An Analysis of Intra-operative Awareness Among Ophthalmologic
advertisement

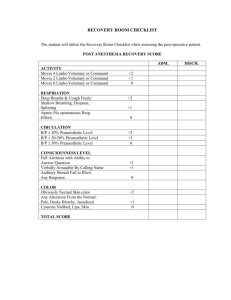
DEPARTMENT OF CLINICAL EPIDEMIOLOGY RESEARCH PROPOSAL An Analysis of Intra-operative Awareness in the Immediate Post-operative Period among Ophthalmologic Surgery Patients under General Intravenous Anesthesia using Propofol in the University of Santo Tomas Hospital AUTHORS: FACTON, Rosabelle T. GERALDOY, Isabelle Reyna G. KARAAN, Christopher James M. QUE, Scylla Kneisel C. TAN, Ernie Joe L. CO-AUTHOR: Romulo A. Buzon Jr., M.D. ABSTRACT General anesthesia is the induction of a state of unconsciousness with the absence of pain sensation over the entire body, through the administration of anesthetic drugs like general anesthetics. General anesthetics depress the central nervous system to a sufficient degree to permit the performance of surgery and other noxious or unpleasant procedures. They are considered to have a narrow margin of safety and thus require great care in administration. While all general anesthetics produce a relatively similar anesthetic state, they are quite dissimilar in their secondary actions. The selection of specific drugs and routes of administration to produce general anesthesia is based on patients’ pharmacokinetic properties and on the secondary effects of the various drugs, in the context of the proposed diagnostic or surgical procedure and with the consideration of the individual patient’s age, associated medical condition, and medication use. However, for reasons not clearly understood, some patients under anesthesia experience unexpected recall of events during surgery that may or may not have psychological implications in the future.The purpose of this study is to establish a localized report on the incidence of intraoperative awareness in order to provide decision tools that may enable the clinician to reduce the frequency of unintended intra-operative awareness. Ophthalmologic surgery patients under Propofol IV will be interviewed post-operatively and will be scored accordingly. Patients will be assigned to the recall group if their first post-induction memory is related to intra-operative events; and to the non-recall group if their first post-induction memory is related to events occurring after completion of surgery. Data of the study will be reported as the incidence of intra-operative awareness among the subjects. An Analysis of Intra-operative Awareness in the Immediate Post-operative Period among Ophthalmologic Surgery Patients under General Intravenous Anesthesia using Propofol in the University of Santo Tomas Hospital RESEARCH QUESTION What is the incidence of intra-operative awareness among ophthalmologic surgery general anesthetized cases (using Propofol IV) in the University of Santo Tomas Hospital; and what may be the contributing factors? HYPOTHESIS Null hypothesis: There will be no incidence of intraoperative recall on patients after general anesthesia (Propofol IV). Alternative hypothesis: There will be incidence of intraoperative recall on patients after general anesthesia (Propofol IV). GENERAL OBJECTIVE 1. To determine the incidence of intraoperative awareness among general intravenous anesthetized ophthalmologic surgery cases using Propofol IV in the University of Santo Tomas Hospital. SPECIFIC OBJECTIVE 1. To determine the extent of recall of patients under the general intravenous anesthesia using Propofol. INTRODUCTION General anesthethics today are the most potent depressors of nervous system activity used in medicine. They affect even the regulation of breathing and heart function. Because of this, these drugs are considered to have a narrow margin of safety. For this reason, individuals undergoing emergency operations, such as trauma victims whose lung and cardiovascular function is already unstable , or patients in the midst of heart surgery must receive a lighter than normal dose of anesthesia, which could make them susceptible to brief awareness incidents (Beverly A. Orser, Scientific American, June 2007, www.sciam.com). All of today’s general anesthetic drugs were developed empirically; they were tested for their ability to produce the desirable effects that define the anesthetized state. The physiologic state of general anesthesia includes sedation (reduced arousability), unconsciousness (also sometimes called hypnosis), immobility, absence of pain (analgesia) and absence of memory for the anesthetized period (amnesia). Studies have shown that activity of these potent drugs involves highly specific interactions with subpopulations of nervous system cells to create each of the separate properties of anesthesia. Anesthetics are categorized based on whether they are delivered by inhalation, such as isoflurane, or intravenously, such as propofol. These drugs induce a state of a pharmacological coma, which is a deep sleep. They prolong the duration of postsynaptic electric currents generated by GABAA receptors. Intravenous anaesthetics have an onset of anaesthetic action faster than the fastest of the inhaled gaseous agents such as desflurane and sevoflurane, making them the agents commonly used for induction of anaesthesia. Both the desirable and unwanted effects of anaesthetic drugs came from their ability to suppress neuronal activity throughout the central nervous system. Propofol, 2,6,-diisopropylphenol, has been in use in the Unites States since November, 1989. Propofol is a low molecular weight (178D) molecule that is virtually insoluble in water and is highly soluble in fat. Propofol infusions are often combined with opioid infusions during anesthesia. Since the decline in propofol concentration is several folds faster than the decline in opioid concentration, it makes pharmacokinetic sense to titrate the propofol while maintaining a constant opioid concentration. Propofol's pharmacokinetic characteristics of extremely rapid metabolism and large distribution clearances relative to distribution volumes result in a unique disposition that is well suited to both induction and maintenance of anesthesia. Patients in hypovolemic shock should not be induced with propofol (Intravenous Anesthesia: Techniques and New Drugs by Steven L. Shafer, M.D., Donald R. Stanski M.D.). The anaesthetic potency of intravenous anaesthetics, including thiopental, ketamine, and propofol, is enough to allow their use as the sole anaesthetic in short surgical procedures when combined with nitrous oxide and opioid analgesics. Adjunctive use of potent opioids, such as fentanyl, contributes cardiovascular stability, enhanced sedation, and profound analgesia. However, pre-anaesthetic administration of benzodiazepines, having a slower onset, can provide a basal level of sedation and amnesia (Basic and Clinical Pharmacology, 9th Edition 2004). Anaesthetics are known to cause amnesia at doses considerably lower than those required for unconsciousness or immobility. Yet for some reasons, some patients experience unexpected recall of events during the surgery itself. Episodes of intraoperative awareness while under general anaesthesia are reported by one or two of every 1,000 patients. The risk of intraoperative awareness seems to vary among types of procedures. The reported incidence of patient awareness during anesthesia depends on the type of anesthesia, strength of the stimulus, and the timing and persistence of attempts to elicit recall. Several resources report the overall incidence of IOA is 0.2% to 1% of the 18.6 million anesthetized procedures performed each year. Cesarean section procedures pose a 2% to 28% risk of awareness; major trauma procedures, 11% to 43%: cardiopulmonary bypass procedures, 1.14% to 23%; and bronchoscopy procedures, 8%. One study limited to "fast-track" cardiac surgical patients cited an incidence of 3.3%. (Monitoring for Intraoperative Awareness, Oullette, Sandra M.; Simpson, Chrysanne AORN Journal 12/1/1998) REVIEW OF RELATED LITERATURE Intraoperative awareness under general anaesthesia is a rare occurrence, with a reported incidence of 0.1-0.2% (Myles et al., 2000). Significant psychological sequelae (e.g., post traumatic stress disorder) may occur following an episode of intraoperative awareness, and affected patients may remain severely disabled for extended periods of time (Lennmarken et al., 2002). In some circumstances, intraoperative awareness may be unavoidable to achieve other critically important anaesthetic goals. In the Philippines, however, the incidence of intraoperative awareness has not yet been fully established. Thus, this study will provide a localized report on the incidence and contributing factors to intraoperative awareness. Awareness is the post-operative recall of events that takes place during general anesthesia. It is an uncommon problem of anesthesia in the adult surgical population, with an incidence of 0.1%–0.2%. In adults, awareness is often a distressing event and may have significant psychological ramifications. There are only few studies known about awareness in modern pediatric anesthesia. One study last June 1993, Recall of Intraoperative Events after General Anaesthesia and Cardiopulmonary Bypass by Phillips et al. reported an incidence of awareness with subsequent recall of intraoperative events of 1.14% in patients undergoing cardiopulmonary bypass with a low-dose narcotic, balanced anesthetic technique in which evaluation of patients undergoing cardiopulmonary bypass for cardiac surgery was done to assess the incidence of the problem and determine any obvious causes of intraoperative awareness. Anesthesia was induced with diazepam or midazolam (1-10 mg), fentanyl (10 μg • kg-1) and when required, thiopentone sodium (0.2-2.0 mg • kg-1). Muscle relaxation was achieved with a bolus of pancuronium (0.12 mg • kg"1). Anaesthesia was maintained with a volatile agent, primarily halothane, with additional boluses of diazepam and fentanyl at the discretion of the anaesthetist. During bypass isoflurane was entrained and benzodiazepines injected into the bypass circuit to help achieve the desired mean perfusion pressure. Post-bypass a volatile agent was introduced in the presence of adequate cardiovascular stability. The records of patients reporting intraoperative recall and of 60 randomly selected patients without recall were further scrutinized to determine the percentage of time volatile agents were entrained in the pre-bypass, bypass and post-bypass periods. Out of a total of 837 patients who underwent cardiopulmonary bypass from the 16th March 1990 to 31st October 1991 majority of patients underwent coronary artery bypass surgery. Seven hundred patients (84%) completed the postoperative interview, their average age, duration of CPB and aortic cross-clamping. The first post-induction recall was intraoperative in eight patients, resulting in a 1.14% incidence of recall of intraoperative events. A subsequent detailed review of the charts of the eight patients who reported recall and of 60 randomly selected non-recall patients' charts revealed there was no difference in the percentage of time volatile agents were entrained in the pre-bypass, bypass and post-bypass periods of the operation. Episodes of awareness seemed to occur at any time during the operation. Because cooling is associated with a decreased level of consciousness and lowered metabolic rate, we wondered if patients undergoing normothermic bypass might have a higher incidence of recall. We were unable to demonstrate an effect of temperature on recall. The smaller number of patients with recall precludes drawing any definitive conclusions on the effect of temperature on recall in these patients. Preliminary power calculations show that to have an 80% power for detecting a halving of the 2% incidence found in the warm patients, 2100 patients per group would have to be studied. Given the problems with monitoring the depth of anaesthesia and the limitations imposed on the investigators by the surgery it is not surprising that there is a measurable incidence of recall in these patients. The incidence that we report following CPB is much lower than in two previously published studies of cardiac surgery patients. Another study, Awareness during Anesthesia in Children: A Prospective Cohort Study by Davidson et al. performed in 2005, wherein from one-thousand-two-hundred-fifty children recruited into the behavior study, only 864 children remained and had at least 1 assessment for awareness. Seven-hundred-fifty-six (88%) were assessed within 1 day of the procedure, 704 (81%) at Day 3, and 590 (68%) at 30 days. The principal investigator interviewed 28 children who had suspected awareness from the screening questions. Twenty-eight reports were generated and sent to the adjudicators. In 12 cases, at least 1 adjudicator reported the case as “awareness.” There were 7 cases of true awareness for an incidence of 0.8% (95% confidence interval, 0.3%– 1.7%). Cases that were not classified as “awareness” were usually children with auditory memories of events that could have occurred in recovery and children with inconsistent or contradictory memories. The awareness assessment was nested within a larger detailed study of predictors of behavior change in children after hospitalization and anesthesia. This article presents only the awareness data. Because of differing anesthesia requirements and techniques, it is possible that the incidence of awareness differs significantly in children, who, compared to adults, also have different expectations, fears, and ways of managing stressful events. The prevention of awareness continues to be a priority for anesthesiologists. SIGNIFICANCE General anaesthesia is one of the primary modes of anaesthesia used in hospitals today for major surgeries, either elective or emergency procedure, in the operating rooms. The aim of general anesthesia is to provide a condition characterized by unconsciousness, muscular relaxation and the suppression of reflex response to noxious stimuli. The problem which continues to disappoint anaesthetists is our limited ability to assess our patients' level of consciousness. Debate have been made regarding the status of the consciousness of patients if intra-operative information is presented them, this correlates to the consciousness of the patient during those times and check on recall postoperatively. With the use of muscle relaxants and balanced anaesthesia, the assessment of depth of anaesthesia is difficult. There have been studies that showed that there is a considerable evidence that specific information both perceived during anaesthesia and remembered following surgery (Merikle and Daneman). But there are also studies contradicting this, saying that anaesthesia such as inhalation ones doesn’t have effect on implicit or explicit memory during anaesthesia and is not recalled after the surgery (Wang and Russell, 1997). Another study conducted also by Russell and Wang showed that intravenous injection using Propofol and Alfetanil showed no significant result on the presence of either explicit or implicit memory. This discrepancy led to the importance of verifying this information because awareness during major surgery is one of the important considerations in anaesthesia as presence of awareness may lead to traumatic experience related to unfamiliar surgical procedure, painful sensation and fear of the unknown. However, when propofol is used without N2O or a potent vapor, there is the possibility of intraoperative awareness. Although intraoperative awareness can also occur when using a N2O/opioid anesthetic technique, NO is a sufficiently potent analgesic that intraoperative awareness of pain almost never occurs during when using N2O with an opioid. This is not the case with propofol. Intraoperative awareness during a propofol/opioid technique (e.g. during total intravenous anesthesia) may include awareness of intraoperative pain (Intravenous Anesthesia: Techniques and New Drugs by Steven L. Shafer, M.D., Donald R. Stanski M.D.). In one study, the investigators reported a case of awareness and recall during propofol anesthesia combined with epidural anesthesia in a patient scheduled for a resection of left ovarian tumor. After induction, anesthesia was maintained with propofol and epidural anesthesia. About one hour into maintenance, the patient was moving with haemodynamic signs suggesting inadequate analgesia. Immediately after extubation, the patient could recall the abdomen being touched during laparotomy. This case indicates that even if appropriate dose of propofol is administrated, intraoperative awareness may occur especially with inadequate analgesia. (Sakio H, Saitoh K, Inoue S, Nakaigawa Y, Hirabayashi Y, Seo N.). As was in a study wherein a woman with mild liver dysfunction underwent lower abdominal surgery, anesthesia was induced with propofol 60 mg and fentanyl 0.1 mg. Tracheal intubation was facilitated with vecuronium 8 mg, and the lungs were ventilated with 33% oxygen in air. The bispectral index (BIS) was continuously monitored. Anesthesia was maintained with propofol infusion and analgesia was provided by thoracic epidural infusion of lidocaine 1.5%. The infusion rate of propofol was altered to maintain the BIS value between 40 and 50. The patient was hemodynamically stable with propofol 1.5 mg.kg-1.hr-1 and the BIS value was maintained about 40 during the operation. Near the end of the operation the patient moved suddenly. Suspecting inadequate anesthesia, a total of 40 mg of propofol IV and 5 ml of the epidural infusion were given. Immediately before the movement the BIS value was about 40. The operation was completed 30 min later. On discharge from the operating room the patient declared that she had been awake. She had heard voices and felt the surgeon working, but had suffered no pain. The BIS is a useful indicator for hypnotic effect, but this case demonstrates that awareness might occur even when BIS value indicates adequate hypnotic state. (Kurehara K, Horiuch T, Takahash M, Kitaguchi K, Furuya H. Surgical Center, Nara Medical University, Kashihara) SCOPE AND LIMITATIONS 1. The Study will be conducted at the university of Santo Tomas Hospital only. 2. This study will only include surgeries of general anesthesia using Propofol IV. 3. This study will only include ophthalmologic surgery patients. 4. This study will not include patients younger than 3 years old, safety and efficacy of Propofol at this age have not been established for maintenance anesthesia. 5. The subject should be able to respond to the questions. Patients with neurotic disorders, under comatose, mute, deaf, or other causes that will render them unfit to be interviewed are all excluded. 6. Patients who have had a history of mental instability, and alcohol and substance abuse will not be included in the study population. 7. Long term effects of intraoperative recall are not included in this study. 8. Interviews will be done post-operation, at a time and condition deemed appropriate by the anaesthetist and attending surgeon. 9. The sampling of subjects is purposive. BUDGET For this study, there will be minimal expenses which will mainly be distributed in the production of the final paper (e.g. printing, binding, photocopying). The study proper is of interview-survey type only and will not therefore require any sort of cost. METHODOLOGY This is a prospective cohort study. A post-anesthetic review will be performed. Included in this assessment is a structured interview relating to intraoperative recall. A series of questions will be asked to the patients. Table 2 and 3 summarizes these questions and the indications of their replies. Post-anesthesia recovery score of Aldrete will be noted. This score records vital signs with patients receiving 0-10 points: 0-2 points for five physiological variables (Table 1). A high score is indicative of full recovery. Table 1. Post-anesthesia recovery score Aldrete Scoring System for Conscious Sedation Activity Voluntary movement of all limbs to command -2 points Voluntary movement of two extremities to command- 1 point Unable to move- 0 points Respiration Breathe deeply and cough- 2 points Dyspnea, hypoventilation- 1 point Apneic- 0 points Circulation BP +/- 20 mm Hg of pre-anesthesia level- 2 points BP > 20-50 mm Hg of preanesthesia level- 1 point BP > 50 mm Hg of preanesthesia level- 0 points Consciousness Fully awake- 2 points Arousable- 1 point Unresponsive- 0 points Color Pink- 2 points Pale, blotch- 1 point Cyanotic- 0 points Total score must be > 8 at conclusion of monitoring. Table 2 Post-anesthetic review questions and indication of replies Question What is the last thing you remember before going to sleep? What is the very next thing you remember upon waking up? Can you remember anything in between these two events? Did you have any dreams? Indication Site of the last pre-induction recall Site of the first post-induction recall Evaluation of recall Table 3 Structured Awareness Screening Interview 1. Were you upset, worried, or frightened about your operation? 2. How upset, worried, or frightened were you? 3. What was the last thing you remember before the operation? 4. How did the doctor make you go to sleep? 5. What is the next thing you remember after the operation? 6. Did you have any dreams or feel or hear anything while you were having the operation? 7. Were you sore after the operation? 8. How much did it hurt? 9. What did you like least about having an operation? 10. What did you like best about having an operation? 11. Did someone talk to you about what the operation was going to be like? 12. Was that about the same as what happened? 13. How do you feel about the operation? 14. Would you like to have known more? Patients will be assigned to the recall group if their first post-induction memory related to intraoperative events; and to the non-recall group if their first post-induction memory related to events occurring after completion of surgery. A review of anesthetic charts will provide a record of the dosages of premedications, induction agents and drugs employed to maintain anesthesia. Sample Results Table 4 Patient characteristics Sex Age Male Female 18-30 years old 31-50 years old >50 years old Table 5 Detail of awareness Period of Time Induction Maintenance Post-operative Remembrance Sound Pain Paralysis Table 6. Possible contributing factors Factor Awareness 37 62 0 89 10 Percentage 37.37 62.63 Awareness Percentage Awareness Percentage Type of surgery Site of surgery Dosage of anesthesia During the consent process, the family will be informed that the study was a survey of intraoperative recall of events after general anesthesia. After a detailed explanation of the questionnaires needed for the assessment, the family will also be informed that there would be questions about the patients’ memories and experiences in the period around the anesthetic. Anesthesiologists will be informed about the awareness study before it started. Once the patient is already in the recovery room, the anesthesiologist will be asked to provide details of anesthetic technique and a description of any critical incidents. Screening questions will be asked once post-surgery to detect possible awareness. The screening interview will be during the hospital stay. For day-stay patients, this will be performed just before discharge. For in-patients, the interview will be on either the same day or the next day if the patient is unwilling or unable to talk on the day of the anesthetic. During this interview, the awareness screening questions will be inserted among data collected for the intraoperative awareness study. The questions are listed in Table 2 and 3. The same questions will be used for all patients. If the patient answered “no,” then the screening questions will not be repeated. No incentives will be given for the patient to answer, and no leading questions will be asked during the screening interview. If the patient answered “no” to Question 6 on Table 3, there will be no further prompting. If the patient answered “yes,” and if we thought there is a possibility that the answer represented awareness, then we will take note of the data. The screening questions will be asked by the authors. A memory was classified as a dream if the patient considered the memory to be a dream. When any potential cases of awareness are identified, the anesthesiologist who performed the anesthetic will be informed. Any comment by the anesthesiologist that is relevant to the possible awareness event will be recorded. Possible contributing factors pertaining to the dosage difference and the site of surgery will be investigated and presented as shown in Table 6. An estimate of the necessary sample size will be based on the intention of confidently excluding the possibility of not detecting an incidence of awareness. Patients experiencing awareness during surgical procedures performed under general anesthesia may subsequently recall intraoperative events. To reduce bias, an effort will be made to keep the profile of this study low. However, as the study progresses, the anesthesia staff becomes more familiar with the study. It is not possible to blind the anesthesia staff, for ethical and medico-legal reasons. It is also useful to be able to gather information about the case from the involved anesthesiologist. It is possible that as the profile of the study gradually increased, the anesthesia staff changes their routine practice. CONCEPTUAL FRAMEWORK CAUSATIVE FACTOR Inadequate level of anesthesia INTERMEDIATE EFFECTS (CONFOUNDERS) - Interpatient pharmacokinetic and pharmacodynamic variability -Inadequate anesthesia (wrong dosage calculation) -Reduced or no use of premedication (adjunctive drugs, e.g. fentanyl and midazolam) - Equipment failure (perfusor pump failure, inaccurate manual titration improperly calibrated or connected vaporizers, empty vaporizers, general problems with anesthesia machines) PRESENCE OF INTRAOPERATIVE AWARENESS SAMPLING DESIGN Non-Probability- Purposive Sampling A. Inclusion Criteria 18 years old and above (Age Range: 18-80 years old) scheduled for ophthalmologic surgical operation (ASA I and II Surgeries) in the UST Hospital Examples: Cataract extraction, lensectomy, lacrimal endoscopy those who will be under Propofol anesthesia via intravenous injection B. Exclusion Criteria those with psychological deficit or illness those with head trauma and/or disease affecting cognition and memory SAMPLE SIZE CALCULATION n ≥ [Np (1-p)] / [(N-1)D + p(1-p)] D= (Margin of Error)2 / (za/2)2 n – Sample size N – Population size P – Prior assumption of the population parameter If the level of confidence is 95% then α = 5% then z value is 1.96 (D = 0.00065077) If the Total Population size (N) is 1000, margin of error is ±5% and the P is 10% n ≥ [Np (1-p)] / [(N-1)D + p(1-p)] n ≥ [(1000*0.10) (1-0.10)] / [(1000 – 1)(0.00065077) + (0.10)(1 – 0.10)] n ≥ [(100) (0.90)] / [(999)(0.00065077) + (0.10) (0.90)] n ≥ [90] / [(0.65011923) + (0.09)] n ≥ [127.5] / [0.74011923] n = 121.6020 ≈ 122 The calculated sample size is 122. This is the minimum recommended size for the study. STATISTICAL ANALYSIS Data of the study will be reported as the incidence of intraoperative awareness among the subjects. The following formula will be used to achieve this: Incidence Proportion = Subjects who experienced intraoperative recall ----------------------------------------------------------- x 100 Total subjects assessed within a given period of time Basically, incidence involves: a condition; a source population at risk of the condition; and the passage of time during which events occur. It could be reported as either incidence rate or incidence proportion. Incidence rate takes into account what happens from moment to moment. One disadvantage of this is that it assumes that the rate is constant over different periods of time. Incidence proportion, on the other hand, is the incidence calculated using a period of time during which all of the individuals in the population are considered to be at risk for the outcome. It is sometimes referred to as cumulative incidence or the attack rate. TIMETABLE Date Activity June-October 2007 November 2007-March 2008 June 2008-June 2010 July 2010 August 2010-September 2010 October 2010 November 2010-March 2011 Research Protocol Presentation Research subgroup discussion: planning level Drafting of protocol Submission of final research protocol Research Proper Sample size selection Distribution and collection of informed consent Conduction of interview/scoring Data collection Final collection of data Interpretation and analysis of data Research paper Final research output Presentation of final research output Submission of final research output (including input from the Review Board) GANTT CHART Activity JuneOct 2007 Subgroup discussion Drafting of Protocol Submission of final research protocol Research Proper Sample size selection Informed consent Interview Analysis of data Research paper Final research output Submission Nov 2007Mar 2008 Timeline June 2008-June July 2010 2010 AugSept 2010 Oct 2010 Nov 2010Mar 2011 Since the study will involve human subjects, free and informed consent will be secured in order to conform to ethical concerns. This will be done by allowing the subjects to thoroughly read and voluntarily sign a form that will be written in the language that they would understand best (English/Filipino). All the important details of the study that are of the subjects’ concern which, on the other hand, would not generate any bias will be included in the consent. Also, they will be assured that their identities will not be revealed in the least manner. Sample informed consent is as follows: [Date] INFORMED CONSENT FORM University of Santo Thomas Faculty of Medicine and Surgery An Analysis of Intra-operative Awareness in the Immediate Post-operative Period among Ophthalmologic Surgery Patients under General Intravenous Anesthesia using Propofol in the University of Santo Tomas Hospital Rosabelle T. Facton, Isabelle Reyna G. Geraldoy, Christopher James M. Karaan, Scylla Kneisel C. Que and Ernie Joe L.Tan You have been asked to take part in a research project described below. The researcher will explain the project to you in detail. You should feel free to ask questions. The investigator in charge will discuss them to you. Description of the project: You have been asked to take part in the study that will investigate on the effects of general anesthesia IV propofol on intraoperative recall of patients undergoing ophthalmologic surgeries. The incidence of recall, according to previous studies, is rare. You are being asked to volunteer in the research because you have been found to fit the criteria needed. These include the type of surgery to which you will be subjected, the anesthesia to be used in your surgery, age, psychological health, and absence of history of any problem regarding memory. Other potential subjects are also being asked to volunteer for this research. Procedures: If you decide to take part in this study here is what will happen: After the operation, post-recovery, you will be interviewed to assess any intraoperative awareness. It will be conducted in your room to avoid any inconveniences. One to three investigators will be present during the interview. It will only be done once and would expect to last within 30 minutes. We do expect your full cooperation and honesty in answering the questions provided. Risks or discomfort: If intraoperative awareness is indeed present, discomfort in recalling the events is possible. But for clarification, the study will have no control over the type of surgery you will be subjected into and the anesthesia to be used. The study merely chooses potential subjects who fit the criteria set for the investigation. Benefits of this study: Although there will be no direct benefit to you for taking part in this study, the researcher may learn more about the link between intraoperative awareness and Propofol and might benefit future patients. Confidentiality: Your part in this study is confidential. None of the information will identify you by name. All records will be kept in a secure place only the investigators know of. Voluntary participation and withdrawal: Participation in research is voluntary. You have the right to refuse to be in this study. If you decide to be in the study and change your mind, you have the right to drop out at any time. Whatever you decide, you will not receive penalty. Questions, Rights and Complaints: If you have any questions about this research project, please call Ysa at +639154536741 or Scy +639273352480 or email at clin_epi@yahoogroups.com. Consent statement By signing this document you consent to participating in “An Analysis of Intra-operative Awareness in the Immediate Post-operative Period among Ophthalmologic Surgery Patients under General Intravenous Anesthesia using Propofol in the University of Santo Tomas Hospital” being given by the medical students at the University of Santo Thomas Faculty of surgery whose names appear above. This statement certifies the following: that you are 18 years of age or older and you have read the consent and all your questions have been answered. You understand that you may withdraw from the study at any time and will not be penalized. All of the answers you provide will be kept private. You should know that you have the right to see the results prior to their being published. A copy of the informed consent will be given to you. __________________________________ Signature over Printed Name of Participant __________________________ Date REFERENCES (1) Andrew J. Davidson, MBBS, GradDipEpiBiostats, FANZCA, Grace H. Huang, BMedSci, (2) Caroline Czarnecki, BMedSci, Margaret A. Gibson, BN, RN, Stephanie A. Stewart, BN, RN,Kris Jamsen, BSc, PGDip(Stats), and Robyn Stargatt, PhD, MAPS Awareness during Anesthesia in Children: A Prospective Cohort Study, Department of Anaesthesia, Royal Children’s Hospital, Flemington Rd., Parkville 3052, Victoria, Australia.Anesth Analg 2005;100:653–61 (3) Andrew A. Phillips MBChB FCAnaes, Richard E McLean MD FRCPC, J. Hugh Devitt MD MSC FRCPC, Ellen M. Harrington BA. Recall of intraoperative events after general anaesthesia and cardiopulmonary bypass (4) Basic and Clinical Pharmacology, 9th Edition 2004 (5) Beverly A. Orser, Scientific American, June 2007, www.sciam.com (6) Kurehara K, Horiuch T, Takahash M, Kitaguchi K, Furuya H. A case of awareness during propofol anesthesia using bispectral index as an indicator of hypnotic effect. Surgical Center, Nara Medical University, Kashihara 634-0813 PMID: 11554023 [PubMed - indexed for MEDLINE] (7) Lennmarken et al., 2002 (8) Merikle and Daneman (9) Myles et al., 2000 (10) Oullette, Sandra M.; Simpson, Chrysanne. Monitoring for Intraoperative Awareness, AORN Journal 12/1/1998 (11) Sakio H, Saitoh K, Inoue S, Nakaigawa Y, Hirabayashi Y, Seo N. Intraoperative awareness during propofol anesthesia with epidural anesthesia Department of Anesthesiology and Clitical Care Medicine, Jichi Medical School, Tochigi 329-0498. PMID: 12428327 [PubMed - indexed for MEDLINE]) (12) Steven L. Shafer, M.D., Donald R. Stanski M.D. Intravenous Anesthesia: Techniques and New Drugs (13) Wang and Russell, 1997 (14) http://www.becomenatural.com/blog/2007/09/introduction-to-general-anesthetics/ (15) http://www.healthline.com/galecontent/anesthesia-general BIOGRAPHICAL SKETCH Rosabelle Tababa Facton 24 years old #95E Cristobal Street Sampaloc, Manila 2007- Present, Third Year Medical Student, Faculty of Medicine and Surgery, UST College: Bachelor of Science in Biology University of the Philippines Diliman rovifacton@yahoo.com Experience in Research: College Thesis Effects of Dietary Oils on Metabolic Rate, Blood Glucose, Body Temperature and Body Weight of Mice Isabelle Reyna G. Geraldoy 23 years old 76 Jasmin Street, Roxas District, Quezon City 1103 2007- Present, Third Year Medical Student, Faculty of Medicine and Surgery, UST College: University of the Philippines Manila Bachelor of Science in Biology sabby08_g@yahoo.com Research Experience: College Thesis: Water Quality Assessment of Laguna Lake Using Developmental Biomarkers in Cane Toad (Bufo marinus) Embryos Christopher James M. Karaan 23 years old 500 Bagbag Seminary Rd. Novaliches, Quezon City 2007- Present, Second Year Medical Student, Faculty of Medicine and Surgery, UST College: University Of Santo Thomas Bachelor of Science in Medical Technology Experience in Research: College Thesis A Study on the Antibacterial Activity of Aqueous Extracts of Parsley (Petroselinum crispum) Against Clinical Isolates Scylla Kneisel C. Que 24 years old 11F North Road San Gabriel Village Tuguegarao City 3500 scykneisel02@yahoo.com; wylanski23@yahoo.com 2007- Present, Third Year Medical Student, Faculty of Medicine and Surgery, UST College: University of Santo Tomas Bachelor of Science in Pharmacy Experience in Research: College Thesis Comparative Studies of the Phytochemical, Toxicological and Antioxidant Properties of the two cultivars of Ipomoea aquatica var. Forsk. (Convolvulaceae) from Tanauan and Talisay, Batangas Ernie Joe L. Tan 23 years old 1246 Pedro Gil St. Paco, Manila erniejoetan@yahoo.com; kngarthr2000@yahoo.com 2007- Present, ThirdYear Medical Student, Faculty of Medicine and Surgery, UST College: University of SantoTomas Bachelor of Science in Medical Technology Experience in Research: College Thesis The Larvicidal Effect of Anona Muricata (Guyabano) Seed Extract Against Mosquito Larvae Romulo A. Buzon Jr., M.D., DPBA, FPBCA, Professor I, Faculty of Medicine and Surgery Department of Epidemiology, Anesthesiology, and Physiology UST Thoracic and Cardiovascular Anesthesiology dr_buzon@yahoo.com