Protease inhibitors in chronic hepatitis C
advertisement

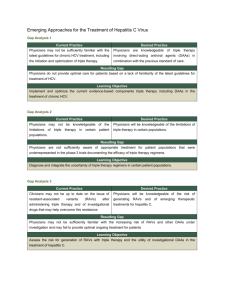
Protease Inhibitors in Chronic Hepatitis C: An Update Chapter 2 – Important Hepatitis C Protease Inhibitor Drug Interactions in Mono and HIV Coinfection Edited by Morris Sherman MD BCh PhD FRCP(C) Associate Professor of Medicine University of Toronto November 2012 Important Hepatitis C Protease Inhibitor Drug Interactions in Mono and HIV Coinfection Alice Tseng, Pharm.D., FCSHP, AAHIVP Toronto General Hospital University of Toronto Outline Review principles of drug interactions Understand how the pharmacology of DAAs contribute to drug interactions Highlight important HCV drug interactions Outline a strategy for identifying and managing drug interactions Identify pertinent HCV drug interaction resources Drug Interactions Pharmacodynamic Change in pharmacological effect of a drug Additive, synergistic, or antagonistic activity or toxicity e.g., ribavirin + AZT = anemia Pharmacokinetic Change in the amount of drug(s) in body Absorption, distribution, metabolism, elimination may be affected Often involves CYP450 system or transporters Interactions Affecting Drug Metabolism Majority of drugs transformed to inactive forms prior to elimination through Phase I (oxidation) or Phase II (conjugation) reactions Phase I primarily involves cytochrome P450 system Superfamily of microsomal heme-containing enzymes Primarily located in liver, small bowel; also kidney, lung, brain CYP3A is the most abundantly expressed isoenzyme, is involved in the metabolism of ~50% of clinically used drugs others: CYP2D6, 2C9, 2B6, 1A2, etc. P-glycoprotein Efflux membrane transporter which prevents drug accumulation in cells; has broad substrate specificity, and inhibiting or inducing the activity of this protein can lead to significant alterations in drug exposure Terms Definition Interaction Impact Common Examples Substrate Agent which is primarily cleared via a certain enzymatic pathway Rate of drug breakdown is affected by presence of enzyme inhibitors or enzyme inducers antidepressants, azoles, benzodiazepines, statins, corticosteroids, calcium channel blockers, macrolides, rifamycins, HIV PIs & NNRTIs Inhibitor Agent which competes with another drug for binding at enzymatic site Decreased clearance macrolides, azoles, HIV of substrate drug; quick protease inhibitors onset & resolution of interaction effect Inducer Drug that stimulates the production of additional metabolic enzymes Increased clearance of substrate drug; slower onset and resolution of interaction effect anticonvulsants, rifamycins, HIV NNRTIs, St. John’s wort Boceprevir and Telaprevir Pharmacology Boceprevir Telaprevir Dosing 800 mg q8h with food 750 mg q8h with food (20 g fat) Substrate CYP3A4, P-gp, AKR CYP3A4, Pgp 3A4, P-gp 3A4, P-gp, renal transporters (?) Inhibitor Inducer No inducing effects in vitro (in vivo?) = +++ potential for interactions with other drugs can be clinically significant sometimes unpredictable Potential Consequences of DAA Drug Interactions Interactions may occur in a two-way manner: Concentrations of DAA may be altered by other drug(s) Concentrations of concomitant drug(s) may be altered by DAA Potential consequences include: Increased risk of toxicity Decreased efficacy Statin Interactions Most statins are P450 substrates DAAs can significantly increase statin levels: Atorvastatin: 130% with boceprevir, 7.88-fold with telaprevir Pravastatin: 60% with boceprevir risk of toxicity, including myopathy and rhabdomyolysis Boceprevir Lovastatin, Simvastatin Telaprevir CONTRAINDICATED Atorvastatin May need to atorvastatin dose; do not exceed >20 mg/d CONTRAINDICATED Pravastatin Start with recommended dose and monitor for toxicity. Possible in statin; use with caution. Rosuvastatin, Fluvastatin Possible in statin; use with caution. [Victrelis & Incivek Product Monographs, 2011. FDA HIV/AIDS Drug Safety Communication, March 1, 2012] Atorvastatin Interactions with Boceprevir and Telaprevir Atorvastatin 20 mg + telaprevir: Atorvastatin AUC 7.88-fold 30,000 100 25,000 Atorvastatin alone Atorvastatin + Boceprevir 20,000 15,000 10,000 5,000 Concentration (ng/mL) Atorvastatin concentration (pg/mL) Atorvastatin 40 mg + boceprevir: Atorvastatin AUC 130% and Cmax 170% vs. atorvastatin alone 0 10.0 With telaprevir 1.00 Without telaprevir 0.10 0.01 0 8 16 24 Time (hrs) 32 40 Suggest atorvastatin dose with concomitant BOC; monitor for symptoms of statin toxicity if using >40 mg/d atorvastatin Hulskotte EGJ et al. HEP DART 2011, Koloa, Hawaii, poster 122 48 0 10 20 30 Nominal time (hrs) 40 50 Combination is contraindicated Lee JE et al. Antimicrob Agents Chemother 2011, 55(10):4569-74 Effect of Steady-State Telaprevir on the Pharmacokinetics of Amlodipine 5 mg Concentration (ng/mL) 5.00 Calcium channel blockers (CCBs) With telaprevir Amlodipine, diltiazem, felodipine, nifedipine, nicardapine, verapamil are CYP3A4 substrates Concentrations may be by boceprevir or telaprevir Use with caution, clinical monitoring Consider dose reduction 0.50 Without telaprevir 0.05 0.01 0 50 100 150 200 250 Nominal time (hrs) Amlodipine AUC 179% Monitor for dose-related toxicity Lee JE et al. Antimicrob Agents Chemother 2011, 55(10):4569-74 Antihypertensive Medications Class Examples Potential DAA Interactions ACEI Enalapril, lisinopril, ramipril (renal) Not expected ARBs Losartan (2C9>>3A4 to active metabolite) Candesartan, irbesartan (2C9) Eprosartan, olmesartan, telmisartan, valsartan (biliary) Possible effect Low Not expected Betablockers Propranolol (2D6, 3A4, 2C19), carvedilol (2D6, 2C9> 1A2, 2E1, 3A4) Acebutolol, labetalol, metoprolol, pindolol (2D6) Atenolol, nadolol (renal) Possible Calcium channel blockers Amlodipine, diltiazem, felodipine, nifedipine, verapamil (3A4) Risk of CCB exposures; use with caution Diuretics Hydrochlorothiazide, furosemide, spironolactone (renal) Indapamide (2C9, 2D6, 3A4) Not expected Possible Low Not expected Treatment of Depression in HCV Place in Therapy Examples (route of metabolism) Potential DAA Interactions First Line Escitalopram, citalopram (2C19, 3A4>>2D6) 35% with TVR, no interaction with BOC Second Line Paroxetine, fluoxetine (2D6), bupropion (2B6) Sertraline (2B6>2C9/19, 3A4, 2D6), venlafaxine (2D6>3A4), desvenlafaxine (UGT>>3A4), mirtazapine (2D6, 1A3, 3A4) Low Possible Third Line Nortriptyline (2D6) Imipramine (2D6, 1A2, 2C19, 3A>UGT) Low Possible No Evidence Modafinil (3A4; induces 3A4) Amantadine (not metabolized) Possible ; DAA Not expected Avoid Duloxetine (1A2, 2D6) - CONTRAINDICATED Additive risk of hepatotoxicity Methadone Interactions Methadone is metabolized by CYP2B6, CYP2C19 & CYP3A, 85% protein bound; R-isomer is biologically active enantiomer Boceprevir interaction: In the presence of steady-state boceprevir, R-methadone AUC 16%, Cmax 10%; no clinical effects noted including opioid withdrawal Boceprevir exposures not affected by methadone Telaprevir interaction: In the presence of steady-state telaprevir, R-methadone Cmin 31%, Cmax 21% and AUC 21%, but median unbound Cmin of R-methadone was similar before and during telaprevir coadministration and no withdrawal symptoms were noted A priori methadone dose adjustments are not required when initiating DAA therapy, but close monitoring is recommended, with methadone dose adjustments if necessary Hulskotte et al. 2012, Van Heeswijk et al. 2011. Hormonal Contraceptives with DAAs Hormonal contraceptives may not be as effective in women taking boceprevir or telaprevir Boceprevir (Victrelis): 99% AUC drospirenone, 24% AUC EE Use 2 alternate effective methods of contraception during treatment with BOC and Peg IFN/RBV Drospirenone (Yaz®, Yasmin®, Angelique®) is contraindicated Telaprevir (Incivek): 28% AUC, 33% Cmin of EE Use 2 additional non-hormonal methods of effective birth control during TVR dosing and for 2 months after the last intake of TVR. Benzodiazepine Interactions Majority are substrates of CYP3A4 Risk for prolonged/excessive sedation Oral midazolam & triazolam are contraindicated with boceprevir and telaprevir IV midazolam: consider dose, close monitoring for respiratory depression or prolonged sedation Other benzodiazepines: dose and monitor Consider using benzodiazepines that are glucuronidated: Lorazepam, oxazepam, temazepam Inhaled Corticosteroids Corticosteroids are CYP3A4 substrates Potential for corticosteroid concentrations resulting in significantly reduced serum cortisol concentrations Inhaled/nasal fluticasone, budesonide: Avoid co-administration with HCV PIs if possible, particularly for extended durations. May wish to use corticosteroid associated with less adrenal suppression (e.g., beclomethasone, ciclesonide) Use lowest possible dose, consider non-steroidal options Victrelis & Incivek. Product Monographs, 2011 PDE5 Inhibitors (sildenafil, tadalafil, vardenafil) PDE5 inhibitors are substrates of CYP3A4 Potential for DAAs to concentrations Dose-related side effects (headache, vasodilation, dyspepsia, visual disturbances) Contraindicated with DAAs if using for PAH For erectile dysfunction, use a lower dose with DAAs: Sildenafil: 25 mg q48h, tadalafil: 10 mg q72h Do not use vardenafil Interactions Between HCV & HIV Medications Challenges in treating HIV/HCV co-infected patients Additive toxicities: Anemia: ribavirin, zidovudine, DAAs CNS: interferon, efavirenz Potential for negative 2-way interactions concentrations of HIV agents concentrations of HCV DAAs Antiretroviral Treatment Options for Patients on Boceprevir or Telaprevir Protease Inhibitors (PIs) Boceprevir Telaprevir Avoid with ritonavir-boosted protease inhibitors Avoid ritonavir-boosted darunavir, fosamprenavir and lopinavir Atazanavir/ritonavir OK Non-Nucleoside Reverse Transcriptase Inhibitors (NNRTIs) Integrase Inhibitor Maraviroc Nucleoside Reverse Transcriptase Inhibitors Avoid efavirenz Dose with efavirenz Etravirine (?) Etravirine OK No data Rilpivirine OK Raltegravir OK No data potential / maraviroc; potential benefit on fibrosis? Tenofovir OK Avoid AZT (anemia) Managing Drug Interactions: 1) Medication Reconciliation Ensure medication records are up to date at each visit Prescription, OTC, vitamins/herbals, recreational drugs, inhalers, topical, prn agents Confirm doses, prn drugs Include all agents that have been started or stopped Patient education: Encourage patients to ask before taking any new prescription/non-prescription drug or supplement Communication with other HCP! Managing Drug Interactions: 2) Identify Potential Interactions Use a systematic approach to identify combinations of potential concern Apply knowledge of known PK characteristics Overlapping CYP pathways, substrate, inducer, inhibitor High index of suspicion with key classes of drugs Utilize current drug information resources: Product monographs, CPS, literature Conference abstracts, specialized HCV drug interaction websites Drugs Contraindicated with Boceprevir and Telaprevir (1) 1-adrenoreceptor antagonist Alfuzosin Antiarrhythmics Quinidine, propafenone, serious/life-threatening cardiac amiodarone. arrhythmia Flecainide (TVR) Antimycobacterials Rifampin Ergot derivatives Hypotension, cardiac arrhythmia Loss of virologic response Acute ergot toxicity Herbal product St. John’s wort Loss of virologic response Statins Lovastatin, simvastatin. Atorvastatin (TVR) Myopathy including rhabdomyolysis Neuroleptic Pimozide Serious/life-threatening cardiac arrhythmia Victrelis & Incivek. Product Monographs, 2011 Drugs Contraindicated with Boceprevir and Telaprevir (2) PDE-5 inhibitor Sildenafil. tadalafil (BOC); vardenafil (TVR) Visual abnormalities, hypotension, prolonged erection, syncope Sedatives/ hypnotics Oral midazolam, triazolam Increased sedation or respiratory depression Other Cisapride, astemizole, terfenadine Serious/life-threatening cardiac arrhythmia Anticonvulsants (BOC) Carbamazepine, phenytoin, phenobarbital Loss of virologic response OC (BOC) Drospirenone Hyperkalemia Aldosterone antagonist (TVR) Eplerenone Hyperkalemia Triptans (TVR) Eletriptan Coronary artery vasospasm, MI, vent. tachycardia, VF Victrelis & Incivek. Product Monographs, 2011 Managing Drug Interactions: Therapeutic Options Determine clinical significance Evaluate therapeutic options: Alter drug dose/dosing frequency Substitute with alternate agent Can any drugs be permanently or temporarily discontinued while on DAA treatment? Consider patient convenience and cost factors Patient counselling & close monitoring is critical Summary High potential for pharmacokinetic interactions between directly acting antivirals and other drug classes Consequences may include therapeutic failure and increased toxicity Often, interactions can be managed, but heightened level of awareness is needed Use a systematic approach to identify and manage individual drug regimens Importance of a specialized, inter-disciplinary team including pharmacy Additional Resources General Hansten PD. Science Med 1998;16-25. Kashuba ADM, Bertino JS Jr. Drug Interactions in Infectious Diseases, 2nd edition, c. 2005, pp:13-39. Metheny CJ et al. Pharmacotherapy 2001;21:778-96. Interactions in HCV and HIV: Kiser J et al. Hepatology 2012;55:1620-8. Tseng & Foisy. Curr Infect Dis Rep 2012;14:67-82. Internet Toronto General Hospital Immunodeficiency Clinic; www.hivclinic.ca Liverpool Pharmacology Group; www.hep-druginteractions.org www.hcvdruginfo.ca The Canadian Liver Foundation gratefully acknowledges the participating health care professionals for their contributions to this project and for their commitment to the liver health of Canadians. The Canadian Liver Foundation (CLF) was the first organization in the world devoted to providing support for research and education into the causes, diagnoses, prevention and treatment of all liver disease. Through its chapters across the country, the CLF strives to promote liver health, improve public awareness and understanding of liver disease, raise funds for research and provide support to individuals affected by liver disease. For more information visit www.liver.ca or call 1-800-563-5483. This project made possible through the financial support of Merck Canada Inc. The views, information and opinions contained herein are those of the authors and do not necessarily reflect the views and opinions of Merck Canada Inc.