Selecting Donor Liver Grafts for Patients with Hepatocellular Cancer
advertisement

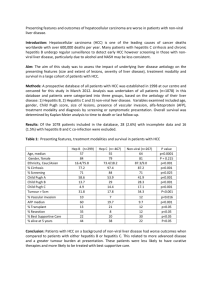
Selecting Donor Liver Grafts for Patients with Hepatocellular Cancer Michael L. Volk, MD, MSc Division of Gastroenterology and Hepatology University of Michigan, U.S.A. Alessandro Vitale, MD, PhD Hepatobiliary and Transplant Surgery Unit University of Padova, Italy Hepatocellular carcinoma (HCC) is the 5th most common malignancy in men and the 8th most common in women worldwide1. The incidence is rising in many countries, in part due to the aging cohort of patients infected with viral hepatitis, and in part due to earlier diagnosis. Correspondingly, survival rates are increasing as more patients are being diagnosed early enough to receive treatments such as liver transplantation2. Although this trend is a favorable one for patients with HCC, it poses a challenge for the already limited supply of organs. For example, in some transplant centers, patients with HCC now make up nearly half of those receiving a liver transplant. Many centers are thus attempting to expand the organ supply by more aggressive use of marginal organs. This review will focus on clinical decision making about donor organ selection for patients with HCC, particularly the use of organs at higher than average risk of graft failure. Liver transplantation as a treatment option for early HCC Initial experience with liver transplantation for HCC was disappointing, with many patients developing rapid tumor recurrence. Then, in 1996 Mazaferro et al3 showed that when patients were carefully selected, transplantation of early HCC was associated with a 75% survival after 4 years. This led to the development of the Milan criteria for transplant eligibility: a single lesion <5 cm or three lesions each <3 cm, without gross vascular invasion or metastatic disease. When these criteria are applied, post-transplant survival is similar to patients transplanted without HCC3. Survival benefit of liver transplantation is not uniform for all patients with early HCC In most countries, patients meeting the Milan criteria receive extra priority for transplantation, increasing their likelihood of receiving an organ beyond what they would receive on the basis of the severity of their liver disease. Organ allocation for HCC is thus conceptually very different than for non-malignant liver disease. In patients with nonmalignant disease, priority is given to the “sickest first” according to the Model for End-stage Liver Disease (MELD) score. This is justified because patients with higher MELD scores receive a larger survival benefit from liver transplantation4. In patients with HCC, priority is conversely given to the “earliest first” in that only those with early stage tumors are allowed access to transplantation. Unfortunately, most organ allocation systems do not differentiate within this group of early stage tumors, and all patients with early HCC receive the same priority for transplantation. However, the available data shows that survival benefit from liver transplantation for HCC is not uniform; rather it depends upon factors such as the patient’s age, tumor stage, and their response to alternative therapies5. This concept has recently been stressed in a study where the transplant survival benefit was correlated to the HCC stage as described by the Barcelona Clinic Liver Cancer (BCLC) classification6. In this study, it was shown that HCC patients in very early and early stages (BCLC stages 0 and A) had the lowest survival benefit after liver transplantation. These findings may reflect in part the fact that the BCLC classification accounts not only for tumor stage, but also the patient’s functional status and severity of liver disease – key factors in determining the availability of alternative therapies such as surgical resection, radiofrequency ablation (RFA), or trans-arterial chemo-embolization (TACE). Among patients with good response to loco-regional therapies, the short to medium-term survival may actually be worse with transplantation compared to no transplantation (Figure 1). For this reason, many authors recommend resection or RFA as a better initial treatment option for patients with small tumors and well-preserved synthetic function, and reserve transplantation as salvage therapy7,8. Thus, the existence of a varying survival benefit from liver transplantation among HCC patients is important to keep in mind when considering donor organ selection. The impact of donor organ quality All donor organs are not created equally. Some organs confer a higher risk of disease transmission, while others confer a higher risk of graft failure. Disease transmission includes rarely malignancy, and more commonly infection. The risk of infectious disease transmission with a particular organ can be estimated by donor behavior. Developed in 1994 by the United States Centers for Disease Control (CDC), the Public Health Service guidelines are shown in Table 1. This classification designates organ donors as ‘high risk’ if they meet any of the criteria for high-risk behaviors that present an increased chance of human immunodeficiency virus (HIV) transmission9. This designation is intended to alert and protect transplant candidates from the risks of infection, because even negative antibody testing of potential donors does not entirely eliminate the possibility of disease transmission. This is due to the window period between infection and serological conversion. Nevertheless, the actual risk of disease transmission is likely very low. Although limited by a voluntary reporting system, current estimates suggest the combined risk of transmission of HIV, hepatitis B or hepatitis C from a serologically negative donor is less than 1% overall, and less than 3% for CDC high risk donors10,11. For example, until recently a case of HIV transmission from solid organ transplantation had not been reported in the United States in more than 20 years. Furthermore, studies have shown that utilizing nucleic acid amplification testing during the screening process can further reduce the risk of disease transmission by up to 10-fold11. Numerically, the donor-derived risks of graft failure are much, much higher. This risk can be estimated by the Donor Risk Index (DRI), which combines factors such as donor age and mechanism of death to predict the risk of graft failure associated with a particular organ. These and other donor-derived risk factors for graft failure are shown in Table 2. Among organs currently transplanted, the 3-year risk of graft survival ranges from 81% with organs having DRI <1 to <65% with organs having DRI≥212. These donor factors have a similar impact on posttransplant survival among HCC patients. The DRI plays a larger role in patients with HCC than recipient factors such as tumor size, alpha-fetoprotein, and pre-transplant MELD score combined (Volk, unpublished data). Thus, the survival benefit of liver transplantation for patients with HCC depends heavily upon the quality of organ. Decision making about donor organs for patients with HCC Each time an organ becomes available, the physician and patient must decide whether to accept the offer or wait in hopes that a better one will come along. If the organ in question is of good quality, the decision is easy. However, the proper course of action becomes less certain when the organ carries higher than average risk. As mentioned above, “high risk” can be divided into two categories: risk of disease transmission and risk of graft failure. Given the low absolute risk of disease transmission, particularly in areas that utilize nucleic acid testing, we advise the majority of patients to accept CDC high risk organs. If the patient’s liver disease is sufficiently severe to accept a 10% risk of death in the first year after transplant, the <3% risk of getting a treatable disease is relatively minor by comparison. This includes organs from donors who are positive for hepatitis B core antibody, but negative for hepatitis B surface antigen. Recipients of these “core positive” organs have a virtually zero chance of de-novo hepatitis if treated lifelong with a newer generation oral antiviral beginning at day 1-2 after transplantation13. For organs with higher than average risk of graft failure, the physician must not only estimate risk based upon all the donor factors in Table 2, but also consider the patient’s risk of death or dropout while waiting for another organ offer. An additional consideration is whether there are any patient-specific factors that would make a given organ a particularly poor choice in that patient. For example, it is well recognized that donor age has a larger impact on patients with hepatitis C than other patients. However, aside from the obvious need to match physical size, these patient-donor interactions have a controversial impact on outcome. Some studies have shown that most donor risk factors are independent of recipient characteristics such as MELD score14. Other studies, conversely, suggest a higher prognostic impact of marginal livers in patients with higher MELD scores than in those with lower MELD scores15. In other words, the traditional dogma that less sick patients are “better able to tolerate high-risk organs” may not always represent the best guiding philosophy. Rather, when considering use of a marginal organ, the primary question should be: “Does this patient have a high short-term risk of waiting list mortality or dropout due to tumor progression?” If not, the use of a high-risk organ may not be justified. A final consideration from the perspective of the transplant system as a whole, is whether the post-transplant outcome will meet some acceptable minimal standard – often quoted as a 50% 5-year survival16. This minimum standard is justified on the basis of maintaining societal support for transplantation, as well as cost concerns. Some patients (e.g. those with advanced tumors and high MELD scores), may derive significant survival benefit from liver transplantation. However, the sum of multiple negative prognostic factors could determine very low post-transplant outcomes. The use of marginal grafts may have contributed to a dramatic decrease in posttransplant survival in some European counties that allocate organs using the MELD score 17. On the bases of these considerations, HCC patients with MELD scores less than 20, but high urgency for transplant (due to larger tumors and/or poor response to alternative therapies), are often considered optimal candidates for marginal organs in countries strictly adopting a MELD based allocation policy18. Split organs A theoretical concern specific to patients with HCC is whether the use of partial organs could increase risk of tumor recurrence secondary to growth factors released by hypertrophy of the transplanted lobe. This concern has been highlighted by evidence from the Adult-to-Adult Living donor Liver transplant (A2ALL) study showing higher rates of tumor recurrence among recipients of living donor liver transplant compared to deceased donor liver transplant 19. However, other studies20 have suggested that the published differences in the risk of posttransplant HCC recurrence between living and deceased donor liver transplantation are mainly due to a selection bias related to the effect of waiting time on tumor biology (dropout of aggressive tumors during the waiting list for deceased donor transplantation). Thus split organs should not be completely avoided in patients with HCC; rather this risk should be considered in the context of the overall organ quality and urgency of the patient’s need for liver transplantation. When to biopsy For logistical reasons, most transplant centers only perform liver biopsy on selected donor liver grafts. Indications for donor liver biopsy include a history of heavy alcohol use, moderately elevated liver enzymes, particularly bilirubin, and risk factors for a severely steatotic liver such as occurs in obesity and diabetes. In general, biopsy should be performed more often in older donors, since autopsy studies reveal cirrhosis – often unrecognized – in up to 5% of deceased individuals21. Additionally, donors livers with chronic hepatitis C (which should only be used in genotype 1 recipients) should always be biopsied, and the results used to determine acceptance. Operative considerations When using marginal organs (those at higher than average risk of graft failure), a multimodal strategy to improve the post-transplant outcome can be based on the following points: 1. While surgeons always strive for the lowest possible cold ischemia time, this is particularly important in cases where a marginal organ is being used. Routine liver biopsy is also helpful, and if possible should be done before procurement to limit the ischemia time22. 2. Some evidence suggests that the surgical technique for procurement may have an impact on the risk of post transplant initial liver dysfunction. In particular, a modified double perfusion technique (aortic and portal cooling with tourniquet clamping of spleno-mesenteric vein inflow) was shown to superior compared with the single aortic perfusion method23. 3. Emerging data on the pre-implantation management of donor organs suggests options in the near future to improve outcomes for marginal organs. For example, the use of machine perfusion show promise in early studies24. Summary In summary, liver transplantation is one of many important treatment options for patients with HCC. However, the benefit of transplantation depends on many things including the stage of the tumor, severity of liver dysfunction, response to alternative therapies, and quality of organ being considered. Organ-specific risks of disease transmission are relatively low, and while they should be discussed with the patient, the risks should play a minor role in clinical decision making. Organ-specific risks of graft failure, such as from older donors or those who suffered cardiac death are more important to consider. While each organ acceptance decision should be tailored to the individual patient, the best candidates for marginal organs tend to be those with larger tumors, poor response to loco-regional therapies, and MELD scores less than 20. In general, evidence suggests that the use of marginal organs should be avoided in patients with fully compensated cirrhosis and small tumors with good response to alternative therapies. Multiple Choice Questions: 1) Survival without transplant among patients with HCC is related to: D A. Tumor burden B. Liver function C. Functional status D. All of the above 2) Which of the following statements are true in patients with HCC? C A. Tumor recurrence after transplantation is influenced by body mass index B. Chemo-embolization increases the risk of metastasis C. Patient age affects transplant outcome D. Transplant survival benefit is best in patients with the smallest tumors 3) The risk of disease transmission: C A. Is increased in older donors B. Is very high regardless of the type of infection C. Is less than 3% for CDC high risk donors D. Is influenced by the type of preservation solution used 4) The risk of donor graft failure: B A. DRI does not have as much effect upon patients with HCC B. Post transplant outcome is influenced by DRI in HCC patients C. Organ quality is not as important in patients with HCC D. A DRI < 1 reduces post transplant survival 5) Transplantation in patients with HCC: D A. Should be avoided if the donor is a high CDC risk B. Should be performed using a high risk CDC organ only if the waiting list mortality risk is > 40% C. Should only be performed using organs from patients who are HBV core negative D. Can be safely done using organs from patients who are HBV core positive and surface antigen negative 6) Survival benefit is better when patients with lower MELD scores accept higher DRI organs: B A. T B. F 7) The use of partial organs in HCC patients: A A. May increase the risk of tumor recurrence B. Should be avoided C. Are associated with an increase in disease transmission D. Should only be used in patients with very small tumors 8) In patients with HCC: C A. Donor cold ischemic times can be longer without significant effect B. Routine donor liver biopsy is not helpful C. Modified double perfusion of the donor graft may improve organ function D. Only low DRI donors should be used 9) The benefit of liver transplant in patients with HCC is influenced by: D A. Stage of the HCC B. Severity of the recipient’s liver disease C. Quality of the donor organ D. All of the above 10) Waiting list mortality in patients with HCC: A A. Is influenced by the response to loco-regional therapy B. Depends more on tumor stage than MELD score C. Is lower than that of non-HCC patients D. There are fewer deaths on the wait list if patients with smaller tumors are transplanted Figure 1: Ratio between transplant(LT) and waiting list(WL)patient-year mortality rates by response to loco-regional therapy and TNM stage. Median follow-up was 10.4 months (3.1–79.2) for waiting list patients and 27.6 months (0.3–99.0) for LT patients. Adapted with permission from Cillo et al.5 Category MSM Description Men who have had sex with another man in the preceding 5 years IDU Persons who report nonmedical intravenous, intramuscular or subcutaneous injection of drugs in the preceding 5 years Hemophiliac Persons with hemophilia or related clotting disorders who have received human derived clotting factor concentrates Prostitution Men and women who have engaged in sex in exchange for money or drugs in the preceding 5 years High-risk sex Persons who have had sex in the preceding 12 months with any person described in items 1–4 above or with a person known or suspected to have HIV infection Exposure to HIV Persons who have been exposed in the preceding 12 months to known or suspected HIV-infected blood through percutaneous inoculation or through contact with an open wound, non-intact skin, or mucous membrane Jail Inmates of correctional systems (This exclusion is to address issues such as difficulties with informed consent and increased prevalence of HIV in this population) Table 1: Centers for Disease Control (CDC) criteria for donors at higher risk of disease transmission Risk factor Donor age Cold ischemia time (estimated based on distance) Steatosis Donation after Cardiac Death Cerebrovascular accident as cause of death Split organ Severe hemodynamic instability Moderately elevated liver enzymes Average value or threshold Mean age in U.S. is 41 years Mean time in U.S. is 7 hours Unknown – not all grafts biopsied. >40% steatosis considered higher risk Mean values in U.S.: AST – 86 ALT – 111 Total bilirubin – 1.1 >14 drinks/week Heavy alcohol use Severe atherosclerosis Table 2: Donor risk factors for graft failure. Components of the Donor Risk Index are in bold. This list does not include factors with minor impact on graft failure, or those whose causality has been inconsistently described. References 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 13. 14. 15. 16. 17. 18. Bosch FX, Ribes J, Diaz M, Cleries R. Primary liver cancer: worldwide incidence and trends. Gastroenterology. Nov 2004;127(5 Suppl 1):S5-S16. Altekruse SF, McGlynn KA, Reichman ME. Hepatocellular carcinoma incidence, mortality, and survival trends in the United States from 1975 to 2005. J Clin Oncol. Mar 20 2009;27(9):14851491. Mazzaferro V, Regalia E, Doci R, et al. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med. Mar 14 1996;334(11):693699. Merion RM, Schaubel DE, Dykstra DM, Freeman RB, Port FK, Wolfe RA. The survival benefit of liver transplantation. Am J Transplant. Feb 2005;5(2):307-313. Cillo U, Vitale A, Volk ML, et al. The survival benefit of liver transplantation in hepatocellular carcinoma patients. Dig Liver Dis. Sep 2010;42(9):642-649. Vitale A, Morales RR, Zanus G, et al. Barcelona Clinic Liver Cancer staging and transplant survival benefit for patients with hepatocellular carcinoma: a multicentre, cohort study. Lancet Oncol. Jul 2011;12(7):654-662. Llovet JM, Fuster J, Bruix J. Intention-to-treat analysis of surgical treatment for early hepatocellular carcinoma: resection versus transplantation. Hepatology. Dec 1999;30(6):14341440. Nathan H, Bridges JF, Schulick RD, et al. Understanding surgical decision making in early hepatocellular carcinoma. J Clin Oncol. Feb 20 2011;29(6):619-625. Guidelines for preventing transmission of human immunodeficiency virus through transplantation of human tissue and organs. Centers for Disease Control and Prevention. MMWR Recomm Rep. May 20 1994;43(RR-8):1-17. Ison MG, Nalesnik MA. An update on donor-derived disease transmission in organ transplantation. Am J Transplant. Jun 2011;11(6):1123-1130. Kucirka LM, Sarathy H, Govindan P, et al. Risk of window period hepatitis-C infection in high infectious risk donors: systematic review and meta-analysis. Am J Transplant. Jun 2011;11(6):1188-1200. Feng S, Goodrich NP, Bragg-Gresham JL, et al. Characteristics associated with liver graft failure: the concept of a donor risk index. Am J Transplant. Apr 2006;6(4):783-790. Chotiyaputta W, Pelletier SJ, Fontana RJ, Lok AS. Long-term efficacy of nucleoside monotherapy in preventing HBV infection in HBsAg-negative recipients of anti-HBc-positive donor livers. Hepatol Int. 2010;4(4):707-715. Maluf DG, Edwards EB, Kauffman HM. Utilization of extended donor criteria liver allograft: Is the elevated risk of failure independent of the model for end-stage liver disease score of the recipient? Transplantation. Dec 27 2006;82(12):1653-1657. Vitale A, D'Amico F, Brolese A, et al. Prognostic impact of model for end-stage liver disease score in patients undergoing liver transplantation with suboptimal livers. Transplant Proc. Jul-Aug 2007;39(6):1907-1909. Volk ML, Vijan S, Marrero JA. A novel model measuring the harm of transplanting hepatocellular carcinoma exceeding Milan criteria. Am J Transplant. Apr 2008;8(4):839-846. Weismuller TJ, Fikatas P, Schmidt J, et al. Multicentric evaluation of model for end-stage liver disease-based allocation and survival after liver transplantation in Germany--limitations of the 'sickest first'-concept. Transpl Int. Jan 2011;24(1):91-99. Angelico M, Cillo U, Fagiuoli S, et al. Liver Match, a prospective observational cohort study on liver transplantation in Italy: study design and current practice of donor-recipient matching. Dig Liver Dis. Feb 2011;43(2):155-164. 19. 20. 21. 22. 23. 24. Fisher RA, Kulik LM, Freise CE, et al. Hepatocellular carcinoma recurrence and death following living and deceased donor liver transplantation. Am J Transplant. Jun 2007;7(6):1601-1608. Lo CM, Fan ST, Liu CL, Chan SC, Ng IO, Wong J. Living donor versus deceased donor liver transplantation for early irresectable hepatocellular carcinoma. Br J Surg. Jan 2007;94(1):78-86. Fujimoto K, Sawabe M, Sasaki M, Kino K, Arai T. Undiagnosed cirrhosis occurs frequently in the elderly and requires periodic follow ups and medical treatments. Geriatr Gerontol Int. Sep 2008;8(3):198-203. Cescon M, Grazi GL, Cucchetti A, et al. Improving the outcome of liver transplantation with very old donors with updated selection and management criteria. Liver Transpl. May 2008;14(5):672679. D'Amico F, Vitale A, Gringeri E, et al. Liver transplantation using suboptimal grafts: impact of donor harvesting technique. Liver Transpl. Oct 2007;13(10):1444-1450. Dutkowski P, de Rougemont O, Clavien PA. Machine perfusion for 'marginal' liver grafts. Am J Transplant. May 2008;8(5):917-924.