
Source:
BMC Pregnancy and Childbirth. 2008 Jan 10;8:2.
Abstract:
The importance of antenatal care (ANC) for improving perinatal
outcomes is well established. However access to ANC in Kenya has
hardly changed in the past 20 years. This study aims to identify the
determinants of attending ANC and the association between attendance
and behavioural and perinatal outcomes (live births and healthy birth
weight) for women in the Kwale region of Kenya. A Cohort survey of
1,562 perinatal outcomes (response rate 100%) during 2004-05 in the
catchment areas for five Ministry of Health dispensaries in two divisions
of the Kwale region. The associations between background and
behavioural decisions on ANC attendance and perinatal outcomes were
explored using univariate analysis and multivariate logistic regression
models with backwards-stepwise elimination. The outputs from these
analyses were reported as odds ratios (OR) with 95% confidence intervals
(CI). Only 32% (506/1,562) of women reported having any ANC. Women
with secondary education or above (adjusted OR 1.83; 95% CI 1.06-3.15)
were more likely to attend for ANC, while those living further than 5km
from a dispensary were less likely to attend (OR 0.29; 95% CI 0.22-0.39).
Paradoxically, however, the number of ANC visits increased with
distance from the dispensary (OR 1.46; 95% CI 1.33-1.60). Women
attending ANC at least twice were more likely to have a live birth (vs.
stillbirth) in both multivariate models. Women attending for two ANC
visits (but not more than two) were more likely to have a healthy weight
baby (OR 4.39; 95% CI 1.36-14.15). The low attendance for ANC,
combined with a positive relationship between attendance and perinatal
16
Safe Motherhood: 2005 - 2008
outcomes for the women in the Kwale region highlight the need for
further research to understand reasons for attendance and nonattendance and also for strategies to be put in place to improve
attendance for ANC. (author's)
Language:
English
Keywords:
KENYA | RESEARCH REPORT | COHORT ANALYSIS |
PREGNANT WOMEN | MOTHERS | ANTENATAL CARE |
PREGNANCY OUTCOMES | EDUCATIONAL STATUS | CLINIC
VISITS | IMPACT | DEVELOPING COUNTRIES | AFRICA,
EASTERN | AFRICA, SUB SAHARAN | AFRICA | RESEARCH
METHODOLOGY | POPULATION CHARACTERISTICS |
DEMOGRAPHIC FACTORS | POPULATION | PARENTS | FAMILY
RELATIONSHIPS | FAMILY CHARACTERISTICS | FAMILY AND
HOUSEHOLD | SOCIOCULTURAL FACTORS | MATERNAL
HEALTH SERVICES | MATERNAL-CHILD HEALTH SERVICES |
PRIMARY HEALTH CARE | HEALTH SERVICES | DELIVERY OF
HEALTH CARE | HEALTH | PREGNANCY | REPRODUCTION |
SOCIOECONOMIC STATUS | SOCIOECONOMIC FACTORS |
ECONOMIC FACTORS | SERVICE STATISTICS | PROGRAM
ACTIVITIES | PROGRAMS | ORGANIZATION AND
ADMINISTRATION | COMMUNICATION
Document Number: 323623
Antibodies among men and children to placental-binding
Plasmodium falciparum-infected erythrocytes that express var2csa.
Author:
Beeson JG, Ndungu F, Persson KE, Chesson JM, Kelly GL, Uyoga S,
Hallamore SL, Williams TN, Reeder JC, Brown GV, Marsh K
Source:
Am J Trop Med Hyg. 2007 Jul;77(1):22-8.
Abstract:
During pregnancy, specific variants of Plasmodium falciparum-infected
erythrocytes (IEs) can accumulate in the placenta through adhesion to
chondroitin sulfate A (CSA) mediated by expression of PfEMP1 encoded
by var2csa-type genes. Antibodies against these variants are associated
with protection from maternal malaria. We evaluated antibodies among
Kenyan, Papua New Guinean, and Malawian men and Kenyan children
against two different CSA-binding P. falciparum isolates expressing
var2csa variants. Specific IgG was present at significant levels among
some men and children from each population, suggesting exposure to
these variants is not exclusive to pregnancy. However, the level and
prevalence of antibodies was substantially lower overall than exposed
17
Safe Motherhood: 2005 - 2008
multigravidas. IgG-binding was specific and did not represent antibodies
to subpopulations of non-CSA-binding IEs, and some sera inhibited IE
adhesion to CSA. These findings have significant implications for
understanding malaria pathogenesis and immunity and may be
significant for understanding the acquisition of immunity to maternal
malaria.
Language:
English
Keywords:
|ADULT |ANIMALS |ANTIBODIES, PROTOZOAN
|BLOOD|*IMMUNOLOGY |ANTIGENS,
PROTOZOAN|*IMMUNOLOGY |CHILD |CROSS-SECTIONAL
STUDIES |ERYTHROCYTES|*PARASITOLOGY |FEMALE
|HUMANS |KENYA |MALARIA, FALCIPARUM|*IMMUNOLOGY
|PARASITOLOGY |MALE
|MIDDLE AGED |PAPUA NEW GUINEA |PLACENTA
|PARASITOLOGY |PLASMODIUM
FALCIPARUM|*IMMUNOLOGY |PREGNANCY|PREGNANCY
COMPLICATIONS,
PARASITIC|*IMMUNOLOGY|PARASITOLOGY
Document Number: 20080605
Biophysical profile scores and resistance indices of the umbilical
artery as seen in patients with pregnancy induced hypertension.
Author:
Nguku SW, Wanyoike-Gichuhi J, Aywak AA,
Source:
East Afr Med J. 2006 Mar;83(3):96-101
Abstract:
Objective:
The role of Biophysical Profile Score and resistive index of
the umbilical artery for monitoring pre-eclampsia patients. DESIGN:
Descriptive prospective study.
Setting:
Kenyatta National Hospital and Mater Hospital, Nairobi, Kenya.
Subjects:
One hundred and ten cases during a three month period.
Results:
Normal biophysical profile scores were found in 93 (84.5%), and 17
(17.5%) cases had abnormal scores ranging from mild to severe foetal
distress. Resistive index of umbilical artery (RI-UA) were normal in 72
18
Safe Motherhood: 2005 - 2008
(66.1%) and high resistive index accounted for 33.9%. Intra-Uterine
Growth Restriction (IUGR) was a prominent finding accounting for
30.5%. A positive relationship was shown to exist between IUGR and RIUA and also with severity of hypertension with P-values < 0.05. Resistive
index of umbilical artery was positively related to the duration of illness
confirming its dependence on chronicity (P = 0.004). Resistive index of
umbilical artery proved to be an earlier indicator of foetal compromise
before any foetal distress becomes obvious.
Conclusion:
Regular obstetrical ultra sound foetal surveillance in pre-eclampsia
patients is important for foetal wellbeing. Doppler evaluation of high risk
patients is more sensitive test than the biophysical profile score.
Language:
English
Keywords:
|ADOLESCENT |ADULT |FEMALE |FETAL GROWTH
RETARDATION |ULTRASONOGRAPHY |HUMANS
|HYPERTENSION, PREGNANCY-INDUCED
|PHYSIOPATHOLOGY |ULTRASONOGRAPHY |KENYA |PRE
ECLAMPSIA|*PHYSIOPATHOLOGY|*ULTRASONOGRAPHY
|PREGNANCY|PROSPECTIVE STUDIES |ULTRASONOGRAPHY,
DOPPLER |ULTRASONOGRAPHY,
PRENATAL|*METHODS|UMBILICAL
ARTERIES|*PHYSIOPATHOLOGY
Document Number: 20060803
Pregnancy outcomes in women with or without placental malaria
infection.
Author:
Kassam SN, - Nesbitt S, Hunt LP, Oster N, Soothill P, Sergi C
Source:
Gynaecol Int J Obstet. 2006 Jun;93(3):225-32. Epub 2006 Apr 13.
Abstract:
Objective:
To assess delivery outcomes in women with placental
malaria who presented at public hospitals in Kisumu, a holoendemic
region in western Kenya.
Methods:
A cross-sectional study using both histology and molecular biology was
conducted with 90 consecutive pregnant women who presented at 3
hospitals during a 2-week period. Data collectors completed
19
Safe Motherhood: 2005 - 2008
standardized questionnaires using each patient's hospital record and
physical examination results, and registered birth indices such as weight,
head circumference, and weight-head ratio. Malaria infection of the
placenta was assessed using a molecular biology approach (for genomic
differences among parasite species) as well as histology techniques. Of
the 5 histologic classes of placental infection, class 1 corresponds to active
infection and class 4 to past infection; class 2 and 3 to active chronic
infection; and class 5 to uninfected individuals. Plasmodium species
typing was determined by polymerase chain reaction amplification of the
parasite's genome.
Results:
In newborns at term, low birth weight was directly associated with
classes 2 and 4 of placental infection (P = 0.053 and P = 0.003,
respectively), and differences in birth weight remained significant
between the 5 classes (P <0.001) even after adjusting for parity and
mother's age. Plasmodium falciparum was the only detected parasite.
Conclusions:
In Kisumu, infection with P. falciparum is an important cause of low birth
weight and morbidity when it is associated with histologic classes 2 and 4
of placental infection. Moreover, polymerase chain reaction assays should
be supported by ministries of health as an ancillary method of collecting
data for malaria control during pregnancy and providing a baseline for
future interventions.
Language:
English
Keywords:
|ADOLESCENT |ADULT |BIRTH WEIGHT |CROSS-SECTIONAL
STUDIES|*ENDEMIC DISEASES |FEMALE |HUMANS |INFANT,
LOW BIRTH WEIGHT |INFANT, NEWBORN
|KENYA |EPIDEMIOLOGY |MALARIA|*EPIDEMIOLOGY
|MALARIA, FALCIPARUM |GENETICS |PARASITOLOGY
|MEDICAL RECORDS |PARASITEMIA |PARITY |PHYSICAL
EXAMINATION|PLACENTA |PARASITOLOGY |PLACENTA
DISEASES|*PARASITOLOGY |PREGNANCY|*PREGNANCY
COMPLICATIONS, PARASITIC|*PREGNANCY OUTCOME
|PREVALENCE |QUESTIONNAIRES
Document Number: 20060522
20
Safe Motherhood: 2005 - 2008
Earth-eating and reinfection with intestinal helminths among
pregnant and lactating women in western Kenya.
Author:
Luoba AI, Wenzel Geissler P, Estambale B
Source:
Trop Med Int Health. 2005 Mar;10(3):220-7.
Abstract:
We conducted a longitudinal study among 827 pregnant women in
Nyanza Province, western Kenya, to determine the effect of earth-eating
on geohelminth re-infection after treatment. The women were recruited
at a gestational age of 14-24 weeks (median: 17) and followed up to 6
months postpartum. The median age was 23 (range: 14-47) years, the
median parity 2 (range: 0-11). After deworming with mebendazole (500
mg, single dose) of those found infected at 32 weeks gestation,
700 women were uninfected with Ascaris lumbricoides, 670 with
Trichuris trichiura and 479 with hookworm. At delivery, 11.2%, 4.6% and
3.8% of these women were re-infected with hookworm, T. trichiura and
A. lumbricoides respectively. The re-infection rate for hookworm was
14.8%, for T. trichiura 6.65, and for A. lumbricoides 5.2% at 3 months
postpartum, and 16.0, 5.9 and 9.4% at 6 months postpartum. There was a
significant difference in hookworm intensity at delivery between
geophagous and non-geophagous women (P=0.03). Women who ate
termite mound earth were more often and more intensely infected with
hookworm at delivery than those eating other types of earth (P=0.07 and
P=0.02 respectively). There were significant differences in the prevalence
of A. lumbricoides between geophagous and non-geophagous women at
3 (P=0.001) and at 6 months postpartum (P=0.001). Women who ate
termite mound earth had a higher prevalence of A. lumbricoides,
compared with those eating other kinds of earth, at delivery (P=0.02), 3
months postpartum (P=0.001) and at 6 months postpartum (P=0.001). The
intensity of infections with T. trichiura at 6 months postpartum was
significantly different between geophagous and non-geophagous women
(P=0.005). Our study shows that geophagy is associated with A.
lumbricoides reinfection among pregnant and lactating women and that
intensities built up more rapidly among geophagous women. Geophagy
might be associated with reinfection with hookworm and T.
trichiura, although these results were less unequivocal. These findings
call for increased emphasis, in antenatal care, on the potential risks of
earth-eating, and for deworming of women after delivery.
Language: English
Keywords:
|ADOLESCENT |ADULT |ANIMALS |ASCARIASIS |ETIOLOGY|
ASCARIS LUMBRICOIDES |FEEDING BEHAVIOR |FEMALE
HELMINTHIASIS|*ETIOLOGY|HOOKWORM
INFECTIONS/ETIOLOG|HUMANS |INTESTINAL DISEASES,
21
Safe Motherhood: 2005 - 2008
PARASITIC|*ETIOLOGY|LACTATION|LONGITUDINAL
STUDIES
|MIDDLE AGED|PICA|*COMPLICATIONS|
PREGNANCY|PREGNANCY
COMPLICATIONS|PARASITIC|*ETIOLOGY
|RECURRENCE|RISK FACTORS|- SOIL/*PARASITOLOGY
TRICHURIASIS/ETIOLOGY
Successful pregnancy outcome following laparoscopic
myomectomy: case report.
Author:
Parkar RB, Wanyonyi S, Kamau WJ, Otieno D
Source:
East Afr Med J. 2008 Jun;85(6):301-5.
Abstract:
Laparoscopic myomectomy is now widely used as an alternative to
laparotomy in the management of symptomatic uterine fibroids. The
advantages of this minimal access approach outweigh those of the open
techniques. The pregnancy outcomes between the two methods have
been studied and are comparable, but there still exists a lot of scepticism
locally concerning this. It is against this background that we present a 31
year old nulliparous lady who had a two year history of primary
infertility secondary to multiple uterine fibroids, the largest being
fundal and measuring 6.6cm. She underwent a successful laparoscopic
myomectomy in November, 2006 and conceived spontaneously in
February 2007. Her antenatal follow up was uneventful. She delivered a
live male, 2,650 grams by Caesarean section in October, 2007 and had an
unremarkable peuperium. With the availability of proper equipment,
instruments, and adequately developing skills, laparoscopic
myomectomy is feasible locally and with proper patient selection could
result in favourable outcome as it is elsewhere.
Language:
English
Document Number: 20080910
Laparoscopic management of an ovarian ectopic pregnancy: case
report.
Author:
Patel Y, Wanyonyi SZ, Rana FS,
Source:
East Afr Med J. 2008 Apr;85(4):201-4.
Abstract:
Ovarian pregnancy is a rare variant of ectopic gestation. The diagnosis is
22
Safe Motherhood: 2005 - 2008
often made at surgery and requires histological confirmation. The
condition has not been reported locally and its diagnosis is easily missed.
A case of an ovarian ectopic pregnancy in a 41 year old para 1 + 1 with
secondary infertility is reported. The patient presented with lower
abdominal pain and vaginal bleeding at six weeks gestation with a serum
B-hCG of 79.12 mlU/L. An ultrasound showed a complex left adnexal
mass. She underwent a diagnostic and operative laparoscopy.
A left oophorectomy was performed due to difficulty in achieving
haemostasis.
Language:
English
Keywords:
|ADULT |FEMALE |HUMANS| LAPAROSCOPY| OVARIECTOMY
|OVARY/*SURGERY| PREGNANCY| PREGNANCY, ECTOPIC
|DIAGNOSIS |SURGERY |ULTRASONOGRAPHY RUPTURE
|SURGERY
Document Number: 20080821
Utility of antenatal HIV surveillance data to evaluate prevention of
mother-to-child HIV transmission programs in resource-limited
settings.
Author:
Bolu, O.; Anand, A.; Swartzendruber, A.; Hladik, W.; Marum, L. H.;
Sheikh, A. A.; Woldu, A.; Ismail, S.; Mahomva, A.; Greby, S., and Sabin,
K. Utility of antenatal
Source:
Am J Obstet Gynecol. 2007 Sep; 197(3 Suppl):S17-25.
Abstract:
Prevention of mother-to-child human immunodeficiency virus (HIV)
transmission (PMTCT) programs are expanding in resource-limited
countries and are increasingly implemented in antenatal clinics (ANC) in
which HIV sentinel surveillance is conducted. ANC sentinel surveillance
data can be used to evaluate the first visit of a pregnant woman to
PMTCT programs. We analyzed data from Kenya and Ethiopia, where
information on PMTCT test acceptance was collected on the 2005 ANC
sentinel surveillance forms. For Zimbabwe, we compared the 2005 ANC
sentinel surveillance data to the PMTCT program data. ANC surveillance
data allowed us to calculate the number of HIV-positive women not
participating in the PMTCT program. The percentage of HIV-positive
women missed by the PMTCT program was 17% in Kenya, 57% Ethiopia,
and 59% Zimbabwe. The HIV prevalence among women participating in
PMTCT differed from women who did not. ANC sentinel surveillance
can be used to evaluate and improve the first encounter in PMTCT
23
Safe Motherhood: 2005 - 2008
programs. Countries should collect PMTCT-related program data
through ANC surveillance to strengthen the PMTCT program.
Highly active antiretroviral therapy versus zidovudine/nevirapine
effects on early breast milk HIV type- 1 Rna: a phase II randomized
clinical trial.
Author:
Chung, M. H.; Kiarie, J. N.; Richardson, B. A.; Lehman, D. A.; Overbaugh,
J.; Kinuthia, J.; Njiri, F., and John-Stewart, G. C.
Source:
Antivir Ther. 2008; 13(6):799-807.
Abstract:
Background:
Defining the effect of antiretroviral regimens on breast milk HIV type-1
(HIV-1) levels is useful to inform the rational design of strategies to
decrease perinatal HIV-1 transmission.
Methods:
Pregnant HIV-1 seropositive women (CD4+ T-cell count >250 and <500
cells/mm3) electing to breastfeed in Nairobi, Kenya were randomized to
highly active antiretroviral therapy (HAART; zidovudine [ZDV],
lamivudine and nevirapine [NVP]) during pregnancy and 6 months postpartum or to short-course ZDV plus single-dose NVP (ZDV/NVP). Breast
milk samples were collected two to three times per week in the first
month post-partum.
Results:
Between November 2003 and April 2006, 444 breast milk samples were
collected from 58 randomized women during the first month after
delivery. Between 3 and 14 days post-partum, women in the HAART and
ZDV/NVP arms had a similar prevalence of undetectable breast milk
HIV-1 RNA. From 15 to 28 days post-partum, women in the HAART arm
had significantly lower levels of breast milk HIV-1 RNA than women
randomized to ZDV/NVP (1.7 log10 copies/ml [limit of detection] versus
>2.10 log10 copies/ml, P<0.001). In contrast to breast milk HIV-1 RNA,
suppression of plasma HIV-1 RNA during the neonatal period was
consistently several log10 greater in the HAART arm compared with the
ZDV/NVP arm.
Conclusions:
HAART resulted in lower breast milk HIV-1 RNA than ZDV/NVP;
however, ZDV/NVP yielded comparable breast milk HIV-1 RNA levels
in the first 2 weeks post-partum. Breast milk HIV-1 RNA remained
suppressed in the ZDV/NVP arm despite increased plasma HIV-1 levels,
which might reflect local drug effects or compartmentalization.
24
Safe Motherhood: 2005 - 2008
Seizing the big missed opportunity: linking HIV and maternity
care services in sub-Saharan Africa.
Author:
Druce, N. and Nolan, A.
Source:
Reprod Health Matters. 2007 Nov; 15(30):190-201.
Abstract:
This paper draws on two reviews commissioned by the UK Department
for International Development in 2006-2007 that explore progress in
linking HIV prevention and maternity services in sub-Saharan Africa.
Although pilot and demonstration projects have been successful, progress
in scaling up PMTCT has been slow, reaching just 11% of pregnant HIV
positive women in much of Africa, less than half the percentage of
coverage achieved by antiretroviral treatment programmes for adults in
need. Despite ongoing efforts to promote comprehensive approaches,
significant policy, financing and institutional barriers, and weak coordination and leadership, continue to hamper progress. Maternal health
services face human and financial resource shortages which affect their
capacity to integrate HIV prevention. Both HIV and maternal health
programmes often receive targeted financial and technical assistance that
does not take the other into account. However, proposals in 2007 from a
number of countries to the Global Fund to Fight AIDS, TB and Malaria
incorporate sexual and reproductive health programming that will have
an impact on HIV, including certain maternity services. Moreover,
Botswana, Kenya and Rwanda have shown that progress can be made
where national commitment and increased resources are enabling
maternal and newborn care to address HIV.
Biophysical profile scores and resistance indices of the umbilical
artery as seen in patients with pregnancy induced hypertension.
Author:
Nguku, S. W.; Wanyoike-Gichuhi, J., and Aywak, A. A.
Source:
East Afr Med J. 2006 Mar; 83(3):96-101.
Abstract:
Objective:
The role of Biophysical Profile Score and resistive index of the umbilical
artery for monitoring pre-eclampsia patients.
Design:
Descriptive prospective study.
Setting:
Kenyatta National Hospital and Mater Hospital, Nairobi, Kenya.
25
Safe Motherhood: 2005 - 2008
Subjects:
One hundred and ten cases during a three month period.
Results:
Normal biophysical profile scores were found in 93 (84.5%), and 17
(17.5%) cases had abnormal scores ranging from mild to severe foetal
distress. Resistive index of umbilical artery (RI-UA) were normal in 72
(66.1%) and high resistive index accounted for 33.9%. Intra-Uterine
Growth Restriction (IUGR) was a prominent finding accounting for
30.5%. A positive relationship was shown to exist between IUGR and RIUA and also with severity of hypertension with P-values < 0.05. Resistive
index of umbilical artery was positively related to the duration of illness
confirming its dependence on chronicity (P = 0.004). Resistive index of
umbilical artery proved to be an earlier indicator of foetal compromise
before any foetal distress becomes obvious.
Conclusion:
Regular obstetrical ultra sound foetal surveillance in pre-eclampsia
patients is important for foetal wellbeing. Doppler evaluation of high risk
patients is more sensitive test than the biophysical profile score.
Seroprevalence of hepatitis B markers in pregnant women in
Kenya.
Author:
Okoth, F.; Mbuthia, J.; Gatheru, Z.; Murila, F.; Kanyingi, F.; Mugo, F.;
Esamai, F.; Alavi, Z.; Otieno, J.; Kiambati, H., and Wanjuki, N.
Source:
East Afr Med J. 2006 Sep; 83(9):485-93.
Abstract:
Objective:
To evaluate hepatitis B serological markers in pregnant women from
Design:
A cross-sectional observational study of women attending antenatal
clinics.
Setting:
The Kenyatta National Hospital and eight hospitals from five provinces
in Kenya.
Subjects:
All women in their third trimester of pregnancy attending the antenatal
clinic over the period June 2001 to June 2002.
26
Safe Motherhood: 2005 - 2008
Main outcome measures:
For each pregnant woman age and gestation were documented. Hepatitis
serological markers were evaluated.
Results:
A total of 2241 pregnant women were enrolled. Among them 205 women
(9.3%) were positive for HbsAg and from these 18 (8.8%) were found to
have HbeAg. Protective antibodies (anti-HbsAg) were detected in 669
(30.2%) of the women. There were notable significant regional differences
for HbsAg rates.
Conclusions:
These results confirm the presence of high disease carrier rate and the
corresponding previously reported low level of HbeAg suggesting
questionable low rate of perinatal transmission but high rate of horizontal
transmission.
Elevated gamma interferon-producing NK cells, CD45RO memorylike T cells, and CD4 T cells are associated with protection against
malaria infection in pregnancy.
Author:
Othoro, C.; Moore, J. M.; Wannemuehler, K. A.; Moses, S.; Lal, A.; Otieno,
J.; Nahlen, B.; Slutsker, L., and Shi, Y. P.
Source:
Infect Immun. 2008 Apr; 76(4):1678-85.
Abstract:
Previous studies have shown that gamma interferon (IFN-gamma)
production in the placenta is associated with protection against placental
malaria. However, it remains unknown which IFN-gamma-producing
cell subpopulations are involved in this protection and whether the
cellular immune components of protection are the same in the peripheral
and the placental blood compartments. We investigated cell
subpopulations for CD4, CD8, and CD45RO memory-like T cells and
CD56+/CD3- natural killer (NK) cells and for IFN-gamma production by
these cells in maternal peripheral and placental intervillous blood in
relation to the status of malaria infection in pregnancy. Of 52 human
immunodeficiency virus-negative enrolled pregnant women residing in
Western Kenya, 20 had placental parasitemia. We found that the
percentages of CD45RO memory-like and CD4 T cells were significantly
higher in the periphery than in the placenta, while the CD56/CD3- NKcell percentage was higher in the placenta than in the periphery,
suggesting differences in immune cell profiles between the two blood
compartments. Furthermore, the percentages of peripheral CD45RO
memory-like and CD4 T cells were significantly elevated in aparasitemic
women compared to levels in the parasitemic group, with aparasitemic
27
Safe Motherhood: 2005 - 2008
multigravid women having the highest percentages of CD45RO memorylike and CD4 T cells. In contrast, at the placental level, IFN-gamma
production by innate NK cells was significantly increased in aparasitemic
women compared to parasitemic women, regardless of gravidity. These
results suggest that the elevated IFN-gamma-producing NK cells in the
placenta and CD45RO memory-like and CD4 T cells in peripheral blood
may be involved in protection against malaria infection in pregnancy.
The effect of health care worker training on the use of intermittent
preventive treatment for malaria in pregnancy in rural western
Kenya.
Author:
Ouma, P. O.; Van Eijk, A. M.; Hamel, M. J.; Sikuku, E.; Odhiambo, F.;
Munguti, K.; Ayisi, J. G.; Kager, P. A., and Slutsker, L.
Source:
Trop Med Int Health. 2007 Aug; 12(8):953-61.
Abstract:
Background:
In 1998, Kenya adopted intermittent preventive treatment (IPTp) with
sulphadoxine-pyrimethamine (SP) for malaria prevention during
pregnancy. We conducted a survey in 2002 among women who had
recently delivered in the rural neighbouring areas Asembo and Gem and
reported coverage of 19% of at least one dose and 7% of two or more
doses of SP. Health care workers (HCW) in Asembo were retrained on
IPTp in 2003.
Objectives:
To evaluate if IPTp coverage increased and if the training in Asembo led
to better coverage than in Gem, and to identify barriers to the effective
implementation of IPTp.
Methods:
Community-based cross-sectional survey among a simple random
sample of women who had recently delivered in April 2005, interviews
with HCW of antenatal clinics (ANC) in Asembo and Gem.
Results:
Of the 724 women interviewed, 626 (86.5%) attended the ANC once and
516 (71.3%) attended two or more times. Overall IPTp coverage was 41%
for at least one dose, and 21% for at least two doses of SP. In Asembo,
coverage increased from 19% in 2002 to 61% in 2005 for at least one dose
and from 7% to 17% for two doses of SP. In Gem, coverage increased
from 17% to 28% and 7% to 11%, respectively. Interviews of HCW in both
Asembo and Gem revealed confusion about appropriate timing, and lack
of direct observation of IPTp.
28
Safe Motherhood: 2005 - 2008
Conclusion:
Training of HCW and use of simplified IPTp messages may be a key
strategy in achieving Roll Back Malaria targets for malaria prevention in
pregnancy in Kenya.
Millennium development goal 5: a review of maternal mortality at
the Kenyatta National Hospital, Nairobi.
Author:
Oyieke, J. B.; Obore, S., and Kigondu, C. S
Source:
East Afr Med J. 2006 Jan; 83(1):4-9.
Abstract:
Objectives: To review if there is a change in the maternal mortality rate at
the Kenyatta National Hospital since the inception of the Millennium
Development Goal strategy in 1990, compared to earlier reviews.
Design:
A retrospective descriptive study.
Setting:
Kenyatta National Hospital.
Subjects:
Maternal deaths attributed directly to obstetric causes.
Main outcome measures:
Determination of maternal mortality rates of all patients admitted to the
Kenyatta National Hospital Maternity and died after admission up till six
weeks of admission. Also determine any avoidable causes of the same.
Results:
During the period under review, there were 27,455 deliveries and 253
maternal deaths giving a maternal mortality ratio of 921.5 per 100,000 live
births. Direct obstetric causes accounted for 71% of all maternal deaths
with sepsis, haemorrhage, and hypertension being the leading causes.
Respiratory tract infections associated with HIV/ AIDS infection was the
prominent indirect cause. 67.5% of deaths occurred in women aged
between 25 and 35 years and 78.7% were Para 2 or less. Evidently there
was poor antenatal clinic attendance with only 28.6% having had any
attendance at all.
Conclusion:
Antenatal clinic attendance needs to be re-emphasised if an impact is to
be realised in curbing maternal mortality; moreover there is need for
early referrals and encouraging mothers to deliver under skilled care.
29
Safe Motherhood: 2005 - 2008
HIV, malaria, and infant anemia as risk factors for postneonatal
infant mortality among HIV-seropositive women in Kisumu,
Kenya.
Author:
van Eijk, A. M.; Ayisi, J. G.; Ter Kuile, F. O.; Slutsker, L.; Shi, Y. P.;
Udhayakumar, V.; Otieno, J. A.; Kager, P. A.; Lal, R. B.; Steketee, R. W.,
and Nahlen, B. L.
Source:
J Infect Dis. 2007 Jul 1; 196(1):30-7.
Abstract:
Background:
HIV and malaria in sub-Saharan Africa are associated with poor
pregnancy outcome and infant survival. We studied the association of
placental malaria, infant malaria and anemia, and infant HIV status with
postneonatal infant mortality (PNIM) among infants of HIV-seropositive
women.
Methods:
During 1996-2001, infants born to 570 HIV-seropositive mothers in
Kisumu, Kenya were monitored monthly for malaria (parasitemia or
clinical malaria) and anemia (hemoglobin level <8 g/dL) and vital status.
Results:
Thirty-nine deaths occurred among 112 HIV-positive infants (420/1000
live births [LBs] [95% confidence interval {CI}, 318-522 LBs]), and 36
occurred among 458 HIV-negative infants (99/1000 LBs [95% CI, 68-130
LBs]) (P<.001). In multivariate Cox regression analysis among HIVnegative infants, PNIM was associated with infant anemia (adjusted
hazard ratio [AHR], 5.03 [95% CI, 1.97-12.81]) but not with placental
malaria (AHR, 1.22 [95% CI, 0.50-2.95]) or infant malaria (AHR, 0.35 [95%
CI, 0.10-1.21]). Among HIV-positive infants, neither placental malaria
(AHR, 0.34 [95% CI, 0.10-1.10]) nor infant malaria (AHR, 0.31 [95% CI,
0.07-1.33]) or anemia (AHR, 1.07 [95% CI, 0.32-3.61]) was significantly
associated with PNIM.
Conclusion:
In this study population, placental malaria and infant parasitemia were
not risk factors for PNIM among infants of HIV-seropositive women. The
prevention of infant anemia may decrease PNIM among HIV-negative
infants of HIV-seropositive women
30
Safe Motherhood: 2005 - 2008
Reproductive health issues in rural Western Kenya.
Author:
Van Eijk, A. M.; Lindblade, K. A.; Odhiambo, F.; Peterson, E.; Sikuku, E.;
Ayisi, J. G.; Ouma, P.; Rosen, D. H., and Slutsker, L.
Source:
Reprod Health. 2008; 5:1.
Abstract:
Background:
We describe reproductive health issues among pregnant women in a
rural area of Kenya with a high coverage of insecticide treated nets (ITNs)
and high prevalence of HIV (15%).
Methods:
We conducted a community-based cross-sectional survey among rural
pregnant women in western Kenya. A medical, obstetric and
reproductive history was obtained. Blood was obtained for a malaria
smear and haemoglobin level, and stool was examined for geohelminths.
Height and weight were measured.
Results:
Of 673 participants, 87% were multigravidae and 50% were in their third
trimester; 41% had started antenatal clinic visits at the time of interview
and 69% reported ITN-use. Malaria parasitemia and anaemia
(haemoglobin < 11 g/dl) were detected among 36% and 53% of the
women, respectively. Geohelminth infections were detected among 76%
of the 390 women who gave a stool sample. Twenty percent of women
were underweight, and sixteen percent reported symptoms of herpes
zoster or oral thrush in the last two months. Nineteen percent of all
women reported using a contraceptive method to delay or prevent
pregnancy before the current pregnancy (injection 10%, pill 8%, condom
0.4%). Twenty-three percent of multigravidae conceived their current
pregnancy within a year of the previous pregnancy. More than half of the
multigravidae (55%) had ever lost a live born child and 21% had lost their
last singleton live born child at the time of interview.
Conclusion:
In this rural area with a high HIV prevalence, the reported use of
condoms before pregnancy was extremely low. Pregnancy health was not
optimal with a high prevalence of malaria, geohelminth infections,
anaemia and underweight. Chances of losing a child after birth were
high. Multiple interventions are needed to improve reproductive health
in this area.
31
Safe Motherhood: 2005 - 2008
Maternal health in the 2003 Kenya Demographic and Health
Survey.
Source:
2003 Kenya Demographic and Health Survey
Abstract:
The 2003 Kenya Demographic and Health Survey provides up-to-date
information on the population and health condition in Kenya. Maternal
health reflects a society's level of development as well as the performance
of the health care delivery system. Maternal health influences the health
of infants, children and families. As of 2003, Kenyan women have an
average of 4.9 children. 39 percent of currently married women use any
method of contraception. Only 14 percent of Kenyan women received a
dose of vitamin A postpartum. Less than 3 percent of Kenyan women
took iron tablets on at least 90 days during pregnancy. (excerpt)
Efavirenz use during pregnancy and for women of child-bearing
potential.
Author:
Chersich, M. F.; Urban, M. F.; Venter, F. W.; Wessels, T.; Krause, A.; Gray,
G. E.; Luchters, S., and Viljoen, D. L.
Source:
AIDS Res Ther. 2006; 3:11.
Abstract:
Background:
Efavirenz is the preferred non-nucleoside reverse transcriptase inhibitor
for first-line antiretroviral treatment in many countries. For women of
childbearing potential, advantages of efavirenz are balanced by concerns
that it is teratogenic. This paper reviews evidence of efavirenz
teratogenicity and considers implications in common clinical scenarios.
Findings:
Concerns of efavirenz-induced fetal effects stem from animal studies,
although the predictive value of animal data for humans is unknown.
Four retrospective cases of central nervous system birth defects in infants
with first trimester exposure to efavirenz have been interpreted as being
consistent with animal data. In a prospective pregnancy registry, which is
subject to fewer potential biases, no increase was detected in overall risk
of birth defects following exposure to efavirenz in the first-trimester.
Discussion:
For women planning a pregnancy or not using contraception, efavirenz
should be avoided if alternatives are available. According to WHO
guidelines for resource-constrained settings, benefits of efavirenz are
likely to outweigh risks for women using contraception. Women who
become pregnant while receiving efavirenz often consider drug
32
Safe Motherhood: 2005 - 2008
substitution or temporarily suspending treatment. Both options have
substantial risks for maternal and fetal health which, we argue, appear
unjustified after the critical period of organogenesis (3-8 weeks postconception). Efavirenz-based triple regimens, initiated after the first
trimester of pregnancy and discontinued after childbirth, are potentially
an important alternative for reducing mother-to-child transmission in
pregnant women who do not yet require antiretroviral treatment.
Conclusion:
Current recommendations for care for women who become pregnant
while receiving efavirenz may need to be re-considered, particularly in
settings with limited alternative drugs and laboratory monitoring. With
current data limitations, additional adequately powered prospective
studies are needed.
Pharmacokinetics of sulfadoxine-pyrimethamine in HIV-infected
and uninfected pregnant women in Western Kenya.
Author:
Green, M. D.; van Eijk, A. M.; van Ter Kuile, F. O.; Ayisi, J. G.; Parise, M.
E.; Kager, P. A.; Nahlen, B. L.; Steketee, R., and Nettey, H. Kenya.
Source:
J Infect Dis. 2007 Nov 1; 196(9):1403-8.
Abstract:
Background:
Sulfadoxine-pyrimethamine (SP) is among the most commonly used
antimalarial drugs during pregnancy, yet the pharmacokinetics of SP are
unknown in pregnant women. HIV-infected (HIV(+)) women require
more frequent doses of intermittent preventive therapy with SP than do
HIV-uninfected (HIV(-)) women. We investigated whether this reflects
their impaired immunity or an HIV-associated alteration in the
disposition of SP.
Methods:
Seventeen pregnant HIV(-) women and 16 pregnant HIV(+) women
received a dose of 1500 mg of sulfadoxine and 75 mg of pyrimethamine.
Five HIV(-) and 6 HIV(+) postpartum women returned 2-3 months after
delivery for another dose. The pharmacokinetics of sulfadoxine and
pyrimethamine were compared between these groups.
Results:
HIV status did not affect the area under the curve (AUC(0-->infinity)) or
the half-lives of sulfadoxine or pyrimethamine in prepartum or
postpartum women, although partum status did have a significant affect
on sulfadoxine pharmacokinetics. Among prepartum women, the median
half-life for sulfadoxine was significantly shorter than that observed in
postpartum women (148 vs 256 h; P<.001), and the median AUC(0--
33
Safe Motherhood: 2005 - 2008
>infinity) was ~40% lower (22,816 vs 40,106 microg/mL/h, P<.001). HIV
status and partum status did not show any significant influence on
pyrimethamine pharmacokinetics.
Conclusion:
Pregnancy significantly modifies the disposition of SP, whereas HIV
status has little influence on pharmacokinetic parameters in pregnant
women.
Incidence of wound infection after caesarean delivery in a district
hospital in central Kenya.
Author:
Koigi-Kamau, R.; Kabare, L. W., and Wanyoike-Gichuhi, J.
Source:
East Afr Med J. 2005 Jul; 82(7):357-61.
Abstract:
Objective:
To determine the incidence of post-caesarean wound infection.
Design:
Prospective descriptive study.
Setting:
Maternity unit of Kiambu District Hospital in Central Province of Kenya.
Subjects:
All women undergoing caesarean delivery during the study period.
Main outcome measures:
Overall incidence of post-caesarean wound infection, relationship
between incidence and socio-demographic characteristics, pre-operative
labour events, intrapartum events as well as HIV status.
Results:
The caesarean delivery rate was 7.8%. The overall post-caesarean wound
infection rate was 19%. The incidence was 32% among single women as
compared to 16% among married women, but this difference is not
statistically significant. Among the 35% of women who laboured for more
than 12 hours, the incidence of wound infection was 33% compared to
15% among those who laboured for 12 hours or less (p < 0.01). Rupture of
membranes (ROM) for more than 12 hours was associated with high
incidence of wound infection than among women in whom ROM was 12
hours or less (38% and 14% respectively, p < 0.001). Also duration of
operation exceeding 60 minutes was associated with much higher
incidence of wound infection (71%) compared to when the operation
lasted 60 minutes or less (16%, p < 0.001). The incidence of post-caesarean
34
Safe Motherhood: 2005 - 2008
wound infection does not appear to be significantly affected by HIV
status or whether caesarean delivery was emergency or elective.
Conclusion:
The overall post-caesarean wound infection rate is quite high. Prolonged
pre-operative duration of labour, prolonged ROM and long duration of
operation are associated with significantly higher incidence of wound
infection. This should be seen against a background of a relatively low
caesarean delivery rate and high incidence of prolonged labour. Strict
labour management policies need to be inculcated in labour wards in
District Hospitals in order to ensure timely caesarean delivery
interventions, and hence, reduce post-caesarean wound infection rates.
Umbilical cord--blood infections with Plasmodium falciparum
malaria are acquired antenatally in Kenya.
Author:
Malhotra I; Mungai P; Muchiri E; Kwiek, J. J., and . = Meshnick SR.
Source:
Journal of Infectious Diseases. 2006 Jul 15; 194(2):176-183.
Abstract:
It is unknown whether the presence of Plasmodium falciparum malaria
parasites in umbilical cord blood denotes infection acquired antenatally
or contamination with infected maternal blood at delivery. Parasites were
quantified by real-time quantitative polymerase chain reaction (RTQPCR) and were genotyped in paired maternal- and cord-blood samples
obtained from 632 pregnant Kenyan women and their newborns.
Placental alkaline phosphatase (PLAP) and polyclonal immunoglobulin E
levels were also quantified in paired maternal- and cord-blood samples,
as markers of admixture of maternal blood with cord blood. Sixty-six
cord-blood samples (10.4%) contained falciparum malaria, as detected by
RTQ-PCR. For 25 of the infected cord-blood samples, either absence of
infection was noted in paired maternal-blood samples at delivery (n = 16)
or amplicon levels in cord-blood samples were 10-fold higher than those
in maternal-blood samples (n = 9). Of the paired maternal- and cordblood samples that were both infected, 57% showed discordant malaria
parasite strains. There was no correlation between maternal parasitemia
and levels of PLAP and immunoglobulin E in cord blood. PLAP levels,
however, were significantly higher in cord-blood samples obtained from
newborns of primigravid or secundigravid women with placental
malaria, compared with cord-blood samples obtained from newborns of
women without placental malaria or multigravid women. These findings
indicate that parity and placental malaria are risk factors for maternofetal
transfusion. Malaria parasites identified in cord blood are acquired
antenatally by transplacental transmission of infected erythrocytes.
Primigravid and secundigravid women with placental malaria are at
increased risk for congenital infection. (author's)
35
Safe Motherhood: 2005 - 2008
Strengthening postnatal care services including postpartum family
planning in Kenya.
Author:
Mwangi A; Warren C; Koskei N, and Blanchard, H.
Abstract:
To improve the health and survival of mothers and infants in the
postnatal period, the Ministry of Health (MOH) in Kenya increased both
the recommended timing and content of postnatal services a women and
her infant should receive to at least three assessments within the first six
weeks after childbirth. The feasibility and acceptability of providing
postnatal care at these times has not been evaluated, however, and most
providers are not aware of this change in policy or how to implement it.
The objectives of the study were develop and introduce a strengthened
postnatal care package into one hospital and four health centers in one
district, to document the feasibility, acceptability and quality of care of
the strengthened postnatal care, and to evaluate the effectiveness of the
postnatal package on women's reproductive health behaviors. The study
was implemented jointly by the Population Council's Frontiers in
Reproductive Health (FRONTIERS) project and by Jhpiego's ACCESS-FP
project, both funded by USAID. The study was conducted in Embu
district, Eastern Province, between 2006 and 2008. The study used a prepost intervention design for assessing quality of care received within the
facilities and compared stratified samples of postpartum women
recruited and interviewed following childbirth and again six months later
before and after introduction of the intervention. For the quality of care
assessment, data were collected through interviews with health care
providers, structured observations of client -provider interactions during
the postnatal consultations and a facility inventory for assessing
availability of equipment, drugs, family planning commodities and
supplies. Postpartum women were recruited and interviewed following
childbirth on the postnatal ward in Embu Provincial General Hospital
and interviewed again in their community after six months. A postnatal
care -family planning (PNC-FP) orientation package for providers was
developed by ACCESS-FP, DRH and FRONTIERS. This incorporated
relevant maternal and newborn health care services in the postnatal
period with a specific focus on postpartum family planning. Job aids
were also produced. The three day orientation training included staff
from the maternity and MCH- FP units from the four health facilities, as
well as provincial and district RH trainers/supervisors. In total, 73 health
care providers were oriented in the PNC -FP package, as well as in the
use of a new postnatal register recently released by the MOH. Regular
supportive supervision visits were made during the intervention period
to reinforce application of the package. (author's)
36
Safe Motherhood: 2005 - 2008
Seroprevalence of hepatitis B markers in pregnant women in
Kenya.
Author:
Okoth, F.; Mbuthia, J.; Gatheru, Z.; Murila, F.; Kanyingi, F.; Mugo, F.;
Esamai, F.; Alavi, Z.; Otieno, J.; Kiambati, H., and Wanjuki, N.
Source:
East Afr Med J. 2006 Sep; 83(9):485-93.
Abstract:
Objective:
To evaluate hepatitis B serological markers in pregnant women from
various geographical sites in Kenya.
Design:
A cross-sectional observational study of women attending antenatal
clinics.
Setting:
The Kenyatta National Hospital and eight hospitals from five provinces
in Kenya.
Subjects:
All women in their third trimester of pregnancy attending the antenatal
clinic over the period June 2001 to June 2002.
Main outcome measures:
For each pregnant woman age and gestation were documented. Hepatitis
serological markers were evaluated.
Results:
A total of 2241 pregnant women were enrolled. Among them 205 women
(9.3%) were positive for HbsAg and from these 18 (8.8%) were found to
have HbeAg. Protective antibodies (anti-HbsAg) were detected in 669
(30.2%) of the women. There were notable significant regional differences
for HbsAg rates.
Conclusions:
These results confirm the presence of high disease carrier rate and the
corresponding previously reported low level of HbeAg suggesting
questionable low rate of perinatal transmission but high rate of horizontal
transmission.
37
Safe Motherhood: 2005 - 2008
Differences in health seeking behaviour among urban poor women
in Nairobi who experienced intended or unintended pregnancies.
Author:
Saliku, T.
Abstract:
The aim of the paper is to illustrate the differences in health seeking that
urban poor women present if the pregnancy they have is intended or not
intended. The premises in this study is that there are differences among
women who had intended or unintended pregnancies. This paper uses
data from a Maternal Health Project carried out by African Population
and Health Research Center within the framework of the Nairobi Urban
Health and Demographic Surveillance System (NUHDSS). NUHDSS
covers two informal settlements, namely Korogocho and Viwandani of
Nairobi City. Both areas have a total of about 60,000 people in about
24,000 households. Using the NUHDSS routinely collected data on
pregnancy outcomes, a total of 1927 women aged 12-54 years who had a
pregnancy outcome in 2004 and 2005 were sampled in this study and
interviewed between April and June 2006. Logistic regression, was used
to explore whether intended or unintended pregnancies were influenced
by the following factors; antenatal clinic attendance, number of times the
women attended ANC, choice of delivery, whether they sought care
during complications, if they went for antenatal clinic, age of women,
number of children women have, number of years of education, exposure
to information, access to health facilities and level of decision making.
Preliminary results suggest that women with unintended pregnancies
(31%) were more likely to seek care from unqualified personnel for
antenatal and delivery care compared those who wanted the pregnancies
(69%). In addition, women with unintended pregnancies had fewer visits
for antenatal care, which were initiated much later compared to those
women who had intended pregnancies. There is a difference in health
seeking behaviour during the pregnancy in terms of when to seek health
care, the type of provider sought and number of times women go to seek
care among women who have intended or unintended pregnancies,
similarly, access to information and the residence of the women were
determinants in the health seeking for these women. (author's)
Caesarian section rates and perinatal outcome at the Aga Khan
University Hospital, Nairobi.
Author:
Wanyonyi S; Sequeira E, and Obura, T
Source:
East African Medical Journal. 2006 Dec; 83(12):651-658.
Abstract:
There has been a persistent rise in the rate of Caesarean sections over the
years. Whether this rise is the cause of the decline in infant mortality and
38
Safe Motherhood: 2005 - 2008
improved neonatal outcome still remains debatable. The objective was to
compare the Caesarian section rate and the perinatal outcome at the Aga
Khan University Hospital for the years 2001 and 2004. The design used
was a retrospective study. The Aga Khan University Hospital, Nairobi
was used for the setting of the study. Main outcome measures: The total
Caesarian section rates, their indication and the perinatal outcome. The
overall Caesarian section rate was 20.4% in 1996, 25.9% in 2001 and 38.1%
in 2004. The rate among patients managed by their private obstetricians
was 27.1% in 1996, 30.8% in 2001 and 41.7% in 2004. Whilst among
general patients, it was 14.7%, 21.5% and 34.5% over the same period. The
main indication for emergency Caesarian section was foetal distress,
while that for elective Caesarian section was a previous uterine scar. The
overall perinatal mortality rate improved from 25.2 per 1,000 births in
2001 to 14.0 per 1,000 births in 2004 (P< 0.001, 95%CL 8.58-30.62). The
early neonatal mortality rate was 12.8 per 1,000 live births in 2001
compared to 10.8 per 1,000 live births in 2004 (p=0.08, 95%CI 9.84-13.76).
There has been a significant increase in Caesarian section rate over the
years. Being a referral unit dealing with many high-risk patients some of
whom are supervised elsewhere and with a significant ratio of private
patients, the high rate of Caesarean section at the Aga Khan University
Hospital is expected. The rise could also be due to early detection of
foetal compromise and improved diagnostic facilities leading to timely
intervention. However, there has been a significant improvement in the
neonatal outcome over the same period of time. Whether this is an effect
of the high Caesarean section rate is debatable and calls for further
research to correlate the two. (author's)
Outcomes following Preterm Pre-labour rupture of the
membranes.
Author:
Elizabeth Irura (1), Roseline Ochieng (2) and William Stones (1)
Source:
Departments of Obstetrics and Gynaecology (1) and Paediatrics (2), Aga
Khan University Hospital, Nairobi
Abstract:
Summary:
Outcomes after PPROM were reviewed following the introduction of a
new management protocol. Home based management following initial
stabilization in hospital was feasible. Use of this approach in other
settings will require consideration of case mix and access to hospital.
Objectives:
To review the maternal and neonatal outcomes with this approach for
PPROM between 24 and 34 weeks’ gestation.
39
Safe Motherhood: 2005 - 2008
Measures:
Impact of the introduction of a new management protocol.
Results:
Five patients were managed at home for between two and 10 days
following stabilization on the ward. Two neonates (birth weights 700g
and 770g) succumbed. Of the eight surviving neonates (including one set
of twins) complications included jaundice possibly related to sepsis
together with respiratory distress not requiring ventilation (two cases).
There were no maternal complications.
Conclusions:
Home based care between rupture of the membranes and delivery is
appropriate in selected cases.
Recommendations:
Application elsewhere of the protocol in use at our institution would
require consideration of the case mix and issues of access to hospital.
Bed rest during pregnancy.
Author:
Dr. Sikolia Wanyonyi MB ChB. Resident II, Dept of Obstetrics and
Gynecology;
Source:
Aga Khan University (EA)
Abstract:
Background:
Bed rest or restricted activity at home or in hospital is commonly advised
for many pregnancy complications. Its role in improving the pregnancy
outcome has been studied. There is need to balance this intervention with
the risk of thrombosis, stress to the women and its economic implications.
Objective:
To evaluate the effect of bed rest during pregnancy in preventing adverse
maternal and neonatal outcomes.
Search strategy:
The Cochrane Database of Systematic Reviews 2007, Issue 4 and PubMed
were searched.
Selection criteria:
Only published systematic reviews and randomized controlled trials with
reported data which compare clinical outcomes in pregnant women who
were prescribed bed rest or restriction of activity either at home or in
hospital for pregnancy-related complications compared with alternative
care or no intervention. The complications related to hypertensive
40
Safe Motherhood: 2005 - 2008
disorders, preterm labour, threatened miscarriage, embryo transfer,
intrauterine growth restriction and placenta previa were sought.
Main Results:
Four systematic reviews (comprising eight trials) and one randomized
control trial were reviewed. Thus a total of nine trials were considered.
No trials were found on the role of bed rest in the management of
placenta previa. In all the reviews there is insufficient evidence of high
quality to support the use of bed in the management of pregnancy
complications, with no benefit in the maternal or neonatal outcomes.
Conclusions:
The risks associated with bed rest and the economic implications thereof
are enormous. There is therefore need for better designed randomized
control trial to test the effectiveness of this intervention in pregnancy.
Recommendations:
Until further evidence is available recommendation of bed rest or
restriction of activity is not justified for routine clinical practice during
pregnancy.
Keywords:
BED REST| MISCARRIAGE| IUGR| PRETERM LABOR|
HYPERTENSION.
A case of Simultaneous viable Intrauterine, and Abdominal Ectopic
pregnancy. Management and outcome presented.
Author:
Dr Njuguna P. Samuel, Consultant Obstetrician and Gynecologist,
P.C.E.A Tumutumu hospital.
Abstract:
Ectopic pregnancy is among the leading causes of mortality among
pregnant women. Although the incidence of ectopic pregnancy is
estimated to be between 1 and 2%, the majority of these pregnancies are
located in the fallopian tube. However, pregnancies also occur implanted
in the cervix, ovary, previous cesarean scar, and at various intra
abdominal sites. The relative infrequency of these sites of implantation;
more so duo implantation makes the study of treatment efficacy difficult.
In fact, much of the knowledge surrounding the treatment of these
conditions remains
largely observational and anecdotal. Abdominal pregnancy may account
for up to 1.4% of ectopic pregnancies. Incidences of simultaneous
intrauterine and any site ectopic pregnancy are largely unknown.
Abdominal pregnancies refer to those with extra uterine implantations in
omentum, vital organs, or large vessels. These pregnancies can go
undetected until an advanced gestational age and often result in severe
41
Safe Motherhood: 2005 - 2008
hemorrhage. Rates of maternal mortality have been reported as high as
20%. Advanced abdominal pregnancy carries a risk of hemorrhage,
disseminated intravascular coagulation, bowel
obstruction, and fistulae. Frequently, these pregnancies are encountered
with a viable fetus, which complicates their management. A case of
simultaneous viable intrauterine, and abdominal ectopic pregnancy is
presented.
Health Workforce competence and Workplace Assessment for Safe
deliveries: Implications for Training and Performance
Improvements at the workplace.
Author:
Dr Alice Mutungi1, Dr Steven Harvey2, Dr Stephen Kinoti2, Thada
Bornstein2, Dr Elizabeth Hizza2, Dr Josephine Kibaru3 MOH/Kenya, Dr
Helen Lugina4 (1 University of Nairobi, Kenya; 2 University Research
company, USA; 3 Ministry of Health, Kenya; 4 East, Central and Southern
Africa Health Community, Arusha, Tanzania) 1Dr Alice Mutungi, Senior
Lecturer, Department of Obstetrics & Gynaecology,
Source:
University of Nairobi, P.O. Box 19676, Nairobi, Kenya. E-mail:
mutungialice@yahoo.com
Abstract:
Summary:
In most African countries, especially in East, Central and Southern Africa
(ECSA) region, maternal and neonatal mortalities are high. The
knowledge, skills mix and the competency of skilled attendants, coupled
with enabling environments that provide adequate supervision and
process standards, as well as essential equipment and supplies for the job,
are crucial to good maternal and newborn health outcomes. Analysis of
competency levels of the attendants and assessment of working
environments have critical implications for training and curricula
standardization in countries and the ECSA region.
Objectives:
To determine the competency levels of the workforce attending to women
during labor, delivery and early postpartum period; the environmental
and organizational factors that affect their productivity and performance;
and implications for performance improvement at the workplace.
Methods:
The study, conducted in 2 districts in each of 3 provinces (Nyanza,
Coast, and Eastern) in Kenya, assessed at least six hospital-based
birth attendants and at least 12 health center-based attendants in
each district. A total sample of 118 attendants and at least 19 health
42
Safe Motherhood: 2005 - 2008
facilities (one hospital and at least one health center in each district)
were assessed.
Levels of birth attendants’ knowledge and skills were assessed using a
knowledge-based questionnaire and anatomical models respectively, on
management of normal labor, delivery and immediate post-partum
period for the mother and newborn. Functionality of health facilities was
assessed using a checklist to document human resource complement,
infrastructure, processes of care, availability of supplies and equipment,
and mortality data.
Results:
Providers performed well in some areas such as knowledge test (63% of
questions were answered correctly), counseling mother on breast-feeding
(94%), and checking the placenta for completeness (>90%). The key weak
areas included the skills area where apart from active management of the
third stage of labour (AMTSL), more than 50% of the participants
completed less than half of the necessary steps correctly including:performing controlled cord traction (43%) and drying newborn
thoroughly (15%). Nonetheless, providers appreciated feedback and
performance improved immediately.
Regarding health systems, some key drugs such as antibiotics and
uterotonics were available in most health facilities but certain aspects were
wanting - for example organization and sustainability of referral/counterreferral systems and use of maternal and neonatal health standards.
Conclusions:
It is concluded that gaps exist with regard to health personnel
competency, infrastructure and referral systems. However there were
indications that some key problems can be resolved easily and at minimal
cost.
Recommendations:
There is need to work with stakeholders to make improvements in the
areas of identified gaps to ensure continuum of care, and to conduct
similar assessments in other ECSA member countries.
Use of Misoprostol for Post Abortion Care: a review.
Author:
Prof Joseph Karanja,
Source:
Associate Professor UoN, Council Member KOGS, PO Box 56772-00200,
Nairobi. 254 722 513881. Email: karanjajg@yahoo.com
43
Safe Motherhood: 2005 - 2008
Abstract:
Introduction:
Unsafely induced abortion is a major cause of maternal mortality and
morbidity in Sub Sahara Africa (SSA). This is mainly due to restrictive
laws and policies, stigma and inadequate reproductive health care
services which force desperate women to seek care from clandestine often
unskilled providers. The SSA region is characterized by a dearth of
physicians and midlevel providers, thus aggravating the problems of
women with incomplete abortion. The standard treatment of incomplete
in Kenya is surgical uterine evacuation using MVA which is only
performed by a few specially trained physicians, nurse-midwives and
clinical officers. In poor resource settings like SSA, a non-surgical method
of uterine evacuation would improve access and safety since it can be
administered by providers and facilities with no MVA capabilities but
linked to referral sites.
Review of the studies and find findings:
Misoprostol, an analogue of PGE1 originally introduced for treating
peptic ulcers, has been extensively studied for use in obstetrics and
gynaecology. Its safety and efficacy for various indications is well
established. In the past five years several randomized clinical trials
comparing its use with MVA for incomplete abortion have been carried
out in Tanzania, Bukina Faso and Mozambique. The studies showed that
misoprostol in a single oral dose of 600mcg is safe, acceptable and has
same or almost same efficacy as MVA in achieving complete uterine
evacuation. In some of the studies, the acceptability of misoprostol was
higher than that of MVA.
Conclusion:
Misoprostol is comparable to MVA in safety, efficacy and acceptability in
the treatment of incomplete abortion.
Recommendation:
Considering its many favourable attributes for low resource settings,
misoprostol should be made more widely available for treatment of
incomplete abortion in Kenya and the rest of Sub Sahara Africa.
Birth defects share the same platform of Congenital Anomalies
but they belong to different worlds. A case presentation.
Author:
Dr Kavoo Linge - Consultant obstretrican/Gynaecologist Nairobi
Hospital
Abstract:
Name T K IPNO 2101530 - Nairobi Hospital
Admitted 20 10 07 with h/o draining liquor at term only.
ANC - Was uneventiful Scan done was reported normal
44
Safe Motherhood: 2005 - 2008
PMH - Non significant
Her general and vital signs were within normal limits.
Her obstetric examination findings revealed a term pregnancy with
smallish bay in cephalic presentation and a normal foetal heart. Her
Cx was closed midline and non effaced. She was however draining
fresh me conium stained liquor in moderate amounts.
An Impression of Foetal distress was made and emergency
caesarean section done. A male child weighing 2150gm score 8/1
and 10/5 was delivered with gastroschisis. All other examination
findings of the baby were within normal limits.
Paediatric surgeon was immediately called in and confirmed the
diagnosis. Repair of the defect was performed under general
anesthesia within few hours after delivery.
Both the mother and the child did well thereafter and were
discharged on treatment on the 27th 10 07 to be followed up in
Sudan.
Discussion:
Gastroschisis (gas-tro-ski-sis) is a birth defect which is a
developmental anomaly. It is an opening in the abdominal wall
through which the internal organs push outside of the baby's body. It
occurs during fetal development whereby the abdominal wall fails to
close properly leaving an opening.
It occurs in approximately 1 out of every 5,000 births. The cause of
gastroschisis is unknown, but it is usually associated with younger
maternal age and small babies as in this case study. It is usually an
isolated defect not associated with chromosomal disorders or any
other birth defects as was found in this baby. The main problems
that are commonly associated with these babies are related to their
gastrointestinal system. Approximately 20 to 40 percent will have some
type of gastrointestinal abnormality such as: malrotation, atresia or
volvulus.
Prenatal diagnosis of gastroschisis may be suspected when the alpha feto
protein (AFP) is elevated. The diagnosis is usually confirmed by
ultrasound. whereby, the bowels and perhaps the liver may be seen
floating in the amniotic fluid. Ultrasound was done in this case
though the diagnosis was missed. Amniocentesis is usually not
necessary. Omphaloceles are associated with chromosomal abnormalities
and an amniocentesis may be offered.
45
Safe Motherhood: 2005 - 2008
The treatment of gastroschisis is immediate surgery soon after birth as
was done on this baby and the prognosis is good was in this case.
The prognosis of developmental disorders especially among the
minor and moderate defects can comfortably be described as
excellent as was like in our patient whose one stage surgical
intervention was all that was required.
In contrast Genetic disorders are a large group of disorders resulting
from either minor or major mutations in the genetic composition or
alterations in chromosomal numbers.
Although a few genetic disorders are curable majority are chronic,
incurable and require lifelong care and management strategies. They
require a multi level management approach through primary care which
is aimed at prevention, secondary care which is geared towards
treatment of the conditions and finally tertiary care which targets the
consequences. Despite advances in medical care, prevention of
hereditary disorders still remains the mainstay management.
The recent advances in the understanding of the molecular and
cellular basis of diseases coupled with availability of tools to
manipulate genetic diseases offer possibilities of new modes of
treatment. Gene therapies have shown potential usefulness among
animal models and sex ratio adjustment has also some promissory
role in managing some of these conditions but still awaits successful
transition into the mainstream clinical medicine.
Reducing Child Mortality and Disease and improving
Maternal health.
Author:
Professor S B O Ojwang. Dept. Of Obstetrics & Gynaecology, University
of Nairobi
Abstract:
Though child disease and mortality has declined in developed countries
the Decline has not been significant in developed parts of the world. This
also Applies to maternal morbidity and mortality especially in the subsaharan Region.
Millennium Development Goal {MDG} agreed upon by world leaders in
the Year 2000 resolved to a 50 percent reduction from 1990 levels of
Maternal Mortality by the year 2000 and a further 50 percent by the year
2015 i.e.an Overall reduction of 75 percent between 1990 – 2015.
46
Safe Motherhood: 2005 - 2008
In addition countries resolved to achieve infant mortality rate of 35 per
1000 Live births by the year 2015. {Source WHO/RHR/00.6}
Though safe motherhood is a human right, inspite of these commitments,
Throughout Africa, women and their children still do not benefit from
cost effective in health care interventions which would have immediate
impact, if used effectively by women and their children.
Death in children is mainly because of infections, including HIV/AIDS
and poor care during pregnancy. These could be prevented by good
health care, good nutrition and effective medical treatment.
In majority of developing countries, complications of pregnancy and
childbirth are the leading causes of death in women in their reproductive
age. It is estimated that over585 000 women die annually, because of these
complications. The majority of them in Africa. Fourty percent of women
experience complication during pregnancy and 15 percent develop lifethreatening problems.
Disease in children, death and maternal morbidity and mortality, in
Africa are partly due to misdirection of funds e.g. Corruption, which
sucks up funds that could be used for safe motherhood, improvement
vision of medicines and nutrition to children.
Medical societies can significantly contribute to prevention of maternal
death and disease and prevention of deaths sickness in children, through
Advocacy, dialogue promotion, addressing in equalities within the
countries and between countries about safe motherhood, disease and
mortality in Children. They can also lobby governments and interested
parties to make Reproductive health and child health priority and focus
of intervention.
Safe Motherhood is Achievable for Developing countries.
Author:
Prof. Joseph Karanja, Associate Professor of Obs/Gynae, UoN, & Council
Member KOGS
Abstract:
Background:
Sweden and other Scandinavian countries recognized 300 hundred years
ago that simple measures can make motherhood safe even at an era when
home delivery was the norm. They trained and empowered midwives to
deliver women at home and manage complications including destructive
operations when indicated.
The International Safe Motherhood Initiative was launched in Nairobi in
1987. Although the target at that time was to reduce maternal mortality
47
Safe Motherhood: 2005 - 2008
ratio by 50% by the year 2000, the situation in many developing countries
today is actually worse.
Objective:
The aim of this paper is to trace the course of safe motherhood initiative
from Nairobi 1987, through Cairo 1994 and Beijing 1995, Colombo in
1997, to the Millennium Summit 2000 and beyond.
Outcome:
Review of evidence shows that it is possible for poor countries to
significantly reduce maternal mortality while relatively wealthier
neighbours remain behind. Examples of Sri Lanka, Malaysia, China, Cuba
and others will be described. Interventions that work include goal
oriented focused antenatal care, the presence skilled attendant at every
birth at home or in the facility, access to emergency obstetric care facilities
in case of complications, use of magnesium sulphate for eclampsia and
severe pre-eclampsia, as well as effectively addressing unwanted
pregnancy and unsafe abortion.
Conclusion:
Commitment at all levels and appropriate prioritization of use of
resources are more important in achievement of safe motherhood than
per capita income per se. Resources should be used to implement
evidence based interventions.
Perceptions and Practices of Vaginal birth after Cesarean among
Privately practicing Obstetricians in Kenya.
Author:
*R. Koigi-Kamau, Senior Lecturer, Department of Obstetrics and
Gynecology, College of Health Sciences, University of Nairobi, P.O. Box
19676. Nairobi.
Source:
P.K. Leting. Registrar, Department of Obstetrics and Gynecology, College
of Health Sciences, University of Nairobi, P.O. Box 19676, Nairobi. J.N.
Kiarie, Consultant Obstetrician-Gynecologist, Kenyatta National
Hospital, P.O. Box 19676, Nairobi.
Abstract:
Objective:
To determine perceptions, preferences and practices of vaginal birth after
cesarean.
Design:
Cross-sectional descriptive study
48
Safe Motherhood: 2005 - 2008
Setting:
Private clinics of obstetricians in five major towns of Kenya
Subjects:
Obstetricians in private practice
Main outcome measures:
Practice and experiences in trial of labor (TOL); need for, and application
of, selection criteria in TOL; perceptions on outcomes of TOL and patient
preference; perception on trends of vaginal birth after cesarean (VBAC)
and need for policy on TOL.
Results:
Nearly all respondents (98.4%) believed in the need for, and application
of, selection criteria for allowing TOL. However, only 23% believed in
routine screening with radiological pelvimetry, while 63.2% believed in
routine fetal weight estimation. All obstetricians (100%) have ever
managed TOL in private practice, and 74% had managed at least one case
in the last 6 months. Despite lack of tangible selection criteria, the 83.1 %
think that most women prefer TOL while 95.1% discourage it if perceived
as inappropriate. Failure rate of TOL was perceived to be more than 50%
by 35.2% of the respondents. A majority of the respondents (about 75%)
would prefer TOL on themselves or their spouses. Those who perceived
that there was a falling trend of VBAC were 58%, citing increased
demand by mothers (45.7%), obstetricians’ convenience (40.0%) and fear
of litigation (26.8%) as the reasons for this observation. A fluid policy of
“TOL whenever it is deemed as appropriate” was preferred by 88.7%.
Conclusion:
The perception of obstetricians is that desire for VBAC predominates over
elective repeat cesarean. However, consensus on appropriate selection
criteria is lacking, which leaves the obstetrician in a management
dilemma. Hence, there is need to study outcomes of both ERC and TOL
in order to come out with objective policy guidelines on management of
one previous cesarean in pregnancy
Antenatal care in the 21st century.
Author:
Dr Zahida Qureshi
Source:
Dept. Of Obs/Gynae University of Nairobi P.O.Box
19676-00202 Nairobi. zqureshi@nbnet.co.ke
Abstract:
The traditional antenatal care originated from models developed in
Europe in the early 20th Century, was ritualistic and emphasis was placed
49
Safe Motherhood: 2005 - 2008
on frequency and numbers rather than on essential goal-directed
elements.
The risk approach adopted as a way of identifying which women are
most likely to develop serious complications has been shown to have
only limited effectiveness: most women who go on to develop life
threatening complications had no apparent risk factors: conversely those
identified as being at risk generally end up with uneventful deliveries .
What is the way forward to Antenatal care in this century? Reduced
number of goal oriented, individualized visits-the evidence of this New
Model of care is presented.
The 2003 KDHS findings of antenatal care in the country are presented
and a brief of the Ministry of Health’s implementation of the “focused
antenatal care” in conjunction with partners –the challenges are
discussed.
Increasing access to Skilled attendant through Community
Midwifery.
Author:
Annie Mwangi, Prof J.Karanja, Charlotte Warren
Source:
Population council, P O Box 17643, Nairobi
Abstract:
Background:
Concerned about high maternal mortality, the International Community
launched the Safe Motherhood Initiative in Nairobi in 1987. The target at
the end that conference was that countries reduced maternal mortality
ratios by 50% by the “magical” year 2000. During the Millennium Summit
2000, it was realized that the maternal morality situation in many
countries was actually worse. Here in Kenya the ratio had increased from
320 to 590 per 100,000 livebirths. The target for the Millennium
Development Goal is to reduce the ration year 75% by the year 2015.
Objective:
The goal of the Community Midwifery initiative (home based midwifery)
in Western Province of Kenya is to contribute to the achievement of the
Millennium Development Goal of reducing maternal and perinatal
mortality in Kenya.
Methods:
Details of the process of this project were reported in KOGS 2005. This
paper will be an update of the progress made so far.
50
Safe Motherhood: 2005 - 2008
Results:
The initial recruitment target was 40 retired or resigned midwives. 34
were trained and are still involved. All of them successfully completed
their update training including conducting 10 deliveries in a facility
under supervision. Thereafter they have conducted deliveries at homes
(0-32, total for the group:
), and referrals 0-4 each, a total of 54). 23
(74%) have forwarded their reports monthly, 3 (9.7%) fortnightly, while 5
(16%) Monitoring and evaluations visits have revealed strong support
from the communities, the provincial administration, and from the health
facilities.
Opportunities and Challenges:
The project has a lot of goodwill from the stakeholders but there are some
challenges too. There is poor payment for service from the community
therefore threatening sustainability. There are also areas where TBAs
strongly oppose the community midwives. There is also insecurity.
Recommendations:
Despite the teething problems the initiative has great potential in making
motherhood safe and it should be supported and scaled up by all the
stakeholders
The Quality of Ante-natal care in respect to Anaemia Assessment
among women delivering at Pumwani Maternity Hospital in
Nairobi Kenya.
Author:
Dr Shiphrah Kuria, P O Box 186 00202 KNH, Email:
shiphonk@yahoo.com
Abstract:
Objectives:
1) To document the proportion of women attending ANC who were
screened for
anaemia.
2) To document the prevalence of anaemia in pregnancy in the study
population.
3) Evaluate the proportion of anaemic women treated for anaemia.
4) To document the social demographic characteristics of the mothers
with anaemia.
The Results:
Of 312 women recruited into the study, 35% of them did not have their
haemoglobin estimation done by the time of delivery. Of the 65% who
had their haemoglobin estimation done, 9.4% were found to be anaemic.
As many as 23% of the mothers were below 20 years of age. For the
women found to be anaemic, one fifth (21%) of them no action was taken,
51
Safe Motherhood: 2005 - 2008
for three quarters (74%) haematinics were given and 5% were given
antihelminthes empirically but no haematinics. Only one fifth (21%) of
these women had a repeat Hb estimation done
Conclusion:
The quality of ANC in respect to anaemia is poor and needs
improvement.
Recommendations:
1. More effort needs to be put in the peripheral clinics for;
Good record keeping
Clinical examination
Laboratory testing
Intervention
2. There is need to determine factors affecting the testing for anaemia.
3. There is need for women to book ANC at an early gestation to allow for
Investigations and management of anaemia
The Vaginal and Anorectal occurrence of group b beta
streptococcus among term pregnant women in Moi Teaching and
Referral Hospital (MTRH), Eldoret.
Authors:
Were E. * Esamai F.*Liechty E. ** Lemons J. **Fuller D. **
Source:
Faculty of Health Sciences, Moi University, Eldoret Indiana University
School of Medicine Correspondences to Were E, P. O. Box 4606 Eldoret
30100, Email:ewere@africaonline.co.ke
Abstract:
Objective:
To determine the proportion of term women seen at the MTRH maternity
who have laboratory evidence of colonization by GBBS.
Design:
Prospective cross-sectional study.
Setting:
Low Risk Antenatal Clinic and Labor Ward, Moi Teaching and Referral
Hospital, Eldoret. February 2002.
Subjects and Methods:
A convenience sample of 89 pregnant women of gestation 38 weeks or
more and intact fetal membranes were studied. Women consenting had
vaginal and anorectal swabs taken. The swabs were transported in a
medium selective for Group B beta hemolytic streptococcus (GBBS). This
was then incubated for 12 – 24 hours at 35 – 37 degrees Celcius. After
52
Safe Motherhood: 2005 - 2008
incubation the culture was analyzed for the presence of GBBS DNA
alongside a control laboratory sample of GBBS. The data was analyzed
using Epi Info Version 3.3.2 and presented in simple tables.
Results:
Of the 89 women studied 34.7 % were term antenatal women. The rest
65.3% were gravidas in labor at term. 20.2 % (95% CI 12.4 - 30.1) of the
vaginal samples had positive smears for GBBS while 34.1 % (95% CI 24.3
– 45) of the anorectal smears were GBBS positive. Positive smears were
obtained in both canals simultaneously in 11.4% (95% CI 5.6 – 19.9) of
cases. There was no significant relationship between GBBS occurrence
and age, gestation, parity, marital status last coital contact and last
vaginal examination
Conclusion:
Occurrence of GBBS the vaginal and or anorectal canals in term women
seen at MTRH maternity unit appears frequent. Implications for maternal
and neonatal health are discussed.
Increasing Access of FAMC/MIP Service in Kenya; the lessons
learnt.
Author:
Dr. J. Kibaru Head Division of reproductive Health P O Box 43319
Nairobi
Abstract:
Objectives:
1. To review the MOH implementation strategies and share the lessons
learnt implementing FANC/MIP.
2. To identify the factors contributing to uptake FANC/MIP services in
Kenya.
3. To propose possible interventions to address factors identified.
Results:
Since 2001, 45 out of the 78 districts in the country have implemented the
FANC/MIP policy. MOH aims at achieving 60% of pregnant women
receiving first IPT dose and 30%of pregnant women receiving second
dose of IPT by the year 2006. Reports from the implementing districts
show uptake of IPT of more than 70%. The KDHS, 2003 shows the IPT
uptake 4%.
Conclusions:
This implementation consists of a number of activities/strategies both at
the national and the district levels. FANC/MIP implementation depends
on a number of factors and key among them is the collaboration of
various stakeholders
53
Safe Motherhood: 2005 - 2008
Evaluation of the predictive ability of Angiogenic factors for
preeclampsia.
Author:
Mr. Evan Sequeira, Clinical Director and Senior Consultant, Department
of Obstetrics and Gynaecology, Aga Khan University Hospital
Source:
Is a multicentric prospective observational study in collaboration with
World Health Organization (WHO)
Abstract:
Summary:
The WHO in collaboration with Harvard University and University of
Chicago is conducting a 2 ½ year study in 6 countries including Kenya,
India, Thailand, Spain, Argentina and Columbia.
The aim of the study is to determine the predictive ability of angiogenic
factors in preeclampsia. Aga Khan University Hospital is one of the 6
centers involved in the study.
Preeclampsia occurs in 5-7% of all pregnancies with a 3-25 fold increase in
maternal and foetal complications.
The objective of the study is to be able to predict preeclampsia 5-6 weeks
before it occurs.
Cost effective urine dip stick kits will then be made available for future
use in the developing world.
Strategies to prevent and treat Preeclampsia.
Author:
Dr Norman K. Njogu. S.H.O. Aga Khan University Hospital.
Abstract:
Preeclampsia is a major cause of morbidity and mortality in mothers,
fetuses and neonates worldwide. The cause of preeclampsia is uncertain
and many controversies exist concerning its prevention and management.
The World Health Organization (WHO) is coordinating a series of
systematic reviews that focus on the etiology and the best strategies for
the screening, prevention and treatment of preeclampsia. There appears
to be no benefits in treating mild preeclampsia. Severe hypertension
requires drug therapy while magnesium sulphate is effective in treating
and preventing eclampsia. Calcium supplementation and antioxidant
therapy have some role in prevention of preeclampsia.
54
Safe Motherhood: 2005 - 2008
Make every Mother and Child count: The case for preventing
postpartum hemorrhage.
Authors:
Dr Zahida Qureshi,
Source :
Dept. Of Obs/Gynae, University of Nairobi. P.O. Box 19676-00202
Nairobi zqureshi@nbnet.co.ke
Abstract:
The Safe Motherhood Initiative launched in Nairobi in 1987 hoped to
reduce maternal mortality by 50% by the year 2000, and in 2006 in most
countries in sub-Saharan Africa Maternal mortality is increasing. All
these countries are now bound by the Millennium declaration –and are
now aiming to achieve a reduction of maternal mortality by 75% between
1990 and 2015.
Over 500,000 maternal deaths occur yearly the world over, 99% of these
women are in the developing world and 25-60% of these deaths are due
to PPH Epidemiology and the approaches to reducing Maternal
Morbidity and Mortality from Postpartum Haemorrhage (PPH) are
reviewed such as use of uterotonics and the active management of third
stage of labour.
Over half of births occur in the absence of a skilled person –thus being
denied the opportunity of active management of third stage of labour –
results of community based trial –using home based care with use of
Misoprostol for reduction of PPH is also reviewed.
Strategies are needed such as scaling up Active Management of Third
Stage of Labour (AMSTAL) and introduction /registration of newer
medications such as Misoprostol –How do we tackle these challenges?
The role of The Kenya Obstetrics and Gynaecology Society in wide
dissemination of the FIGO/ICM Global Initiative for the Prevention of
Post Partum Haemorrhage and advocacy for registration of Misoprostol
is discussed
The Rising Caesarian section rates: Always a cause for concern?
Author:
Dr. Wanyonyi Sikolia1 Mr. Evan Sequeira2 Dr.Timona Obura3
Source:
Aga Khan University Hospital: Box 30270-00100, Nairobi.
55
Safe Motherhood: 2005 - 2008
Abstract:
Background:
There has been a persistent rise in the rate of caesarian sections over the
years. Whether this rise is the cause of the decline in infant mortality and
improved neonatal outcome still remains debatable.
Objective:
To determine the caesarian section rate and the perinatal outcome at the
Aga Khan University hospital between 2001 and 2004.
Design:
A hospital-based cross sectional study.
Setting:
The Aga Khan University Hospital, Nairobi
Methods:
A retrospective audit was done for all deliveries and the perinatal
outcome for the year 2001 and 2004.
Main outcome measures
The total caesarian section rates, their indication and the perinatal
outcome.
Results:
The overall caesarian section rate was 20.4% in 1996, 25.9% in 2001 and
38.1% in 2004. The rate among patients managed by their private
obstetricians was 27.1% in 1996, 30.8% in 2001 and 41.7% in 2004. Whilst
among general patients, it was 14.7%, 21.5% and 34.5% over the same
period. The main indication for Emergency Caesarian Section was fetal
distress, and for Elective caesarian section was a previous uterine scar.
The overall perinatal mortality rate improved from 25.2 per 1,000
deliveries in 2001 to 14.0 per 1,000 deliveries in 2004. The early neonatal
mortality rate (for deaths occurring while the neonate is still within the
hospital) also improved from 12.8 per 1, 000 deliveries in 2001 to 10.8 per
1, 000 deliveries.
Conclusion:
There has been a significant increase in caesarian section rate over the
years. Being a referral unit dealing with many high-risk patients some of
whom are supervised elsewhere, and with a significant ratio of private
patients, the high rates at The Aga Khan University Hospital are
expected. The rise could also be due to early detection of fetal
compromise and improved diagnostic facilities leading to timely
intervention. Despite the high cesarean section rates there is a significant
drop in perinatal mortality and early neonatal mortality rate at the
hospital. This calls for a renewed debate on the subject to compare
56
Safe Motherhood: 2005 - 2008
outcome from other centers, as the rising caesarean section rate may not
always be a major cause for concern.
Anaphylactic reaction to Extra Amniotic Prostaglandins on
induction of Labour.
Author:
Dr. Omondi-Ogutu, Chairman KOGS P O Box 19450-00202 Nairobi.
Abstract:
Background:
Anaphylactic reaction to prostaglandin is a known but rear complication
of extra amnoitic and intra amnoitic prostaglandin use. It maybe difficult
to predict those who may have the reaction. When it occurs immediate
discontinuation of the procedure, use of steroids and oxygen use and
need for ICU support maybe necessary. There is therefore a need for
clinicians to watch out for this reaction when using the drug.
Case:
This was a 34 year old lady who was admitted with a history of a sever
congenital abnormality at 14 weeks for termination of pregnancy. On
admission all the parameters were normal. Extra amniotic prostaglandin
was instilled starting with 4Mls having been diluted as 10mg in 18mls of
normal saline. With instillation of the first 3mls the patient started
sweating complaining of dizziness tightness of the chest, and vomiting
with immediate disorientation. The drug was immediately stopped and
resuscitation done with the ICU team of the hospital. After 30 min the
condition improved and the patient recovered. Induction was continued
with plain catheter and syntocinon. She eventually expelled the fetus and
was discharged home 3 days later
Conclusion:
This case is presented for the health workers to know the risks involved
in the use of prostaglandins.
Severe Meconium Aspiration syndrome: Case report.
Author:
R Koigi-Kamau and E.C. Kungu
Source:
R. Koigi-Kamau, MBChB, MMed (O/G). Senior Lecturer, Department of
Obstetrics and Gynecology, College of Health Sciences, University of
Nairobi, P.O. 19676 – 00202, Nairobi, Kenya. Also Chairman, Division of
Obstetrics & Gynecology, The Nairobi Hospital, Nairobi, Kenya. EC
Kungu, MBChB, MMed (Pediatrics), Neonatology (MacGill). Consultant
pediatrician and neonatologist, The Nairobi Hospital, P.O. Box 52545 –
00200, Nairobi, Kenya.
57
Safe Motherhood: 2005 - 2008
Abstract:
Summary:
This is a case report on severe meconium aspiration syndrome (MAS) that
resulted in early neonatal death. The mother had presented to the
principal author for booking at the Nairobi Hospital at 32 weeks of
gestation. Antenatal care was provided at an NGO clinic. First stage of
labour was rapid and lasted for only 2hours and 45 minutes. There were
no fetal heart rate abnormalities that were noted during the first stage of
labour. Artificial rupture of membranes was done in second stage of
labour. There was no liquor amnii seen but scanty thick old meconium
was noted. Delivery was easy but the baby’s skin and nails, and the
vernix were deeply stained yellow with old meconium. Resuscitation
included suction through direct laryngoscopy, naso-tracheal intubation
with pulmonary toilet, as well as administration of 100% oxygen. The
condition of the baby did not improve. A diagnosis of severe MAS with
haemorrhagic ischaemic encephalopathy (HIE), persistent pulmonary
hypertension, persistent foetal circulation syndrome (PFCS) and
meconium chemical pneumonitis was made. The baby was admitted to
the intensive care unit (ICU) for assisted ventilation and critical care. The
condition of the baby continued to deteriorate and demise occurred 18
hours after birth.
The purpose of this case report is to discuss and review literature on MAS
in order to provide further insight on the understanding of the
mechanisms of meconium production in utero, meconium-associated
pathophysiological processes, impact of intrauterine meconium release
on pregnancy outcome, as well as management challenges.
Pain relief in Labour- A new approach.
Source:
polang@wananchi.com
Abstract:
Introduction:
The pain of childbirth is the worst pain that most women will ever
experience in their entire lives.
Spinals and Epidurals are the most effective and reliable means of pain
relief during childbirth.
Many mothers-to-be are concerned about the safety of these pain relief
techniques.
There are many frightening stories about anesthesia, most of which are
baseless.
58
Safe Motherhood: 2005 - 2008
Women attending childbirth education classes report that some
instructors put a negative spin on spinals and epidurals, dismissing them
as ‘unnatural’ or even harmful interventions.
Women sometimes refrain from asking for pain medication out of
concern that it will be harmful to their babies.
It is important to note that when an epidural is chosen for labour and
delivery, the procedure should be performed as soon as it is established
that the patient is in labour. Unfortunately, most patients receive the
epidural after their pain becomes unbearable.
Relationship between Cervical dilation at initial presentation in
Labour and subsequent intervention at Kenyattta National
Hospital, labour ward.
Author:
Dr. Aruasa/Dr. Wanyoike G.
Source:
Kenyatta National Hospital, P.O. Box 19676, Nairobi.
Abstract:
Objectives:
The aim of the study was to assess the relationship between cervical
dilation at which parturients presented in labour and subsequent
interventions. It also aimed at determining the maternal and fetal
outcomes of mothers presenting early in labour (latent phase) and those
presenting late in labour(active phase).
Design:
This was a prospective comparative study
Setting:
Kenyatta National Hospital, Nairobi.
Population:
200 parturients who met the entry criteria from 12th August 2004 to 31st
October 2004.
Methods:
A total of 200 parturients presenting to Kenyatta National Hospital in
latent and active phases of first stage of labour between 12th August and
31st October 2004 were identified after meeting the study’s criteria.
Systematic sampling was used and 2 sets of parturients recruited: 100 in
latent and 100 in active groups, depending on their cervical dilatation at
first assessment. They were followed up in time and data collected using
a precoded questionnaire.
59
Safe Motherhood: 2005 - 2008
Main outcome measures:
The primary outcome was the rate of caesarean section. Secondary
outcomes were the number of vaginal examinations carried out, labour
augmentation with oxytocin, use of obstetric analgesia, episiotomy rates,
length of labour, fetal birth weight, one-and five minute Apgar scores,
primary postpartum haemorrhage and early puerperal sepsis.
Results:
The number of vaginal examinations was high in those presenting at 03cm group >3 in 41% vs >3 in 10% in 4-10cm, p-value < 0.001, which is
significant.
There was significantly greater oxytocin use rate in women presenting
earlier in labour. Primigravidas at 0-3cm 62.7 % vs 33.9 % in 4-10cm, pvalue 0.002; multipara at 0-3cm 68.3 % vs 34.1 % in 4-10cm, p-value 0.001
which were significant.
Obstetric analgesia (opiates) use showed a significant difference in
primigravidas, 0-3cm 49.2 % vs 29.8 % in 4-10cm, p-value 0.01. However,
among multipara, there was no significant difference ;0-3cm 29.3 % vs 25
% in 4-10cm, p-value 0.6.
The likelihood of caesarean section increased with increasing cervical
dilatation at presentation. However, the increase was not significant
when analyzed according to parity. Primigravidas presenting at 0-3cm
22% vs 32.1% in 4-10cm (p-value 0.2). Multiparous women presenting at
0-3cm 12.2% vs 27.3% in 4-10cm (p-value 0.08).
The proportion of labour at home was significantly longer in those
presenting in active phase of labour irrespective of parity (for
primigravid 33.8% 0-3cm vs 50% in 4-10cm(p= 0.0002) and multiparous
34.2% vs 59.4% in 4-10cm(p=0.02).
Fetal vital status at birth were similar in the 2 groups (fetus alive in 96%
of both groups).Apgar score at 1 minute was < 7 in 24% in 0-3cm vs 8.3%
in 4-10cm , p-value 0.003. However, at 5 mins it was not significantly
different in the 2 groups, 8% vs 6.8% respectively, p-value 0.3.
Conclusions:
Women who present to hospital at 0-3cm spent less time in labour before
presentation and were less likely to have a caesarean section compared to
those presenting in advanced labour. However, other obstetric
interventions like labour augmentation with oxytocin and use of obstetric
analgesia were significantly more likely to be carried out in women who
presented to hospital at 0-3cm than in those presenting in advanced
labour.
60
Safe Motherhood: 2005 - 2008
Recommendations:
Admission to labour ward of patients in early labour (0-3cm) can
be delayed since this does not significantly alter immediate foetal
outcome as assessed by foetal Apgar score at 5 minutes. There was
also no significant increase of caesarean section rates due to
delayed admissions. Instead patients in early labour can safely be
admitted to the lying-in (antenatal) wards.
An optimal level of labour interventions such as oxytocin
augmentation of labour need to be determined through further
studies.
The factors which cause women to seek early admission in labour
ward are an important area of study.
IBP case study: Using best practices to reduce maternal mortality in
seven districts of Kenya.
Author:
Josephine Kibaru*, Maureen Kuyoh**, Violet Bukusi**
Source:
Division of Reproductive Health – Ministry of Health, Kenya, Family
Health International
Abstract:
Introduction:
The Kenya Country team was formed under the Implementing Best
Practices Initiative of WHO and consortium partners under the Ministry
of Health (MOH) leadership. The team attended the IBP Africa Launch
meeting held in Entebbe, Uganda in June 2004. Following the meeting,
the team developed an action plan to reduce maternal mortality in seven
selected districts in Kenya within eighteen months by increasing family
planning uptake through advocacy, training, and logistics management.
Methods:
An IBP task force was formed by the Division of Reproductive Health
(DRH), MOH that brought together reproductive health (RH)
stakeholders working in Kenya. The role of the task force was to advise
the DRH on the latest evidence-based and other demonstrated practices
that improve the quality and delivery of RH Services; help to identify and
facilitate synergies among all RH agencies working in the country;
provide a network operating at country level to promote harmonized
approaches and share experiences, tools and lessons learned; advocate to
the policy makers to re-position RH; facilitate efforts to ensure that RH
evidence-based standards, norms, guidelines and proven practices get
relayed into the hands of policy makers, program managers, and
providers; advise the DRH on how to facilitate the documentation,
review and sharing of effective practices that have proven successful in
other countries; identify and mobilize resources to support the initiative
61
Safe Motherhood: 2005 - 2008
including a budget line and; ensure monitoring and evaluation of the
initiative through quarterly meetings and data collection. The task force
met quarterly to review IBP Kenya performance goal implementation.
Family Health International facilitated the IBP task force activities in
Kenya. This task force has since been amalgamated into the FP working
group which also meets quarterly. Components of the IBP performance
goal are being implemented by three sub-committees namely advocacy,
training and logistics management. These are led by MOH personnel and
partner organizations who are members of the FP working group.
Results:
During the past year, the team has made significant progress. Notable
accomplishments include: securing a line item for RH commodities in the
national health budget; forming a caucus for family planning among
members of parliament; hosting a meeting with budget managers from
different government sectors to identify opportunities for a multi-sectoral
approach in financing FP activities; developing advocacy briefs and
posters; developing a training module for service providers on
contraceptive technology, infection prevention, counseling, and
facilitative supervision and conducting training and facilitative
supervision: developing materials including radio spots, posters and
simple client pamphlets to create demand for family planning. The team
plans to host exploratory community forums, compile data on
contraceptive stock and availability and collect data to measure the effect
of this intervention.
Conclusions:
The main lessons learned in this process were that Ministry of Health
leadership and support of stakeholders and funding agencies are a critical
component for success. Logistics management remains a challenge.
More lessons learnt from this process will inform future activities of the
Kenya Country Team as well as implementation of action plans in other
countries where the IBP concept has been and will be launched.
Using Global policy documents to increase women’s access to safe
abortion services in select countries in Africa.
Author:
Dr. Josephine Moyo, Dr. Brookman-Amissah, Leila Hessini, Nina
Kavuma
Source:
Ipas Africa Alliance, FAWE House, 1st Floor Chania Avenue. P.O Box
1192 00200 Nairobi – Kenya. Tel: 3877239/3870248
62
Safe Motherhood: 2005 - 2008
Abstract:
Background:
In recent decades, international understanding of the basic civil, social
and economic rights with which all people are born has deepened and
been progressively articulated in international covenants, treaties and
regional policy instruments. Such agreements create a solid basis for real
improvement in people’s lives, as ratifying nations commit themselves to
uphold the rights enumerated therein, including adjusting laws and
policies.
To assist health systems and policy makers in translating these policy
agreements into action, the World Health Organization (WHO) issued a
Safe Abortion: Technical and Policy Guidance for Health Systems in 2003.
Ipas Africa Alliance and key regional and national institutions have been
instrumental in disseminating the guidance, promoting its use by
national health systems, and encouraging policy makers and health
professionals to ensure that elective abortion services are available to the
fullest extent of the law in Africa.
Objectives:
This research documents and analyzes the role of international
documents and treaties in providing a conceptual and practical
framework for ensuring that African women have access to safe, quality
abortion services, supportive policies, and an enabling environment.
Measures:
In researching the problem, information was gathered through:
Telephone interviews
Literature review of popline and medline
Conclusion:
Global policy has affected regional policies in Africa as witnessed in the
decision of the African Union to support women’s rights to abortions
under certain circumstances in its chapter. While generalizations are
difficult given the great diversity in the countries included, the research
showed that access to safe abortion services have increased in the
majority of African countries surveyed although restrictive laws and
policies continue to serve as a barrier to women’s access to abortion
services in some
Recommendations:
National Governments have a number of options and opportunities to
reduce maternal mortality in Africa by addressing unsafe abortion as a
result of recent treaties and charters by international bodies such as the
African Union, WHO and the ICPD Conferences. Considering that every
country in the region has at least one legal indication for elective abortion,
the following are among the options:
63
Safe Motherhood: 2005 - 2008
i.
There are opportunities that have been created by the pronouncement
and coming into force of the Protocol on Women’s rights by the
African Union in November 2005 for governments to implement the
protocol and authorize elective abortion in cases of sexual assault,
rape, incest, and where the continued pregnancy endangers the
mental and physical health of the mother or the life of the mother or
the unborn child.
ii. In circumstances where abortion is not against the law, health systems
should train and equip health-service providers and should take other
measures to ensure that [legal] abortion is safe and accessible.
Additional measures should be taken to safeguard women’s health.(ICPD+5)
iii. Review and reform the abortion laws and policies where they are
restrictive.
iv. Develop barrier-free standards and guidelines compatible with the
existing or reformed abortion laws and policies. (WHO, 2003).
v. Authorize additional providers in the form of mid-level providers
such as nurses, midwives, clinical officers and other relevant cadres to
provider post abortion and elective abortion care. (WHO, 2003).
vi. Register Misoprostol for reproductive health use and include it on the
national essential drug lists- (In July 2005, The WHO recommended
Misoprostol to be included in the essential drug list for Safe
Motherhood.)
vii. Expand Medical or medication and use of vacuum aspiration for
provision of Abortion in view of the following considerations:
National laws rarely specify procedures for abortion so there are
no legal barriers
Most laws do not specify who can perform abortions, so it can be
administered by a range of providers– e.g. In Ghana midwives
cannot dilate cervix but can ostensibly provide medical abortion?
Medication abortion allows women to be in charge of the abortion
process and can be used at the community level.
Professional responsibility in Maternal Mortality reduction in Subsaharan Africa: “thinking outside the box”.
Author:
V. M. Lema M.B;Ch.B. (Mak); M.Med.O/G (Nbi) Professor of Obstetrics
and Gynaecology,
Research and Evaluation Manager - IPPF-ARO,
Nairobi
Abstract:
The risk of death due to complications of pregnancy and childbirth is
highest in sub-Saharan Africa, at 1:16, compared to 1:2700 for the
developed regions of the world; 1:61 for the developing regions, and 1:74
globally.
64
Safe Motherhood: 2005 - 2008
Although the main causes of maternal deaths are largely the same
globally, there are inter- and intra-regional variations in the rank-order
and the proportions thereof. In SSA complications of unsafe abortion, an
easily avoidable condition, account for up to 30% of maternal deaths.
Prolonged/obstructed labour which may predispose to deaths through
hemorrhage, sepsis, and ruptured uterus, a thing of the past in the
developed and some developing countries is responsible for a
considerable proportion of these deaths. There are concerns that the
recent increases in MMR’s in some of our countries are partly due to the
HI/AIDS epidemic which has particularly hit SSA as well, accounting for
up to 20% in some countries.
The major determinants of maternal deaths are well known and so too are
effective strategies for reducing them, which have been shown to be
effective even in some developing countries such as Sri Lanka. In all
instances where maternal mortality has declined significantly
professionals, i.e. obstetricians and gynaecologists have taken the lead.
They have been accountable and hold others accountable too. In this they
have had to get out of their usual confines, i.e. health facilities to the
communities and public domains.
Sadly in many of our countries professionals have continued to operate
within their confines, i.e. hospitals and private practices. We have not
taken advantage of the massive good will from the international
community and available knowledge as well as our comparative social
positioning within our communities to become accountable and hold
others accountable. We have not responded to the cries of the many
women and their families who die in our hands or facilities.
Factors predisposing to maternal deaths and their preventive strategies
are cross-cutting and multi-sectoral in nature. They can not be addressed
within the box. We therefore need to not only think but work outside the
box if we are to make significant inroads in reducing the high and
unnecessary maternal deaths in sub-Saharan Africa. It is our professional
responsibility, an ethical and moral calling.
Repositioning Post partum care in Kenya: Lessons learnt.
Authors:
Charlotte Warren, Anne Mwangi
Source:
Institution: Population Council
Abstract:
Background:
Despite the fact that around forty five percent of maternal deaths occur
within the first 24 hours after childbirth, and over sixty five percent of
maternal deaths occur during the first week of the postpartum period,
65
Safe Motherhood: 2005 - 2008
health care providers continue to advise on a first check up at 6 weeks
after childbirth. This period is also critical to newborn survival with
between 50 to 70% of life threatening newborn illnesses occurring in the
first week. Yet most strategies to reduce maternal and perinatal morbidity
and mortality have focused on pregnancy and birth (e.g. comprehensive
antenatal care and skilled attendance at birth). There is limited record of
any postpartum care visits in health facilities.
Purpose:
To improve the provision of early postpartum care for both women and
newborns to contribute towards a reduction in maternal and perinatal
morbidity and mortality.
Methodology:
In an attempt to address this gap in service delivery a workshop was held
to have consensus on timing of postnatal visits. A series of meetings were
held to agree on the content of visits, and subsequent development of
postpartum care register. Population Council in conjunction with the
Ministry of Health (MOH) and other stakeholders defined three postnatal
visits to provide minimal services a mother and her baby should receive
from a skilled attendant after birth. For the mother three consultations are
recommended within 48 hours, within the first two weeks and again at, 6
weeks. Registers were subsequently developed and piloted prior to
printing and distribution. Health care providers were trained on how to
fill the register and on other aspects of providing postpartum care.
Results:
Where FANC and birth planning take place women are more likely to
give birth with, a skilled attendant and seek early postpartum care.
Following introduction of a new register and the re-orientation of health
care providers an increase in attendance by women attending postpartum
clinics increased from 7% at baseline to 28% at endline.
Conclusions:
Early Postpartum Care must be repositioned to complete the strategies
for the continuum of skilled care from pregnancy (Focused Antenatal
Care) Skilled Attendance at Birth and early Postpartum Care. The
development of a standardized postpartum register is one step towards
advocating for providing Early Postpartum Care among the health
service providers.
66
Safe Motherhood: 2005 - 2008
Adaptation of International Best practices: prospects and challenges for who
focused antenatal care in Kenya
Authors:
Harriet Birungi, W.Onyango Ouma. Ian Askew
Source:
FRONTIERS, Population Council and Institute of African Studies,
University of Nairobi
Abstract:
Introduction:
The risk of dying from pregnancy-related complication in Kenya is very
high. Problems of malaria, anemia, and STD/HIV/AIDS have
contributed to the high maternal mortality. However, ANC services that
are important in monitoring the progress of a pregnancy and identifying
complications for intervention at appropriate lime are not fully utilized
by most women. But even when women make an ANC visit they are
likely to receive poor quality of services that are not comprehensive. To
respond to the pressing reproductive health needs of antenatal clients as
when as to the service delivery problems, Kenya has adopted the WHO.
Goal oriented ANC (focused ANC) that recommends reducing the
number of clinic visits to four; strengthening detection, management and
prevention of health conditions likely to increase the risk of specific
adverse pregnancy outcomes; providing of therapeutic -interventions
known to be beneficial for pregnant women; and alerting pregnant
women to potential emergency situations and instructing them on
appropriate responses. The presentation describes what: Kenya’s MOH
has done to adapt the focused ANC. examines the extent to which
adaptation of the package increases coverage and quality of ANC services
and highlights some of the challenges of engaging focused,ANC in the
local context.
Methods:
The study was carried over a period of nine months, covering two
districts exposed to the WHO-goal oriented package and one district
practicing the traditional ANC approach. Data for the study were
gathered through a variety of methods including document reviews. Key
informant interviews (19) at national and district levels, 5 focus group
discussions, client-provider interactions (419), exit interviews, ANC card
reviews (1247), and provider interviews and facility assessment.
Results:
Implementation of the package has had much effect on integrating birth
planning and malaria prevention into ANC, but its effect on
counseling/detection of HIV/AIDS in pregnancy and use of family
planning post-partum has been very limited. None of the clients received
a full range of services recommended under the focused ANC schedule.
Timing, continuity and care by competent provider are critical elements
in focused ANC in Kenya, however; 25 percent of provider offering ANC
67
Safe Motherhood: 2005 - 2008
ha not received training; clients ANC utilization behavior remains
unchanged with only 9 percent of 344 making their first visit at < 16
weeks as recommended.
Conclusions:
Considerable effort has been made to adjust the content of the WHO
package to the local ANC problems. However, focused ANC still remains
disengaged from the local context because limited consultation of actors
at national and district level and fragmentation in program support.
Adaptation of the package faces problems of integration, limited
community awareness and lack of minimum infrastructure for
comprehensive approach to the delivery of ANC services. Embedding the
package to the Kenya context will require a balance between the purely
technical issues (content), consultation and organization/management or
ANC and the health care system in general.
The magnitude of abortion complications in Kenya. Gebreselassie
The magnitude of abortion.
Authors:
H.; Gallo, M. F.; Monyo, A., and Johnson, B. R.
Source:
Abstract:
BJOG. 2005 Sep; 11:12292(9) -35.
Objective:
To estimate and describe the magnitude of abortion complications
presenting at public hospitals in Kenya.
Design:
Cross-sectional descriptive study.
Setting:
Hospital-based. Population Records of all women presenting prior to 22
weeks of gestation with abortion-related complications at selected
hospitals during a three-week study period. All public tertiary and
provincial hospitals were included; stratified random sampling was
employed to select a subset of 54 district hospitals nationwide.
Methods:
Data collectors identified 809 patients with abortion complications on all
hospital wards and completed a standardised questionnaire for each by
extracting information from the patient's hospital record. Main
Outcome measures:
Incidence, aetiology, morbidity and mortality of abortion complications.
68
Safe Motherhood: 2005 - 2008
Results:
Most women (80%) presented with incomplete abortion. Approximately
34% of the women had reached the second trimester of pregnancy.
Adolescents (14-19 years old) accounted for approximately 16% of the
study sample. Manual vacuum aspiration was used to manage 80% of
first trimester cases. The projected annual number of women with
abortion complications admitted to public hospitals in Kenya is 20,893.
The case fatality rate was estimated to be 0.87% (95% CI 0.71-1.02%), so an
estimated 182 (95% CI 148-213) of these women die annually. The annual
incidence of incomplete abortion and other abortion-related
complications per 1000 women aged 15 to 49 years is projected to be 3.03.
Conclusions:
The high rate of abortion-related morbidity and mortality documented in
the study highlights the critical need to address the issue of unsafe
abortion in Kenya.
Hospital admissions resulting from unsafe abortion: estimates from 13
developing countries.
Author:
Singh, S.
Source:
Lancet. 2006 Nov 25; 368(9550):1887-92.
Abstract:
Background:
Complications from unsafe abortion are believed to account for the
largest proportion of hospital admissions for gynaecological services in
develoSourping countries. The WHO estimates that one in eight
pregnancy-related deaths result from unsafe abortions. The social stigma
and legal restrictions associated with abortion in many countries means
that data on the magnitude of this problem are scarce; this article
estimates the rate and numbers of hospital admissions resulting from
unsafe abortions in developing countries to help quantify the problem.
Methods:
National estimates of abortion-related hospital admissions in women
aged 15-44 years were compiled for 13 developing countries: Africa
(Egypt, Nigeria, and Uganda), Asia (Bangladesh, Pakistan, and the
Philippines), and Latin America and the Caribbean (Brazil, Chile,
Colombia, Dominican Republic, Guatemala, Mexico, and Peru). These
data were combined with supplementary data from five countries in subSaharan Africa (Burkina Faso, Ghana, Kenya, Nigeria, and South Africa)
to give estimates for the three world regions.
69
Safe Motherhood: 2005 - 2008
Findings:
The annual hospitalisation rate varies from a low of about 3 per 1000
women in Bangladesh to a high of about 15 per 1000 in Egypt and
Uganda. Nigeria, Pakistan, and the Philippines have rates of 4-7 per 1000,
and two countries in Latin America with recent data have rates of almost
9 per 1000. In the developing world as a whole, an estimated five million
women are admitted to hospital for treatment of complications from
induced abortions each year. This equates to an average rate of 5.7 per
1000 women per year in all developing regions, excluding China. By
comparison, in developed countries complications from abortion
procedures or hospitalisation are rare.
Interpretation:
These results help quantify the magnitude of the adverse health effects of
unsafe abortion in developing countries and highlight the need for
improved access to post-abortion care. The provision of abortion services
is changing to include the drug misoprostol and this could reduce the
severity of abortion complications and the number of women who are
hospitalised. Researchers will need to monitor these changes to provide
countries with up-to-date information on illness and death from unsafe
abortion. Improved contraceptive services are necessary to prevent
unintended pregnancy. However, increasing access to safe abortion
services is the most effective way of preventing the burden of unsafe
abortion, and remains a high priority for developing
Community Postabortion Care Project (COMMPAC) in Nakuru
District, Kenya.
Source:
Summary report, Phase I: July 2005 - September 2006.
Abstract:
The Nakuru Community Postabortion Care (COMMPAC) Project was
designed to use the same process for community engagement that was
used in Bolivia. To replicate the Bolivia experience, representatives from
the ACQUIRE Project and SWAK visited Bolivia to gain an
understanding of the use of the community action cycle and a facilitator's
guide for community self-diagnosis developed and used there. In Bolivia,
COMMPAC facilitated sessions that enabled community groups to use
the community action cycle as a process to bring the community together
around a specific issue related to PAC. Together, they took action,
evaluated their action, and moved on to a new issue, replicating the cycle
multiple times. In Kenya, the action cycle was completed once during
Phase I. In Phase II, the process will be replicated to help reinforce the
skills learned under Phase I. Phase I began in July 2005, ended in
September 2006, and covered the first four parts of the action cycle-1)
prepare to mobilize, 2) organize the community for action, 3) explore the
70
Safe Motherhood: 2005 - 2008
health issues and set priorities, and 4) plan together-with 16 community
groups, composed of 412 individuals, completing their action plans. Key
opinion leaders and other stakeholders were involved from the beginning
as a means of developing champions and to create an enabling
environment for PAC activities. (excerpt)
Abortion and Media Reporting in Kenya.
Author:
Kinaro J., PPFA Africa Regional Office, Kenya
Abstract:
Objective:
The review of media reporting in Kenya was carried out to examine how
abortion is viewed in Kenya and the implications in the implementation
of quality RH services.
Outcome measures:
Planned Parenthood Federation of America International carried out a
review of articles by two major daily newspapers in Kenya. The articles
reviewed were those between May 2004 and May 2005.
Results:
The messages disseminated through the media were varied between
legal, political, moral, health and women rights. Messages relating to
legal were 22, political 2, moral 14, health 3 and women rights 13.
Majority of the articles showed preference for the fetus (32) while the rest
(19) showed preference for the mother.
Conclusions:
The articles were not explicit in educating the public on what abortion is
nor did they discuss traditions relating to abortions. Health issues were
list among the indications of abortion despite empirical evidence that
unsafe abortion is one of the leading causes of death among women in
their reproductive age in Africa. If unsafe abortion is not addressed,
women will continue to be denied reproductive health services and those
from poor families will continue to die from a cause that is preventable.
Recommendations:
If the public is interested in averting deaths' of women resulting from
pregnancy related complications, then, reproductive health services must
be expanded to include unsafe abortion. Quality and comprehensive
reproductive health services and information should be more accessible
to all women who are sexually active to use when they need them. Men
should also be involved to support women in making their reproductive
health choices. The value of a mother's live should not be viewed as equal
to that of a fetus as this has implications to the family and the generations
to come.
71
Safe Motherhood: 2005 - 2008
More studies should be carried out on how different traditional
communities and segments of the population are dealing with the issue of
unwanted pregnancies. The medical professionals should work more
with the media in highlighting unsafe abortion as a public health issue
that requires urgent attention. No woman should be left to die from a
cause that is preventable and her health should be made paramount.
72