Idiopathic Neonatal Hepatitis
advertisement

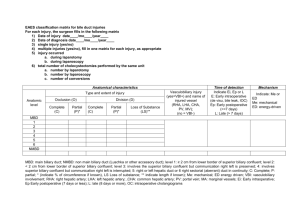
Neonatal direct hyperbilirubinemia defined as prolonged elevation of serum levels of conjugated bilirubin in neonatal period but usually beyond the 1st 14 days of life. That caused by defect in bile formation and excretion due to hepatocyte dysfunction or From obstruction to the flow of bile through the intrahepatic and extrahepatic biliary tree leading to accumulation of conjugated bilirubin, bile acids, and cholesterol in blood and extrahepatic tissues . so there will be retention of bilirubin & bile acid causing malabsorption of fat & fat soluble vit (A,K,D.E ) , xanthemas ( accumulation of cholesterol ), itching also develop due to accumulation of bile acid . associated with dark color urin (usually +ve for bilirubin ) & acholic stool . We regard the case as direct hyperbilirubinemia when the direct B. is > 20% of total bilirubin . It is not neurotoxic but it indicate serious disease Causes of neonatal Direct hyperbilirubinaemia (Cholestasis ) Intrahepatic disease 1 – Hepatocyte injury Idiopathic Neonatal Hepatitis Infection Metabolic cause Toxic Miscellanouse 2 – Intrahepatic billiary dis or flow obst Extrahepatic bile flow obst. ( neonatal cholestasis ) intrahepatic disease intrahepatic bile duct disease hepatocyte injury metabolic disease viral disease extrahepatic disease idiopathic neonatal hepatitis 1 intrahepatic bile duct paucity or hypoplasia extrahepatic biliary atresia & disease Intrahepatic disease Idiopathic Neonatal Hepatitis : which is the most common cause if patient not taking TPN Infection : - Bacterial Sepsis , UTI . Viral Infections TORCH ,HIV ,Varicella Zoster ,Coxacki , Hepatitis. TB , Syphilis . Metabolic cause as alpha1Antitrypsin deficiency , Tyrosinaemia Galactossaemia Fructossaemia , Wolman disease , Nieman pig , Glycogen storage disease , Zellweger (cerebro -hepato-renal syndrome ) . Toxic : - Total Parenteral Nutrition , most common cause in neonatal care unit .Sepsis with endotoxaemia , Drug related . Miscellanouse : Hypopituitarism , Hypothyroidism , Cystic Fibrosis intrahepatic billiary hypoplasia or paucity as Algile synd, Caroli disease , autosomal dominant polycystic liver disease (cysts in liver only) , autosomal recessive polycystic kidney disease (cysts in liver and kidney ) Intrahepatic cholestasis due to Disorders of membrane transport and secretion of bile acid as Progressive familial intrahepatic cholestasis (formerly known as Byler disease) Defective bile acid biosynthesis Extrahepatic bile flow obst. Biliary atresia , Choledochal cysts , Neonatal sclerosing cholangitis , Spontaneous perforation of common bile duct, Congenital hepatic fibrosis , Bile duct stenosis , Inspissated bile/mucous plug , Cholelithiasis , Tumors/masses (intrinsic and extrinsic) 2 Clinical presentation Clinically the jaundice of direct hyperB. is usually greenish yellowish in contrast to jaundice of indirect hyperB. which is usually orang-yellowish in colour . also it is associated with dark color urin (usually +ve for bilirubin ) & light or acholic stool . Some time patient may complain itching because of accumulation of bile acid & salt Also it may be associated with hepatosplenomegally with signs of chronic liver disease , bleeding , varices of portal hypertension , xanthemas , or associated with hepatic encephalopathy , ascites , signs of fat soluble vitamin deficiency due to retension of bile salts as Rickets ( D ) , neuromuscular disorder ( E ) , bleeding ( K ) , xerophthalmia ( A ) . coarse features of trisomy 21 & Zellweger , Algille Cataract , microcephally , Hx of infection in pregnancy as congenital infection TORCH . hypotonia , CNS manifestation in metabolic ,storage disease. hypoglycemia , vomiting , lethargy , signs of metabolic disease , carbohydrate intolerance , galactosaemia fructossaemia Hx of neonatal death suggest metabolic dis or infection delay passage of meconium may suggest cystic fibrosis . Complication Malnutrition resulting from malabsorption of dietary long-chain triglycerides Fat-soluble vitamin malabsorption: Vitamin A deficiency (night blindness, thick skin) Vitamin E deficiency (neuromuscular degeneration) Vitamin D deficiency (metabolic bone disease) Vitamin K deficiency (hypoprothrombinemia) Micronutrient deficiency , Deficiency of water-soluble vitamins Retention of biliary constituents such as bile acid , cholesterol causing itch or xanthomas Progressive liver disease and biliary cirrhosis; portal hypertension (variceal bleeding, ascites, hypersplenism) End-stage liver disease (liver failure) 3 Lab. Investigation of patient with direct hyperbilirubinemia. include liver function test and Complete blood count Radiological examination Specific test for Dx cause liver function test TSB with direct & indirect , direct should be more than 2mg / dL or more than 20 % of total . Liver enz. ( ALT ) SGPT (liver specific )S. Glutamic Pyruvic Transaminase , ( AST ) SGOT ; S.Glutamic Oxaloacetic acid Transaminase . increase these enz. indicate hepatocellular damage , the increase more marked in acute hepatic dis. than chr. liver dis. & intra or extra biliary obstruction . test for synthetic function that include (S. Albumin ) hypoalbuminaemia indicate severe liver dis. also ( PT & PTT ) , prolonged PT & PTT because of deficiency of vit. K dependant factor ( 1972 ) & other coagulation factor . It may indicate severe liver dis. Or fulminant hepatic failure . test for excretory function which include Alk. Phosphatase ( not specific to liver , also in bone) , also 5 nucleotidase , gamma glutamyl transpeptidase . They increase when there is defect in bile excretion as in biliary dis. or in hepatocellular dis. Cholesterol , increase in cholestasis & decrease in acute liver dis. as hepatitis serum ammonia, , serum glucose . Complete blood count, including platelet count Specific test for Dx cause Blood , urine & CSF analysis & culture for bact. , virus as HIV , Herpes , CMV . Serological exam. For TORCH , VDRL for syphilis Urine for B. , glucose , reducing substance as galactose , Red blood cell galactose-1-phosphate uridyl transferase. Paracentesis for ascites (examine for bile and infection) Serum & urine chromatography for a.a. dis. Thyroxine , TSH . Sweat test for cystic fibrosis analysis for alpha 1 anti trypsin deficiency . 4 Bone marrow examination and skin fibroblast culture for suspected storage disease Genetic testing for Alagille syndrome, three forms of PFIC, other Ultrasound U / S size of liver ,texture , echogencity ( increase echogenicity in fatty liver ) , mass, stone , choledocal cyst , gall bladder size , biliary tract , ascitic fluid , portal hypertension , patency of portal vein , presence of collatral . presence of other anomalies specially renal . Findings in infants with biliary atresia include an atretic gallbladder and a thin, indistinct gallbladder wall with an irregular or lobulated contour , An absent common bile duct , dilatation of the intrahepatic bile duct occurs infrequently hepatic parenchyma is often inhomogeneous . triangular cord sign located cranial to the portal vein bifurcation Central biliary cysts and choledochal cysts may be associated with biliary atresia , other Congenital anomalies as situs inversus and polysplenia • Till now the diagnosis of most cases of direct hyperB is done with these Ix except some time we need to do more investigation to diagnose & differntiate of idiopathic neonatal hepatitis , intra hepatic bile duct paucity , biliary atresia , so we need to do :- • • • • Magnetic resonance cholangiography Liver scan Duodenal intubation Liver biopsy Magnetic resonance cholangiography (MRC) , widely used to assess the biliary tract in all age groups Liver scan Tc 99m iminodiacetic acid dye with the use phenobarbitone 5mg/kg/day orally for 5 – 7 days to induce biliary excretion then we do the scan , In biliary atresia there is good uptake but no excretion , while in hepatitis uptake is sluggish with fair excretion . Duodenal intubation for measurement of B. in bile befor & after use of phenobarbitone where there is no B. in biliary atresia while there is good amount of B. in hepatitis . liver biopsy provide the most reliable discriminatory evidence & Dx . In biliary atresia there is bile ductular proliferation , bile plug ,portal or perilobular oedema & fibrosis , lobular achitecture is intact . In neonatal hepatitis , severe diffuse hepatocellular dis. , distortion of the lobular crchitecture , infl. Cell infilteration , focal hepatocellular necrosis , bile ductules show little alteration . Giant cell transformation present in both condition & have no dignostic specificity exploratory laporatomy some time may be needed 5 treatment of direct hyperbilirubinemia. (cholestasis ) include treatment of complication & original cause for complication with any cause of neonatal cholestasis, whether idiopathic neonatal hepatitis, intrahepatic cholestasis, or biliary atresia, affected patients are at increased risk for chronic complications. These are due to diminished bile flow. Give diet or formula with medium chain triglyceride , due to malabsorption of longchain triglyceride (there is fat malabsorption due to bile salt &acid retention ) , give high dose fat soluble vit for the same reason . Give some micronutrient as Ca ,Ph ,zink. Give choleretics as ursodeoxycholic acid or bile acid binder as cholestyramine to decrease itching , xanthoma . develop progressive billiary cirrhosis ,portal hypertention , he may develop oesophageal varices so we do endoscopy for proper Rx . Oedema & ascites treated by salt restriction & diuretics as frussemide alone or in combination with spironolactone . End stage hepatic failure may need liver transplant . Rx of the cause of direct hyperB. as in Galactossaemia we give him lactose free formula , some infection may need Rx , surgery may be needed in biliary atresia or choledochal cyst . Biliary Atresia The incidence is 1/10,000-15,000 live births , it is more in female , involve extrahepatic billiary duct , but in some cases there is intra & extrahepatic involvement Etiology It is unknown , but bile duct obliteration may be secondary to infection , toxins , or autoimmune process . So any patient with jaundice at 2 month must be evaluated for biliary atresia because surgery most effective before 2 months , otherwise biliary cirrhosis & ascending cholangitis may occur Clinical manifestation Full term infants in whom J. develop during the 2nd – 3rd week of life , Acholic stool , Hepatomegally , Splenomegally which detectable by 8 weeks , Other than these physical findings the infants appear healthy , But if patient not treated , they will develop progressive liver dis. , cirrhosis & portal hypertesion. A few infants with fetal onset of biliary atresia have an increased incidence of other abnormalities, such as the polysplenia syndrome with abdominal heterotaxia, malrotation, levocardia, and intra-abdominal vascular anomalies. Lab investigation LFT It demonstyrate direct Hyperbilirubinaemia & elevated serum alkaline phosphatase , gamma glutamyl transpeptidase . U / S mention previously Liver scan following 5 days of phenibarbital ( 5mg/kg/day ) , Percutaneous liver biopsy show bile duct proliferation with plugging & confirm the Dx in 95 % of cases . exploratory laporatomy some time may be needed , All patients suspected of having biliary atresia should undergo exploratory laparotomy and direct cholangiography to determine the presence and site of obstruction & ; if biliary atresia Kasai procedure (hepatoportoenterostomy ) 6 Treatment & prognosis A hepatoportoenterostomy, or Kasai portoenterostomy is a surgical treatment performed on infants with biliary atresia to allow for bile drainage . the earlier the operation ( <2 m. of age ) the greater the chance of establishing the bile flow. Surgical success is judged by improvement in bile drainage ; Without surgery Kasai procedure , patient will die cirrhosis before 2 yr. of age 25 – 50 % of patients survive 5 yr. after a successful Kasai procedure , but complications of the procedure include progressive biliary cirrhosis & ascending cholangitis . Another Rx for most infants is liver transplant which has 80 – 90 % survival rate . Idiopathic Neonatal Hepatitis ( INH ) It is responsible for most of cases of idiopathic cholestasis in infants who are not receiving parenteral nutrition . It is more in male , may be associated with growth retardation . INH represents more than one dis. Resulting from infectiouse Or familial causes . Normal color stool with transient acholic stool , little increase ALP or gamma glutamyl transpeptidase ( GGT ). Biliary scan show the patency of the bile duct . Liver biopsy shows numerous giant cells , lobular disorganisation , necrosis , & inflammation without the neoductular proliferation & fibrosis characteristic of extrahepatic atresia . Prognosis is good & most patient recover within 6 - 8 month . Differentiation of Idiopathic Neonatal Hepatitis & Biliary Atresia Idiopathic Neonatal Hepatitis ¨ Familial incidence is 20 %. ¨ Usually no other abnormality Biliary Atresia Unlikely to recur in same family . There is other abnormality as polysplenia , malrotation levo cardia , intra abdominal vascular abnormality No relation . Persistant acholic stool Persistant bile stained fluid after duodenal intubation against Dx of BA More in premature & SGA infants. ¨ Normal color stool with transient acholic stool ¨ In duodenal intubation the fluid is bile stained . ¨ Liver size less common to be ¨ Hepatobiliary scintography there is sluggish uptake & fair excretion . en ¨Liver biopsy . the most reliable discreminatory test larged Abnormal liver size & consistency There is good uptake but no excretion ¨Liver biopsy , exploratory laporatomy (intrahepatic bile duct paucity) Biliary Hypoplasia It is either syndromic as Aligille syndrome , arteriohepatic dysplasia ,or non syndromic . Infants with Aligille syn.present with sign & symptomes of direct hyperB.with facial features , cardiac valvular or peripheral pulm. stenosis , butter fly vertebrae , dysplastic kidney , hypercholesterolaemia with cutaneous xanthomas , dis. is AD 7 8