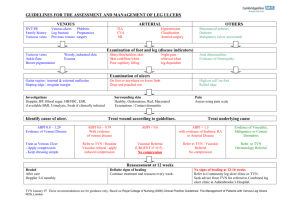
Management of patients with venous leg ulcers
advertisement

The management of patients with venous leg ulcers Audit Protocol The management of patients with venous leg ulcers Audit Protocol Acknowledgements Produced by the Dynamic Quality Improvement Programme, RCN Institute in conjunction with the Clinical Governance Research and Development Unit, Department of General Practice and Primary Health Care, University of Leicester We should like to thank the following who undertook peer review of this protocol. Steering group: Carol Dealey, Andrea Nelson, Edward Dickinson, Karen Jones, Lesley Duff Advisory Panel: Richard Baker, Ian Seccombe, Mary Clay, Julia Schofield, Sir Norman Browse, Sara Twaddle Users group: Dawne Squires, Sarah Pankhurst, Kath Robinson, and Kate Panico Protocol developed by Xiao Hui Liao, Francine Cheater The National Sentinel Audit Project for the Management of Venous Leg Ulcers, from which this audit protocol was developed, was funded by the NHS Executive, Department of Health Published by the Royal College of Nursing, 20 Cavendish Square, London W1M OAB Management of patients with venous leg ulcers Audit protocol Publication code 001 269 ISBN 1-873853-89-0 July 2000 Price RCN members: £3.50 RCN non-members: £4.50 The management of patients with venous leg ulcers Contents 1. Introduction Why an audit of patients with leg ulcers Background of national sentinel audit What is included in the protocol How to use this protocol Which patients are included Evidence grading 2 2 2 2 2 3 3 2. Summary of criteria The criteria - assessment The criteria - management The criteria - cleansing, dressing, contact sensitivity 4 5 13 15 3. Introducing change 19 References 20 Sources of further information 23 Appendix 1 -Documentation 24 Appendix 2 -Audit Form 24 The management of patients with venous leg ulcers Contents 1 1. Introduction A. Why an audit of patients with leg ulcers? The total cost to the NHS of treating leg ulcers is estimated to be as high as £600 million a year (Douglas et al 1995). audit tools, the RCN and its project partners will be able to help local teams improve the quality of care to patients. It is hoped that results will be collated nationally in an anonymised form to enable comparative data analysis to take place. This will allow individual teams to benchmark their performance against others, and by establishing regional networks, to share good ideas and learn from the experiences of colleagues. A recent Effective Health Care Bulletin on compression therapy for venous leg ulcers concluded: “There is widespread variation in practice, and evidence of unnecessary suffering and costs due to inadequate management of venous leg ulcers in the community.” (NHS Centre for Reviews and Dissemination, 1997) The initial project in which this audit protocol was piloted was led by a collaborative partnership, coordinated by the RCN Dynamic Quality Improvement Programme, a steering group of representatives from other professional organisations, and an advisory group of experts in the management of leg ulcers. Epidemiological data suggest that between 1.5-3.0 per 1000 of the population have active leg ulcers (Fletcher et al 1997), and the prevalence increases to 20 per 1000 in people over 80 years-of-age. Experience from initiatives set up to improve community-based nursing management of leg ulcers (Moffat et al 1992; Thompson, 1993) highlighted the potential for more clinical and cost-effective practice through more widespread adoption of evidence-based interventions. C. This protocol was originally developed for the national sentinel audit management of leg ulcers. It contains: ◆ ◆ B. Background for national sentinel audit for leg ulcers The National Sentinel Audit Project for the management of venous leg ulcers was funded by the NHS Executive for an 18-month period. The aim was to pilot a methodology to improve the quality of care for leg ulcer patients in terms of clinical and cost effectiveness. Evidence-based review criteria were developed, based on the national guideline: ‘Clinical practice guidelines for the management of patients with venous leg ulcers: recommendations for assessment, compression therapy, cleansing, debridement, dressings, contact sensitivity, training/ education and quality assurance’ (RCN et al 1998). Methods of data collection have been developed drawing on the experience of practitioners, alongside the process of agreeing the evidencebased review criteria. Twenty pilot sites were recruited to help the project team to test the development of the audit package and methodology. The projrct team is grateful to the participating sites for their input and feedback in the development of the audit form. The purpose of clinical audit is to improve the quality of care to patients locally. It is intended that by providing nationally-produced guidelines and 2 The management of patients with venous leg ulcers ◆ ◆ ◆ instructions to community nurses on how to conduct the audit detailed explanation and justification of the criteria from research evidence criteria prioritised according to the strength of the research evidence and impact on the outcome (Baker et al 1995) data collection form brief advice about change. D. How to use this protocol Planning the audit A project leader must be identified who will take responsibility for involving clinical staff. Involvement in a clinical audit project is about developing clinical practice, not just collecting data. It is vital that the project leader seeks to enable clinical staff to improve the service. Further information on this can be found in the implementation guide. If you are using this audit protocol as a part of a regional or national project, comparing your results with others, you will need to audit all the criteria. If you are using this protocol locally you may choose only to use the ‘must do’ criteria. You may wish to add criteria which refer to protocols for organising care locally. Ethical issues will also need to be considered at the planning stage. It is important to ensure that local procedures for ethical approval are followed. Introduction Introduction Data collection - one form per patient You should use one data collection form for each individual patient. It is recommended that the data collection will last for a three month period. The completed form should be sent back to the project leader in your organisation. E. Which patients are included in the audit? The protocol has been designed for community nurses working in leg ulcer clinics as well as home care-based practice. Leg ulcers are defined as areas of “loss of skin below the knee on the leg or foot which take more than six weeks to heal” (Effective Health Care Bulletin 1997). Patients diagnosed with venous leg ulcers are included in the project. This includes new patients, patients who are in the process of treatment and patients who have a recurrent ulcer. For more detailed criteria, please read the Instruction for Audit Form in Appendix 2 before you complete the form. F. The evidence, on which the guideline recommendations from which the audit criteria were developed, was graded as follows: I Generally consistent findings in a majority of multiple acceptable studies. II Either based on a single acceptable study, or a weak or inconsistent finding in multiple acceptable studies. III Limited scientific evidence that does not meet all the criteria of acceptable studies, or absence of direct studies of good quality. This includes published or unpublished expert opinion (Waddell et al 1996). The management of patients with venous leg ulcers Introduction 3 2. Summary of Criteria Assessment 1. The records show that at the first assessment*, a clinical history (ulcer history, past medical history), physical examination (blood pressure measurement, weight, urinalysis) has been undertaken. 2. The records show that on the first assessment, the ankle/brachial pressure index (ABPI) has been measured. 12. The records show that products containing lanolin or other potential allergens have not been used on the patient. 13. The records show that topical antibiotics have not been used on the patient. * First assessment - a full assessment takes place within two weeks of first contact with the patient 3. The records show that the ulcer size and wound status (edge, base, position, surrounding skin) is documented at the first assessment. 4. The records show a referral via general practitioner to a specialist has been made in the following situations: the ABPI is <0.8; the patient is diabetic; there is suspected malignancy; foot infection; healing has not started after 12 weeks of compression bandaging. 5. The records show that a bacterial swab has only been taken when there is evidence of clinical infection for example, pyrexia, cellulitis, increased pain and rapidly enlarging ulcer. 6. The records show that on the first assessment, the patient’s pain level has been assessed and where indicated, appropriate management commenced. 7. The records show that the measurement of ABPI has been undertaken at least three monthly or in any of the following situations: sudden increase in size of ulcer; ulcer becomes painful; change in colour/temperature of foot/leg). Management 8. The records show that patient with venous leg ulcers and an ABPI ≥ 0.8 has received high compression (multi-layer e.g. four-layer, threelayer or short stretch) bandaging. 9. The records show that the patient with a healed ulcer has been educated about the need to wear, and how to correctly apply, compression stockings. 10. The records show that when wound cleansing is indicated, tap water or saline has been used for cleansing. 11. The records show that the patient has received simple, low-cost, non-adherent wound dressings unless more costly dressings are indicated (for example, odour, and excessive exudate). 4 The management of patients with venous leg ulcers Summary 2.1 Assessment of Patients with Leg Ulcers 1. The records show that at the first assessment, a clinical history (ulcer history, past medical history), physical examination (blood pressure measurement, weight, urinalysis) has been undertaken. Justification Lack of appropriate clinical assessment of patients with limb ulceration in the community has often led to long periods of ineffective and often inappropriate treatment (Cornwall et al 1986; Roe et al 1993; Stevens et al 1997; Elliott et al 1996). In addition, inadequate diagnosis of ulcers of arterial origin (Callam et al 1987a) leading to inadequate treatment can have serious adverse consequences for the patient (for example, ischaemia). It is essential, therefore, that a patient presenting with leg ulcers has a thorough clinical history and physical examination (Callam and Ruckley 1992). The clinical history and physical examination will assist the identification of both the underlying cause of leg ulcers and any associated diseases, and will influence decisions about prognosis, referral, investigation and management. If the practitioner is unable to conduct a physical examination, they must refer the patient to an appropriately trained professional. Ulcer history Guideline recommendations indicate that information relating to ulcer history should include: the year of occurrence of the first ulcer; the site of the ulcers and of any previous ulcers; the number of previous episodes of ulceration; the time taken to heal in previous episodes; the time free of ulcers; past treatment methods; previous and current use of compression hosiery (RCN et al 1998). The ulcer history will enable consideration of clinical factors that may impact on treatment and healing progress, as well as provide baseline information on ulcer history. Medical history Taking a medical history is an important part of the assessment to identify the type of ulcer. The person conducting the assessment must be aware that ulcers may be arterial, diabetic, rheumatoid or malignant and should record any unusual appearance. This will assist the accurate identification of the aetiology of the ulcer, which has major implications for treatment choice (RCN et al 1998). The management of patients with venous leg ulcers Although methods and populations make comparison between studies difficult, there is general consensus on the aetiological factors and the medical criteria used to define venous, nonvenous and mixed aetiology ulcers (Alexander House Group 1992). Arterial Ulcers - caused by an insufficient arterial blood supply to lower limb, resulting in ischaemia and necrosis (Belcarno et al 1983; Carter 1973). Rheumatoid ulcers - are commonly described as deep, well-demarcated and punched-out in appearance. They are usually situated on the dorsum of the foot or calf (Lambert and McGuire 1989) and are often slow to heal. Diabetic ulcers - are usually found on the foot, often over a bony prominence such as the bunion area, or under the metatarsal heads, and usually have a sloughy or necrotic appearance (Cullum and Roe 1995). An ulcer in a diabetic patient may have neuropathic, arterial and/or venous components (Browse et al 1988; Nelzen et al 1993). It is essential to identify the underlying aetiology. Malignant ulcers - are a rare cause of ulceration and exceptionally are a consequence of chronic ulceration (Yang et al 1996; Baldursson et al 1995; Ackroyd and Young 1983). Physical examination A good examination of the legs and the ulcers is important to recognise the signs of chronic venous insufficiency and arterial disease. Venous disease The ulcer is usually shallow (usually on the gaiter area of leg) and may be associated with oedema, eczema, ankle flare, lipodermatosclerosis, varicose veins, hyperpigmentation, atrophie blanche. Arterial disease The ulcer has a ‘punched out’ appearance, and the base of wound is poorly perfused and pale. Other symptoms may include: cold legs/feet; shiny, taut skin; dependent rubour; pale or blue feet; gangrenous toes. Assessment 5 2.1 Assessment of Patients with Leg Ulcers Mixed venous/arterial The ulcers have features of venous ulcer in combination with signs of arterial impairment. To assist in determining the type of ulcer the criterion used for examining the appearance of the ulcer is based on consensus statements, and literature reviews that concur on well-known features of the different types of ulcers (Browse et al 1988; Alexander House Group 1992). Other important elements of the assessment include taking the patient’s blood pressure, weight and a urinalysis. Blood pressure is taken to screen for hypertension, and urinalysis is taken to screen for undiagnosed diabetes mellitus. Although there is some empirical evidence of inadequate assessment in practice, there are no studies that examine patient outcomes that compare people who are given, or not given the benefit of a full clinical history and physical examination. The recommendations for what should comprise a clinical history and physical examinations are therefore based on consensus opinion (RCN et al 1998). Strength of evidence III 6 The management of patients with venous leg ulcers Assessment 2. The records show that on the first assessment, the ankle/brachial pressure index (ABPI) has been measured. 3. The records show that the ulcer size and wound status (edge, base, position, surrounding skin) is documented at the first assessment. Justification Justification Measurement of ABPI is to enable identification of arterial disease for referral to specialist vascular clinics and to assess the appropriateness for compression bandaging. All patients must be given the benefit of Doppler ultrasound measurement of ABPI by an appropriately trained professional. This prevents misdiagnosis that could result in inappropriate therapy, with possibly serious adverse consequences for the patient. A detailed assessment and accurate written record of ulcer characteristics should include the size, the edge, and the base, position of the ulcer and its surrounding skin. Research suggests that diagnosis should not be solely based on the absence/presence of pedal pulses because there is generally poor agreement between manual palpation and ABPI (Brearley et al 1992; Callam et al 1987b: Moffatt et al ,1994). Two large studies have shown that 67% and 37% of limbs respectively with an ABPI of <0.9 had palpable foot pulses, with the consequent risk of applying compression to people with arterial disease (Moffatt et al 1995; Callam et al 1987b). Serial measurement of size (length and width) of the ulcer is a reliable index of healing. Appropriate techniques include tracing of the margins, measuring the two maximum perpendicular axes, or photography (Stacey 1991). The ulcer edge often gives a good indication of progress and should be carefully documented (for example, shallow, epithelialising, punched out, rolling). The base of the ulcer should be described (for example, granulating, sloughy, and necrotic). The position of the ulcers should be clearly described (SIGN 1998). Strength of evidence III The importance of making an objective assessment of the ulcer by measuring ABPI is highlighted by a number of studies (Nelzen et al 1994; Moffatt et al 1994; Simon et al 1994). Strength of evidence IAssessment of Patients with Leg Ulcers The management of patients with venous leg ulcers Assessment 7 2.1 Assessment of Patients with Leg Ulcers 4. The records show a referral via general practitioner to a specialist has been made in the following situations: the ABPI is <0.8; the patient is diabetic; there is suspected malignancy; foot infection; healing has not started after 12 weeks of compression bandaging. Justification Although no studies examining the outcomes of patients with leg ulcers referred from primary care or between health professionals within primary care were found, the principal criteria for appropriate referral are widely agreed by experts. There is good evidence suggesting that patients may not be referred appropriately for specialist assessment. One study of district nurse records indicated that only 35% of leg ulcer patients were referred at any stage for a specialist assessment, and only 7% had been examined by a vascular surgeon (Lees and Lambert 1992). Nevertheless, most of the nurses in this study felt that further investigation of patients was necessary. Another study found that only six of 146 nurses would refer patients with rheumatoid or diabetic ulcers for specialist advice (Roe et al 1993). Urgent vascular referral An urgent vascular referral should be made in the following circumstances: ◆ the patient has an acutely infected or ischaemic foot ◆ there is an ischaemic complication from compression bandaging. Routine vascular referral The patient should be referred to the vascular surgeon if: ◆ venous ulcers treated for three months have not improved ◆ ulcers fail to heal completely in one year ◆ patients with healed ulcers and a history of varicose veins with a view to surgery ◆ there is suspected malignancy. Referral to dermatologist The patient should be referred to the dermatologist if there is: ◆ a rash associated with the ulcer ◆ recurrent contact dermatitis ◆ unusual or atypical ulcers ◆ cellulitis, especially recurrent ◆ inflammatory reaction around the ulcer. Referral to diabetologist The patient should be referred to the diabetologist if there is: ◆ newly diagnosed diabetes ◆ unstable diabetes ◆ diabetic complications of the lower limbs ◆ neuropathy. Strength of evidence III Urgent physician /dermatologist referral The patient with severe cellulitis causing systemic toxicity should be referred to the on-call physician/dermatologist. 8 The management of patients with venous leg ulcers Assessment Assessment of Patients with Leg Ulcers 5. The records show that a bacterial swab has only been taken when there is evidence of clinical infection. For example, pyrexia, cellulitis, increased pain and rapidly enlarging ulcer. 6. The records show that on the first assessment, the patient’s pain level has been assessed and where indicated, appropriate management commenced. Justification Justification Routine bacteriological swabbing is unnecessary unless there is evidence of clinical infection such as: ◆ inflammation/ redness/ evidence of cellulitis ◆ increased pain ◆ purulent exudate ◆ rapid deterioration of the ulcer ◆ pyrexia. The influence of bacteria on ulcer healing has been examined in a number of studies (Trengove et al 1996; Skene et al 1992; Ericksson et al 1984), and most have found that ulcer healing is not influenced by the presence of bacteria. Strength of evidence I Leg ulcers are frequently painful. A significant proportion of patients with venous ulcers report moderate to severe pain (Dunn 1997; Hamer et al 1994; Walshe 1995; Steven et al 1997; Cullum and Roe 1995; Hofman et al 1997). However, one survey found that 55% of district nurses did not routinely assess pain in patients with leg ulcers (Roe et al 1993). Increased pain on mobility may be associated with poorer healing rates (Johnson 1995), and may also be a sign of some underlying pathology such as arterial disease or infection (indicating that the patient may require referral for specialised assessment). Leg elevation is important since it can aid venous return and reduce pain and swelling in some patients. However, leg elevation may make the pain worse in others (Hofman et al 1997). Compression counteracts the harmful effects of venous hypertension and compression may relieve pain (Franks et al 1995). Strength of the evidence II The management of patients with venous leg ulcers Assessment 9 2.1 Assessment of Patients with Leg Ulcers 7. The records show that the measurement of ABPI has been undertaken at least three-monthly or in any of the following situations: sudden increase in size of ulcer; ulcer became painful; change in colour/temperature of foot/leg. Justification Arterial disease may develop in patients with venous disease (Sindrup et al 1987; Callam et al 1987c; Scriven et al 1997) and significant reductions in ABPI can occur over relatively short periods (Nelzen et al 1994; Simon et al 1994; Scriven et al 1997). ABPI will also fall with age. Strength of evidence II 10 The management of patients with venous leg ulcers Assessment 2.2 Management of Patients with Venous Leg Ulcers 8. The records show that patients with venous leg ulcer and an ABPI ≥ 0.8 have received high compression (multi-layer – that is four-layer, threelayer, or short stretch) bandaging. 9. The records show that the patient with a healed ulcer has been educated about the need to wear and how to correctly apply compression stockings. Justification Justification Compression therapy is the most important element of treatment of venous leg ulcers (Effective Health Care Bulletin, 1997). Research has shown that compression improved healing rates compared to treatments using no compression (Rubin et al 1990; Eriksson et al 1984), and is also more cost-effective because the faster healing rate saved nursing time (Taylor et al 1992 unpublished). There is reliable evidence that high compression (25-35 mmHg - Thomas 1990) achieves better healing rates than low compression (Callam et al 1992). Research has shown the benefits of multilayer high compression system over single layer (Nelson et al 1995b; Travers et al 1992). Compression hosiery is an important element in the prevention of recurrence of venous ulceration (Effective Health Care Bulletin, 1997). One trial has shown that three to five year recurrence rates were lower in patients using strong support from class three compression stockings (21%) than in those randomised to receive medium support from class two compression stockings (32%). Class two stockings, however, were better tolerated by patients (Harper et al 1995). Strength of the evidence II It is important to apply compression bandages correctly. Research has shown that incorrectly applied compression bandages may be harmful or ineffective and may predispose the patient to cellulitis or skin breakdown. It has been shown that more experienced or well-trained bandagers obtain better and more consistent pressure results (Logan et al 1992; Nelson et al 1995a). Strength of the evidence I The management of patients with venous leg ulcers Cleansing, Debridement,Dressings, Contact Sensitivety 11 2.3 Cleansing, Debridement, Dressings, Contact Sensitivity 10. The records show that when wound cleansing is indicated, tap water or saline has been used for cleansing. 11. The records show that the patient has received simple, low cost, non - adherent wound dressings unless more costing dressing are indicated (for example, odour, excessive exudate). Justification Wounds and skin are colonised with bacteria that do not appear to impede healing. The purpose of the dressing technique is not to remove bacteria but rather to avoid cross-infection with sources of contamination – for example, other sites of patient or other patients. A trial of clean versus aseptic technique in the cleansing of tracheotomy wounds failed to demonstrate any difference in infection rates between the two methods (Sachine-Kardase et al 1992). There are no trials comparing aseptic technique with clean technique in cleaning chronic wounds, including leg ulcers. There is no evidence that the use of antiseptics confers any benefit to preventing infection. In one study, cleansing traumatic wounds with tap water was associated with a lower rate of clinical infection when compared to sterile isotonic saline (Angeras et al 1992). Justification There is strong evidence that the type of wound dressing has no effect on ulcer healing. A recent systematic review (Nelson et al 1997) has concluded that hydrocolloid dressings confer no benefit over simple, low-adherent dressings. The most important aspect of treatment is the application of high compression bandaging. In the absence of evidence, wound dressings should be low cost, simple to reduce risk of contact sensitivity and low, or non-adherent, to avoid any damage to the ulcer bed (RCN et al 1998). Strength of evidence I Strength of the evidence III 12 The management of patients with venous leg ulcers Cleansing, Debridement,Dressings, Contact Sensitivety Cleansing, Debridement, Dressings, Contact Sensitivity 12. The records show that products containing lanolin or other potential allergens have not been used on the patient. Justification Patients with venous leg ulcers have variable rates of sensitivity to products containing potential allergens. Preparations commonly used as part of the leg ulcer treatment reported to cause contact sensitivity in certain individuals are listed below. Frequency of contact sensitivity and the commonest allergens in leg ulcer patients have been examined in a number of studies (Blondeel et al 1978; Kulozik et al 1988; Cameron 1990; Cameron et al1991; Dooms-Goossens et al 1979; Frake et al 1979; Malten and Kuiper 1985; Paramsothy et al 1988). Strength of evidence III List of common allergens Type Name of allergen Potential source Lanolin wool alcohol, amerchol 101 bath additives, creams, emollients, barriers and some baby products Rubber mercapto / carba/ thiuram mix elastic bandages and supports, elastic stockings, latex gloves worn by carer Perfume fragrance mix, Balsam of Peru bath oils, over the counter preparations such as moisturisers and baby products Preservatives parabens (hydroxybenzoates) medicaments, creams and paste bandages Vehicle cetyl alcohol, stearyl alcohol, cetylstearyl alcohol, paste bandages most creams, including corticosteriod creams, aqueous cream, emulsifying ointment and some Adhesive resin colophony, ester of rosin adhesive backed bandages and dressings The management of patients with venous leg ulcers Cleansing, Debridement,Dressings, Contact Sensitivety 13 2.3 Cleansing, Debridement, Dressings, Contact Sensitivity 13. The records show that topical antibiotics have not been used on the patient. Justification Colonisation of venous leg ulcers is the norm (Skene et al 1992) and there is no firm evidence that it slows ulcer healing (Trengove et al 1996). The use of antibiotics therefore, should be kept to a minimum to discourage an increase in antibiotic resistant bacteria. Topical antibiotics should not be applied on patients with leg ulcers. The criterion is supported by consensus opinion (RCN et al 1998). Strength of evidence III List of topical antibodies Topical antibiotics 14 Examples Source neomycin, framycetin, bacitracin medicaments, tulle dressings, antibiotic creams and ointments The management of patients with venous leg ulcers Cleansing, Debridement,Dressings, Contact Sensitivety 3. Introducing Change The primary health care team will need to make sure that all concerned have the opportunity to study the findings. A multi-disciplinary seminar or discussion meeting at a local level may be appropriate to discuss the findings. Identify the criteria and standards of which you did less well and identify the possible reasons why. Your team will then need an agreed action plan to improve leg ulcer care. Consider the following suggestions: ◆ an educational and training programme for district nurses and practice nurses and general practitioners ◆ a revised policy for the assessment and management of patients with leg ulcers ◆ the introduction of a structured assessment form ◆ use of a computer record for patients with leg ulcers ◆ liaison with local tissue viability specialists, vascular surgeons, dermatologists, rheumatologists and diabetologists. ◆ keep any change as simple as possible to implement. The organisation - community NHS trust ◆ discuss the findings at manager level ◆ compare the results with the national average of standards. Identify strengths and weaknesses ◆ consider the following suggestions for strategies for implementation of the clinical guideline recommendations: ◆ providing resources (personnel, facilities, time, equipment etc) for regular training and education ◆ introducing new technologies (health technology and information technology) into primary care ◆ developing a local structured assessment form for leg ulcers. ◆ support from other agencies such as the RCN or local clinical audit office. For more information see the Implementation Guide in this series. The management of patients with venous leg ulcers Intoducing Change 15 References Ackroyd JS, Young AE 1983 Leg ulcers that do not heal. BMJ; 286 (6360):207-8. Ahroni JH, Boyko EJ, Pecoraro RE 1992 Reliability of computerised wound surface area determinations. Wounds: a compendium of clinical research and practice; 4(4):133-7. Alexander House Group. Consensus paper on venous leg ulcers 1992 Phlebology; 7:48-58. Angeras HM, Brandberg A, Falk A, Seeman T 1992 Comparison between sterile saline and tap water for the cleansing of acute soft tissue wounds. European Journal of Surgery;158:347-50. Baker R, Fraser RC 1995 Development of review criteria: linking guidelines and assessment of quality. BMJ; 311: 370-3. Baldursson B, Sigureirsson B and Lindelof B 1995 Venous leg ulcers and squamous cell carcinoma: a large scale epidemiological study. Br J Dermatology; 133:571-574. Belcaro G et al 1983 Arterial pressure measurements correlated to symptoms and signs or peripheral arterial disease. Acta Chir Belg; 83 (5):320-6. Blondeel A, Oleffe J, Achten G 1978 Contact allergy in 330 dermatological patients. Contact Dermatitis; 4(5):270-6. Brearley SM, Simms MH, Shearman CP 1992 Peripheral pulse palpation: an unreliable physical sign. Annals of the Royal College of Surgeons of England; 74:169-171. Browse NL, Burns KG, Lea Thomas M 1988 Diseases of the veins: Pathology, Diagnosis and treatment. Edward Arnold. London. Buntinx F, Becker H, Briers MD, De Keyser G, Flour M, Nissen G, Raskin T, De Vet H 1996 Interobserver variation in the assessment of skin ulceration. J of Wound Care; 5(4):166-169. Callam MJ 1992 Prevalence of chronic leg ulceration and severe chronic disease in Western Countries. Phlebology Supplement; 1:6-12. Callam M, Harper D R, Dale JJ et al 1992Lothian Forth Valley leg ulcer healing trial - part 1: elastic versus non-elastic bandaging in the treatment of chronic leg ulceration. Phlebology; 7:136-41. Callam MJ, Harper DR, Dale JJ et al 1987b Arterial disease in chronic leg ulceration: an underestimated hazard? Lothian and Forth Valley leg ulcer study. BMJ; 294 (6577):929-31. Callam MJ, Ruckley C, Dale JJ et al 1987c Hazards of compression treatment of the leg: an estimate from Scottish surgeons. BMJ; 295:1382. Cameron J 1990 Patch testing for leg ulcer patients. Nursing Times (Wound Care Suppl); 86(25):63-75. Cameron J, Wilson C, Powerll S, Cherry GW, Tyan T 1991 An update on contact dermatitis in leg ulcer patients. Symposium on Advanced Wound Care. San Francisco 7,8,9, 26. Carter SA 1973 The relationship of distal systolic pressures to healing of skin lesions in limbs with arterial occlusive disease, with special reference to diabetes mellitus. Scand J Clin Lab Invest; 31:239 (suppl 128). Cornwall JV, Dore CJ, Lewis JD 1986 Leg ulcers: epidemiology and aetiology. Br J Surg; 73 (9):693-6. Corson JD, Jacobs RL, Karmody AM, Leather RP, Shah DM 1986 The diabetic foot. Curr Probl Surg; 10:725-88. Cullum N, Fletcher A, Semylen A, Sheldon TA 1997 Compression therapy for venous leg ulcers. Quality in Health Care; 6:226-231. Cullum N and Roe B 1995 Leg ulcers nursing management - a research-based guide. Bailliere Tindall: London. Dooms-Goossens A, Degreef H, Parijs M, Maertens M 1979 A retrospective study of patch test results from 163 patients with stasis dermatitis or leg ulcers. II. Retesting of 50 patients. Dermatology; 159(3):231-8. Douglas WS, Simpson NB 1995 Guidelines for the management of chronic venous leg ulceration. Report of a multidisciplinary workshop. British Journal of Dermatology; 132: 446-452. Dunn C, Beegan A, Morris S 1997 Towards evidence based practice. Focus on Venous ulcers Mid term Review Progress Report compiled for Kings Fund PACE project. London Kings Fund. Callam MJ, Harper DR, Dale JJ et al 1987a Chronic ulcer of the leg: clinical history, BMJ; 294 (6584):1389-91. 16 The management of patients with venous leg ulcers References References Effective Health Care Bulletin. Compression therapy for venous leg ulcers 1997 NHS Centre for Reviews and Dissemination, University of York, August; 3(4). Elliott E, Russell B, Jaffrey G 1996 Setting a standard for leg ulcer assessment. J of Wound Care; 5(4):173-175. Eriksson G, Eklund A, Liden S et al 1984 Comparison of different treatments of venous leg ulcers: a controlled study using stereophotogrammetry. Curr Ther Res; 35:678-84. Etris MB, Pribble J, LaBrecque J 1994 Evaluation of two wound measurement methods in a multicenter, controlled study. Ostomy Wound Management; 40(7):44-48. Fletcher A, Cullum N, Sheldon TA 1997 A systematic review of compression therapy for venous leg ulcers. BMJ; 315:576-579. Frake JE, Peltonen L, Hopsu-Havu VK 1979 Allergy to various components of topical preparations in stasis dermatitis and leg ulcer. Contact Dermatitis; 5(2):97-100. Franks PJ, Oldroyd MI, Dickson D et al 1995 Risk factors for leg ulcer recurrence: a randomized trial of two types of compression stocking. Age and Ageing; 24:4490-4494. Gould DJ, Campbell S, Harding EF. Short stretch versus long stretch bandages in the treatment of chronic venous ulcers. Unpublished. Hamer C, Cullum NA, Roe BH 1994 Patients’ perceptions of chronic leg ulcers. J of Wound Care; 3(2):99-102. Harper DR, Nelson EA, Gibson B et al 1995 A prospective randomised trial of class 2 and class 3 elastic compression in the prevention of venous ulceration. Phlebology; suppl1:872-873. Hofman D, Ryan TJ, Arnold F, Cherry GW, Lindholm C, Bjellerup M, Glynn C 1997 Pain in venous leg ulcers. J of Wound Care; 6(5):222-224. Johnson M 1995 Patient characteristics and environmental factors in leg ulcer healing. J. Wound Care; 4(6):277-282. Johnson M and Miller R 1996 Measuring healing in leg ulcers: practice considerations. Applied Nursing Research; 9(4):204-208. The management of patients with venous leg ulcers Kralj B, Kosicek M Randomized comparative trial of single-layer and multi-layer bandages in the treatment of venous leg ulcers. Unpublished. Kulozik M, Powell SM, Cherry G, Ryan TJ 1988 Contact sensitivity in community-based leg ulcer patients. Clin Exp Dermatol; 13(2); 82-4. Lambert E, McGuire J 1989 Rheumatoid leg ulcers are notoriously difficult to manage. How can one distinguish them from gravitational and large vessel ischaemic ulceration? What is the most effective treatment? Br J Rheumatol; 28 (5):421. Lees TA and Lambert D 1992 Prevalence of lower limb ulceration in an urban health district. Br J Surg; 79:1032-1034. Liskay AM, Mion LC, Davis BR 1993 Comparison of two devices for wound measurement. Dermatology Nursing; 5(6):437-440. Logan RA, Thomas S, Harding EF, Collyer GJ 1992 A comparison on sub-bandage pressures produced by experienced and inexperienced bandagers. J of Wound Care; 1(3):23-26. Majeske C 1992 Reliability of wound surface area measurements. Physical Therapy; 72(2):138-41. Malten KE, Kuiper JP 1985 Contact allergic reactions in 100 selected patients with ulcus cruris. Vasa; 14(4):340-5. Moffatt CJ, Franks PJ, Oldroyd M, Bosanquet N, Brown P, Greenhalgh, McCollum CN 1992 Community clinics for leg ulcers and impact on healing. BMJ; 305(5):1389-1392. Moffatt CJ, Oldroyd MI, Greenhalgh RM, Franks PJ 1994 Palpating ankle pulses is insufficient in detecting arterial insufficiency in patients with leg ulceration. Phlebology; 9:170-172. Moffatt CJ and O’Hare L 1995 Ankle pulses are not sufficient to detect impaired arterial circulation in patients with leg ulcers. Journal of Wound Care; 4(3):134-137. Nelson EA, Ruckley CV, Barbenel JC 1995a Improvements in bandaging technique following training. Journal of Wound Care; 4(4):181-184. Nelson EA, Harper DE, Ruckley CV et al 1995b A randomized trial of single layer and multi-layer bandages in the treatment of chronic venous ulceration. Phlebology; suppl 1:915-916. References 17 References Nelson EA and Jones JE 1997 The development, implementation and evaluation of an educational initiative in leg ulcer management. Research and Development Unit, Department of Nursing, University of Liverpool Nelzen O, Bergqvist D, Lindhagen A 1993 High prevalence of diabetes in chronic leg ulcer patients: a cross-sectional population study. Diabetic Medicine; 10:345-350. Nelzen O, Bergqvist D, Lindhagen A 1994 Venous and non-venous leg ulcers: clinical history and appearance in a population study. Br Journal of Surgery; 81:182-187. Northeast A, Layer G, Wilson N et al 1990 Increased compression expedites venous ulcer healing. Presented at Royal Society of Medicine Venous Forum. London: RSM Paramsothy Y, Collins M, Smith AG 1988 Contact dermatitis in patients with leg ulcers. The prevalence of late positive reactions and evidence against systemic ampliative allergy. Contact Dermatitis; 18(1):30-6. RCN Institute, Centre for Evidence Based Nursing, University of York, and the School of Nursing, Midwifery and Health Visiting, University of Manchester, 1998, Clinical practice guidelines for the management of patients with venous leg ulcers: recommendations for assessment, compression therapy, cleansing, debridement, dressings, contact sensitivity, training/education and quality assurance. Roe BH, Luker KA, Cullum NA, Griffiths JM, Kenrick M 1993 Assessment, prevention and monitoring of chronic leg ulcers in the community: report of a survey. J of Clin Nurs; 2:299-306. Rubin J, Alexander J, Plecha E et al 1990 Unna’s boot vs polyurethane foam dressings for the treatment of venous ulceration. A randomized prospective study. Arch Surg; 125:489-90. Sachine-Kardase A, Bardake Z, Basileiadou A, Dimpinoydes, Ouxoyne A, Patse O 1992 Study of clean versus aseptic technique of tracheotomy care based on the level of pulmonary infection. Noseleutike; 31(141):201-11. Scottish Intercollegiate Guidelines Network: The care of patients with chronic leg ulcer. SIGN July 1998. Simon DA, Freak L, Williams IM, McCollum CN 1994 Progression of arterial disease in patients with healed venous ulcers. J of Wound Care; 3(4):179-180. Sindrup JH, Groth S, Avnstorp C, Tonnesen KH, Kristensen JK 1987 Coexistence of obstructive arterial disease and chronic venous stasis in leg ulcer patients. Clin Exp Dermatol; 12(6):160-3. Skene AI, Smith JM, Dore CJ, Charlett A, Lewis JD 1992 Venous leg ulcers: a prognostic index to predict time to healing. BMJ; 7:1191-1121. Stacey MC, Burnadnd KG, Layer GT, Pattison M, Browse NL 1991 Measurement of the healing of venous ulcers. Aust N Z J Surg; 61:844-8. Stevens J, Franks PJ, Harrington MA 1997 community/hospital leg ulcer service. J of Wound Care; 6(2):62-68. Taylor P 1992 An examination of the problems and perceptions patients’ experience in complying with venous leg ulcer management. Unpublished Bachelor of Nursing Dissertation, Swansea Institute Library, Swansea. Thomas S, Bandagers and Bandaging 1990 Nursing Standards; Vol. 4; No. 39; pp46-47. Thompson B A 1993 A management protocol for leg ulcers. Wound Management; 4: 81-84. Travers J, Dalziel K, Makin G 1992 Assessment of new one-layer adhesive bandaging method in maintaining prolonged limb compression and effects on venous ulcer healing. Phlebology; 7:59-63. Trengove NJ, Stacey MC, McGechie DF, Mata S 1996 Qualitative bacteriology and leg ulcer healing. J of Wound Care; 5(6):277-280. Waddell G, Feder G, McIntosh A, Lewis M, Hutchinson A 1996 Low Back Pain Evidence Review. London: Royal College of General Practitioners. Walshe C 1995 Living with a venous ulcer: a descriptive study of patients’ experiences. Journal of Advanced Nursing; 22(6):92-100. Yang D, Morrison BD, Vandongen YK, Singh A, Stacey MC 1996 Malignancy in chronic leg ulcers. Med J Aust; 164:718-721. Scriven JM, Hartshorne T, Bell PRF, Naylor AR, London NJM. Single-visit venous ulcer assessment clinic: the first year. Br J of Surg 1997; 84:334-336. 18 The management of patients with venous leg ulcers References Sources of Further Information Useful contact addresses: Tissue Viability Society Glanville Centre Salisbury district Hospital Salisbury SP2 8BJ. Tel: 01722 336262 http://www.tvs.org.uk/ Quality Improvement Programme Information Service RCN 20 Cavendish Square London W1M 0AB Tel: 020 7647 3831 http://www.rcn.org.uk The Audit Commission 1 Vincent Square London SW1P 2PN Tel: 020 7828 1212 http://www.audit-commission.gov.uk/ Scottish Intercollegiate Guidelines Network The SIGN secretariat Royal College of Physicians 9 Queen Street Edinburgh EH2 1JQ Tel: 0131 225 7324 http://www.show.scot.nhs.uk/sign/home.htm The Cochrane Wounds Group Department of Health Studies University of York. York Y01 5DD Tel: 01904 43411 http://www.york.ac.uk/depts/hstd/centres/evidence /ev-intro.htm#cochrane-wounds-group Clinical Governance Research and Development Unit Department of General Practice and Primary Health Care University of Leicester Leicester General Hospital Leicester LE5 4PW Tel: 0116 258 4873 http://www.le.ac.uk/cgrdu/index.html NICE (National Institute for Clinical Excellence) 90 Long Acre London, WC2E 9RZ Tel: 020 7849 3444 http://www.nice.org.uk The management of patients with venous leg ulcers Sources 19 Appendix 1. Documentation Development of review criteria Based on the national clinical guideline for leg ulcer management (RCN et al 1998), the review criteria were developed according to a method developed by researchers in the Clinical Governance Research and Development Unit (Baker et al 1995; Fraser et al 1997) The method involved: identification of the key elements of care ◆ focused systematic reviews based on the national clinical practice guideline (RCN et al 1998) and justified by evidence ◆ taking into account consensus based recommendation considered to have an important impact on outcome ◆ presentation of the criteria in a protocol. ◆ The standards A standard in this audit protocol refers to the level of performance for each criterion, to which community nurses are aiming. The purpose of criteria and standards is to assist in the improvement of care. The ultimate aim for most of the criteria is the achievement of a standard of 100%, although it is recognised that there may be perfectly acceptable reasons for falling short of this level on some occasions in relation to some criteria. 20 The management of patients with venous leg ulcers Appendix 1: Audit Form Appendix 2. Nursing Management of Venous Leg Ulcers in the Community: Audit Form Please read the Instructions for audit form before you complete the form. Date completed: Ref. No. _______________ DOB ____________ Sex: M ❑ F❑ First assessment by district nurse ❑ practice nurse ❑ specialist nurse ❑ other ______ grade ______ Patient mostly seen at home ❑ general clinic ❑ leg ulcer clinic ❑ other _________________ Patient mostly seen by district nurse ❑ practice nurse ❑ specialist nurse ❑ other ______ grade ______ Q 1. A clinical history and physical examination at assessment visit Has the medical history been documented? yes ❑ no ❑ Has BP been recorded? yes ❑ no ❑ Has urinalysis been undertaken? yes ❑ no ❑ Has weight been recorded? yes ❑ no ❑ Did record show that patient had a previous ulcer history ? yes ❑ no ❑ If yes, have the following items been documented? duration of previous ulcer ❑ number ❑ method of treatment ❑ time to heal ❑ type ❑ site ❑ First assessment visit: a full assessment takes place within two weeks of first contact of leg ulcer patient Q 2. Doppler ABPI at first assessment visit yes ❑ no ❑ If not applicable, reason_____________________________________________________________ Level of ABPI L __________ R __________ Q 3. Has ulcer(s) size been measured at first assessment visit? If yes, was this by: tape measure ❑ mapping ❑ other ______________________________ yes ❑ no ❑ date measured__________ photograph ❑ Ulcer 1: length __cm width __cm duration of ulcer __mth Ulcer 2: length __cm width __cm duration of ulcer __mth Ulcer 3: length __cm width __cm duration of ulcer __mth Q 4. Has pain assessment been undertaken? length and width ❑ is this a recurrent ulcer? is this a recurrent ulcer? is this a recurrent ulcer? yes ❑ no ❑ yes ❑ no ❑ yes ❑ no ❑ yes ❑ no ❑ Is the ulcer painful? yes ❑ no ❑ If yes, did patient receive analgesia? yes ❑ no ❑ Please complete the following items at the end of the audit period or if patient is lost to follow-up/is referred/ulcer healed/patient died. Date of completion: __________________________________________ Q 5. Referral Was referral made? yes ❑ no ❑ if yes, reasons: ____________________ date of referral_________ Referred to: specialist nurse ❑ GP ❑ vascular surgeon ❑ dermatologist ❑ other ______________________________ diabetologist ❑ Q 6. Bacterial swab Has a bacterial swab been taken? yes ❑ no ❑ was ulcer infected? yes ❑ no ❑ Please turn over page The management of patients with venous leg ulcers Appendix 2: Audit Form 21 Appendix 2. Nursing Management of Venous Leg Ulcers in the Community: Audit Form Q 7. Leg ulcer re-assessment yes ❑ no ❑ Has measurement of ulcer(s) size been repeated? If yes, has ulcer size been repeated at every __________wk/wks Q 8. Graduated compression yes ❑ no ❑ if not applicable, reasons ___________________________ If yes, type of bandage used Setopress ❑ Surepress ❑ Tensopress ❑ Comprilan ❑ Robertson’s Ultra 4 ❑ Rosidal K ❑ 4 layer bandage ❑ Class 2/3 hosiery ❑ other – list no more than five products __________________________________________________ Q 9. Which cleansing agent was used? tap water ❑ normal saline ❑ none r other – list no more than five products __________________________________________________ Q10. Which dressings were used? Hydrocolloid ❑ Foam ❑ Alginate ❑ Tulle gras ❑ NA Tricotex r other – please state __________________________________________________ Q11. Skin care Have you used any skin care preparation? yes ❑ no ❑ If yes, was it: emollient ❑ steroid cream or ointment ❑ Q12. Outcome died ❑ if other, please state________________ healed ❑ improved ❑ no change ❑ referral ❑ leg ulcer related admission ❑ other __________________________________________________ If ulcer(s) completely healed, please indicate the time to heal: Ulcer 1 __________wks Ulcer 2 ________wks Ulcer 3 ________wks Q13. Prevention of recurrence Did patient receive education on compression stockings? yes ❑ no ❑ If ulcer healed, did patient receive compression stockings? yes ❑ no ❑ not applicable ❑ If not applicable, please give reasons ____________________________________________________ Q14. Work load On average, how many visits a week (leg ulcer care only)? _______________ Total number of visits (leg ulcer care only) ______ Average time for each visit <20 mins ❑ 20 mins ❑ (excluding travel time) 22 The management of patients with venous leg ulcers 30 mins ❑ 40 mins ❑ >40 ❑ Appendix 2: Audit Form Appendix 2. Instructions for Audit Form Which patients are included in this audit? Patients diagnosed with venous leg ulcers are included in the project. This includes new patients, patients who are in the process of treatment and patients who have a recurrent ulcer. This retrospective audit will include patients with venous leg ulcers under your care at the present time. All patients who participate in the audit project should have a sticker on their case records and an audit form attached. Data collection - one form per patient You should use one audit form for each individual patient. Questions 1 to 4 should be completed for patients with venous leg ulcers at the start of the audit. Questions 5 to 14 should be completed at the end of the audit or if the patient is lost to follow-up/ is referred/ has a healed ulcer/ has died. Please state the date of completion. General information The beginning of the form is general information about the patient. The reference number will be the patient’s case record number or any code number for identifying the patient locally. Q 1. A clinical history and physical examination has been undertaken at the first assessment. Previous ulcer history - if the patient has a leg ulcer history, the yes box should be ticked, and the follow-up questions answered according to available information in the case notes at the time of the assessment visit. Medical history - the yes box should only be ticked when a full medical history is documented in the case records. The no box ticked if there is no medical history documented (if a patient does not have a history of relevant medical conditions for example, vascular disease, coronary heart disease etc, it must be documented at the assessment visit). BP, urinalysis, weight - the yes box should only be ticked where those items were undertaken and documented at the assessment visit. Q 2. Doppler ABPI (ankle/brachial pressure index) has been measured at the first assessment visit. Yes box is ticked when ABPI has been measured within two weeks of first contact. If yes, please state the date of assessment and the level of ABPI. If a Doppler machine is not available in the team or practice or for any other reason the ABPI could not be undertaken, please tick the not applicable box and state the reason. Q 3. Ulcers recorded at first assessment The yes box should only be ticked when the ulcer size is documented at the first assessment visit. Please indicate how you measure ulcer size normally. If you use any other method of measurement, please tick other and state the method you have used. If the patient has more than one ulcer on both legs, please describe ulcer two or add ulcer three if necessary. If more than three ulcers, please document the largest three sites. Q 4. Pain assessment The yes box should only be ticked where pain assessment has been undertaken on the patient at the assessment visit. For analgesia, the yes box should be ticked when the patient has received analgesia from any professional. Form Q 5. Referral If the patient needs to be referred to a specialist, please give the date of referral, the main reason for referral and tick the type of specialist to which you have referred your patient. For most practices, the referral will go to the GP first. In this situation, please tick GP and also tick any other specialist to which you consider the patient should be referred. Q 6. Bacterial swab If the yes box is ticked, please state the reasons. The management of patients with venous leg ulcers Appendix 2: Audit Form 23 Appendix 2. Instructions for Audit Form 2. Instructions for Audit Q 7. Leg ulcer re-assessment If yes box is ticked, please indicate how often the ulcer size has been re-measured. Q 8. Graduated compression Please indicate the products you have used on this patient (for the whole time of treatment) and tick more than one type of bandage if necessary. For other, please do not list more than five products. If the patient was not suitable for high compression (for example, acute heart failure, rheumatoid arthritis, grossly distended leg or any other reasons), please tick not applicable and state the reason. Q 9. Cleansing agent As you might use different agents for the patient during care, please tick the one you used most commonly more than one if necessary. If you have used other cleansing agents, please list no more than five products. Q10. Dressings This applies to all dressings you have used for this patient during the whole treatment period. Please tick more than one if necessary. If you tick other, please list up no more than five products you have used. Q11. Skin care If yes, please tick the preparation you have used - you can tick more than one box if it is necessary. If you tick other, please state no more than five products. Q12. Outcome Please indicate the outcome for this patient. If the ulcer healed, please indicate the time to heal the ulcer(s). If the patient has more than one ulcer or ulcers on both legs, please describe the outcome of ulcer 2 or add ulcer 3 if necessary. Q13. Prevention of recurrence For patients who have received education on compression stockings, the yes box should only be ticked if this has been documented. If the ulcer is not healed by the end of the audit, or is not suitable for compression stockings, please tick not applicable and state the reasons. Q14. Work load Number of visits a week - this will be the average number of visits per week in the period of care/or for most of the period of care. The average time for each visit will not include the first visit and will exclude travel time. Where should you send the completed forms? Once you have completed the form, please ensure all the items are filled in. The completed form should be sent back to the project leader in your organisation. Please make a photocopy of each form before sending it. 24 The management of patients with venous leg ulcers Appendix 2: Audit Form The management of patients with venous leg ulcers Notes 25 26 The management of patients with venous leg ulcers Notes RCN Members £3.50 Non RCN Members £4.50 © Copyright 2000: Royal College of Nursing. All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted in any form or by any means electronic, mechanical, photocopying, recording or otherwise, without prior permission of the Publishers or a licence permitting restricted copying issued by the Copyright Licensing Agency, 90 Tottenham Court Road, London W1P 9HE. This publication may not be lent, resold, hired out or otherwise disposed of by way of trade in any form of binding or cover other than that in which it is published, without the prior consent of the Publishers. ISBN 1-873853-89-0 Publication code: 001 269