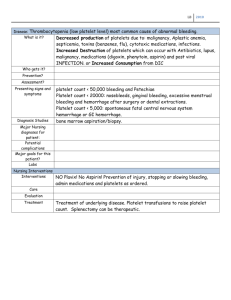
Point-of care evaluation of coagulation: technical aspects
advertisement

Point-of care evaluation of coagulation: technical aspects, indications, limitations, pitfalls Andreas Calatzis Institute for Prevention of Cardiovascular Diseases University of Munich Disclosure of commercial interest: The author is a coinventor of the ROTEM and Multiplate analyzers and CEO of Verum Diagnostica, Munich (manufacturer of the Multiplate system), which is a 100% subsidiary of Roche. Bleeding in Surgery Causes liver dysfunction bone marrow dysfunction renal dysfunction hereditary disorders trauma hemodilution consumption coagulopathy heparin artificial surface contact anti-platelet drugs clotting factors concerns platelets fibrinolysis Platelet Function Main Mechanisms positive feedback release of ADP positive feedback formation of Thromboxane A2 via COX hemostasis during operation, trauma, menstruation, after injuries stent thrombosis myocardial infarction ischemic stroke other ischemic events aggregation via GpIIbIIIa (fibrinogen receptor) Platelet Function Inhibitors Main Mechanisms positive feedback release of ADP positive feedback formation of Thromboxane A2 via COX hemostasis during operation, trauma, menstruation, after injuries stent thrombosis myocardial infarction ischemic stroke other ischemic events aggregation via GpIIbIIIa (fibrinogen receptor) Point-of-care testing – definition Methods, which are applied - in a near-patient setting - in environments other than classical laboratories (e.g. ICU or OR) - which can be applied by personnel without extensive laboratory education (NB: national regulations may apply) Synonyms - „near patient testing“ - “bedside testing" - "alternative site testing" Point of Care Testing why? - fast availability of results - targeted coagulation management (e.g. of bleeding complications) - simplified workflow (TAT shorter, no transport of sample, no transmission of results between laboratory and POC site), however additional effort for performing the test at the point of care Point of Care Testing why? - fast availability of results - targeted coagulation management (e.g. of bleeding complications) - simplified workflow (TAT shorter, no transport of sample, no transmission of results between laboratory and POC site), however additional effort for performing the test at the point of care But: - costs are often higher than for the laboratory analysis - important to define roles and responsibilities - quality management important Point of care evaluation of coagulation – parameters immunologic tests D-Dimer plasmatic coagulation ACT, PT, aPTT viscoelastic tests ´ ROTEM, TEG, Sonoclot platelet function tests PFA-100 / 200, Multiplate, Verifynow Parameters that are available in the laboratory and in the POC D-Dimer PT and aPTT Advantages: - short TAT - faster therapeutic decisions - in out-patient care: patient can get his result immediately, therapeutic consequence can be discussed (e.g. Warfarin therapy) Parameters that are available in the laboratory and in the POC D-Dimer PT and aPTT NB: - only the INR is (relatively) well standardised - results of different aPTT, ACT, or D-Dimer assays should be reported seperately in laboratory information systems or in the patient file to circumvent misinterpretations (changes of the values which rely on different assay systems could be misinterpreted as therapeutic effects or changes in the course of disease) Example: Differences between POC D-Dimer assays vs. the reference method Int. Jnl. Lab. Hem. 2012, 34, 495–501 Parameters that are available in the laboratory and in the POC D-Dimer PT und aPTT Not every instrument is equally well suited for the analysis of hemodiluted samples or other altered samples from the ICU or OR Applicability of the particular method in the context of the patient sample should be verified (e.g. specifications by manufacturer, publications, in house validation) Activated Clotting Time (ACT) blood + contact phase activation detection of clotting time is mainly applied to monitor UFH therapy several different instruments available: poor standardisation relatively weak correlation to actual heparin concentration low sensitivity towards LMWH or pentasaccharide Viscoelastic methods: ROTEM, TEG and Sonoclot: Background • mechanical, quantitative and continuous assessment of clot formation in whole blood • coagulation activation, clot formation and clot stability or fibrinolysis are recorded Viscoelastic methods: ROTEM, TEG and Sonoclot: Detection principle • Clot firmness is continuously recorded via the elasticity (ROTEM / TEG) or clot resonance (Sonoclot) • ROTEM and TEG significantly more popular than Sonoclot ROTEM Principle: Relative movement of Cup (7) and Pin (6): 4,75° Sonoclot principle aus: Hartert H., Klin. Wochenschrift 26: 577−583 (1948) aus: Hartert H., Klin. Wochenschrift 26: 577−583 (1948) aus: Hartert H., Zschr. f. d. ges. exp. Medizin 117: 189−203 (1951 aus: Hartert H., Klin. Wochenschrift 26: 577−583 (1948) Haemoscope TEG 2 channels leveling required manual pipetting platelet mapping assay very expensive very few clinical publications ROTEM 4 channels for parallel tests robust detection system using a ball bearing (ROTEM) electronic pipetting ROTEM delta 4 channels touch screen broad menu of tests: EXTEM INTEM HEPTEM FIBTEM APTEM Single test reagents available Viscoelastic methods: ROTEM, TEG and Sonoclot: Applications Hemostasis management in patients with complex coagulation disorders: - trauma - surgery (vascular surgery, GI surgery, orthopedics …) - obstetrics Viscoelastic methods: ROTEM, TEG and Sonoclot: pros and cons + comprehensive and clinically relevant information on the coagulation status of patients + increasing evidence on the improvements in the coagulation management (less costs, less bleeding) via a targeted coagulation management vs. conventional “empiric” coagulation therapy + implementation of viscoelastic methods increases the understanding and education on coagulation alterations in anesthesia and intensive care - low sensitivity for Warfarin, LMWH, NOACs - no detection of VWS, Aspirin, Clopidogrel - additional efforts and costs Percutaneous tracheostomy • • • • Thrombo: 33.000/µl PZ: 66% aPTT: 40,4 sec Fibrinogen: 413 mg/dl Clinical case 1 Patient 68 years old, elective CABG x3, (ASA 100 mg 1xd) extracorporeal circulation 99 min, ischemia 71 min, severe postoperative bleeding After 2 g Tranexamic acid and 4 g Fibrinogen Stop bleeding Clinical case 2 Patient 88 years old, elective aortic valve replacement and CABG x 2, extracorporeal circulation 79 min, aortic clamp 54 min, severe postoperative bleeding After 2 g Tranexamic acid and 4 g Fibrinogen Stop bleeding Clinical case 3 Patient 75 years old, rheumatic and ischemic heart disease, elective mitral and aortic valve replacement + CABG x1, extracorporeal circulation 184 min, aortic clamp 119min, severe postoperative bleeding (myelodisplastic disease with thormbocytopenia, Thrombocytes 42 G/l) Platelets 5 units Fibtem MCF OK Thrombocytes 118 G/l Stop bleeding PFA-100/200 Principle high shear rate >5000 /s Epinephrine or ADP membrane with collagen coating red cell platelet FLOW capillary 200µm citrated blood is aspirated through a small aperture in a collagencoated membrane Platelets adhere to the collagen surface and lead to a cessation of blood flow parameter = Closure Time (CT) 3 cartridges: - EPI: costimulation by: shear stress, collagen, epinephrin - ADP: costimulation by: shear stress, collagen, ADP - P2Y: costimulation by: shear stress, ADP, PGE1 and Ca++. Siemens PFA-100/200 Innovance P2Y Cartridge No predictivity for stent thrombosis or bleeding n=588 Popular study. JAMA. 2010 Feb 24; 303(8):754-62. updated data from 06-2011 In the only clinical study so far on the new PFA-100 P2Y cartridge clopidogrel low responders according to PFA-100 had less stent thromboses, less trokes and less target vessel revascularisations compared to clopidogrel responders. The Kaplan-Meier curves divided only after 190 days, which makes any use of this cartridge for the clinical management highly questionable. There was no predictivity of the PFA-100 tests for bleeding events found in this study. PFA-100 / 200: Pros / Cons + widely used easy-to use method + high sensitivity for von Willebrand Disease and Aspirin - few studies with clinical endpoints - most studies on prediction of bleeding are negative - only clopidogrel test on the market that has never shown predictivity for stent thrombosis - main element of proof for preoperative screening (Koscielny et al, CATH 2004) is actually statistically wrong Accumetrics Verifynow Principle Mixing Chambers/ Detection Well Accumetrics Verifynow Principle / Assays platelet function testing in whole blood optical detection of platelets aggregating on fibrinogen-coated polystyrene beads fully automated one tube of blood (2 ml) required per test Assays: Aspirin assay: stimulation of platelets by arachidonic acid P2Y12 assay: stimulation of platelets by ADP + PGE1 IIbIIIa assay: stimulation of platelets by iso-TRAP Mixing Chambers/ Detection Well Accumetrics Verifynow Pros and Cons + very easy to use + some data on prediction of stent thrombosis - most studies on prediction of bleeding were negative - almost no data on use of Verifynow in anesthesia - recently two large negative studies on the clinical management of platelet inhibitors using Verifynow: - GRAVITAS (Price et al, JAMA) - ARCTIC (Collet et al, NEJM) Mixing Chambers/ Detection Well Multiplate® Detection principle analysis of platelet function in whole blood twin impedance sensor platelets aggregate on metal sensors and increase electrical resistance platelet function analysis on surfaces Multiplate® analyzer 5 channels for parallel tests electronic pipetting applicable for laboratory and near patient analysis Example: Near-patient use of Multiplate in combination to TEG Multiplate Main tests TRAPtest TRAP TXA2 ADPtest ADP TXA2 ASPItest Arachidonic Acid Aspirin ® NSAID activation inhibition Clopidogrel Prasugrel Ticagrelor GpIIb/IIIa antagonists: COX Reopro ® (abciximab) Aggrastat ® (Tirofiban) Integrillin ® (Eptifibatid) Multiplate tracings Examples TRAPtest no platelet inhibition 113 U ASPItest 102 U ADPtest 89 U 17 U 100 mg aspirin qd 139 U 134 U 31 U 75 mg clopidogrel qd 98 U 100 mg aspirin + 75 mg clopidogrel qd 89 U 8U 17 U 3U 3U 88 U tirofiban (Aggrastat® i.v.) 7U case report: trauma patient H. Schöchl, AUVA Trauma Centre, Salzburg case report: trauma patient 52 yo male • Motorcycle race • multiple trauma • ISS: 34 severe bleeding H. Schöchl, AUVA Trauma Centre, Salzburg case report: trauma patient 52 yo male • Motorcycle race • multiple trauma • ISS: 34 severe bleeding laboratory analysis: Hb: 10,4g Plt: 193.000/µl PT: 70% aPTT: 31,4sec Fbg: 127 mg/dl acceptable H. Schöchl, AUVA Trauma Centre, Salzburg platelet function ? platelet function ? platelet function ? abnormal platelet function due to dual anti-platelet therapy most likely the reason for the bleeding complication 1 month follow-up OR 9.8 JACC 2009 Mar 10;53(10):849-56. Am Heart J. 2010 Aug;160(2):355-61. 5-10 x increased risk for ST, q-wave MI and stroke for clopidogrel low-responders (20% of the patients) very low (=prasugrel-like) risk for clopidogrel „responders“ (80% of the patients) Multiplate Clopidogrel monitoring: prediction of bleeding cut-off TIMI major bleeding 500 500 0 0 200 200 400 400 600 600 800 800 1000 1000 1200 1200 2,0 300 300 major bleeding (%) Number Number of of patients patients (n) (n) 400 400 Sibbing D et al, JTH 2010 n=2533 200 200 100 100 2.6x 1,5 P=0.005 1,0 0,5 n = 975 0,0 High responders n = 1558 Remaining patients 0 0 0 0 200 200 400 400 600 600 800 800 1000 1000 platelet ADPADP-induced induced aggregation ADP-induced platelet aggregation aggregation (AU*min) (AU*min) 1200 1200 Cardiac surgery in patients pre-treated with thienopyridines Prediction of excessive bleeding „The main finding of our study is that the MEA ADPtest in patients under thienopyridine therapy undergoing cardiac operations is independently associated with the postoperative bleeding and transfusion of fresh frozen plasma and platelets after the operation, and it provides an accurate preoperative prediction of patients who will suffer from excessive postoperative bleeding.“ „Only 8% of the patients with an MEA ADP test AUC greater than 31 U experienced excessive bleeding.“ 31 U Ranucci M et al. Multiple electrode whole-blood aggregometry and bleeding in cardiac surgery patients receiving thienopyridines. Ann Thorac Surg. 2011 Jan;91(1):123-9. Anesthesia / Intensive Care 2012 guidelines The Society of Thoracic Surgeons Clinical Practice Guidelines “For patients on dual antiplatelet therapy, it is reasonable to make decisions about surgical delay based on tests of platelet inhibition rather than arbitrary use of a specified period of surgical delay”. Class of Recommendation IIa, Level of Evidence B “Point-of-care testing to assess perioperative platelet function may be useful in limiting blood transfusion”. Class of Recommendation IIb, Level of Evidence B “Assessments of platelet function with devices such as … Multiplate analyzer, VerifyNow, and PFA-100 proved useful in predicting increased bleeding risk”… Point-of-care platelet function testing can guide perioperative transfusion management and reduce blood component utilization [77, 78]. … Multiplate analyzer, and PFA-100 are used as part of point-of-care–guided transfusion algorithms”. Ann Thorac Surg. 2012 Nov;94(5):1761-81. Clinical case 4 Patient 64 years old, elective CABG x5, (ASA 100 mg 1xd and Plavix 75mg 1xd until operation), severe postoperative bleeding OK ADP receptor inhibition by clopidogrel Platelets 5 units Stop bleeding Clinical case 5 NSTEMI CABG X4 after loading dose (180mg) and 48h therapy of tigagrelor 90mg tid 8U Strong ADP receptor ihnibition Platelets 5 units 14U Persist poor ADP receptor activity potentially inhibition of transfused platelets by the reversible ADP receptor antagonist Ticagrelor (Brilique) Mortality-free survival rate A prospective study of the use of point of care coagulation testing (including Multiplate) for the management of coagulopathy in cardiac surgery – Effect of point of care testing on mortality n=100 Kaplan–Meier curve demonstrating survival by type of performed coagulation management during the 6-month follow-up period (4% vs. 20%; p=0,013) . Weber CF at al, Anesthesiology. 2012 Sep;117(3):531-47 A prospective study of the use of point of care coagulation testing (including Multiplate) for the management of coagulopathy in cardiac surgery – Effect of point of care testing on blood loss Postoperative chest tube blood loss (ml) 2500 p = 0.021 n=100 Conventional group p = 0.003 2000 1500 Point-of-care group p = 0.015 1000 500 0 n = 50 n = 50 n = 50 6 n = 50 12 Time (hours) Weber CF at al, Anesthesiology. 2012 Sep;117(3):531-47 n = 43 n = 35 24 A prospective study of the use of point of care coagulation testing (including Multiplate) for the management of coagulopathy in cardiac surgery – Effect of point of care testing on costs Cumulative costs in Euro [€] for applied hemostatic therapies conventional group POC-guided group Packed erythrocytes [72 €/U] 18,648 13,176 FFP [0.162 €/g] 13,530 4,665 PC [231 €/U] 28,755 15,123 Fibrinogen [233 €/g] 35,882 27,727 PCC [114 €/600 IU] 10,944 6,726 rVIIa [2,784 €/240 kIU] 44,544 5,568 Total blood products and hemostatic therapy 155,531 76,397 ̶ ̶ 4,093 2,427 155,431 82,918 3,109 1,658 ROTEM® test costs Multiplate® test costs Cumulative [€] Mean costs per patient [€] FFP = fresh frozen plasma; IU = international units; PC = pooled platelet concentrate; PCC = prothrombin complex concentrate; rVIIa = recombinant activated factor VIIa concentrate. Lower costs in the guided group Platelet dysfunction before surgery Consequences Potential consequences: Be prepared! check that platelet concentrates / other therapeutic options are available experienced staff? less traumatic approach / surgical approach with good visability ? consider to use less / no colloids / less aggressive hemodilution Reversible reason for the dysfunction? (e.g. patient was on clopidogrel) consider waiting 1-3 days till the operation Platelet function testing during bleeding complications Consequences Platelet function normal or close to normal: platelets are rather unlikely to be the cause of the bleeding check other reasons for bleeding first (plasmatic factors, fibrinolysis, fibrinogen, surgical bleeding?) Platelet function abnormal: platelets are a potential cause for the bleeding complication consider application of platelet concentrates or desmopressin (Minirin ®) laboratory analysis vs. Point of Care analysis usually lower reagent costs usually shorter turn-around-time personnel with education in laboratory analysis allows the targeted management of coagulation disorders environment with established quality management procedures better understanding of the clinical context of the samples which are analyzed (treatments, preanalytics) larger menu of tests available (antithrombin, D-Dimer, fibrinogen) analysis of “young” samples (samples analyzed in the laboratory may be up to 3-4 hours old) POC diagnostics are preferable when … the transport of the sample to a laboratory is not feasible or not practicable or the POC diagnostics contributes to an improved patient treatment (time / costs / targeted treatment) > Choice of method Question ? Consequence ? Ressources ? - staff - logistics - know how Urgency ? Test Consequence thank you for your attention ! ? “A total of 5649 unselected adult patients were enrolled to identify impaired hemostasis before surgical interventions…. The sensitivity of the PFA-100: collagenepinephrine was the highest (90.8%) in comparison to the other screening tests (BT, aPTT, PT, vWF: Ag). The positive predictive value of the PFA-100: collagenepinephrine was high (81.8%), but the negative predictive value was higher (93.4%). “ >100 x citations “A total of 5649 unselected adult patients were enrolled to identify impaired hemostasis before surgical interventions…. The sensitivity of the PFA-100: collagenepinephrine was the highest (90.8%) in comparison to the other screening tests (BT, aPTT, PT, vWF: Ag). The positive predictive value of the PFA-100: collagen-epinephrine was high (81.8%), but the negative predictive value was higher (93.4%). “ What was evaluated? anamnestic evaluation coagulation tests no significant difference between PFA-100 in pts with and without a bleeding history correlation with bleeding was not evaluated ??? where do the 90% sensitivity come from ??? no significant difference between PFA-100 in pts with and without a bleeding history correlation with bleeding was not evaluated ??? where do the 90% sensitivity come from ??? patients with abnormal coagulation tests were stratified as “impaired hemostasis”. Then based on the same tests that were used to define “impaired hemostasis” the sensitivity and specificy was calculated no significant difference between PFA-100 in pts with and without a bleeding history correlation with bleeding was not evaluated ??? where do the 90% sensitivity come from ??? using this method a dice would also have 90% sensitivity and specificity patients with abnormal coagulation tests were stratified as “impaired hemostasis”. Then based on the same tests that were used to define “impaired hemostasis” the sensitivity and specificy was calculated