Workshop D - Quality Improvement Hub
advertisement

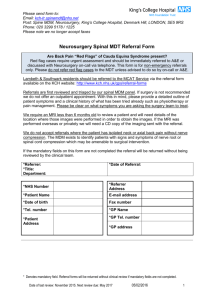
BtB - Computerised CBT The Matched Care Model STEP 4 STEP 3 STEP 2 PSYCHOLOGY BRIEF THERAPY BEATING THE BLUES STEP 1 MOODJUICE GPs BtB – Clinical Outcomes 2.50 2.00 Core Score 1.50 Before After Clinical Cut-Off 1.00 (CORE-OM Manual, 1998) 0.50 0.00 Well Being Problems Functioning Risk Mean Mean - Risk Measured Core OM scores taken at beginning of Average score taken from 77 patients. 1st and end of 8th sessions. Systems Success NUMBERS OF REFERRALS 30/04/2006 181 1400 30/04/2007 30/04/2008 836 339 30/04/2009 1040 30/04/2010 1154 30/04/2011 1133 1200 Number of Referrals 1154 1133 30/04/2009 30/04/2010 30/04/2006 30/04/2007 30/04/2008 1040 31 29 33 42 Waiting Days 34 Average1000 9 11 13 sent letter 26 referral and appointment Average Days between 24 30/04/2011 32 11 836 800 600 400 339 200 181 0 2006 2007 2008 2009 2010 2011 Reporting year (1st May to 30th April) The percentage DNA for 1st sessions = 28.7%. The percentage DNA overall = 11.7%. Average waiting time for treatment = 31 days Number of Primary Care Doctors (GPs) = 220 Percentage of Psychology Referrals = 46% The Cost COST PER PATIENT £350.00 £300.00 £250.00 £200.00 Column B £150.00 £100.00 £50.00 £0.00 1 2006 2 2007 3 2008 4 2009 2010 System becomes more efficient with increased use 2011 Where to Start Phases of Implementation 1) 2) 3) DEVELOPMENT OF OBJECTIVES IDENTIFY RESTRICTIONS CONSIDER WIDER IMPACT Objectives impact on all phases of implementation 4) 5) DESIGN OF SERVICE MODEL DEVELOP IMPLEMENTATION STRATEGY 6) 7) IMPLEMENTATION OF MODEL MARKETING OUTCOME: SUSTAINABLE SERVICE WHICH ACHIEVES OBJECTIVES Impact of Objectives and Restrictions OBJECTIVES; RESTRICTIONS; EFFICIENCY, MAXIMUM CAPACITY, ACCESSIBLE, MINIMAL WASTAGE • • • • Maximum numbers of patients seen Accessible across the region Efficiency of patient access Minimise DNA's FUNDING, ACCESS TO CLINICAL STAFF • Changes administration of services • May limit accessibility to service across region, will impact on referrals • Limits growth and may lead to restricted development of service • Limited access to clinical input Combination of Objectives and Restrictions provides foundation of service design and implementation Example Models Forth Valley and Tayside – Aims; efficiency, maximum capacity, accessible Locations distributed across region Clinical responsibility remaining with referrer Different clinical models applied in psychology and GP’s Phased developments with capacity expanding due to needs and readiness of service Target time for referral to appointment System working to maximum levels of patient throughput allowed by targets Service part of matched/stepped care systems for added patient support Additional Aim in Tayside – minimal wastage of treatments Assign further appointment to patients that DNA A Working Service Access Across a Region Service proves accessible by spreading machines across entire region including rural and deprived areas supported by onsite administrators Location vary greatly in style but not quality of service through combination of right location, good training and consistency of treatment. Referral Routes Systems run in parallel Direct GP Access Point of Referral to Beating the Blues Upon patients are either discharged or offered further treatment GPs have option of referring to psychology to gain access Psychology and Other Mental Health Services Patients attend treatment, referrers kept informed of progress with Progress Reports Patients assessed for suitability Patients are given exit interview to determine success of program Multiple streams of referral can be developed with minimal variation in process Central Processing MACHINE LOCATIONS Location contacted, appointment arranged Central Coordination of all initial appointments, across all locations Patient contacted and asked to attend appropriate location All refers use single point of access and standardised referral form KEY ADVANTAGES • Monitoring flow of referral • Diverting patients to prevent waiting times • Increased support of locations and patients • Connection to psychology • Addressing Suicide Alerts REFERS Key Aspects for Success The Right Workforce Key Requirements • Point of contact in relation to referral and enquiry • Ability to address clinical issues and make informed decisions • Co-ordinate and develop service • Address IT issues as they arise • Motivate and maintain high levels of communication Clinical vs. Customer Services Experience Costs of clinical staff is high Clinical support is only required on few occasions Assess support network and position of service Non-clinical equals less threatening Availability to staff is essential • Be available Development of the correct intra-structure and systems will enable the minimisation of staffing needs and therefore costs Forth Valley employs a single coordinator to run service with customer services and IT background Communication With Referrers and Users Good communication with referrers = flexibility in service and the ability to manage referral patterns, clinical issues and support for future work Development of a clear understanding between referrers and service Efficiency when dealing with referrer requests either on a service or patient basis Recognition of referrer skills and abilities to determine best course of action for patient? Maintenance of links through updates and continued contact Good communication with patients = greater motivation, increased patience with program, better outcomes for patient Development of a clear understanding of program, its benefits and the need to complete course (this particularly on getting them past first two sessions) Support and assist users to overcome any barriers that prevent the completion of course Be accessible at all times and have the required information and understanding at finger tips Friendly, approachable and non-threatening Marketing/Education Marketing to referrer groups = increase in referrals Requirements Outcomes/Actions Marketing Strategy Development of clearer defined targets, messages and requirements based on original service aims Delivery of Key Messages Creates clear understanding of what BtB does, who it is for and how to access service. Delivery of messages is dependant on scale Scale Targets generated from objectives, will focus on the numbers of referrals to be generated and desired impact of service Timing Marketing to different groups and levels needs to be timed around service development to ensure controlled increase of referral and use Key outcome of marketing would be integration into clinical structures and practice Our Advice Genuine commitment to development and running service Dedicated team with right individuals to implement and then run service Allow focus to remain on patient by ensuring efficiency of process and administration Do not over complicate the service and administration systems Clearly defined responsibilities Develop clear lines of communication with referrers and patients Look to integrate service into exists structures Get the right clinical and managerial support structures in place before you start Approaching the service with the right mind set is essential Clearly define objectives and requirements before thinking about logistics of service Do not underestimate complexity and subtly of task, having the right understanding and drive to develop the service within those involved is essential The Local Impact Features of the Forth Valley Matched Care Model comments from Head of Primary Care Psychology It has doubled the number of people receiving psychological therapy – 1100 new referrals a year to BtB The waiting time for individual therapy has decreased. Before the start of the system, it was up to 2.5 years, now it is no more than 6 months The waiting time for other forms of psychological therapy (non-individual) is lower than this, meaning that a far higher proportion of people are meeting the 18 week waiting time target for psychological treatment Audit of BtB has revealed that referrals are appropriate and treatment is effective The mild to moderate system is now having a significant impact on the population of Forth Valley. There are about 12000 new case of depression and anxiety in per year about 2000 (or 1 in 6) are receiving specialist psychological treatment, in addition to the people accessing Moodjuice (a total of 110,000 selfhelp resources are delivered through Moodjuice a year) Preliminary data suggests that BtB is helping reduce the increase in antidepressant prescribing by GPs Greatest impact was achieved by integrating mild to moderate stepped care into existing service models and local structures such as GP Enhance Service.